Abstract
Background
Intramedullary devices have increasingly become popular and are widely used for fixation of unstable intertrochanteric and subtrochanteric fractures. These implants have been designed taking into consideration of the anthropometry of the western population which varies from those of other ethnic groups. This study was carried out to assess the geometry of proximal femur for the placement of short cephalomedullary nails in our subset of patients and suggest suitable design modifications based on these parameters.
Materials and Methods
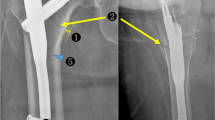
The study was conducted in the following three groups: (1) Anthropometric study of 101 adult human dry femora, (2) radiographs of the same femora, and (3) radiographs of the contralateral uninjured limb of 102 patients with intertrochanteric or subtrochanteric fractures. In Group 1, standard anthropometric techniques were used to measure neck shaft angle (NSA), minimal neck width (NW), trochanteric offset, and distance from the tip of greater trochanter (GT) to the lower border of lesser trochanter on the femoral shaft axis (distance X). In Group 2 and 3, the NSA, minimal NW, NW at 130° and 135°, trochanteric shaft angle (TSA), trochanteric offset, distance X, distance between the tip of GT and the point where the neck axis crosses the line joining the tip of the GT to the lower border of the lesser trochanter on the femoral shaft axis (distance Y), and canal width at 10, 15, and 20 cm from tip of GT were measured on standard radiographs. The values obtained in these three groups were pooled to obtain mean values. Various parameters of commonly used short cephalomedullary nails available for fixation of pertrochanteric fractures were obtained. These were compared to the results obtained to suggest suitable modifications in the nail designs for our subset of patients.
Results
The mean parameters observed were as follows: NSA 128.07° ± 4.97 (range 107°–141°), minimum NW 29.0 ± 2.8 mm (range 22–42 mm), NW at 130° 30.12 ± 2.86 mm (range 22.2–42.5 mm), NW at 135° 30.66 ± 3.02 mm (range 22.8–40.3 mm), TSA 10.45° ± 2.34° (range 3°–15.5°), distance X 65.73 ± 6.45 mm (range 28.6–88.4 mm), distance Y 38 ± 4.91 mm (range 16.6–55.3 mm), and canal width at 10, 15, and 20 cm from the tip of GT 13.46 ± 2.34 mm, 11.40 ± 2.27 mm, and 11.64 ± 2.04 mm, respectively.
Conclusion
The measurements of the proximal femur are not significantly different from other ethnic groups and are adequate to accept the current commonly available short cephalomedullary nails. However, certain modifications in the presently available short cephalomedullary nail designs are recommended for them to better fit the anatomy of our subset of population (a) two nails of 125° and 135°, (b) the medio-lateral angle at the level of 65 mm from the tip of the nail, (c) two femoral neck screw placements (35 and 45 mm from the tip of the nail), and (d) five different sizes of distal width for better fit in canal (9–13 mm).
Similar content being viewed by others
References
Chiu CK, Chan CY, Singh VA. Is the femoral neck geometry adequate for placement of the proximal femoral nail in the Malaysian population? A review of 100 cases. Med J Malaysia 2009;64:22–6.
Streubel PN, Wong AH, Ricci WM, Gardner MJ. Is there a standard trochanteric entry site for nailing of subtrochanteric femur fractures? J Orthop Trauma 2011;25:202–7.
Koval KJ. Intramedullary nailing of proximal femur fractures. Am J Orthop (Belle Mead NJ) 2007;36 4 Suppl: 4–7.
Mishra AK, Chalise P, Singh RP, Shah RK. The proximal femur–A second look at rational of implant design. Nepal Med Coll J 2009;11:278–80.
Ravichandran D, Muthukumaravel N, Jaikumar R, Das H, Rajendran M. Proximal femoral geometry in Indians and its clinical applications. J Anat Soc India 2011;60:6–12.
Siwach RC, Dahiya S. Anthropometric study of proximal femur geometry and its clinical application. Indian J Orthop 2003;37:247–51.
Menezes DF, Gamulin A, Noesberger B. Is the proximal femoral nail a suitable implant for treatment of all trochanteric fractures? Clin Orthop Relat Res 2005;439:221–7.
Lv C, Fang Y, Liu L, Wang G, Yang T, Zhang H, et al. The new proximal femoral nail antirotation-Asia: Early results. Orthopedics 2011;34:351.
Soucanye de Landevoisin E, Bertani A, Candoni P, Charpail C, Demortiere E. Proximal femoral nail antirotation (PFN-ATM) fixation of extra-capsular proximal femoral fractures in the elderly: Retrospective study in 102 patients. Orthop Traumatol Surg Res 2012;98:288–95.
Schipper IB, Bresina S, Wahl D, Linke B, Van Vugt AB, Schneider E. Biomechanical evaluation of the proximal femoral nail. Clin Orthop Relat Res 2002;405:277–86.
Takigami I, Matsumoto K, Ohara A, Yamanaka K, Naganawa T, Ohashi M, et al. Treatment of trochanteric fractures with the PFNA (proximal femoral nail antirotation) nail system–Report of early results. Bull NYU Hosp Jt Dis 2008;66:276–9.
Lakhwani OP. Correlation of trochanter-shaft angle in selection of entry site in antegrade intramedullary femoral nail. ISRN Orthop 2012;2012:431374.
Jain AK, Maheshwari AV, Nath S, Singh MP, Nagar M. Anteversion of the femoral neck in Indian dry femora. J Orthop Sci 2003;8:334–40.
Singh PI, Bhasin ML. Anthropometry. 1st ed. Delhi: Educational Publishers and Booksellers; 1968. p. 142.
Ryder CT, Crane L. Measuring femoral anteversion; the problem and a method. J Bone Joint Surg Am 1953;35-A: 321–8.
Leung KS, Procter P, Robioneck B, Behrens K. Geometric mismatch of the gamma nail to the Chinese femur. Clin Orthop Relat Res 1996;323:42–8.
Ogata K, Goldsand EM. A simple biplanar method of measuring femoral anteversion and neck-shaft angle. J Bone Joint Surg Am 1979;61:846–51.
Patron MS, Duthie RA, Sutherland AG. Proximal femoral geometry and hip fractures. Acta Orthop Belg 2006;72:51–4.
Parsons FG. The characters of the English thigh-bone. J Anat Physiol 1914;48(Pt 3):238–67.
Schofield G. Metric and morphological features of the femur of the New Zealand Maori. J R Anthropol Inst 1959;89:89.
Davivongs V. The femur of the Australian aborigine. Am J Phys Anthropol 1963;21:457–67.
Walensky NA, O’Brien MP. Anatomical factors relative to the racial selectivity of femoral neck fracture. Am J Phys Anthropol 1968;28:93–6.
Tan CK. Some characteristics of the Chinese femur. Singapore Med J 1973;14:505–10.
Noble PC, Alexander JW, Lindahl LJ, Yew DT, Granberry WM, Tullos HS. The anatomic basis of femoral component design. Clin Orthop Relat Res 1988;235:148–65.
Rubin PJ, Leyvraz PF, Aubaniac JM, Argenson JN, Estève P, de Roguin B. The morphology of the proximal femur. A three-dimensional radiographic analysis. J Bone Joint Surg Br 1992;74:28–32.
Dragojevic MD, Grkovic I, Bobinac D, Dujmovic M, Nemec B. Relationship between femoral anteversion and neck shaft angle. Coll Antropol 1996;20:111–7.
Toogood PA, Skalak A, Cooperman DR. Proximal femoral anatomy in the normal human population. Clin Orthop Relat Res 2009;467:876–85.
Osorio H, Schorwer K, Coronado C, Delgado J, Aravena P. Proximal femoral epiphysis anatomy in Chilean population. Int J Morphol 2012;30:258–62.
Baharuddin MY, Kadir M.A, Zulkifly AH, Saat A, Aziz AA, Lee MM. Morphology study of the proximal femur in Malay population. Int J Morphol 2011;29:1321–5.
Saikia KC, Bhuyan SK, Rongphar R. Anthropometric study of the hip joint in northeastern region population with computed tomography scan. Indian J Orthop 2008;42:260–6.
Bridle SH, Patel AD, Bircher M, Calvert PT. Fixation of intertrochanteric fractures of the femur. A randomised prospective comparison of the gamma nail and the dynamic hip screw. J Bone Joint Surg Br 1991;73:330–4.
Halder SC. The gamma nail for peritrochanteric fractures. J Bone Joint Surg Br 1992;74:340–4.
Raviraj A, Anand A, Chakravarthy M, Pai S. Proximal femoral nail antirotation (PFNA) for treatment of osteoporotic proximal femoral fractures. Eur J Orthop Surg Traumatol 2012;22:301–5.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pathrot, D., Ul Haq, R., Aggarwal, A.N. et al. Assessment of the geometry of proximal femur for short cephalomedullary nail placement. IJOO 50, 269–276 (2016). https://doi.org/10.4103/0019-5413.181785
Published:
Issue Date:
DOI: https://doi.org/10.4103/0019-5413.181785