Journal of Rehabilitation Practices and Research Volume 4 (2023), Article ID: JRPR-145
https://doi.org/10.33790/jrpr1100145Research Article
An Innovative Approach Towards The Treatment of The Cervical Myelopathy: A Case Study
Lopamudra Sahoo, Student, MPT1, Debiprasanna Samal, MPT2*, & Thiagarajan Subramanian3
1,3Department of Physiotherapy, School of Applied Medical Sciences, Lovely Professional University
2SVNIRTAR, Olatpur, Cuttack, Odisha, India.
Corresponding Author Details: Debiprasanna Samal, MPT, SVNIRTAR, Olatpur, Cuttack, Odisha, India.
Received date: 05th September, 2023
Accepted date: 09th June, 2023
Published date: 12th June, 2023
Citation: Sahoo, L., Samal, D., & Subramanian, T., (2023). An Innovative Approach Towards The Treatment of The Cervical Myelopathy: A Case Study. J Rehab Pract Res, 4(1):145.
Copyright: ©2023, This is an open-access article distributed under the terms of the Creative Commons Attribution License 4.0, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Abstract
Background: A 32 years female diagnosed with Cervical Myelopathy from 6 months, came to the department with the chief complain of pain in both the lower limb, difficulty in walking and medically diagnosed with Cervical Myelopathy (CM).
Methodology: A initial assessment has been done for the patient came to the department with the medical diagnosis of CM, treated with Levator Muscle Stretching and other conventional exercises for 5 days per week for 5weeks.
Result: After the whole sessions the client improved with the Symptoms, like Pain, Improvement in Balance, Gait and the Quality of Life as well.
Conclusion: Levator Muscle Stretching along with other conventional exercises used as an innovative approach for the management of the CM is found to be helpful.
Key Words: Levator stretching, Cervical Myelopathy, Pain, Quality of Life.
Introduction
Background
Myelopathy could be defined as the dysfunction of the Spinal cord. Cervical myelopathy is a disorder that acquits compression at the cervical level of the spinal column that haps when the size of the canal is decreased and / or the volume of its content is increased supervening in spasticity (sustained muscle contractions), hyperreflexia, pathological reflexes, digit/hand clumsiness, and/or gait disruption. If not managed congruously the patient may lead to paralysis with progression of stepwise functional decline [1-12]. Cervical myelopathy could be congenital (has more prevalence) or acquired in origin, caused due to degenerative changes in the cervical spine such as disc degeneration, degeneration of facet joints, osteophyte formation, segmental ossification of the posterior longitudinal ligament, ligamentum flavum hypertrophy, disc herniation etc. Extradural mass (tumours), post-traumatic deformities, infections (tuberculosis), posttraumatic kyphosis, vascular disorders (vascular malformations, spinal cord infarct and epidural hematoma), nutritional disorders etc. could be some possible causes [14].
Literature Survey
Common Presentation of Case
It does not have a single pathological signs or symptoms, sometimes the onset is insidious with a long duration of episodic, stepwise progression and can present a vast array patient to patient search result. (2) Patients of cord compression can be completely asymptomatic with regards to both pain and neurological function. Others can have moderate signs of just neck pain or an aspect of a radicular arm pain, with non-dermatomal pattern presentation in the upper extremities. Signs and symptoms of myelopathy may vary significantly based on the location and severity of the dysfunction [3]. In 75% of the patients, episodic worsening with neurological deterioration occurs, 20% have slow steady progression, and 5% experience rapid onset and progression. (PP Sir) Extensive Literature survey have explained that patients with CSM reported that gait disturbances occurred in 80% of patients, clumsiness in 67%, weakness of arms in 47%, and numbness of arms in 84% [4].
Diagnostic Criteria
Physical Diagnosis: Cook et al. stated that the any of the combination of any 4/5 symptoms of the following can raise the probability of the disease of 94-99%. i.e. a. Gait Deviation b. +Ve Hoffmann’s Sign c. Inverted supinator sign d. +ve Babinski test e. 45 or elderly age group Population f. Spurling’s Test or Distraction Test g. Hyperreflexia of Biceps/ Quadriceps/ Achilles h. Pain Constancy i. L’hermitte Sign h. Romberg Test [11].
Questionnaire
The DOWN questionnaire (Sensitivity of 72%, a Specificity of 89%) is composed of 4 questions that encompass common symptoms associated with CSM are as following:
• Have you noticed that you are Dropping things or that your hands feel clumsy?
• Have you felt more Off-balance or unsteady on your feet?
• Do you feel Weakness in one or both of your arms or hands?
• Do you feel Numbness or tingling in one or both of your arms or hands?
The Nurick score, the Japanese Orthopaedic Association score (JOA) and its modified version (mJOA), and the Cooper Myelopathy Scale are the other important screening tools for CM, but due to their complexity those are not very much familiar in the clinical setting or for screening and instead are typically used in research settings [4].
Radiological Findings
Anteroposterior, lateral and oblique radiographs should be performed on patients suspected of having cervical myelopathy. Spondylotic changes, such as narrowing of the disc space, osteophyte formation and listhesis, may be appreciated. The lateral radiograph should be critically reviewed for evidence of decrease in the sagittal dimension of the osseous canal resulting from congenital stenosis, spondylosis or ossification of the PLL. Any decrease in the segmental and global lordosis may indicate the same [6]. A detailed & Pain staking neurological examination along with MRI is the most valuable and appropriate diagnostic tool for Cervical Myelopathy having the Specificity (82%-89%) and Sensitivity (79%-95%) (LR+=4.39- 7.92, LR-=0.06-0.27), MRI typically show intramedullary signal abnormalities due to oedema and structural changes with a hyperintense signal on T2W imaging (WI) (58–85% of patients with clinical myelopathy) and, less commonly, hypointense signal on T1- WI. A pancake-like gadolinium enhancement on sagittal images and a circumferential enhancement on axial images are also indicative of Spondylosis as one of the causes of CM [2,15].
In neurological condition like Cervical Myelopathy rehabilitation, psychological Assessment has the most important role to play in various aspects like, collecting diagnostic information, increasing the ease of assessment tools, and many other critical information for to Neurological, Psychological and Neurological assessment [4].
Management
Surgical Management: The primary goal of all of these surgical techniques is to relieve compression of the spinal cord and its associated microcirculation. The surgical management of CSM has evolved from the classic anterior cervical discectomy and fusion procedure developed by Smith, Robinson, and Cloward to now include combined anterior/posterior decompression and fusion procedures as well as a myriad of laminotomy techniques [16]. A score of ≤ 12 on modified Japanese Orthopaedic Association score (mJOA) is a definite indication for surgery in patients with CSM [17]. Anterior cervical corpectomy is indicated for 1. patients with pathology that extends beyond the interspace level (for example, migrated disc fragment behind the vertebral body or an associated ossified posterior longitudinal ligament (OPLL) behind the vertebral body). Single-level corpectomy is generally considered safe and associated with successful outcomes for CSM. Laminectomy has traditionally been the gold standard for posterior approaches for CS is considered as a safe surgical procedure. However, the biggest complication after laminectomy is post-laminectomy instability/ kyphosis [16].
Conservative Management: Cervical Myelopathy can be treated with many conservative managements like, Mechanical Traction, Soft tissue Mobilization, Passive Stretching of the muscles surrounding upper Limb and neck. Manual stretching causes the neuro-dynamic gliding between nerves and fascial sheath surrounding it, producing hypoalgesia and decreased sympathetic response possibly due to activation of descending inhibitory pain modulation pathway. Stretching can be helpful in reducing pain, Increasing the Range of Motion (Neck & shoulder Joint) and Quality of Life. Previously conducted, studies state that Cervicothoracic Stretching can improve blood circulation, reduce stiffness & spasm in muscles, leads to return in normal Neuromuscular balance between muscle groups, improves postural awareness & body posture. Study by Thavatchai et.al. proves that both stretching & Isometric Strengthening can improve neck Disability, pain intensity, CVA Angle & neck muscle strength in chronic mechanical neck pain. Levator Scapulae (originating from posterior tubercule of the transverse process of Cervical Vertebra, supplied by cervical Nerve (C3-C4) and dorsal scapular Nerve (C5) muscle often gets tensed and associated with Mechanical Neck Pain, dysfunction of the muscles of Cervical Spine, that may lead to tightness cause the forced lateral Flexion of the Cervical Spine which may cause further compression of Spinal Canal. So this study aims to find out the effectiveness of Levator Scapulae muscle Stretching as a new innovative approach for the Cervical Myelopathy management.
Case Description
The Ethical Consent for this case study has been taken, from the University Ethical Committee, with the reference Number LPU/ IEC/2021/01/14.
Subjective Examination
History
A 32 years old Female (Right-Handed, 4.8inch height) came to the department with the chief complain of pain in both the lower limb and difficulty in walking in the last 6 months, with the Medical Diagnosis of Cervical Myelopathy. She explained that She got injury to her neck before 1 and ½ years during some household activities, then she did not have much difficulty at instant, but after her pregnancy following the injury, she is having ain of gradual onset over the neck and upper Limb. Assessed with NPRS of 7 in the 0-11 NPRS scale,
Presenting Complains and Presentation
She had referred to Physician and got a Magnetic Resonance Imaging (MRI) done, with the findings that, hypersensitive area in the spinal cord at C3-C4 level-likely Myelitis, C3-C4 disc shows postero-lateral Herniating towards the right side producing moderate compression of thecal sac and Spinal Cord, moderate right lateral recess, moderate canal with moderate right side neural foraminal narrowing and mild left side neural foraminal narrowing. C2-C3 disc shows diffuse disc bulge producing mild thecal sac indentation and mild canal narrowing. Mild Spinal Canal narrowing at C4-C5, C5 C6, C6-C7, C7-T1 levels. Cervical Spondylosis with degenerative changes in C2-C3, C3-C4, C4-C5 and C5-C6 discs. Now her condition is worsening over the period gradually progressed to Imbalance, and difficulty in walking along with very much evident Clumsiness over the hand and jerking response of the Knee joint by a simple tap over the Joint. Also having difficulty in doing the household activities. The pain is aggravating over walking for a distance, and getting relaxed over a period of rest.
Additional Pertinent findings or symptoms
Past History and Systems Review
Patient has not explained any kind of past history of any recurrent episode of the same before, nor any other systematic involvement, and any other additional complaints. The patient is on Hymusa, Spondin Syrup and some other tablets of Homeopathy Medicines.
Examation
The patient presented to the out-patient department walking with the support of one of the attendants, presented with minor forward bending posture both in standing and sitting. rounded shoulder, with swelling present over the right side of the face and Cervical area. All the movements around the Cervical Spine, Upper Limbs, and lower Limbs measured with Goniometer following the procedures established by Norkin and White (2009) are painful at the end range during Active Range of Motion. Muscle Strength measured by MMT grading scale shows a good strength (4+) over the muscles around the lower Limb and Proximal muscles of Upper Limb, while the distal muscles around the wrist and Fingers shows grade (3+) strength. Sensory Examination, is conducted with the Fine Touch, Crude Touch, Vibration with Tunning Fork is tested along the dermatome of C4, C5, C6, C7, C8, T1 and T2 distribution. Sensation is intact, but the patient is having numbness and altered sensation (cold icing feeling over the plantar aspect of foot while touching the ground).
DTR checked with Knee Hammer of both the Upper Limb and Lower Limb is 4+ [Hyperactive, repeating reflex (Clonus) elicited over a tap] [8].
Special Tests
A positive Hoffman Sign with 0.31 (0.25–0.35) Sensitivity, 0.73 (0.59–0.84) Specificity and 4.9 (2.6–9.6) suggests upper motor neuron lesion and corticospinal weakness presumably due to cervical cord compression [1,9]. The gold standard for the diagnosis of cervical myelopathy is MRI. A 2015 study showed that positive cord signal improvements observed on the MRI were associated with 67% of those seen on the Hoffman sign [10].
Clinical Interpretation
Based on the result of the history and physical examination the patient showed evidence regarding the provisional diagnosis of Compression of the Spinal Nerve at Cervical region of C3, C4, C5, C6, C7. The Radiological Investigation (MRI) also showed positive findings for the same. In this study Pain on NPRS as a Primary outcome measure and SF-36 for Quality of Life, Gait on Functional Gait Assessment & Balance on Berg Balance Scale have been used in ruling out the consequences of the client and also the effect of Treatment (Levator Stretching) on the condition.
Intervention
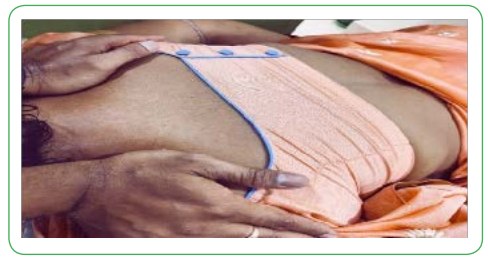
Participants were placed in the Prone Position with their head contralaterally rotated to the side of the shortened LS. Then the examiner pulls in cervical flexion with their own hand. An inferolateral force was applied by the examiner to the superior angle of the scapula on the side of shortened LS until that a “good stretch” had been achieved, without causing any discomfort [20]. As Cervical ROM increased by 5.9° after PP compared to baseline [19]. Holding stretches for 20 to 30 seconds is a good standard because most of the stress relaxation in passive stretches occurs in the first 20 seconds [17]. The client was treated 5 days per week, for 5 weeks, where, Levator muscle Stretching till the centralization of the radiating pain exclusively has been given till 1 week. Afterwards set of co ordination exercises, balance exercises advised along with patient education of don’ts like lifting any heavy weights, doing strenuous activities etc.
Outcome After the Sessions
After 25 sessions she reported reduction in pain, on NPRS scale (Sensitivity 71% & Specificity 81%) pain reduces from 9 to 4, able to walk with better stability assessed on FGA and reported a good Quality of Life on SF-36 (Sensitivity=84.4%, Specificity=93.9%).Discussion
Stretching helps in improving neuromuscular control & the establishes sensory Motor control over cervical spine. Studies have explained that Stretch training will decrease muscle stiffness, possibly even decrease the increases in muscular stiffness that results from strength training [18]. Initial changes those produced in stretching involves mechanical adaptation that are followed by neural adaptation.
A study states that stretching triggers release of neuroendocrine factor which brings sense of relaxation. Stretching can lead to functional adaptation of the nervous system which reduces central & Peripheral reflex activities & increase Pain tolerance (Weppler et.al. 2010) the lady in this case study has reported decrease in Pain, and has improvement in Balance and Quality of Life, after the whole session of the Levator Muscle Stretching. As per our knowledge there has been no studies described about the effect of the same.
Abnormal and noxious factors such as spasticity, immobilization, changes in fascial architectures etc. takes more time to produce a change. The manual stretching of Levator scapulae muscle also stretches the deep cervical fascia paravertebral layer covering it. Peripherally this mechanical force through mechano-transduction property of fascial tissue tends to modulate the nociceptive pathways and cell signalling through stimulation of mechano-receptors (Ruffini and paccini corpuscles) [11]. Stretching decreases the passive tension in the muscle at a given length. This decrease in passive tension in the muscle at a particular joint angle is due to stress relaxation. Stress relaxation is the decrease in stress (force per unit area) in a material elongated and held at a constant length [17]. Stretching creates an acute increase in joint range of motion that is related to an analgesic effect that allows the person to tolerate higher levels of passive tension required to stretch the muscle farther than it was before.
From all the Physical Examinations and Radiological Imaging along with other already done medical diagnosis, CM is highlighted, where Levator Muscle Stretching along with other conventional exercises have been proved to be helpful in reducing the symptoms and delaying the surgery for a certain period.
Conclusion
Cervical Myelopathy may be one of the most under-diagnosed serious conditions of the cervical spine in the Rehabilitation profession. It is of great importance to be aware of its presentation, signs and symptoms, and appropriately test these, as the condition in its more severe states can have serious consequences. This case demonstrates a typical presentation of cervical myelopathy, where stiffness, clumsiness and changes to gait are accompanied by upper motor neuron signs. This case a lady was treated over 25 sessions of Levator Muscle Stretching and Conventional Exercises has improvement in Pain and Quality of Life, suggesting that the surgical procedure can be avoided for a certain period of time.
What This Case Adds to the Evidence-Based Practice Beyond the Research Literature
This could be the first literature which can suggest that Patient with acute or sub-acute Cervical Myelopathy can improve with Pain and Quality of Life up to a certain extent, which can help the person in leading a better life and avoiding Surgery to an possible extent.
Acknowledgement
The authors thank Physical Therapist Debi Prasanna Samal and Physical Therapist Thiagarajan Subramanian for being such a wonderful Support, Guide and to be always willing to help.
Competing interests:
The authors declare that they have no competing interests.
References
Cook, C., Brown, C., Isaacs, R., Roman, M., Davis, S., & Richardson, W., (2010). Clustered clinical findings for diagnosis of cervical spine myelopathy. Journal of Manual & Manipulative Therapy. Dec 1;18(4):175-80.View
Edwards, II C.C., Riew, K.D., Anderson, P. A., Hilibrand, A.S., & Vaccaro, A.F. (2003). Cervical myelopathy: current diagnostic and treatment strategies. The Spine Journal. 1;3(1):68-81.View
Bridges, J., Sandoval, R. (2018). Clinical outcomes following conservative management of chronic traumatic cervical myelopathy: A case report. Physiotherapy theory and practice. 4;34(3):231-40.View
Barkoh, K., Ohiorhenuan, I. E., Lee, L., Lucas, J., Arakelyan, A., Ornelas, C., Buser, Z., Hsieh, P., Acosta, F., Liu, J., Wang, J. C. (2019). The DOWN Questionnaire: A Novel Screening Tool for Cervical Spondylotic Myelopathy. Global spine journal. 2019 Sep;9(6):607-12.View
Walker, H. K. (1990). Deep tendon reflexes. InClinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Butterworths.View
Edwards, II C.C., Riew, K. D., Anderson, P. A., Hilibrand, A. S., & Vaccaro, A. F. (2003). Cervical myelopathy: current diagnostic and treatment strategies. The Spine Journal. 1;3(1):68-81.View
Bridges, J., Sandoval, R. (2018). Clinical outcomes following conservative management of chronic traumatic cervical myelopathy: A case report. Physiotherapy theory and practice. 4;34(3):231-40.View
O'Doherty, L. J., Hickey, A., Hardiman, O. (2010). Measuring life quality, physical function and psychological well-being in neurological illness. Amyotrophic Lateral Sclerosis. 1;11(5):461-8.View
Cao, J., Liu, Y., Wang, Y., Zhao L, Wang W, Zhang M, Wang L. A (2019). Clinical Correlation Research of the Hoffmann Sign and Neurological Imaging Findings in Cervical Spinal Cord Compression. World neurosurgery. 1;128:e782-6.
Nemani, V. M., Kim, H. J., Piyaskulkaew, C., Nguyen, J. T., Riew, K.D., (2015). Correlation of cord signal change with physical examination findings in patients with cervical myelopathy. Spine. 1;40(1):6-10.View
Mohanty P. Myofacial Release for the Management of Cervical Compressive Myelopathy–Case Study. Japan Journal of Clinical & Medical Research. SRC/JJCMR-105. DOI: https:// doi. org/10.47363/JJCMR/2021 (1). 2021;105:2-5.View
Kong, L. D., Meng, L. C., Wang, L. F., Shen, Y., Wang, P., Shang, Z. K. (2013). Evaluation of conservative treatment and timing of surgical intervention for mild forms of cervical spondylotic myelopathy. Experimental and Therapeutic Medicine. 1;6(3):852-6.
Cook, C., Roman, M., Stewart, K. M., Leithe, L. G., Isaacs, R. (2009). Reliability and diagnostic accuracy of clinical special tests for myelopathy in patients seen for cervical dysfunction. journal of orthopaedic & sports physical therapy. 39(3):172-8.View
Pessini Ferreira, L. M., Auger, C., Kortazar Zubizarreta, I., Gonzalez Chinchon, G., Herrera, I., Pla, A., de Barros, A., Tortajada, C., Rovira, A. (2021). MRI findings in cervical spondylotic myelopathy with gadolinium enhancement: Review of seven cases. BJR| case reports. 7(2):20200133.View
Sah, S., Wang, L., Dahal, M., Acharya, P. (2012). Surgical management of cervical spondylotic myelopathy. Journal of Nepal Medical Association. 52(188).View
Taylor, D. C., Dalton JR J. D., Seaber, A. V., Garrett, J. R. WE. (1990). Viscoelastic properties of muscle-tendon units: the biomechanical effects of stretching. The American journal of sports medicine. 18(3):300-9View
Sah, S., Wang, L., Dahal, M., Acharya, P. (2012). Surgical management of cervical spondylotic myelopathy. Journal of Nepal Medical Association. 52(188).View
Knudson, D. (2006). The biomechanics of stretching. Journal of Exercise Science and Physiotherapy. 2:3-12.View
Bandy, W. D., Irion, J. M., Briggler, M. (1997). The effect of time and frequency of static stretching on flexibility of the hamstring muscles. Physical therapy. 1;77(10):1090-6.View
Jeong, H. J., Cynn, H. S., Yi, C. H., Yoon, J. W., Lee, J. H., Yoon, T. L., Kim, B. B. (2017). Stretching position can affect levator scapular muscle activity, length, and cervical range of motion in people with a shortened levator scapulae. Physical Therapy in Sport. 1;26:13-9.View