Abstract
Kleine–Levin Syndrome is a rare neurological disorder with onset typically during adolescence that is characterized by recurrent episodes of hypersomnia, behavioral changes, and cognitive abnormalities, in the absence of structural changes in neuroimaging. As for many functional brain disorders, the exact disease mechanism in Kleine-Levin Syndrome is presently unknown, preventing the development of specific treatment approaches or protective measures. Here we review the pathophysiology and genetics of this functional brain disorder and then present a specific working hypothesis. A neurodevelopmental mechanism has been suspected based on associations with obstetric complications. Recent studies have focused on genetic factors whereby the first genome-wide association study (GWAS) in Kleine–Levin Syndrome has defined a linkage at the TRANK1 locus. A Gene x Environment interaction model involving obstetric complications was proposed based on concepts developed for other functional brain disorders. To stimulate future research, we here performed annotations of the genes under consideration for Kleine–Levin Syndrome in relation to factors expected to be associated with obstetric complications. Annotations used data-mining of gene/protein lists related to for hypoxia, ischemia, and vascular factors and targeted literature searches. Tentative links for TRANK1, four additional genes in the TRANK1 locus, and LMOD3-LMO2 are described. Protein interaction data for TRANK1 indicate links to CBX2, CBX4, and KDM3A, that in turn can be tied to hypoxia. Taken together, the neurological sleep disorder, Kleine-Levin Syndrome, shows genetic and mechanistic overlap with well analyzed brain disorders such as schizophrenia, autism spectrum disorder and ADHD in which polygenic predisposition interacts with external events during brain development, including obstetric complications.
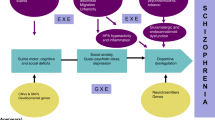
Graphical Abstract
Gene x Environment interaction (G x E) model for the sleep disorder, Kleine-Levin Syndrome (KLS). This hypothesis-generating study proposes that perturbations during neurodevelopment affect the formation of neural circuits for sleep regulation in KLS. Thereby, genetic factors linked to KLS interact (“x”) with obstetric complications as environmental factors. A subset of genes may mediate between the risk for KLS and hypoxia, ischemia, or vascular changes during obstetric complications.



Similar content being viewed by others
References
Adamovich Y, Ladeuix B, Golik M, Koeners MP, Asher G (2017) Rhythmic oxygen levels reset circadian clocks through HIF1α. Cell Metab 25:93–101. https://doi.org/10.1016/j.cmet.2016.09.014
Al Shareef SM, Basit S, Li S, Pfister C, Pradervand S, Lecendreux M, Mayer G, Dauvilliers Y, Salpietro V, Houlden H, BaHammam AS, Tafti M (2019) Kleine–Levin syndrome is associated with LMOD3 variants. J Sleep Res 28(3):e12718. https://doi.org/10.1111/jsr.12718
Ambati A, Hillary R, Leu-Semenescu S, Ollila HM, Lin L, During EH, Farber N, Rico TJ, Faraco J, Leary E et al (2021) Kleine–Levin syndrome is associated with birth difficulties and genetic variants in the TRANK1 gene loci. Proc Natl Acad Sci U S A 118(12):e2005753118. https://doi.org/10.1073/pnas.2005753118
Androvic P, Kirdajova D, Tureckova J, Zucha D, Rohlova E, Abaffy P, Kriska J, Valny M, Anderova M, Kubista M, Valihrach L (2020) Decoding the transcriptional response to ischemic stroke in young and aged mouse brain. Cell Rep 31(11):107777. https://doi.org/10.1016/j.celrep.2020.107777
Arnulf I, Zeitzer JM, File J, Farber N, Mignot E (2005) Kleine–Levin syndrome: a systematic review of 186 cases in the literature. Brain 128(Pt 12):2763–2776. https://doi.org/10.1093/brain/awh620
Arnulf I, Lin L, Gadoth N, File J, Lecendreux M, Franco P, Zeitzer J, Lo B, Faraco JH, Mignot E (2008) Kleine–Levin syndrome: a systematic study of 108 patients. Ann Neurol 63(4):482–493. https://doi.org/10.1002/ana.21333
Arnulf I, Rico TJ, Mignot E (2012) Diagnosis, disease course, and management of patients with Kleine-Levin syndrome. Lancet Neurol 11(10):918–928. https://doi.org/10.1016/S1474-4422(12)70187-4
Arnulf I, Groos E, Dodet P (2018) Kleine-Levin syndrome: a neuropsychiatric disorder. Rev Neurol (paris) 174(4):216–227. https://doi.org/10.1016/j.neurol.2018.03.005
BaHammam AS, GadElRab MO, Owais SM, Alswat K, Hamam KD (2008) Clinical characteristics and HLA typing of a family with Kleine–Levin syndrome. Sleep Med 9(5):575–578. https://doi.org/10.1016/j.sleep.2007.06.015
Beard E, Lengacher S, Dias S, Magistretti PJ, Finsterwald C (2021) Astrocytes as key regulators of brain energy metabolism: new therapeutic perspectives. Front Physio 12:825816. https://doi.org/10.3389/fphys.2021.825816
Beyer S, Kristensen MM, Jensen KS, Johansen JV, Staller P (2008) The histone demethylases JMJD1A and JMJD2B are transcriptional targets of hypoxia-inducible factor HIF. J Biol Chem 283(52):36542–36552. https://doi.org/10.1074/jbc.M804578200
Bono H, Hirota K (2020) Meta-analysis of hypoxic transcriptomes from public databases. Biomedicines 8(1):10. https://doi.org/10.3390/biomedicines8010010
Campiglio M, Costé de Bagneaux P, Ortner NJ, Tuluc P, Van Petegem F, Flucher BE (2018) STAC proteins associate to the IQ domain of CaV1.2 and inhibit calcium-dependent inactivation. Proc Natl Acad Sci U S A 115(6):1376–1381. https://doi.org/10.1073/pnas.1715997115
Chang H, Cai X, Yang ZH, Xiao X, Li M (2021) Regulation of TRANK1 by GSK-3 in the brain: unexpected interactions. Mol Psychiatry 26(11):6109–6111. https://doi.org/10.1038/s41380-021-01120-2
Chauvet C, Bois-Joyeux B, Berra E, Pouyssegur J, Danan JL (2004) The gene encoding human retinoic acid-receptor-related orphan receptor alpha is a target for hypoxia-inducible factor 1. Biochem J 384(Pt 1):79–85. https://doi.org/10.1042/BJ20040709
Chen DT, Jiang X, Akula N, Shugart YY, Wendland JR, Steele CJ, Kassem L, Park JH, Chatterjee N, Jamain S, Cheng A et al (2013) Genome-wide association study meta-analysis of European and Asian-ancestry samples identifies three novel loci associated with bipolar disorder. Mol Psychiatry 18(2):195–205. https://doi.org/10.1038/mp.2011.157
Chu LH, Rivera CG, Popel AS, Bader JS (2012) Constructing the angiome: a global angiogenesis protein interaction network. Physiol Genom 44(19):915–924. https://doi.org/10.1152/physiolgenomics.00181.2011
Engström M, Latini F, Landtblom AM (2018) Neuroimaging in the Kleine–Levin Syndrome. Curr Neurol Neurosci Rep 18(9):58. https://doi.org/10.1007/s11910-018-0866-y
Filippenkov IB, Stavchansky VV, Denisova AE, Valieva LV, Remizova JA, Mozgovoy IV, Zaytceva EI et al (2021) Genome-wide RNA-sequencing reveals massive circular RNA expression changes of the neurotransmission genes in the rat brain after ischemia-reperfusion. Genes (basel) 12(12):1870. https://doi.org/10.3390/genes12121870
Gardener H, Spiegelman D, Buka SL (2011) Perinatal and neonatal risk factors for autism: a comprehensive meta-analysis. Pediatrics 128(2):344–355. https://doi.org/10.1542/peds.2010-1036
Geoffroy PA, Arnulf I, Etain B, Henry C (2013) Kleine–Levin syndrome and bipolar disorder: a differential diagnosis of recurrent and resistant depression. Bipolar Disord 15(8):899–902. https://doi.org/10.1111/bdi.12119
Gratzinger D, Zhao S, West R, Rouse RV, Vogel H, Gil EC, Levy R, Lossos IS, Natkunam Y (2009) The transcription factor LMO2 is a robust marker of vascular endothelium and vascular neoplasms and selected other entities. Am J Clin Pathol 131(2):264–278. https://doi.org/10.1309/AJCP5FP3NAXAXRJE
Gu X, Wang X, Su D, Su X, Lin L, Li S, Wu Q, Liu S, Zhang P, Zhu X, Jiang X (2018) CBX2 inhibits neurite development by regulating neuron-specific genes expression. Front Mol Neurosci 11:46. https://doi.org/10.3389/fnmol.2018.00046
Gunawardena HP, Huang Y, Kenjale R, Wang H, Xie L, Chen X (2011) Unambiguous characterization of site-specific phosphorylation of leucine-rich repeat Fli-I-interacting protein 2 (LRRFIP2) in Toll-like receptor 4 (TLR4)-mediated signaling. J Biol Chem 286(13):10897–10910. https://doi.org/10.1074/jbc.M110.168179
Hédou J, Cederberg KL, Ambati A, Lin L, Farber N, Dauvilliers Y, Quadri M, Bourgin P, Plazzi G, Andlauer O et al (2022) Proteomic biomarkers of Kleine–Levin syndrome. Sleep 45(9):zsac097. https://doi.org/10.1093/sleep/zsac097
Ianzano L, Zhao XC, Minassian BA, Scherer SW (2003) Identification of a novel protein interacting with laforin, the EPM2a progressive myoclonus epilepsy gene product. Genomics 81(6):579–587. https://doi.org/10.1016/S0888-7543(03)00094-6
Jiang X, Detera-Wadleigh SD, Akula N, Mallon BS, Hou L, Xiao T, Felsenfeld G, Gu X, McMahon FJ (2019) Sodium valproate rescues expression of TRANK1 in iPSC-derived neural cells that carry a genetic variant associated with serious mental illness. Mol Psychiatry 24(4):613–624. https://doi.org/10.1038/s41380-018-0207-1
Kas A, Lavault S, Habert MO, Arnulf I (2014) Feeling unreal: a functional imaging study in patients with Kleine-Levin syndrome. Brain 137(Pt 7):2077–2087. https://doi.org/10.1093/brain/awu112
Katz JD, Ropper AH (2002) Familial Kleine-Levin syndrome: two siblings with unusually long hypersomnic spells. Arch Neurol 59(12):1959–1961. https://doi.org/10.1001/archneur.59.12.1959
Khurana P, Sugadev R, Jain J, Singh SB (2013) HypoxiaDB: a database of hypoxia-regulated proteins. Database (oxford) 2013:bat074. https://doi.org/10.1093/database/bat074
Lavault S, Golmard JL, Groos E, Brion A, Dauvilliers Y, Lecendreux M, Franco P, Arnulf I (2015) Kleine–Levin syndrome in 120 patients: differential diagnosis and long episodes. Ann Neurol 77(3):529–540. https://doi.org/10.1002/ana.24350
Leu-Semenescu S, Le Corvec T, Groos E, Lavault S, Golmard JL, Arnulf I (2015) Lithium therapy in Kleine-Levin syndrome: an open-label, controlled study in 130 patients. Neurology 85(19):1655–1662. https://doi.org/10.1212/WNL.0000000000002104
Li J, Xu Y, Long XD, Wang W, Jiao HK, Mei Z, Yin QQ, Ma LN, Zhou AW, Wang LS, Yao M, Xia Q, Chen GQ (2014) Cbx4 governs HIF-1α to potentiate angiogenesis of hepatocellular carcinoma by its SUMO E3 ligase activity. Cancer Cell 25(1):118–131. https://doi.org/10.1016/j.ccr.2013.12.008
Li W, Cai X, Li HJ, Song M, Zhang CY, Yang Y, Zhang L, Zhao L, Liu W, Wang L, Shao M, Zhang Y et al (2021) Independent replications and integrative analyses confirm TRANK1 as a susceptibility gene for bipolar disorder. Neuropsychopharmacology 46(6):1103–1112. https://doi.org/10.1038/s41386-020-00788-4
Lynch HT, Lynch PM, Lanspa SJ, Snyder CL, Lynch JF, Boland CR (2009) Review of the Lynch syndrome: history, molecular genetics, screening, differential diagnosis, and medicolegal ramifications. Clin Genet 76:1–18. https://doi.org/10.1111/j.1399-0004.2009.01230.x
Mihaylova VT, Bindra RS, Yuan J, Campisi D, Narayanan L, Jensen R, Giordano F, Johnson RS, Rockwell S, Glazer PM (2003) Decreased expression of the DNA mismatch repair gene Mlh1 under hypoxic stress in mammalian cells. Mol Cell Biol 23(9):3265–3273. https://doi.org/10.1128/MCB.23.9.3265-3273.2003
Mogavero MP, DelRosso LM, Bruni O, Salemi M, Salsone M, Novellino F, Zucconi M, Ferini Strambi L, Ferri R (2023) Genetics and epigenetics of rare hypersomnia. Trends Genet. https://doi.org/10.1016/j.tig.2023.02.003
Mole DR, Blancher C, Copley RR, Pollard PJ, Gleadle JM, Ragoussis J, Ratcliffe PJ (2009) Genome-wide association of hypoxia-inducible factor (HIF)-1alpha and HIF-2alpha DNA binding with expression profiling of hypoxia-inducible transcripts. J Biol Chem 284(25):16767–16775. https://doi.org/10.1074/jbc.M901790200
Nguyen QT, Groos E, Leclair-Visonneau L, Monaca-Charley C, Rico T, Farber N, Mignot E, Arnulf I (2016) Familial Kleine–Levin syndrome: a specific entity? Sleep 39(8):1535–1542. https://doi.org/10.5665/sleep.6014
Oraki Kohshour M, Papiol S, Ching CRK, Schulze TG (2022) Genomic and neuroimaging approaches to bipolar disorder. Bjpsych Open 8(2):e36. https://doi.org/10.1038/mp.2011.157
Oughtred R, Rust J, Chang C, Breitkreutz BJ, Stark C, Willems A, Boucher L, Leung G, Kolas N, Zhang F et al (2021) The BioGRID database: a comprehensive biomedical resource of curated protein, genetic, and chemical interactions. Protein Sci 30(1):187–200. https://doi.org/10.1002/pro.3978
Parsons MJ, Lester KJ, Barclay NL, Nolan PM, Eley TC, Gregory AM (2013) Replication of genome-wide association studies (GWAS) loci for sleep in the British G1219 cohort. Am J Med Genet B Neuropsychiatr Genet 162B:431–438. https://doi.org/10.1002/ajmg.b.32106
Peraita-Adrados R, Vicario JL, Tafti M, García de León M, Billiard M (2012) Monozygotic twins affected with Kleine–Levin syndrome. Sleep 35(5):595–596. https://doi.org/10.5665/sleep.1808
Polster A, Dittmer PJ, Perni S, Bichraoui H, Sather WA, Beam KG (2018) Stac proteins suppress Ca2+-dependent inactivation of neuronal l-type Ca2+ channels. J Neurosci 38(43):9215–9227. https://doi.org/10.1523/JNEUROSCI.0695-18.2018
Qasrawi SO, BaHammam AS (2023) An update on Kleine–Levin syndrome. Curr Sleep Med Rep 9(1):35–44. https://doi.org/10.1007/s40675-022-00246-1
Reilly ML, Stokman MF, Magry V, Jeanpierre C, Alves M, Paydar M, Hellinga J, Delous M, Pouly D, Failler M et al (2019) Loss-of-function mutations in KIF14 cause severe microcephaly and kidney development defects in humans and zebrafish. Hum Mol Genet 28(5):778–795. https://doi.org/10.1093/hmg/ddy381
Rocamora R, Gil-Nagel A, Franch O, Vela-Bueno A (2010) Familial recurrent hypersomnia: two siblings with Kleine–Levin syndrome and menstrual-related hypersomnia. J Child Neurol 25(11):1408–1410. https://doi.org/10.1177/0883073810366599
Rosenberg AB, Roco CM, Muscat RA, Kuchina A, Sample P, Yao Z, Graybuck LT, Peeler DJ, Mukherjee S et al (2018) Single-cell profiling of the developing mouse brain and spinal cord with split-pool barcoding. Science 360(6385):176–182. https://doi.org/10.1126/science.aam8999
Schiavone S, Mhillaj E, Neri M, Morgese MG, Tucci P, Bove M, Valentino M, Di Giovanni G, Pomara C, Turillazzi E, Trabace L, Cuomo V (2017) Early Loss of Blood–brain barrier integrity precedes NOX2 elevation in the prefrontal cortex of an animal model of psychosis. Mol Neurobiol 54(3):2031–2044. https://doi.org/10.1007/s12035-016-9791-8
Schmidt-Kastner R, van Os J, Esquivel G, Steinbusch HW, Rutten BP (2012) An environmental analysis of genes associated with schizophrenia: hypoxia and vascular factors as interacting elements in the neurodevelopmental model. Mol Psychiatry 17(12):1194–1205. https://doi.org/10.1038/mp.2011.183
Schmidt-Kastner R, Guloksuz S, Kietzmann T, van Os J, Rutten BPF (2020) Analysis of GWAS-derived schizophrenia genes for links to ischemia-hypoxia response of the brain. Front Psychiatry 11:393. https://doi.org/10.3389/fpsyt.2020.00393
Schrode N, Ho SM, Yamamuro K, Dobbyn A, Huckins L, Matos MR, Cheng E, Deans PJM, Flaherty E, Barretto N, Topol A, Alganem K, Abadali S, Gregory J, Hoelzli E, Phatnani H, Singh V, Girish D, Aronow B, Mccullumsmith R, Hoffman GE, Stahl EA, Morishita H, Sklar P, Brennand KJ (2019) Synergistic effects of common schizophrenia risk variants (2019). Nat Genet 51(10):1475–1485. https://doi.org/10.1038/s41588-019-0497-5
Shved N, Warsow G, Eichinger F, Hoogewijs D, Brandt S, Wild P, Kretzler M, Cohen CD, Lindenmeyer MT (2017) Transcriptome-based network analysis reveals renal cell type-specific dysregulation of hypoxia-associated transcripts. Sci Rep 7(1):8576. https://doi.org/10.1038/s41598-017-08492-y
Smith TF, Schmidt-Kastner R, McGeary JE, Kaczorowski JA, Knopik VS (2016) Pre- and perinatal ischemia-hypoxia, the ischemia-hypoxia response pathway, and ADHD risk. Behav Genet 46(3):467–477. https://doi.org/10.1007/s10519-016-9784-4
Sui Y, Gu R, Janknecht R (2021) Crucial functions of the JMJD1/KDM3 epigenetic regulators in cancer. Mol Cancer Res 19(1):3–13. https://doi.org/10.1158/1541-7786.MCR-20-0404
Tiana M, Acosta-Iborra B, Puente-Santamaría L, Hernansanz-Agustin P, Worsley-Hunt R, Masson N, García-Rio F et al (2018) The SIN3A histone deacetylase complex is required for a complete transcriptional response to hypoxia. Nucleic Acids Res 46(1):120–133. https://doi.org/10.1093/nar/gkx951
Ueno T, Fukuhara A, Ikegami A, Ohishi F, Kume K (2012) Monozygotic twins concordant for Kleine–Levin syndrome. BMC Neurol 12:31. https://doi.org/10.1186/1471-2377-12-31
Uguccioni G, Lavault S, Chaumereuil C, Golmard JL, Gagnon JF, Arnulf I (2016) Long-term cognitive impairment in Kleine–Levin syndrome. Sleep 39(2):429–438. https://doi.org/10.5665/sleep.5458
Vandamme J, Völkel P, Rosnoblet C, Le Faou P, Angrand PO (2011) Interaction proteomics analysis of polycomb proteins defines distinct PRC1 complexes in mammalian cells. Mol Cell Proteomics 10(4):110002642. https://doi.org/10.1074/mcp.M110.002642
Wang N, Langfelder P, Stricos M, Ramanathan L, Richman JB, Vaca R, Plascencia M, Gu X, Zhang S, Tamai TK et al (2022) Mapping brain gene coexpression in daytime transcriptomes unveils diurnal molecular networks and deciphers perturbation gene signatures. Neuron 110(20):3318-3338.e9. https://doi.org/10.1016/j.neuron.2022.09.028
Wenz E, Tafti M, Bassetti CLA (2022) LMOD3 gene variant in familial periodic hypersomnolence. Sleep Med 91:105–108. https://doi.org/10.1016/j.sleep.2022.02.019
Wortinger LA, Engen K, Barth C, Andreassen OA, Nordbø Jørgensen K, Agartz I (2019) Asphyxia at birth affects brain structure in patients on the schizophrenia-bipolar disorder spectrum and healthy participants. Psychol Med 52(6):1050–1059. https://doi.org/10.1017/S0033291720002779
Xiong T, Qu Y, Wang H, Chen H, Zhu J, Zhao F, Zou R, Zhang L, Mu D (2018) GSK-3β/mTORC1 Couples synaptogenesis and axonal repair to reduce hypoxia ischemia-mediated brain injury in neonatal rats. J Neuropathol Exp Neurol 77(5):383–394. https://doi.org/10.1093/jnen/nly015
Yamada Y, Pannell R, Forster A, Rabbitts TH (2000) The oncogenic LIM-only transcription factor Lmo2 regulates angiogenesis but not vasculogenesis in mice. Proc Natl Acad Sci U S A 97(1):320–324. https://doi.org/10.1073/pnas.97.1.320
Yuen M, Sandaradura SA, Dowling JJ, Kostyukova AS, Moroz N, Quinlan KG, Lehtokari VL, Ravenscroft G, Todd EJ, Ceyhan-Birsoy O, Gokhin DS, Maluenda J et al (2014) (2014) Leiomodin-3 dysfunction results in thin filament disorganization and nemaline myopathy. J Clin Invest 124(11):4693–4708. https://doi.org/10.1172/JCI75199
Zaghloul N, Patel H, Ahmed MN (2017) A model of Periventricular Leukomalacia (PVL) in neonate mice with histopathological and neurodevelopmental outcomes mimicking human PVL in neonates. PLoS ONE 12:e0175438. https://doi.org/10.1371/journal.pone.0175438
Zeisel A, Muñoz-Manchado AB, Codeluppi S, Lönnerberg P, La Manno G, Juréus A, Marques S, Munguba H, He L et al (2015) Brain structure: cell types in the mouse cortex and hippocampus revealed by single-cell RNA-seq. Science 347(6226):1138–1142. https://doi.org/10.1126/science.aaa1934
Acknowledgements
Michael Hamper dedicates his work on KLS to the Kleine-Levin Syndrome community for their continued support. Rainald Schmidt-Kastner acknowledges support from Dept. Clinical Neuroscience, College of Medicine, FAU.
Funding
The senior author is supported by departmental funding by Dept. Clinical Neuroscience, College of Medicine, FAU.
Author information
Authors and Affiliations
Contributions
Both authors contributed equally to the manuscript’s conception and writing. MH: provided expertise on Kleine–Levin Syndrome. RS-K: provided expertise on hypoxia–ischemia gene interactions and performed the gene annotations. Both authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial or non-financial interests to disclose.
Ethics Approval
This work presents a review of literature and makes use of published databases for genomics. No original patient data or experimental work was used. Accordingly, no ethics approval was required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hamper, M., Schmidt-Kastner, R. Sleep Disorder Kleine–Levin Syndrome (KLS) Joins the List of Polygenic Brain Disorders Associated with Obstetric Complications. Cell Mol Neurobiol 43, 3393–3403 (2023). https://doi.org/10.1007/s10571-023-01391-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-023-01391-z