Abstract
Objectives
The stabilization of the transcription factor and prognostic tumor marker hypoxia-inducible factor 1α (HIF1α) is considered to be crucial for cellular metabolic adaptations to hypoxia. However, HIF1α has also been shown to accumulate under normoxic conditions, although this phenomenon is poorly understood.
Methods
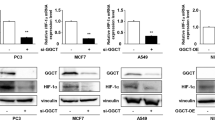
We investigated the conditions for normoxic HIF1α stabilization in different tumor cell lines (e.g., two mammary carcinoma cell lines and three oral squamous cell carcinoma cell lines) via Western blot analysis or immunohistochemical staining. The transcriptional activity of HIF1 was demonstrated by analyzing the messenger RNA (mRNA) expression of the HIF1 target carbonic anhydrase 9 (CA9) via PCR.
Results
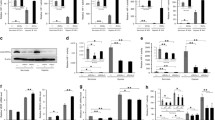
Our data demonstrate that the combined incubation of tumor cells with glutamine and growth factors (e.g., EGF, insulin, and serum) mediates the normoxic accumulation of HIF1α in vitro. Consequently, the inhibition of glutaminolysis by a glutaminase inhibitor blocked the normoxic accumulation of HIF1α. Additionally, the normoxic HIF1α protein displayed nuclear translocation and transcriptional activity, which was confirmed by the induction of CA9 mRNA expression. Furthermore, the normoxic accumulation of HIF1α was associated with impaired proliferation of tumor cells. Finally, ammonia, the toxic waste product of glutaminolysis, induced a normoxic accumulation of HIF1α to the same extent as glutamine.
Conclusion
Our study suggests that HIF1α is involved in the regulation of glutamine metabolism and the cellular levels of the toxic metabolic waste product ammonia under normoxia. Hence, our results, together with data presented in the literature, support the hypothesis that HIF1α and its target genes play a crucial role in metabolic pathways, such as glutaminolysis and glycolysis, under both hypoxic and normoxic conditions.
Clinical relevance
Therefore, the inhibition of HIF1α (and/or HIF1α target genes) could emerge as a promising therapeutic approach that would result in the accumulation of toxic metabolic waste products in tumor cells as well as the reduction of their nutrition and energy supply.





Similar content being viewed by others
References
Semenza GL (2009) Regulation of cancer cell metabolism by hypoxia-inducible factor 1. Semin Cancer Biol 19(1):12–16. doi:10.1016/j.semcancer.2008.11.009
Semenza GL (2010) HIF-1: upstream and downstream of cancer metabolism. Curr Opin Genet Dev 20(1):51–56. doi:10.1016/j.gde.2009.10.009
Vander Heiden MG, Cantley LC, Thompson CB (2009) Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science 324(5930):1029–1033. doi:10.1126/science.1160809
Koppenol WH, Bounds PL, Dang CV (2011) Otto Warburg’s contributions to current concepts of cancer metabolism. Nat Rev Cancer 11(5):325–337. doi:10.1038/nrc3038
DeBerardinis RJ, Lum JJ, Hatzivassiliou G, et al. (2008) The biology of cancer: metabolic reprogramming fuels cell growth and proliferation. Cell Metab 7(1):11–20. doi:10.1016/j.cmet.2007.10.002
Miller AL (1999) Therapeutic considerations of L-glutamine: a review of the literature. Altern Med Rev 4(4):239–248
Dang CV (2010) Glutaminolysis: supplying carbon or nitrogen or both for cancer cells? Cell Cycle 9(19):3884–3886. doi:10.4161/cc.9.19.13302
Dang CV, Hamaker M, Sun P, et al. (2011) Therapeutic targeting of cancer cell metabolism. J Mol Med 89(3):205–212. doi:10.1007/s00109-011-0730-x
Dang CV (2010) Rethinking the Warburg effect with Myc micromanaging glutamine metabolism. Cancer Res 70(3):859–862. doi:10.1158/0008-5472.CAN-09-3556
Smolková K, Bellance N, Scandurra F, et al. (2010) Mitochondrial bioenergetic adaptations of breast cancer cells to aglycemia and hypoxia. J Bioenerg Biomembr 42(1):55–67. doi:10.1007/s10863-009-9267-x
Smolková K, Plecitá-Hlavatá L, Bellance N, et al. (2011) Waves of gene regulation suppress and then restore oxidative phosphorylation in cancer cells. Int J Biochem Cell Biol 43(7):950–968. doi:10.1016/j.biocel.2010.05.003
Fendt S, Bell EL, Keibler MA, et al. (2013) Reductive glutamine metabolism is a function of the α-ketoglutarate to citrate ratio in cells. Nat Commun 4:2236. doi:10.1038/ncomms3236
Epstein AC, Gleadle JM, McNeill LA, et al. (2001) C. elegans EGL-9 and mammalian homologs define a family of dioxygenases that regulate HIF by prolyl hydroxylation//C. elegans EGL-9 and mammalian homologs define a family of dioxygenases that regulate HIF by prolyl hydroxylation. Cell 107(1):43–54. doi:10.1016/S0092-8674(01)00507-4
Ivan M, Kondo K, Yang H, et al. (2001) HIFalpha targeted for VHL-mediated destruction by proline hydroxylation: implications for O2 sensing. Science 292(5516):464–468. doi:10.1126/science.1059817
Semenza GL (2003) Targeting HIF-1 for cancer therapy. Nat Rev Cancer 3(10):721–732. doi:10.1038/nrc1187
Semenza GL (2012) Hypoxia-inducible factors in physiology and medicine. Cell 148(3):399–408. doi:10.1016/j.cell.2012.01.021
Kappler M, Taubert H, Holzhausen H, et al. (2008) Immunohistochemical detection of HIF-1α and CAIX in advanced head-and-neck cancer. Strahlenther Onkol 184(8):393–399. doi:10.1007/s00066-008-1813-7
Bache M, Kappler M, Said HM, et al. (2008) Detection and specific targeting of hypoxic regions within solid tumors: current preclinical and clinical strategies. Curr Med Chem 15(4):322–338. doi:10.2174/092986708783497391#sthash.igXXfwmp.dpuf
Eckert AW, Lautner MHW, Schütze A, et al. (2010) Co-expression of Hif1alpha and CAIX is associated with poor prognosis in oral squamous cell carcinoma patients. J Oral Pathol Med 39(4):313–317. doi:10.1111/j.1600-0714.2009.00829.x
Eckert AW, Lautner MHW, Schütze A, et al. (2011) Coexpression of hypoxia-inducible factor-1α and glucose transporter-1 is associated with poor prognosis in oral squamous cell carcinoma patients. Histopathology 58(7):1136–1147. doi:10.1111/j.1365-2559.2011.03806.x
Vaupel P, Mayer A (2007) Hypoxia in cancer: significance and impact on clinical outcome. Cancer Metastasis Rev 26(2):225–239. doi:10.1007/s10555-007-9055-1
Zhang H, Bosch-Marce M, Shimoda LA, et al. (2008) Mitochondrial autophagy is an HIF-1-dependent adaptive metabolic response to hypoxia. J Biol Chem 283(16):10892–10903. doi:10.1074/jbc.M800102200
Koivunen P, Hirsilä M, Remes AM, et al. (2007) Inhibition of hypoxia-inducible factor (HIF) hydroxylases by citric acid cycle intermediates: possible links between cell metabolism and stabilization of HIF. J Biol Chem 282(7):4524–4532. doi:10.1074/jbc.M610415200
King A, Selak MA, Gottlieb E (2006) Succinate dehydrogenase and fumarate hydratase: linking mitochondrial dysfunction and cancer. Oncogene 25(34):4675–4682. doi:10.1038/sj.onc.1209594
Ashrafian H, O’Flaherty L, Adam J, et al. (2010) Expression profiling in progressive stages of fumarate-hydratase deficiency: the contribution of metabolic changes to tumorigenesis. Cancer Res 70(22):9153–9165. doi:10.1158/0008-5472.CAN-10-1949
Kwon SJ, Lee YJ (2005) Effect of low glutamine/glucose on hypoxia-induced elevation of hypoxia-inducible factor-1alpha in human pancreatic cancer MiaPaCa-2 and human prostatic cancer DU-145 cells. Clin Cancer Res 11(13):4694–4700. doi:10.1158/1078-0432.CCR-04-2530
Vordermark D, Kraft P, Katzer A, et al. (2005) Glucose requirement for hypoxic accumulation of hypoxia-inducible factor-1alpha (HIF-1alpha). Cancer Lett 230(1):122–133. doi:10.1016/j.canlet.2004.12.040
Zundel W, Schindler C, Haas-Kogan D, et al. (2000) Loss of PTEN facilitates HIF-1-mediated gene expression. Genes Dev 14(4):391–396
Peng X, Karna P, Cao Z, et al. (2006) Cross-talk between epidermal growth factor receptor and hypoxia-inducible factor-1alpha signal pathways increases resistance to apoptosis by up-regulating survivin gene expression. J Biol Chem 281(36):25903–25914. doi:10.1074/jbc.M603414200
Wang L, Zhou W, Gou S, et al. (2010) Insulin promotes proliferative vitality and invasive capability of pancreatic cancer cells via hypoxia-inducible factor 1alpha pathway. J Huazhong Univ Sci Technol Med Sci 30(3):349–353. doi:10.1007/s11596-010-0355-2
Blancher C, Moore JW, Robertson N, et al. (2001) Effects of ras and von Hippel-Lindau (VHL) gene mutations on hypoxia-inducible factor (HIF)-1alpha, HIF-2alpha, and vascular endothelial growth factor expression and their regulation by the phosphatidylinositol 3′-kinase/Akt signaling pathway. Cancer Res 61(19):7349–7355
Dayan F, Bilton RL, Laferrière J, et al. (2009) Activation of HIF-1alpha in exponentially growing cells via hypoxic stimulation is independent of the Akt/mTOR pathway. J Cell Physiol 218(1):167–174. doi:10.1002/jcp.21584
Mayer A, Höckel M, Vaupel P (2008) Endogenous hypoxia markers: case not proven! Adv Exp Med Biol 614(614):127–136. doi:10.1007/978-0-387-74911-2_15
Hernandez VJ, Weng J, Ly P, et al. (2013) Cavin-3 dictates the balance between ERK and Akt signaling. Elife 2:e00905. doi:10.7554/elife.00905
Parks SK, Chiche J, Pouysségur J (2013) Disrupting proton dynamics and energy metabolism for cancer therapy. Nat Rev Cancer 13(9):611–623. doi:10.1038/nrc3579
Kappler M, Taubert H, Eckert AW (2011) Oxygen sensing, homeostasis, and disease. N Engl J Med (365):1845–1846. doi:10.1056/NEJMc1110602#SA2
Kappler M, Taubert H, Schubert J, et al. (2012) The real face of HIF1α in the tumor process. Cell Cycle 11(21):3932–3936. doi:10.4161/cc.21854
Griffiths JR, McSheehy PMJ, Robinson SP, et al. (2002) Metabolic changes detected by in vivo magnetic resonance studies of HEPA-1 wild-type tumors and tumors deficient in hypoxia-inducible factor-1beta (HIF-1beta): evidence of an anabolic role for the HIF-1 pathway. Cancer Res 62(3):688–695
Lu H, Forbes RA, Verma A (2002) Hypoxia-inducible factor 1 activation by aerobic glycolysis implicates the Warburg effect in carcinogenesis. J Biol Chem 277(26):23111–23115. doi:10.1074/jbc.M202487200
Lu H, Dalgard CL, Mohyeldin A, et al. (2005) Reversible inactivation of HIF-1 prolyl hydroxylases allows cell metabolism to control basal HIF-1. J Biol Chem 280(51):41928–41939. doi:10.1074/jbc.M508718200
Semenza GL (2013) HIF-1 mediates metabolic responses to intratumoral hypoxia and oncogenic mutations. J Clin Invest 123(9):3664–3671. doi:10.1172/JCI67230
Sun RC, Denko NC (2014) Hypoxic regulation of glutamine metabolism through HIF1 and SIAH2 supports lipid synthesis that is necessary for tumor growth. Cell Metab 19(2):285–292. doi:10.1016/j.cmet.2013.11.022
Tallis S, Caltana LR, Souto PA, et al. (2014) Changes in CNS cells in hyperammonemic portal hypertensive rats. J Neurochem 128(3):431–444. doi:10.1111/jnc.12458
Hobiger G (1996) Ammoniak in Wasser: Ableitung einer Formel zur Berechnung von Ammoniak in wäßrigen Lösungen. Berichte/Umweltbundesamt, Umweltbundesamt, Wien
Denko NC (2008) Hypoxia, HIF1 and glucose metabolism in the solid tumour. Nat Rev Cancer 8(9):705–713. doi:10.1038/nrc2468
DeBerardinis RJ, Mancuso A, Daikhin E, et al. (2007) Beyond aerobic glycolysis: transformed cells can engage in glutamine metabolism that exceeds the requirement for protein and nucleotide synthesis. Proc Natl Acad Sci U S A 104(49):19345–19350. doi:10.1073/pnas.0709747104
Feron O (2009) Pyruvate into lactate and back: from the Warburg effect to symbiotic energy fuel exchange in cancer cells. Radiother Oncol 92(3):329–333. doi:10.1016/j.radonc.2009.06.025
Meng M, Chen S, Lao T, et al. (2010) Nitrogen anabolism underlies the importance of glutaminolysis in proliferating cells. Cell Cycle 9(19):3921–3932. doi:10.4161/cc.9.19.13139
Ward PS, Thompson CB (2012) Metabolic reprogramming: a cancer hallmark even Warburg did not anticipate. Cancer Cell 21(3):297–308. doi:10.1016/j.ccr.2012.02.014
Demidenko ZN, Blagosklonny MV (2014) The purpose of the HIF-1/PHD feedback loop: to limit mTOR-induced HIF-1α. Cell Cycle 10(10):1557–1562. doi:10.4161/cc.10.10.15789
Wise DR, Thompson CB (2010) Glutamine addiction: a new therapeutic target in cancer. Trends Biochem. Sci. 35(8):427–433. doi:10.1016/j.tibs.2010.05.003
Shanware NP, Bray K, Eng CH, et al. (2014) Glutamine deprivation stimulates mTOR-JNK-dependent chemokine secretion. Nat Commun 5:4900. doi:10.1038/ncomms5900
Stiehl DP, Jelkmann W, Wenger RH, et al. (2002) Normoxic induction of the hypoxia-inducible factor 1alpha by insulin and interleukin-1beta involves the phosphatidylinositol 3-kinase pathway. FEBS Lett 512(1–3):157–162
Hernández-Bedolla MA, Carretero-Ortega J, Valadez-Sánchez M, et al. (2015) Chemotactic and proangiogenic role of calcium sensing receptor is linked to secretion of multiple cytokines and growth factors in breast cancer MDA-MB-231 cells. Biochim Biophys Acta 1853(1):166–182. doi:10.1016/j.bbamcr.2014.10.011
McQueen A, Bailey JE (1990) Effect of ammonium ion and extracellular pH on hybridoma cell metabolism and antibody production. Biotechnol Bioeng 35(11):1067–1077. doi:10.1002/bit.260351102
Ferreira TB, Carrondo MJT, Alves PM (2007) Effect of ammonia production on intracellular pH: consequent effect on adenovirus vector production. J Biotechnol 129(3):433–438. doi:10.1016/j.jbiotec.2007.01.010
Chiche J, Brahimi-Horn MC, Pouysségur J (2010) Tumour hypoxia induces a metabolic shift causing acidosis: a common feature in cancer. J Cell Mol Med 14(4):771–794. doi:10.1111/j.1582-4934.2009.00994.x
Trivedi B, Danforth WH (1966) Effect of pH on the kinetics of frog muscle phosphofructokinase. J Biol Chem 241(17):4110–4112
Yu Z, Persson H, Eaton JW, et al. (2003) Intralysosomal iron: a major determinant of oxidant-induced cell death. Free Radic Biol Med 34(10):1243–1252. doi:10.1016/S0891-5849(03)00109-6
Brahimi-Horn MC, Bellot G, Pouysségur J (2011) Hypoxia and energetic tumour metabolism. Curr Opin Genet Dev 21(1):67–72. doi:10.1016/j.gde.2010.10.006
Parks SK, Chiche J, Pouyssegur J (2011) pH control mechanisms of tumor survival and growth. J Cell Physiol 226(2):299–308. doi:10.1002/jcp.22400
Parks SK, Mazure NM, Counillon L, et al. (2013) Hypoxia promotes tumor cell survival in acidic conditions by preserving ATP levels. J Cell Physiol 228(9):1854–1862. doi:10.1002/jcp.24346
Chiche J, Le Fur Y, Vilmen C, et al. (2012) In vivo pH in metabolic-defective ras-transformed fibroblast tumors: key role of the monocarboxylate transporter, MCT4, for inducing an alkaline intracellular pH. Int J Cancer 130(7):1511–1520. doi:10.1002/ijc.26125
Fang JS, Gillies RD, Gatenby RA (2008) Adaptation to hypoxia and acidosis in carcinogenesis and tumor progression. Semin Cancer Biol 18(5):330–337. doi:10.1016/j.semcancer.2008.03.011
Kroemer G, Pouyssegur J (2008) Tumor cell metabolism: cancer’s Achilles’ heel. Cancer Cell 13(6):472–482. doi:10.1016/j.ccr.2008.05.005
Warburg O (1956) On respiratory impairment in cancer cells. Science 124(3215):269–270
Kappler M, Rot S, Taubert H, et al. (2007) The effects of knockdown of wild-type survivin, survivin-2B or survivin-3 on the radiosensitization in a soft tissue sarcoma cells in vitro under different oxygen conditions. Cancer Gene Ther 994–1001. doi:10.1038/sj.cgt.7701090
Kappler M, Bache M, Bartel F, et al. (2004) Knockdown of survivin expression by small interfering RNA reduces the clonogenic survival of human sarcoma cell lines independently of p53. Cancer Gene Ther 11(3):186–193. doi:10.1038/sj.cgt.7700677
Acknowledgments
We thank our colleagues from the Department of Oral and Maxillofacial Plastic Surgery and the Department of Radiotherapy for their continuous support. We thank S. Hanke and Dr. T. Klapperstück for assistance in cell cycle analysis. We would like to thank NPGLE Support Team (Pamela F, Jacqueline C., Man-Tsuey T. and Leann B., Briana V., Denise R.) for providing English language editing for our manuscript. M.K. was supported by the Wilhelm-Roux-Programm of BMBF/NBL3 (FKZ: 21/25, 24/19, 27/22).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of interest
The authors declare that they have no competing interests.
Funding
The work was supported by the Wilhelm-Roux-Programm of BMBF/NBL3 (FKZ: 21/25, 24/19, 27/22).
Informed consent
For this type of study, formal consent was not required.
Additional information
Matthias Kappler, Ulrike Pabst, Dirk Vordermark, and Alexander W. Eckert contributed equally to this work.
Rights and permissions
About this article
Cite this article
Kappler, M., Pabst, U., Rot, S. et al. Normoxic accumulation of HIF1α is associated with glutaminolysis. Clin Oral Invest 21, 211–224 (2017). https://doi.org/10.1007/s00784-016-1780-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-016-1780-9