Abstract
Purpose
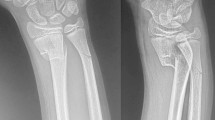
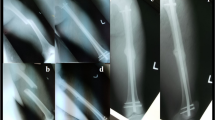
Ankle fracture dislocations represent a great threat for soft tissue viability and articular instability. The use of a temporary ankle bridging ExFix plays a fundamental role in the local damage control orthopaedics while waiting for definitive synthesis.
Methods
For this prospective research, we have developed a full application protocol of innovative diaphyseal monocortical screws fixator (Unyco–OrthofixTM) exclusively under local anaesthesia. Rigid selection criteria allowed us to collect nine patients during a period of almost 2 years. VAS score was analysed for the feasibility of the procedure, and a thorough radiologic evaluation was performed.
Results
Results pointed out that the calcaneus pin insertion (VAS: 3.44) followed by the local anaesthetics injection (VAS: 3.22) was the most painful, without precluding to continue the procedure; fracture temporary stability was achieved in all the cases.
Conclusions
The procedure of monocortical diaphyseal application in bridging external fixation is comparable to the conventional transcalcaneal traction maintaining the advantage in terms of speediness, independence from anaesthetists and feasibility within few minutes from hospital admittance even in patients under anticoagulants therapy, but increasing the stability of the reduction and improving the quality of nursing (so-called portable traction).






Similar content being viewed by others
References
Inman VT (1976) The joints of the ankle. Williams & Wilkins, Baltimore
Mann RA (1986) Biomechanics of the foot and ankle. In: Coughlin MJ, Mann RA (eds) Surgery of the foot and ankle. CV Mosby, St. Louis, pp 2–35
Sculco PK, Lazaro LE, Little MM, Berkes MB, Warner SJ, Helfet DL, Lorich DG (2016) Dislocation is a risk factor for poor outcome after supination external rotation type ankle fractures. Arch Orthop Trauma Surg 136(1):9–15. doi:10.1007/s00402-015-2353-0
Papakostidis C, Kanakaris KK, Pretel J, Faour O, Morell DJ, Giannoudis PV (2011) Prevalence of complications of open tibial shaft fractures stratified as per the Gustilo–Anderson classification. Injury 42(12):1408–1415
Assal M, Ray A, Stern R (2007) The extensile approach for the operative treatment of high-energy pylon fractures: surgical technique and soft tissue healing. J Orthop Trauma 21:198–206
Mauffrey C, Vasario G, Battiston B, Lewis C, Beazley J, Seligson D (2011) Tibial pylon fractures: a review of incidence, diagnosis, treatment, and complications. Acta Orthop Belg 77(4):432–440
Oh JK, Hwang J-H, Sahu D, Jun S-H (2011) Complication rate and pitfalls of temporary bridging external fixator in periarticular comminuted fractures. Clin Orthop Surg 3:62–68
Joveniaux P, Ohl X, Harisboure A, Berrichi A, Labatut L, Simon P, Mainard D, Vix N, Dehoux E (2010) Distal tibia fractures: management and complications of 101 cases. Int Orthop 34(4):583–588
Tscherne H, Gotzen L (1984) Fractures with soft tissue injuries. Springer, Berlin
Tscherne H, Oestern HJ (1982) A new classification of soft-tissue damage in open and closed fractures. Unfallheilkunde 85(3):111–115
Sirkin M, Sanders R, DiPasquale T, Herscovici D Jr (2004) A staged protocol for soft tissue management in the treatment of complex pylon fractures. J Orthop Trauma 18(8 Suppl):S32–S38
Haidukewych GJ (2002) Temporary external fixation for the management of complex intra- and periarticular fractures of the lower extremity. J Orthop Trauma 16(9):678–685
Carroll EA, Koman LA (2011) External fixation and temporary stabilization of femoral and tibial trauma. J Surg Orthop Adv 20(1):74–81
Tong D, Ji F, Zhang H, Ding W, Wang Y, Cheng P, Liu H, Cai X (2012) Two-stage procedure protocol for minimally invasive plate osteosynthesis technique in the treatment of the complex pylon fracture. Int Orthop 36(4):833–837
Lareau CR, Daniels AH, Vopat BG, Kane PM (2015) Emergency department external fixation for provision treatment of pylon and unstable ankle fractures. J Emerg Trauma Shock 8(1):61–64
Lavini F, Dall’Oca C, Mezzari S, Maluta T, Luminari E, Perusi F, Vecchini E, Magnan B (2014) Temporary bridging external fixation in distal tibial fracture. Injury 45(Suppl 6):S58–S63
Quayle J, Gougoulias N (2016) Foot and ankle surgery the effect of different methods of stability assessment on fixation rate and complications in supination external rotation (SER) 2/4 ankle fractures. Foot Ankle Surg 21(2):86–90. doi:10.1016/j.fas.2014.09.010
Browner B, Levine AJJ (1998) Malleolar fractures and soft tissue injuries of the ankle. skeletal trauma: basic science, management, and reconstruction, vol 2, 5th edn. Elsevier Inc, Amsterdam. doi:10.1016/B978-1-4557-7628-3.00066-1
Shibuya N, Davis ML, Jupiter DC (2016) Epidemiology of foot and ankle fractures in the United States: an analysis of the national trauma data bank (2007 to 2011). J Foot Ankle Surg 53(5):606–608. doi:10.1053/j.jfas.2014.03.011
Connors JC, Coyer MA, Hardy MA (2016) Irreducible ankle fracture dislocation due to tibialis posterior tendon interposition: a case report. J Foot Ankle Surg 2015:1–6. doi:10.1053/j.jfas.2015.06.014
Ehrenfreund T, Haluzan D, Dobric I, Zigman T, Rajacic D, Antoljak T (2016) Operative management of unstable ankle fractures in the elderly: our institutional experience. Injury 44(2013):S20–S22. doi:10.1016/S0020-1383(13)70192-X
Kurar L (2016) Clinical audit of ankle fracture management in the elderly *. Ann Med Surg 6:96–101. doi:10.1016/j.amsu.2015.12.061
Mbchb MS, Mbchb GM, Johnstone AJ, Orth F (2016) Percutaneous screw fixation of unstable ankle fractures in patients with poor soft tissues and significant co-morbidities. Foot Ankle Surg. doi:10.1016/j.fas.2015.11.008
Van Son MAC, Vries J De, Roukema JA, Den Oudsten BL (2016) Health status, health-related quality of life, and quality of life following ankle fractures: a systematic review. Injury 44(11):1391–1402. doi:10.1016/j.injury.2013.02.018
Van Zuuren WJ, Schepers T, Beumer A, Sierevelt I, Noort A Van, Van Den Bekerom MPJ (2016) Acute syndesmotic instability in ankle fractures: a review. Foot Ankle Surg. doi:10.1016/j.fas.2016.04.001
Dodd AC, Lakomkin N, Attum B, Bulka C, Karhade AV, Douleh DG, Sethi MK (2016) Predictors of adverse events for ankle fractures: an analysis of 6800 patients. J Foot Ankle Surg. doi:10.1053/j.jfas.2016.03.010
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Lavini, F., Maluta, T., Carpeggiani, G. et al. A new approach to local DCO in ankle fracture dislocations: external fixation with diaphyseal unicortical screws applied by local anaesthesia. Musculoskelet Surg 101, 229–235 (2017). https://doi.org/10.1007/s12306-017-0472-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-017-0472-1