Abstract
Some genetic males undergo voluntary castration, with and without hormonal supplementation. Here, we investigate the sexual function of 163 such individuals (average age = 52 ± 16-years-old). Specifically, we explored how hormonal, social, and psychological factors play a role in their sexual function. In this study, 47% identified their gender as “eunuch”, and 36% identified their gender as “man.” Furthermore, 64% were in a relationship (80% with a woman), and 28% had a strong attraction for both sexes (Kinsey 2–4). We found that castrated individuals with androgen supplementation have higher sexual function than those without any hormone supplementation. Individuals with anxiety symptoms reported better sexual parameters (better orgasm satisfaction, easier to achieve an erection and an orgasm) than those without anxiety symptoms. Among those low in anxiety, individuals without hormone supplementation had a weaker sex drive and more difficulty in getting sexually aroused than those on supplemental estrogen or androgen. Hierarchical multiple regressions indicated that control variables (i.e., age, depressive symptoms, time since castration, type of hormone supplementation) accounted for 13–30% of the variances in sexual parameters. Including sexual guilt in the models predicted 4–8% additional variances in all sexual parameters except for ease in getting and maintaining an erection. Adding in participants’ sexual trauma scores accounted for an additional 3.7% in the strength of their reported sex drive. In conclusion, various factors—hormone therapy, anxiety, sexual guilt, and childhood trauma—may influence the sexual outcomes for castrated individuals.


Similar content being viewed by others
Availability of Data and Material
Data are not archived in a repository.
References
Beitchman, J. H., Zucker, K. J., Hood, J. E., daCosta, G. A., Akman, D., & Cassavia, E. (1992). A review of the long-term effects of child sexual abuse. Child Abuse & Neglect, 16(1), 101–118. https://doi.org/10.1016/0145-2134(92)90011-F
Bergman, B., Damber, J. E., Littbrand, B., Sjogren, K., & Tomic, R. (1984). Sexual function in prostatic cancer patients treated with radiotherapy, orchiectomy or oestrogens. British Journal of Urology, 56(1), 64–69. https://doi.org/10.1111/j.1464-410X.1984.tb07166.x
Brett, M. A., Roberts, L. F., Johnson, T. W., & Wassersug, R. J. (2007). Eunuchs in contemporary society: Expectations, consequences, and adjustments to castration (part II). Journal of Sexual Medicine, 4(1), 946–955. https://doi.org/10.1111/j.1743-6109.2007.00522.x
Briere, J., & Elliott, D. M. (2003). Prevalence and psychological sequelae of self-reported childhood physical and sexual abuse in a general population sample of men and women. Child Abuse & Neglect, 27(10), 1205–1222. https://doi.org/10.1016/j.chiabu.2003.09.008
Corona, G., Rastrelli, G., Morgentaler, A., Sforza, A., Mannucci, E., & Maggi, M. (2017). Meta-analysis of results of testosterone therapy on sexual function based on international index of erectile function scores. European Urology, 72(6), 1000–1011. https://doi.org/10.1016/j.eururo.2017.03.032
Daskalos, C. T. (1998). Changes in the sexual orientation of six heterosexual male-to-female transsexuals. Archive of Sexual Behavior, 27(6), 605–614. https://doi.org/10.1023/A:1018725201811
Dinh, K. T., Reznor, G., Muralidhar, V., Mahal, B. A., Nezolosky, M. D., Choueiri, T. K., & Nguyen, P. L. (2016). Association of androgen deprivation therapy with depression in localized prostate cancer. Journal of Clinical Oncology, 34(16), 1905–1912. https://doi.org/10.1200/JCO.2015.64.1969
Dinh, K. T., Yang, D. D., Nead, K. T., Reznor, G., Trinh, Q. D., & Nguyen, P. L. (2017). Association between androgen deprivation therapy and anxiety among 78 000 patients with localized prostate cancer. International Journal of Urology, 24(10), 743–748. https://doi.org/10.1111/iju.13409
Finkelstein, J. S., Lee, H., Burnett-Bowie, S. M., Pallais, J. C., Yu, E. W., Borges, L. F., & Leder, B. Z. (2013). Gonadal steroids and body composition, strength, and sexual function in men. New England Journal of Medicine, 368(11), 1011–1022. https://doi.org/10.1056/NEJMoa1206168
Friedman, M. S., Marshal, M. P., Guadamuz, T. E., Wei, C., Wong, C. F., Saewyc, E., & Stall, R. (2011). A meta-analysis of disparities in childhood sexual abuse, parental physical abuse, and peer victimization among sexual minority and sexual nonminority individuals. American Journal of Public Health, 101(8), 1481–1494. https://doi.org/10.2105/AJPH.2009.190009
Gilbert, D. C., Duong, T., Kynaston, H. G., Alhasso, A. A., Cafferty, F. H., Rosen, S. D., & Abel, P. D. (2016). Quality-of-life outcomes from the Prostate Adenocarcinoma: TransCutaneous Hormones (PATCH) trial evaluating luteinising hormone-releasing hormone agonists versus transdermal oestradiol for androgen suppression in advanced prostate cancer. BJU International, 119(5), 667–675. https://doi.org/10.1111/bju.13687
Hackathorn, J. M., Ashdown, B. K., & Rife, S. C. (2016). The sacred bed: Sex guilt mediates religiosity and satisfaction for unmarried people. Sexuality and Culture, 20(1), 153–172. https://doi.org/10.1007/s12119-015-9315-0
Handy, A. B., Jackowich, R. A., Wibowo, E., Johnson, T. W., & Wassersug, R. J. (2016). Gender preference in the sexual attractions, fantasies, and relationships of voluntarily castrated men. Sexual Medicine, 4(1), e51–e59. https://doi.org/10.1016/j.esxm.2015.11.001
Holmes, W. C., & Slap, G. B. (1998). Sexual abuse of boys—definition, prevalence, correlates, sequelae, and management. Journal of the American Medical Association, 280(21), 1855–1862. https://doi.org/10.1001/jama.280.21.1855
Huber, S., & Huber, O. W. (2012). The Centrality of Religiosity Scale (CRS). Religions, 3(3), 710–724. https://doi.org/10.3390/rel3030710
Jabbour, J., Holmes, L., Sylva, D., Hsu, K. J., Semon, T. L., Rosenthal, A. M., & Bailey, J. M. (2020). Robust evidence for bisexual orientation among men. Proceedings of the National Academy of Sciences of the United States of America, 117(31), 18369–18377. https://doi.org/10.1073/pnas.2003631117
Janda, L. H., & Bazemore, S. D. (2011). The revised mosher sex-guilt scale: Its psychometric properties and a proposed ten-item version. Journal of Sex Research, 48(4), 392–396. https://doi.org/10.1080/00224499.2010.482216
Johnson, T. W., & Irwig, M. S. (2014). The hidden world of self-castration and testicular self-injury. Nature Reviews. Urology, 11(5), 297–300. https://doi.org/10.1038/nrurol.2014.84
Johnson, T. W., Wassersug, R. J., Roberts, L. F., Brett, M. A., Sutherland, M., & First, M. B. (2010). Desire for castration is not a body integrity identity disorder (BIID): A response. Journal of Sexual Medicine, 7(2pt1), 852–855. https://doi.org/10.1111/j.1743-6109.2009.01603.x
Kinsey, A. C., Pomeroy, W. B., & Martin, C. E. (1948). Sexual behavior in the human male. W. B. Saunders Co.
Laurent, S. M., & Simons, A. D. (2009). Sexual dysfunction in depression and anxiety: Conceptualizing sexual dysfunction as part of an internalizing dimension. Clinical Psychology Review, 29(7), 573–585. https://doi.org/10.1016/j.cpr.2009.06.007
Lawrence, A. A. (2005). Sexuality before and after male-to-female sex reassignment surgery. Archives of Sexual Behavior, 34(2), 147–166. https://doi.org/10.1007/s10508-005-1793-y
Lowe, B., Decker, O., Muller, S., Brahler, E., Schellberg, D., Herzog, W., & Herzberg, P. Y. (2008). Validation and standardization of the Generalized Anxiety Disorder Screener (GAD-7) in the general population. Medical Care, 46(3), 266–274. https://doi.org/10.1097/MLR.0b013e318160d093
McGahuey, C. A., Gelenberg, A. J., Laukes, C. A., Moreno, F. A., Delgado, P. L., McKnight, K. M., & Manber, R. (2000). The Arizona Sexual Experience scale (ASEX): Reliability and validity. Journal of Sex & Marital Therapy, 26(1), 25–40. https://doi.org/10.1080/009262300278623
Najman, J. M., Dunne, M. P., Purdie, D. M., Boyle, F. M., & Coxeter, P. D. (2005). Sexual abuse in childhood and sexual dysfunction in adulthood: An Australian population-based study. Archives of Sexual Behavior, 34(5), 517–526. https://doi.org/10.1007/s10508-005-6277-6
Radloff, L. S. (1977). The CES-D scale: A self-report depression scale for research in the general population. Applied Psychological Measurement, 1(3), 385–401. https://doi.org/10.1177/014662167700100306
Roberts, L. F., Brett, M. A., Johnson, T. W., & Wassersug, R. J. (2008). A passion for castration: Characterizing men who are fascinated with castration, but have not been castrated. Journal of Sexual Medicine, 5(7), 1669–1680. https://doi.org/10.1111/j.1743-6109.2007.00636.x
Sweet, T., & Welles, S. L. (2012). Associations of sexual identity or same-sex behaviors with history of childhood sexual abuse and HIV/STI risk in the United States. Journal of Acquired Immune Deficiency Syndromes, 59(4), 400–408. https://doi.org/10.1097/QAI.0b013e3182400e75
Thombs, B. D., Bernstein, D. P., Ziegelstein, R. C., Scher, C. D., Forde, D. R., Walker, E. A., & Stein, M. B. (2006). An evaluation of screening questions for childhood abuse in 2 community samples: Implications for clinical practice. Archives of Internal Medicine, 166(18), 2020–2026. https://doi.org/10.1001/archinte.166.18.2020
Vale, K., Siemens, I., Johnson, T. W., & Wassersug, R. J. (2013). Religiosity, childhood abuse, and other risk factors correlated with voluntary genital ablation. Canadian Journal of Behavioural Science, 45(3), 230–237. https://doi.org/10.1037/a0031122
Wassersug, R. J., Zelenietz, S. A., & Squire, G. F. (2004). New age eunuchs: Motivation and rationale for voluntary castration. Archives of Sexual Behavior, 33(5), 433–442. https://doi.org/10.1023/B:ASEB.0000037424.94190.df
Wong, S. T. S., Wassersug, R. J., Johnson, T. W., & Wibowo, E. (2020). Differences in the psychological, sexual, and childhood experiences among men with extreme interests in voluntary castration. Archives of Sexual Behavior, 50(3), 1167–1182. https://doi.org/10.1007/s10508-020-01808-6
Acknowledgements
We thank the Eunuch Archive Steering Committee for helping us post our survey on eunuch.org. We also thank Robyn Jackowich for critical feedback on the draft manuscript.
Funding
SW was supported by a grant from NSERC (RGPIN 8194–2002) to Richard Wassersug.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
Our survey was approved by both the Institutional Review Board of California State University—Chico, and the Eunuch Archive Steering Committee, which manages the web site.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
10508_2021_2094_MOESM1_ESM.tif
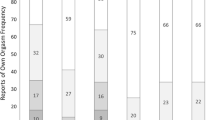
Supplementary Fig. 1 Percentages of individuals taking either no supplemental gonadal hormones (none) and an androgen supplement plotted against sexual attraction as assessed by the Kinsey scale. The proportion of individuals with Kinsey 5 and asexual differed significantly depending on whether they were on androgen treatment or not. *Significantly different from those without hormone supplementation, p < .05; ** p < .01. #Difference in the proportions for Kinsey 3 only approached significance, p = .066 (TIF 2091 kb)
Rights and permissions
About this article
Cite this article
Wibowo, E., Wong, S.T.S., Wassersug, R.J. et al. Sexual Function After Voluntary Castration. Arch Sex Behav 50, 3889–3899 (2021). https://doi.org/10.1007/s10508-021-02094-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10508-021-02094-6