Abstract
Background: Physicians play a critical role across health care delivery systems, yet their own well-being is often overlooked; mindfulness has been widely recommended as a promising modality to support physician wellness. We sought to explore how physicians experience and engage with a 5-week applied mindfulness program and how they perceive its impact on their personal well-being in the context of their daily lives.
Method: We delivered the Applied Mindfulness Program for Medical Personnel (AMP-MP) at a tertiary care hospital in downtown Toronto, Canada. This prospective qualitative study consists of a thematic analysis of post-program interviews with physicians, from across different specialties, who participated in the AMP-MP. The program includes 2-hour sessions, delivered once a week over 5 weeks, and is based on the teachings of Thích Nhất Hạnh.
Results: We interviewed 28 physicians after they completed the AMP-MP. Our data show that a 5-week training was sufficient for physicians to develop a foundational level of mindfulness that integrated into their daily life. Two themes were identified: mindfulness encourages behavioural and cognitive changes that facilitate well-being, and mindfulness improves communication with patients and colleagues.
Interpretation: Our results show applied mindfulness to be well received by physicians as an effective modality to increase their perceived sense of wellness and enhance communication with their patients and colleagues. Further research is necessary to better understand the individual and systemic implications of mindfulness training, and how this modality can complement other efforts being made to address and maintain physician wellness.
Physicians play a critical role in the physical and mental health of our society, yet their own well-being is often overlooked. The expectation that physicians will prioritize the wellness of others over their own can be perpetuated by physicians, the institutions for which they work, and the wider communities they serve.1–3 Prioritizing the wellness of others is a key contributing factor to the high levels of attrition seen among physicians.2,4 Physicians’ work environments have a unique set of stressors, including experiences related to patients’ fear, suffering and death; challenging interactions with patients, families, colleagues and staff; and high expectations placed on their individual performance. 1,4–7 The adverse impacts of a highly stressful work environment are not limited to a small handful of particularly susceptible physicians,8 but are common across health care environments and specialties.6,9 Physician well-being has been shown to have substantial impacts beyond the personal lives of physicians, including on their patients and health care delivery systems.1,4–7,9 Therefore, it should be of concern not only to individual physicians, but also to health care administrators and the public. Given the increase in challenges related to physician retention, recruitment, mental health, and attrition due to the COVID-19 pandemic, studies exploring ways to pragmatically enhance physician wellness have become more important than ever.10,11
Mindfulness has been widely recommended across the literature as a promising approach to support physician wellness.12–15 However, few empirical studies have been conducted that combine physician wellness and mindfulness-based interventions (MBIs). These studies have shown promising potential for mindfulness to benefit physician well-being, decrease emotional exhaustion and perceived stress, increase compassion and empathy, and enhance patient-centred care.16–21 These studies have been primarily quantitative, leaving a gap in understanding the lived experience and practical application of mindfulness in the context of physicians’ daily lives. With our study’s qualitative design, we aim to address this gap.
We delivered an innovative MBI, the Applied Mindfulness Program for Medical Personnel (AMP-MP), which is based on the teachings of scholar and Zen Master Thích Nhất Hạnh. Although his work is considered seminal in the field,22 to date, we are unaware of any MBIs that have been explicitly or primarily based on his teachings. His pragmatic approach to what he has termed as Applied Mindfulness23 is well suited to physicians, as it provides a training pathway that goes beyond bare attention, with the aim to develop inner and interpersonal resiliency and communication skill sets.24,25 Thích Nhất Hạnh describes mindfulness as an observational lucid awareness of our present-moment experience (e.g., awareness of relevant stimuli’s impact on one’s internal and external states).26
Informed by this body of literature and real-life clinical experience, we had 2 main objectives: to deliver an innovative mindfulness program tailored specifically to the needs and interests of physicians, and to explore how physicians engage with an applied mindfulness program and how they perceive its impact on their well-being and daily life.
Methods
We conducted post-program qualitative interviews with physicians from across different specialties, who participated in a 5-week mindfulness training. Our study design was theoretically grounded within the interpretive paradigm (discussed further in the Application of theory subsection). We recruited physicians practising within the Greater Toronto Area. Medical students and other nonphysician health care professionals were excluded, along with physicians participating in other mindfulness trainings during our study period.27 Recruitment for the intervention was conducted through the University of Toronto’s Temerty Faculty of Medicine and associated teaching hospitals. The intervention was delivered on site at a tertiary care hospital in downtown Toronto, Canada. Participants were enrolled in 1 of 3 intervention groups, based on the timeslot they selected at the time of recruitment. Building on other studies that have delivered MBIs in group settings,28,29 a minimum of 8 and maximum of 22 participants were enrolled in each of the 3 intervention groups. To enhance sample specificity, we applied a purposive sampling approach at the time of intervention enrolment.30 We gave enrolment priority to physicians who reported having a longer period of medical practice and fewer years of experience with mindfulness.
All intervention participants were invited to participate in qualitative post-program interviews. Based on the theory of information power,30 our sample is seen to have high information power, with each participant’s lived experience bringing a highly specific and relevant perspective to our study’s research question.27
Intervention
The Applied Mindfulness Program for Medical Personnel (AMP-MP) includes 2-hour mindfulness training sessions, delivered once a week over 5 weeks (Table 1). Each session includes a mixture of didactic lecture and experiential practices. The didactic lectures provide a theoretical underpinning for the hands-on experiential practices. We provide an overview of the program’s weekly topics and content in Table 1. The AMP-MP is based on the foundational teachings of Thích Nhất Hạnh, which aim to adapt mindfulness practices for practical daily application. Further discussion of Thích Nhất Hạnh’s teachings can be found in our published protocol paper.27
Program overview of the Applied Mindfulness Program for Medical Personnel
Program facilitators
The program was led by 2 facilitators who were not part of the research team. Both facilitators were registered health care professionals with professional training in mindfulness, along with a long-term personal practice rooted in the tradition of Thích Nhất Hạnh.
Data collection
The primary data for this study was generated through qualitative semistructured post-program interviews. We selected qualitative interviews to support the study’s central aim to generate data grounded in the physician participants’ own words and lived experience.31 The interview guide was developed and iterated in consultation with E.W.’s academic thesis program advisory committee, which included experts in qualitative methodology. The development and iteration of the interview guide was reviewed by an external expert in qualitative methodology, who previously served as the director of the Centre for Critical Qualitative Healthcare Research at the Dalla Lana School of Public Health, University of Toronto. All qualitative experts mentioned above are included in the acknowledgements section. The full interview guide is included in Appendix 1, available at www.cmajopen.ca/content/11/6/E1083/suppl/DC1.
Interviews lasted 40–60 minutes and were conducted within 4 weeks of the final program session, either in person or over secure video conferencing. All interviews were audio recorded and transcribed. During the interview process, E.W. generated a weekly report on all interviews conducted to date, which was reviewed by the external expert in qualitative methodology described above. This report included a summary of the participants, iterations to the interview guide and observations on initial themes.
Qualitative rigour and data collection
Participant observation
To mitigate potential fragmentation issues related to the process of coding, organizing, tagging and segmenting interview data,32,32 the first author (E.W.) was present during all program sessions as a participant observer to generate field notes. We used field notes to generate 2-page summary portraits34 describing key characteristics of in situ group dynamics and interactions. These portraits were used during the interview and analysis phases to re-immerse the research team in the context of the program sessions. With this approach, we aimed to mitigate potential fragmentation issues by keeping the broader context of the program delivery alive while analyzing individual interviews.34,35
Reflexivity and transparency
The main lenses deployed in relation to this study by the first author (E.W.) are rooted in their experience as a long-term mindfulness practitioner and academic researcher. E.W. holds a certificate from the Centre for Critical Qualitative Health Research in the Dalla Lana School of Public Health, University of Toronto. In addition, this study was guided by experts in qualitative methodology described in the data collection section above and noted in the acknowledgements. Author N.C. has designed and led mixed-methods studies, and author L.T.Y. has considerable experience with clinical trials.
Transcription
Three key strategies were applied to enhance the rigour of the transcription process and minimize potential transcription errors: providing detailed guidelines to the transcriptionist, reviewing the first transcription against the audio recording and providing further guidelines before the remainder of transcription, and reviewing the transcriptions against the original audio recordings before proceeding with textual analysis.36 Further details on transcription can be found in our published protocol.27
Application of theory
The interpretive paradigm was applied for congruency across all phases of the research study. The epistemology of interpretivism approaches knowledge production as a co-creation between participant perceptions and interpretations of their lived experience, combined with the researcher’s interpretation of their accounts.37–39 This epistemological approach is well suited to our study’s research question,27 which relates to exploring the lived experience of participants within the context of “their daily lives.” We applied the mechanisms of mindfulness theory40 as the study’s middle range theory to assist in the analysis and interpretation phases.41 Further details on our application of theory are discussed in our published protocol.27
Triangulation of data
As a check on the quality of knowledge production, findings were reviewed by all coauthors, along with the first author’s program advisory committee, made up of researchers from the Institute of Medical Science and Dalla Lana School of Public Health at the University of Toronto. A monastic advisory committee made up of senior Dharma Teachers from Thích Nhất Hạnh’s mindfulness practice centre, Plum Village, also reviewed the findings. The program advisory committee and the monastic advisory committee provided feedback across all 6 steps of thematic analysis, described below.
We conducted member reflection sessions with participants 16 months after the initial study. Member reflections seek further “input [from participants] during the processes of analyzing data and producing the research report.”42 Member reflection sessions were held over Zoom and consisted of E.W. presenting a summary of the current analysis and interpretation of the interview data, with time given afterward for participants to provide input. All study participants were invited to participate in 1 of 3 member reflection sessions.
Data analysis
We used thematic analysis to analyze the data. Thematic analysis allows for a clear and systematic approach that accounts for the complex and dynamic nature of exploring human interactions and behaviours.43 A primarily inductive approach was used, resulting in themes being strongly linked to the data, or being “data-driven,” rather than fitting into a preconceived coding format. We used NVivo software to manage the coding process, but not as a tool for analysis or interpretation. Data analysis was conducted in line with the 6 steps of thematic analysis, as described by Braun and Clark.43
In the first step of thematic analysis, we re-read transcripts multiple times to generate initial notes and become familiar with the data. In the second step of thematic analysis, we generated initial codes. The third step involved moving from generating codes to the broader work of developing themes. We created thematic maps in the third step to help develop candidate themes. The fourth step involved refining the candidate themes. In the fifth step, we reviewed the collated data to give each theme a name and begin writing the detailed analysis. In the sixth step, we identified data extracts for each theme and produced a final report.
Ethics approval
Institutional ethics approval was obtained from the Hospital for Sick Children (no. 1000059931) and the University of Toronto (no. 36675). Additional details on study design and procedures can be found in our published protocol.27
Results
A total of 45 physicians participated in the 5-week intervention, and 28 participants were interviewed. A flow chart showing our intervention enrolment process is included in Appendix 2 (available at www.cmajopen.ca/content/11/6/E1083/suppl/DC1). Previous studies using qualitative research methods that combine physician wellness and mindfulness-based trainings have reported similar sample sizes.16,18–20
The 28 participants in this study represent a wide range of different specialties (Box 1). The mean age of participants was 41.3 years, and 1 resident participated in the study. The mean number of years in practice was 14. In response to the registration survey’s “current knowledge of mindfulness” scale, most participants ranked themselves as having 0 (none) to 1 (some knowledge, 0–2 years) of “mindfulness experience.” The question regarding “current knowledge of mindfulness” from the recruitment survey is included in Appendix 3 (available at www.cmajopen.ca/content/11/6/E1083/suppl/DC1). The average number of sessions attended was 3.7 out of 5. Compared with similar studies, this was seen as a sufficient level of attendance.16,44
Specialties represented across interview participants
Adolescent medicine
Anesthesiology
Cardiology
Emergency medicine
Family medicine
Sleep medicine
Obstetrics and gynecology
Oncology (pediatric)
Ophthalmology
Palliative care
Pediatrics
Adult psychiatry
Child and adolescent psychiatry
Forensic psychiatry
Rheumatology
Sports medicine
Surgery
Results of thematic analysis
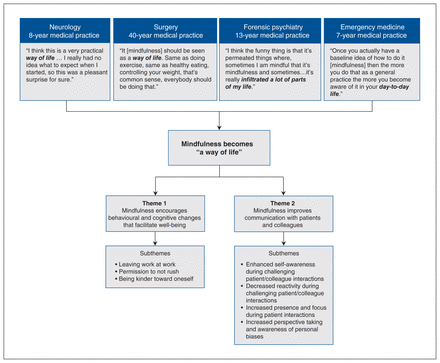
Our analysis showed the AMP-MP program to be well received by participants (Table 2). Further examination of the data showed that mindfulness became a “way of life,” within which 2 key themes were identified: mindfulness encourages behavioural and cognitive changes that facilitate well-being, and mindfulness improves communication with patients and colleagues (Figure 1).
Representative quotations showing the Applied Mindfulness Program for Medical Personnel was well received by participants
Thematic map of key themes and subthemes.
Theme 1: Mindfulness encourages behavioural and cognitive changes that facilitate well-being
Illustrated through 3 subthemes, this data set (Table 3) shows that the integration of mindfulness can decrease workplace stressors, resulting in a greater sense of wellness.
Theme 1: Mindfulness encourages behavioural and cognitive change that facilitates well-being
Subtheme 1: Leaving work at work
Participants report that integrating brief mindfulness practices at the beginning and end of their workday can lead to more effective regulation of workplace stressors, which can lead to feeling more energized at the end of the day. Participants also report that a brief mindful reset at the end of the day can reduce the transfer of occupational stressors, such as frustration, to their home environment.
Subtheme 2: Permission to not rush
This data set reveals that feeling pressure to multitask is a major stressor for physicians. Mindfulness can help physicians observe harmful thought patterns in relation to work pressures, which results in them being “less anxious,” “less worried,” “more calm and confident,” and “relaxed and more present” with patients and colleagues. Analysis of the data indicates that this is due in part to an increase in self-awareness around inner narratives. Physicians can reduce their mental load by first becoming aware of, and then actively reframing, unhelpful thoughts. For example, rather than thinking that “my day looks crazy” or having the “panic button go off,” physicians instead take a mindful pause to observe and rework their thoughts. Their accounts suggest that this allows them to “give themselves permission not to rush.” The data show that “permission to not rush” does not diminish work ethic or output; rather, it suggests that a mindful pause can increase efficiency and engagement with their work.
Subtheme 3: Being kinder toward oneself
Mindfulness also has the potential to shift harmful internal narratives rooted in the culture of medicine (e.g., individual achievement, self-reliance and self-sacrifice). This shift can result in greater permission for self-care (e.g., prioritizing and recognizing their own mental health needs) and setting healthier boundaries with patients.
Theme 2: Mindfulness improves communication with patients and colleagues
The data set supporting this theme (Table 4) includes 4 subthemes that illustrate the potential for mindfulness to beneficially affect interactions with both patients and colleagues.
Theme 2: Mindfulness improves communication with patients and colleagues
Subtheme 1: Enhanced self-awareness during challenging patient and colleague interactions
Participants describe having a greater awareness of what they contribute to challenging interactions with patients and colleagues. Through this understanding, they can implement more compassionate communication styles, which helps them set and maintain clearer boundaries for themselves during frustrating or irritating interactions.
Subtheme 2: Decreased reactivity during challenging patient and colleague interactions
Participants report that the application of mindfulness helps to de-escalate interactions that otherwise might lead to anger, frustration and “negative” communication styles. The data indicate that this decrease in reactivity benefits both communication and delivery of care during challenging patient and colleague interactions.
Subtheme 3: Increased presence and focus during patient interactions
Our data show that mind wandering during patient interactions is quite common. For example, while examining a patient, physicians often think about the next patient. Several participants described an increased ability to remain present and focused while with a patient, resulting in an enhanced quality of care provided.
Subtheme 4: Increased perspective taking and awareness of personal biases
Several participants describe mindfulness positively affecting patient interactions by increasing awareness of their preconceived perceptions of a patient, resulting in their diagnosis and treatment plans being more patient-centred. The data also indicate that applying mindfulness during interactions with patients and colleagues can increase the “human” element of interactions. Participants reported that this shift in perspective positively benefits their own sense of well-being, delivery of care, and communication patterns with patients, colleagues, and leadership and teams.
Additional data: practical application of mindfulness in daily life
Additional data, included in Appendix 4 (available at www.cmajopen.ca/content/11/6/E1083/suppl/DC1), illustrate specialty-specific contexts in which participants apply mindfulness, including surgeons while the operating room is being cleaned, emergency department physicians while sanitizing, and ophthalmologists while taking notes between patients. In Appendix 5 (available at www.cmajopen.ca/content/11/6/E1083/suppl/DC1), we have included a 2-page graphic summarizing the top 6 mindfulness practices and concepts that physicians in our study report using most frequently.
Interpretation
Our findings indicate that a 5-week period can be sufficient for physicians to develop a foundational level of mindfulness that can positively affect their individual well-being, along with enhancing interactions with their patients and colleagues. Our data show that pairing “small doses” of mindfulness throughout the day with regular activities, such as breathing, eating, walking and commuting, is a practical approach for physicians to integrate mindfulness in the context of their busy schedules. The data also indicate that mindfulness can increase the likelihood of a patient-centred pattern of care, and can help physicians manage occupational stressors and develop a better work–life balance.
Across the literature, MBIs have been shown to be a potentially effective means to increase clinician wellness.45–47 The most prolific MBIs included in the literature, developed primarily for patient populations, are typically 8 weeks in length.48 Studies combining physician wellness and MBIs consistently report the need to modify and adapt the length and content of MBIs to suit physicians’ work contexts (e.g., busy and unpredictable schedules).49–52 Our finding that 5 weeks is a sufficient length for, and well received by, physicians is consistent with the recommendations from these studies and adds further evidence that less than 8 weeks can be effective when delivering an MBI to physicians.
Our study’s use of qualitative measures complements the existing quantitative evidence base and is consistent with the few empirical studies that have applied a qualitative lens.16,19 For example, a qualitative study by Beckman and colleagues16 reports improvement in attentive listening to patients, greater self-awareness and enhanced communication with colleagues. These results correspond with our findings that mindfulness has the potential to beneficially permeate across a physician’s life in relation to the requirements and pressures of their occupational environment.
While the findings from this study are encouraging, they also show that there is no one-size-fits-all approach to mindfulness and well-being initiatives. Future research should consider how to involve wider institutional structures to support the ongoing integration of mindfulness across health care organizations. Future studies could be run with medical students and other groups of allied health care providers, along with interdisciplinary groups of health care providers. Integrating and centring BIPOC (Black, Indigenous and other people of colour) and other marginalized communities’ voices within research, mindfulness and well-being initiatives is an important consideration for future studies. Future studies could also consider examining the delivery of AMP-MP through online platforms.
A strength of this study was the use of qualitative methods to generate data from the direct lived experiences of physicians. Thích Nhất Hạnh’s teachings as the foundation for the intervention adds to the novelty of this study.
Limitations
Study results should be considered in light of some limitations. Our purposive sampling approach enhances sample specificity by including physicians with more years of medical practice and less mindfulness experience. However, this approach limits our current understanding of how medical students and other health care providers would respond. Physicians in this study also self-selected to respond to the recruitment efforts. Self-selection may mean that some participants had a predisposition to accepting mindfulness. However, analysis of the data shows the majority of participants expressed some level of skepticism about mindfulness at the outset of the intervention. Literature on the delivery of MBIs in health care settings indicates that self-selection can be considered acceptable and pragmatic.16 Program facilitators were selected based on a high-quality set of credentials. While this supported the successful delivery of the intervention, it limits our understanding of how AMP-MP can be transferred into contexts that may not have access to facilitators with the same level of expertise. Quantitative outcomes were not used in this study. Therefore, a future direction that could broaden the understanding of our findings would be to implement a mixed-methods, randomized controlled trial or quantitative study design.
Conclusion
This study shows the promising potential for applied mindfulness to benefit the broader health care delivery system by positively affecting physicians’ individual well-being, along with enhancing their interactions with patients and colleagues. We hope this paper can serve as a call to action for clinicians and policy-makers to continue exploring how applied mindfulness can complement ongoing efforts to cultivate healthy and compassionate health care environments, where clinician well-being is the norm rather than the exception. The accounts of our participants show that applied mindfulness can be implemented right away to effect positive change at both the individual and institutional levels. At the same time, further work is needed to effect change at a systems level to support the broader implementation and long-term sustainment of mindfulness and other modalities that can support physicians to thrive.
Acknowledgements
The authors acknowledge the insights and support provided by Blake Poland, Sara Ahola Kohut, Brenda Toner and Pauli Gardner (Academic Advisory Committee from the University of Toronto); Brother Pháp Hữu, Brother Pháp Dung, Brother Pháp Linh, and Sister True Dedication (Monastic Advisory Committee from Plum Village International); along with the generous support of Agnes Wong. Thanks to Denise Gastaldo for her qualitative expertise and support across this study. With deep gratitude, we thank Zen Master Thích Nhất Hạnh for his teachings and work in the fields of Engaged and Applied Buddhism, upon which the training program in this study is based.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Elli Weisbaum and Nicholas Chadi contributed to the conception and design of the work. Elli Weisbaum, Nicholas Chadi and L. Trevor Young contributed to the analysis and interpretation of the data. Elli Weisbaum wrote the original draft and all authors revised the manuscript for important intellectual content. All authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This study was funded by a supervisor’s research grant through The Hospital for Sick Children and the Institute of Medical Sciences, University of Toronto (E.W.). Author N.C. was supported by a Junior 1 Career Development Award from the Fonds de recherche du Québec – Santé.
Data sharing: All data relevant to the study are included in the article or uploaded as supplementary information.
Previous presentations: The full study protocol is available online: https://www.frontiersin.org/articles/10.3389/fpubh.2022.807792/full.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/11/6/E1083/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2023 CMA Impact Inc. or its licensors