Atypical Base of Skull Osteomyelitis Presenting as Bilateral Facial Palsy
Received: 08-Nov-2018 / Accepted Date: 06-Dec-2018 / Published Date: 17-Dec-2018 DOI: 10.4172/2314-7326.1000282
Abstract
Base of skull osteomyelitis is a rare cause of headaches and cranial neuropathies in general, and cranial nerve VII palsy in particular. Both typical and atypical skull base osteomyelitis can have similar presentation and Magnetic Resonance Imaging of the brain is very important to differentiate between them since each is caused by a different organism and requires different treatment. However, bone sampling remains crucial for diagnosis in atypical cases. We hereby report a case of atypical skull base osteomyelitis presenting as bilateral peripheral facial nerve palsy. We also present a new and less invasive diagnostic and therapeutic approach especially when bone sampling is not possible and intravenous empiric treatment cannot be initiated.
Keywords: Aspergillus; Base of skull osteomyelitis; Bilateral facial nerve palsy
Introduction
Bilateral facial palsy and non-specific headaches may occasionally be encountered in outpatient clinics and emergency rooms. Lyme disease is the most common cause, followed by Guillain-Barre syndrome, trauma, sarcoidosis and acquired immune deficiency syndrome [1]. Base of skull osteomyelitis is a rare cause of cranial neuropathies in general and cranial nerve VII palsy. It typically involves cranial nerves VI, IX, X, XI and XII [2]. We hereby present a case of atypical skull base osteomyelitis presenting as bilateral peripheral facial nerve palsy, as well as discuss a new and less invasive diagnostic and therapeutic approach.
Skull base osteomyelitis (SBO) is an infrequent condition that is potentially life threatening if not recognized and treated promptly. Typical cases begin with otitis externa that later involves the temporal bone and adjacent soft tissues. Patients at risk are typically elderly, diabetic, immunocompromised (example secondary to steroids use or Human Immunodeficiency Virus infection) or have a chronic inflammatory sphenoid disease. The most common organism involved in skull base osteomyelitis arising from otitis externa is Pseudomonas Aeruginosa [3].
Atypical skull base osteomyelitis is difficult to diagnose, as it occurs less frequently and is not preceded by otitis externa. Responsible organisms consist mainly of fungal and Gram-positive bacterial species [4]. It involves the sphenoid and occipital bones rather than the temporal bone [3]. In both cases, diagnosis relies heavily on characteristic Magnetic Resonance Imaging (MRI) findings; however, bone sampling is crucial in atypical cases. As for treatment of fungal skull base osteomyelitis, Amphotericin B is recommended as an empirical treatment pending culture results [5]. The challenge is still in atypical cases of fungal SBO where tissue cannot be obtained for adequate sampling and classic empiric treatment cannot be administered.
Case Report
A 66-year-old man presented with 1-month history of bilateral facial weakness associated with headache reported as bi-parietal, pressure- like, reaching 10/10 in intensity, worse when lying supine, unrelieved by analgesics and associated with nausea and photophobia. He subsequently developed hoarseness, hearing loss, dysarthria, decreased appetite and a 13-kg weight loss over 2 weeks. There were no reported visual symptoms, fever or chills. He had no chronic or recent sinusitis, otitis media or otitis externa.
Patient’s medical history was pertinent for poorly-controlled diabetes mellitus (HbA1c 10.9% of total hemoglobin) and hypertension. He worked as a farmer and is an ex-smoker (80 pack years). He was not taking any immunosuppressive medications.
Physical examination upon presentation (1 month after symptoms onset) revealed severely diffuse scalp tenderness upon palpation, neck stiffness, flaccid dysarthria, hoarseness, bilateral peripheral facial palsy (House-Brackmann 6) and decreased vibratory sense in both lower extremities at the toes level.
Inflammatory markers were elevated, with C-reactive protein (CRP) of 106.8 mg/L, and Erythrocyte Sedimentation Rate (ESR) of 130 mm/hour.
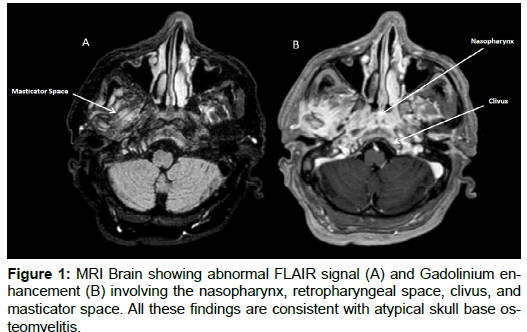
Lumbar puncture was prominent for lymphocytic pleiocytosis (WBC of 35/cu-mm with 85% lymphocytes), a slightly elevated protein count (0.66 g/L) and a normal glucose level (96 mg/dL). A comprehensive meningitis panel and cerebrospinal fluid cultures were all negative. An audiology test revealed bilateral moderate-to-severe sensorineural hearing loss. Magnetic Resonance Imaging (MRI) of the brain showed abnormal Fluid Attenuated Inversion Recovery (FLAIR) signal and gadolinium enhancement of the clivus, nasopharynx, retropharyngeal and masticator spaces in keeping with atypical or central osteomyelitis of the skull base (Figure 1).
He was evaluated by an Ear Nose and Throat specialist with work up including right middle ear fluid sampling with cultures grew Aspergillus. Both otitis media and externa were excluded. He was started on oral Voriconazole which lead to a significant improvement in his headache and hearing capacities.
Discussion
Both typical and atypical skull base osteomyelitis can present with similar non-specific intractable headache and subsequent cranial neuropathies [3]. MRI is very important to help us differentiate between them since each is caused by a different organism and thus requires different treatment. MRI findings of atypical or central SBO consist of abnormal signals in occipital or sphenoid bones, typically in the clivus. Hypointensity on T1 images, which enhances post-contrast, and homogeneous or heterogeneous high-FLAIR signals of the clivus are found in all atypical cases [3].
Our patient was considered to have atypical SBO due to the abnormal characteristic clival imaging on MRI, lack of preceding otitis externa, otitis media and sinusitis, and absence of classic signs of infection such as fever, elevated white blood cell count, and positive blood and CSF cultures.
Skull bone sampling, considered a gold-standard confirmatory test, could not be obtained. Instead, right middle ear fluid was collected as he was found to have middle ear fluid on imaging, without any symptoms to suggest external or middle ear pathology. This is thought to be secondary to Eustachian tube dysfunction in the setting of abnormal nasopharyngeal submucosal soft tissue inflammation [3].
Cultures heavily grew Aspergillus species out of which A. fumigatus is the most commonly involved in invasive Aspergillosis. Although most CNS Aspergillosis is associated with osteomyelitis, diagnosis is often delayed because cultures growing fungi are usually misinterpreted as an opportunistic colonization [6]. Our patient was considered to have Aspergillus SBO due to proximity. Empiric treatment with Amphotericin B was not initiated since the patient refused prolonged intravenous treatment, so he was started on oral Voriconazole with marked improvement of his symptoms in 1 week. Although a prolonged course of oral Voriconazole was shown to be effective in some cases of invasive Aspergillus causing Otitis Externa, it is still considered a non-classic treatment in these patients [7]. In addition, we like to shed light on the importance of involving patients in treatment-related decision-making, especially in cases requiring prolonged follow-up, as well as the importance of involving a care manager, who would ensure a better compliance and follow up with care recommendations [8].
Conclusion
In conclusion, we report a case of Skull Base Osteomyelitis presenting as bilateral facial nerve palsy. We also present a new and less invasive diagnostic and therapeutic approach specially when bone sampling is not possible, and intravenous Amphotericin B cannot be administered.
References
- Jain V, Deshmukh A, Gollomp S (2006) Bilateral facial paralysis: case presentation and discussion of differential diagnosis. J Gen Intern Med 21: C7-10.
- Clark MP, Pretorius PM, Byren I, Milford CA (2009) Central or atypical skull base osteomyelitis: Diagnosis and treatment. Skull Base 19: 247-254.
- Chang PC, Fischbein NJ, Holliday RA (2003) Central skull base osteomyelitis in patients without otitis externa: imaging findings. AJNR Am J Neuroradiol 24: 1310-1316.
- Grobman LR, Ganz W, Casiano R, Goldberg S (1989) Atypical osteomyelitis of the skull base. Laryngoscope 99: 671-676.
- Blyth CC, Gomes L, Sorrell TC, Da Cruz M, Sud A, et al. (2011) Skull-base osteomyelitis: Fungal vs. bacterial infection. Clin Microbiol Infect 17: 306-311.
- Nicholson S, King R, Chumas P, Russell J, Liddington M (2016) Aspergillus osteomyelitis of the skull. J Craniofac Surg 27: e504-506.
- Parize P, Chandesris MO, Lanternier F, Poiree S, Viard JP, et al. (2009) Antifungal therapy of Aspergillus invasive otitis externa: Efficacy of voriconazole and review. Antimicrob Agents Chemother 53: 1048-1053.
- Ciccone MM, Aquilino A, Cortese F, Scicchitano P, Sassara M, et al. (2010) Feasibility and effectiveness of a disease and care management model in the primary health care system for patients with heart failure and diabetes (Project Leonardo). Vasc Health Risk Manag 6: 297-305.
Citation: Ibrikji S, Halabi TE, Makki A, Salameh J (2018) Atypical Base of Skull Osteomyelitis Presenting as Bilateral Facial Palsy. J Neuroinfect Dis 9: 282. DOI: 10.4172/2314-7326.1000282
Copyright: © 2018 Ibrikji S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Share This Article
Open Access Journals
Article Tools
Article Usage
- Total views: 3318
- [From(publication date): 0-2018 - Apr 27, 2024]
- Breakdown by view type
- HTML page views: 2727
- PDF downloads: 591