Abstract
Purpose
Adolescent and young adult (AYA) head and neck (H&N) cancer survivors are at risk of long-term complications. A cross-sectional study of survivors recalled for clinical evaluation was performed to evaluate late effects in this population.
Methods
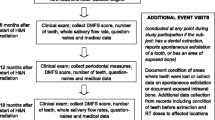
Surviving patients who had been diagnosed with H&N cancer between the ages of 15 and 39 years and treated with radiation therapy (RT) in British Columbia between 1970 and 2010 were invited to participate in this study. Survivors were assessed in consultation by a radiation oncologist for a complete history and physical exam. Comprehensive data collection of subjective and objective late effects of RT and screening investigations were completed.
Results
Of 36 AYA H&N participants, the majority were female (61%), and the most common tumour sites were thyroid (28%), oropharynx (17%), salivary gland (14%) and larynx (14%). Dental extractions post treatment was performed for 33% and dental implants for 17%. The majority (72%) reported xerostomia, 50% had dysphagia to solids and 25% hearing loss. Of the non-thyroid cancer patients who underwent RT to their neck, 45% developed hypothyroidism. There were 28% of participants with asymptomatic carotid stenosis and 27% with thyroid nodules; all were diagnosed after recall screening.
Conclusions
Survivors of AYA H&N cancer treated with RT reported numerous long-term complications. Comprehensive follow-up and screening guidelines should be established for this at-risk population.
Implications for Cancer Survivors
AYA H&N cancer survivors and their primary care practitioners should be educated on screening recommendations and the risk of late effects.


Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
Hammerlid E, Taft C. Health-related quality of life in long-term head and neck cancer survivors: A comparison with general population norms. Br J Cancer. 2001;84(2):149–56. https://doi.org/10.1054/bjoc.2000.1576.
C. O. Group. Long-term follow-up guidelines for survivors of childhood, adolescent, and young adult cancers long-term follow-up guidelines for survivors of childhood, adolescent, and young adult cancer children’s oncology group, 2013.
Hamilton SN, et al. Documentation and incidence of late effects and screening recommendations for adolescent and young adult head and neck cancer survivors treated with radiotherapy. Support Care Cancer. 2019;27(7):2609–16. https://doi.org/10.1007/s00520-018-4559-5.
Cooperstein E, et al. Vanderbilt head and neck symptom survey version 2.0: Report of the development and initial testing of a subscale for assessment of oral health. Head Neck. 2012;34(6):797–804. https://doi.org/10.1002/hed.21816.
Hays RD, Sherbourne CD. The RAND 36-Item Health Survey 1.0. Health Econ. 1993;2(3):217–27.
ASCO Survivorship Care Plan. [Online]. Available: https://www.cancer.net/survivorship/follow-care-after-cancer-treatment/asco-cancer-treatment-and-survivorship-care-plans.
Gupta N, et al. Radiation-induced dental caries, prevention and treatment - a systematic review. Natl J Maxillofac Surg. 2015;6(2):160. https://doi.org/10.4103/0975-5950.183870.
Moore C, McLister C, Cardwell C, O’Neill C, Donnelly M, McKenna G. Dental caries following radiotherapy for head and neck cancer: a systematic review. Oral Oncol. 2020;100:104484. https://doi.org/10.1016/j.oraloncology.2019.104484.
Aarup-Kristensen S, Hansen CR, Forner L, Brink C, Eriksen JG, Johansen J. Osteoradionecrosis of the mandible after radiotherapy for head and neck cancer: risk factors and dose-volume correlations. Acta Oncol (Madr). 2019;58(10):1373–7. https://doi.org/10.1080/0284186X.2019.1643037.
Ortiz-Comino L, et al. Upper body motor function and swallowing impairments and its association in survivors of head and neck cancer: a cross-sectional study. PLoS One. 2020;15(6):e0234467. https://doi.org/10.1371/journal.pone.0234467.
Krasin MJ, et al. Jaw dysfunction related to pterygoid and masseter muscle dosimetry after radiation therapy in children and young adults with head-and-neck sarcomas. Int J Radiat Oncol Biol Phys. 2012;82(1):355–60. https://doi.org/10.1016/j.ijrobp.2010.09.031.
King SN, Dunlap NE, Tennant PA, Pitts T. Pathophysiology of radiation-induced dysphagia in head and neck cancer. Dysphagia. 2016;31(3):339–51. https://doi.org/10.1007/s00455-016-9710-1 (Springer New York LLC).
De Felice F, et al. Late radiation-associated dysphagia in head and neck cancer patients: evidence, research and management. Oral Oncology. 2018;77:125–30. https://doi.org/10.1016/j.oraloncology.2017.12.021 (Elsevier Ltd).
Starmer HM, et al. Speech-language pathology care and short- and long-term outcomes of laryngeal cancer treatment in the elderly. Laryngoscope. 2015;125(12):2756–63. https://doi.org/10.1002/lary.25454.
Rosenthal DI, Lewin JS, Eisbruch A. Prevention and treatment of dysphagia and aspiration after chemoradiation for head and neck cancer. J Clin Oncol. 2006;24(17):2636–43. https://doi.org/10.1200/JCO.2006.06.0079.
Platteaux N, Dirix P, Hermans R, Nuyts S. Brachial plexopathy after chemoradiotherapy for head and neck squamous cell carcinoma. Strahlenther Onkol. 2010;186(9):517–2520.
Chen AM, et al. Dose-volume modeling of brachial plexus-associated neuropathy after radiation therapy for head-and-neck cancer: Findings from a prospective screening protocol. Int J Radiat Oncol Biol Phys. 2014;88(4):771–7. https://doi.org/10.1016/j.ijrobp.2013.11.244.
McDowell LJ, et al. Long-term late toxicity, quality of life, and emotional distress in patients with nasopharyngeal carcinoma treated with intensity modulated radiation therapy. Int J Radiat Oncol Biol Phys. 2018;102(2):340–52. https://doi.org/10.1016/j.ijrobp.2018.05.060.
Boomsma MJ, Bijl HP, Langendijk JA. Radiation-induced hypothyroidism in head and neck cancer patients: a systematic review. Radiother Oncol. 2011;99(1):1–5. https://doi.org/10.1016/j.radonc.2011.03.002.
Mercado G, Adelstein DJ, Saxton JP, Secic M, Larto MA, Lavertu P. Hypothyroidism: a frequent event after radiotherapy and after radiotherapy with chemotherapy for patients with head and neck carcinoma. Cancer. 2001;92(11):2892–7. https://doi.org/10.1002/1097-0142(20011201)92:11.
Agrawal C, Guthrie L, Sturm MS, Stanek J, Martin L, Henwood-Finley M, et al. Comparison of thyroid nodule prevalence by ultrasound in childhood cancer survivors with and without thyroid radiation exposure. J Pediatr Hematol Oncol. 2016;38(1):43–8. https://doi.org/10.1097/MPH.0000000000000473.
Crom DB, Kaste SC, Tubergen DG, Greenwald CA, Sharp GB, Hudson MM. Ultrasonography for thyroid screening after head and neck irradiation in childhood cancer survivors. Med Pediatr Oncol. 1997;28(1):15–21. https://doi.org/10.1002/(sici)1096-911x(199701)28:1<15::aid-mpo4>3.0.co;2-w.
Trojanowski P, Sojka M, Trojanowska A, Wolski A, Roman T, Jargiello T. Management of radiation induced carotid stenosis in head and neck cancer. Transl Oncol. 2019;12(8):1026–31. https://doi.org/10.1016/j.tranon.2019.05.001.
Carpenter DJ, Mowery YM, Broadwater G, Rodrigues A, Wisdom AJ, Dorth JA, et al. The risk of carotid stenosis in head and neck cancer patients after radiation therapy. Oral Oncol. 2018;80:9–15. https://doi.org/10.1016/j.oraloncology.2018.02.021.
Partap S. Stroke and cerebrovascular complications in childhood cancer survivors. Semin Pediatr Neurol. 2012;19(1):18–24. https://doi.org/10.1016/j.spen.2012.02.012.
O’Donnell MJ, et al. Global and regional effects of potentially modifiable risk factors associated with acute stroke in 32 countries (INTERSTROKE): a case-control study. Lancet. 2016;388(10046):761–75. https://doi.org/10.1016/S0140-6736(16)30506-2.
Boehme AK, Esenwa C, Elkind MSV. Stroke risk factors, genetics, and prevention. Circ Res. 2017;120(3):472–95. https://doi.org/10.1161/CIRCRESAHA.116.308398 (Lippincott Williams and Wilkins).
Watt TC, et al. Radiation-related risk of basal cell carcinoma: a report from the childhood cancer survivor study. J Natl Cancer Inst. 2012;104(16):1240–50. https://doi.org/10.1093/jnci/djs298.
Alterio D, Gugliandolo SG, Augugliaro M, et al. IMRT versus 2D/3D conformal RT in oropharyngeal cancer: A review of the literature and meta-analysis. Oral Dis. 2020;00:1–10.
Laskar S, et al. Nasopharyngeal carcinoma in children: comparison of conventional and intensity modulated radiotherapy. Int J Radiation Oncology Biol Phys. 2008;72(3):728–36.
Funding
This study was generously funded by Rob and Diane Milne through the BC Cancer Foundation and a BC Cancer Prospective Outcomes Support Initiative (POSI) grant.
Author information
Authors and Affiliations
Contributions
SH, ET, SD, KG, FH, and ISM contributed to the design and implementation of the study. SH and KG assessed the patients in consultation. NA performed the data analysis. All the authors contributed to the preparing and editing of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the BC Cancer and University of British Columbia Research Ethics Board.
Consent to participate
All participants consented to participate in this study, participation was voluntary.
Consent for publication
Not applicable,
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hamilton, S.N., Mahdavi, S., Martinez, I.S. et al. A cross-sectional assessment of long-term effects in adolescent and young adult head and neck cancer survivors treated with radiotherapy. J Cancer Surviv 16, 1117–1126 (2022). https://doi.org/10.1007/s11764-021-01103-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-021-01103-w