Abstract
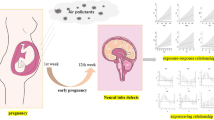
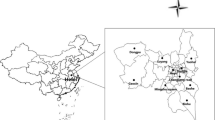
Current studies on air pollutant exposure during pregnancy and orofacial clefts (OFCs) have inconsistent results, and few studies have investigated refined susceptible windows for OFCs. We aim to estimate association between air pollution and OFCs during the first trimester of pregnancy and identify specific susceptible windows. Birth data was obtained from Birth Defects Surveillance Network in Lanzhou from 2014 to 2019. Air pollution data and temperature data were obtained from ambient air monitoring stations and China Meteorological Data Network, respectively. A distribution lag nonlinear model (DLNM) was applied to estimate weekly-exposure-lag-response association between air pollutant levels and OFCs. The study included 320,787 perinatal infants from 2014 to 2019, of which 685 (2.14‰) were OFCs. The results demonstrated that exposure of pregnant women to aerodynamic diameter ≤ 10 μm (PM10) at lag 4–5 weeks was significantly associated with the risk of OFCs, with the greatest impact at the lag 4 week (RR = 1.029, 95% CI = 1.001–1.057). Exposure to sulfur dioxide (SO2) at lag 2–4 weeks was significantly associated with the risk of OFCs, with the greatest impact at the lag 3 week (RR = 1.096, 95% CI = 1.041–1.177). This study provides further evidence that exposure to air pollution increases the risk of OFCs in the first trimester of pregnancy.




Similar content being viewed by others
Data availability
Not applicable.
References
Buser MC, Pohl HR (2015) Windows of sensitivity to toxic chemicals in the development of cleft palates. J Toxicol Env Heal B 18(5):242–257. https://doi.org/10.1080/10937404.2015.1068719
Erickson AC, Arbour L (2014) The shared pathoetiological effects of particulate air pollution and the social environment on fetal-placental development. J Environ Public Health 2014:901017. https://doi.org/10.1155/2014/901017
Estarlich M, Ballester F, Aguilera I, Fernandez-Somoano A, Lertxundi A, Llop S, Freire C, Tardon A, Basterrechea M, Sunyer J, Iniguez C (2011) Residential exposure to outdoor air pollution during pregnancy and anthropometric measures at birth in a multicenter cohort in Spain. Environ Health Perspect 119(9):1333–1338. https://doi.org/10.1289/ehp.1002918
Fan D, Wu S, Liu L, Xia Q, Tian G, Wang W, Ye S, Wang L, Rao J, Yang X, Yu Z, Xin L, Li S, Duan Z, Zhang T, Wu S, Guo X, Liu Z (2018) Prevalence of non-syndromic orofacial clefts: based on 15,094,978 Chinese perinatal infants. Oncotarget 9(17):13981–13990. https://doi.org/10.18632/oncotarget.24238
Garland MA, Reynolds K, Zhou CJ (2020) Environmental mechanisms of orofacial clefts. Birth Defects Res 112(19):1660–1698. https://doi.org/10.1002/bdr2.1830
Gasparrini A (2011) Distributed Lag linear and non-linear models in R: The Package dlnm. J Stat Softw 43(8):1–20. https://doi.org/10.18637/jss.v043.i08
Gilboa SM, Mendola P, Olshan AF, Langlois PH, Savitz DA, Loomis D, Herring AH, Fixler DE (2005) Relation between ambient air quality and selected birth defects, seven county study, Texas, 1997–2000. Am J Epidemiol 162(3):238–252. https://doi.org/10.1093/aje/kwi189
Girguis MS, Strickland MJ, Hu XF, Liu Y, Bartell SM, Vieira VM (2016) Maternal exposure to traffic-related air pollution and birth defects in Massachusetts. Environ Res 146:1–9. https://doi.org/10.1016/j.envres.2015.12.010
Ha S, Hu H, Roussos-Ross D, Kan HD, Roth J, Xu XH (2014) The effects of air pollution on adverse birth outcomes. Environ Res 134:198–204. https://doi.org/10.1016/j.envres.2014.08.002
Hansen CA, Barnett AG, Jalaludin BB, Morgan GG (2009) Ambient air pollution and birth defects in Brisbane, Australia. Plos One 4(4):e5408. https://doi.org/10.1371/journal.pone.0005408
Hao JW, Peng L, Cheng P, Li S, Zhang C, Fu WN, Dou LJ, Yang F, Hao JH (2021) A time series analysis of ambient air pollution and low birth weight in Xuzhou, China. Int J Environ Health Res 32(6):1238–1247. https://doi.org/10.1080/09603123.2020.1867828
Hwang BF, Jaakkola JJK (2008) Ozone and other air pollutants and the risk of oral clefts. Environ Health Perspect 116(10):1411–1415. https://doi.org/10.1289/ehp.11311
Ji Y, Garland MA, Sun B, Zhang SW, Reynolds K, McMahon M, Rajakumar R, Islam MS, Liu Y, Chen YP, Zhou CJJ (2020) cellular and developmental basis of orofacial clefts. Birth Defects Res 112(19):1558–1587. https://doi.org/10.1002/bdr2.1768
Li S, Peng L, Wu XC, Xu G, Cheng P, Hao JW, Huang ZH, Xu M, Chen ST, Zhang C, Hao JH (2021) Long-term impact of ambient air pollution on preterm birth in Xuzhou, China: a time series study. Environ Sci Pollut Res Int 28(30):41039–41050. https://doi.org/10.1007/s11356-021-13621-2
Liu FH, Dai HX, Gong TT, Zhang JY, Li J, Chen ZJ, Li LL, Chen YL, Liu S, Jiang CZ, Huang YH, Zhao YH, Wu QJ (2020) Maternal preconception and first trimester exposure to PM(10) and the risk of oral clefts in offspring: a population-based, case-control study. Occup Environ Med 77(10):721–727. https://doi.org/10.1136/oemed-2020-106434
Liu YR, Dong JY, Zhai GY (2021) Association between air pollution and hospital admissions for hypertension in Lanzhou, China. Environ Sci Pollut Res Int 29(8):11976–11989. https://doi.org/10.1007/s11356-021-16577-5
Marshall EG, Harris G, Wartenberg D (2010) Oral cleft defects and maternal exposure to ambient air pollutants in New Jersey. Birth Defects Res A Clin Mol Teratol 88(4):205–215. https://doi.org/10.1002/bdra.20650
Martinelli M, Palmieri A, Carinci F, Scapoli L (2020) Non-syndromic cleft palate: an overview on human genetic and environmental risk factors. Front Cell Dev Biol 8:592271. https://doi.org/10.3389/fcell.2020.592271
Meng ZQ (2003) Oxidative damage of sulfur dioxide on various organs of mice: sulfur dioxide is a systemic oxidative damage agent. Inhalation Toxicol 15(2):181–195. https://doi.org/10.1080/08958370304476
Nasreddine G, El Hajj J, Ghassibe-Sabbagh M (2021) Orofacial clefts embryology, classification, epidemiology, and genetics. Mutat Res-Rev Mutat 787:108373. https://doi.org/10.1016/j.mrrev.2021.108373
Niu ZC, Qi YJ, Zhao PQ, Li YD, Tao Y, Peng L, Qiao ML (2021) Short-term effects of ambient air pollution and meteorological factors on tuberculosis in semi-arid area, northwest China: a case study in Lanzhou. Environ Sci Pollut Res Int 28(48):69190–69199. https://doi.org/10.1007/s11356-021-15445-6
Risom L, Moller P, Loft S (2005) Oxidative stress-induced DNA damage by particulate air pollution. Mutat Res 592(1-2):119–137. https://doi.org/10.1016/j.mrfmmm.2005.06.012
Ritz B, Yu F, Fruin S, Chapa G, Shaw GM, Harris JA (2002) Ambient air pollution and risk of birth defects in southern California. Am J Epidemiol 155(1):17–25. https://doi.org/10.1093/aje/155.1.17
Saenen ND, Plusquin M, Bijnens E, Janssen BG, Gyselaers W, Cox B, Fierens F, Molenberghs G, Penders J, Vrijens K, De Boever P, Nawrot TS (2015) In utero fine particle air pollution and placental expression of genes in the brain-derived neurotrophic factor signaling pathway: an ENVIRONAGE birth cohort study. Environ Health Perspect 123(8):834–840. https://doi.org/10.1289/ehp.1408549
Salavati N, Strak M, Burgerhof JGM, de Walle HEK, Erwich JJHM, Bakker MK (2018) The association of air pollution with congenital anomalies: an exploratory study in the northern Netherlands. Int J Hyg Environ Health 221(7):1061–1067. https://doi.org/10.1016/j.ijheh.2018.07.008
Sun S, Zhang Q, Sui XM, Ding L, Liu J, Yang M, Zhao QH, Zhang C, Hao JH, Zhang XJ, Lin SL, Ding R, Cao JY (2021) Associations between air pollution exposure and birth defects: a time series analysis. Environ Geochem Health 43(11):4379–4394. https://doi.org/10.1007/s10653-021-00886-2
Wang LL, Xiang XM, Mi BB, Song H, Dong M, Zhang SP, Bi YX, Zhao YL, Li Q, Zhang Q, Zhang L, Yan H, Wang DL, Dang SN (2019) Association between early prenatal exposure to ambient air pollution and birth defects: evidence from newborns in Xi’an, China. J Public Health-Uk 41(3):494–501. https://doi.org/10.1093/pubmed/fdy137
Wang F, Shi CR, Dong JY, Nie H (2021) Association between ambient temperature and atopic dermatitis in Lanzhou, China: a time series analysis. Environ Sci Pollut Res Int 28(47):67487–67495. https://doi.org/10.1007/s11356-021-15198-2
Wehby GL, Cassell CH (2010) The impact of orofacial clefts on quality of life and healthcare use and costs. Oral Dis 16(1):3–10. https://doi.org/10.1111/j.1601-0825.2009.01588.x
Wu TT, Ma Y, Wu X, Bai M, Peng Y, Cai WT, Wang YX, Zhao J, Zhang Z (2019) Association between particulate matter air pollution and cardiovascular disease mortality in Lanzhou, China. Environ Sci Pollut Res Int 26(15):15262–15272. https://doi.org/10.1007/s11356-019-04742-w
Xiong LL, Xu ZH, Wang H, Liu ZY, Xie DH, Wang AH, Kong FJ (2019) The association between ambient air pollution and birth defects in four cities in Hunan province, China, from 2014 to 2016. Medicine 98(4):e14253. https://doi.org/10.1097/MD.0000000000014253
Yitshak-Sade M, Kloog I, Schwartz JD, Novack V, Erez O, Just AC (2021) The effect of prenatal temperature and PM2.5 exposure on birthweight: weekly windows of exposure throughout the pregnancy. Environ Int 155:106588. https://doi.org/10.1016/j.envint.2021.106588
Zhang Q, Sun S, Sui XM, Ding L, Yang M, Li CL, Zhang C, Zhang XJ, Hao JH, Xu YC, Lin SL, Ding R, Cao JY (2021) Associations between weekly air pollution exposure and congenital heart disease. Sci Total Environ 757:143821. https://doi.org/10.1016/j.scitotenv.2020.143821
Zhao JZ, Zhang B, Yang SP, Mei H, Qian ZM, Liang SW, Zhang YM, Hu K, Tan YF, Xian H, Belue R, Jordan SS, Xu SQ, Zheng TZ, Du YK (2018) Maternal exposure to ambient air pollutant and risk of oral clefts in Wuhan, China. Environ Pollut 238:624–630. https://doi.org/10.1016/j.envpol.2018.03.053
Zhou Y, Gilboa SM, Herdt ML, Lupo PJ, Flanders WD, Liu Y, Shin M, Canfield MA, Kirby RS (2017) Maternal exposure to ozone and PM2.5 and the prevalence of orofacial clefts in four U.S. states. Environ Res 153:35–40. https://doi.org/10.1016/j.envres.2016.11.007
Zhu YY, Zhang CL, Liu DP, Grantz KL, Wallace M, Mendola P (2015) Maternal ambient air pollution exposure preconception and during early gestation and offspring congenital orofacial defects. Environ Res 140:714–720. https://doi.org/10.1016/j.envres.2015.06.002
Zhu S, Xia L, Wu J, Chen S, Chen F, Zeng F, Chen X, Chen C, Xia Y, Zhao X, Zhang J (2018) Ambient air pollutants are associated with newly diagnosed tuberculosis: a time-series study in Chengdu, China. Sci Total Environ 631–632:47–55. https://doi.org/10.1016/j.scitotenv.2018.03.017
Funding
This work was supported by Lanzhou Talents Innovation and entrepreneurship Project (2019-RC-25) and the Lanzhou Chengguan District Science and Technology Project (2020–2-11–13).
Author information
Authors and Affiliations
Contributions
Conceptualization: NC, Y-NB, and Y-JY. Data collection: LZ, LP, Y-PB, R-JW, and Y-BH. Data cleaning and discrepancy checks: NC and LZ. Analytic strategy: Y-JY, Y-YL. Analysis and interpretation of data: Y-YL, LZ, W-LZ, and X-YR. Manuscript preparation: Y-YL, LZ, and NC. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The research was approved by the Lanzhou Maternal and Child Health Care Hospital.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, Y., Zhou, L., Zhang, W. et al. Time series analysis on association between ambient air pollutants and orofacial clefts during pregnancy in Lanzhou, China. Environ Sci Pollut Res 29, 72898–72907 (2022). https://doi.org/10.1007/s11356-022-19855-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-022-19855-y