Abstract
Background
Economic factors are a limiting factor toward the implementation of many health programmes and interventions. Economic evaluation has a great potential to contribute toward cost-effective healthcare delivery in South Africa. Little is known about the characteristics and quality of health economic (including pharmacoeconomic) research in South Africa.
Objective and Methods
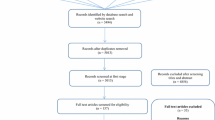
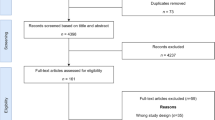
This study assessed the state of health economic (including pharmacoeconomic) research in South Africa. PUBMED, MEDLINE, HealthSTAR, EconLit and PsycINFO databases were searched to identify health economic articles pertaining to South Africa published between 1 January 1977 and 30 April 2010. The searches used the following Medical Subject Headings (MeSH) terms and text words alone and in combination: ‘costs’, ‘health’ and ‘south Africa’. Our study included only original economic studies/analyses that pertained to South Africa, addressed a health-related topic, and had a statement or word in the title, abstract or keywords that indicated that an economic (including cost) analysis had been conducted. The study only included complete peer-reviewed publications (e.g. abstracts were excluded) that were reported in the English language. Two reviewers independently scored each article in the final sample using the data collection form designed for the study.
Results
In total, 108 studies investigating a wide variety of diseases were included in the study. These articles were published in 39 different journals mostly based outside of South Africa between 1977 and 2010. On average, each article was written by three authors. Most first authors had medical/clinical training and resided in South Africa at the time of publication of their study. Based on a 1–10 scale, with 10 indicating the highest quality, the mean quality score for all studies was 7.59 (SD 1.42) and half of the articles were of good quality (score 8–10) The quality of studies was related to the country in which the journal publishing the article was based (outside South Africa = higher); current residence of the primary author (outside South Africa = higher); method of economic analysis (economic evaluations higher than cost studies); type of data used (secondary higher than primary); primary training of the first author (health economics/pharmacoeconomics = higher); type of medical function (diagnosis = higher); study perspective (societal = higher); primary health intervention (pharmaceuticals = higher); study design (modelling = higher); number of authors (more = higher); and year of publication (more recent = higher) [p≥0.05].
Conclusion
Half of the articles were of poor or fair quality. Measures are needed to promote the commissioning of more and better quality health economic and pharmacoeconomic studies in South Africa.



Similar content being viewed by others
References
Anderson AN, Wessels F, Moodley I, et al. AT1 receptor blockers: cost-effectiveness within the South African context. S Afr Med J 2000; 90 (5): 494–8.
Joint United Nations Programme on HIV/AIDS (UNAIDS). 2004 report on the Global AIDS epidemic: 4th Global Report. Geneva: UNAIDS/WHO, 2004.
Cleary S, Mooney G, McIntyre D. Equity and efficiency in HIV-treatment in South Africa: the contribution of mathematical programming to priority setting. Health Econ 2010; 19 (10): 1166–80.
Rosen S, Ketlhapile M, Sanne I, et al. Cost to patients of obtaining treatment for HIV/AIDS in South Africa. S Afr Med J 2007; 97 (7): 524–9.
Stefan DC, Stones D. How much does it cost to treat children with Hodgkin lymphoma in Africa? Leukemia Lymphoma 2009; 50 (2): 196–9.
Hukins GB, Richter AM, van Staden N. Day clinics and hospitals: a cost comparison. S Afr Med J 2001; 91 (1): 66–72.
Kane-Berman JD, Taylor SP. Containing costs in public sector hospitals: a strategy for the future — lessons from a large teaching hospital. S Afr Med J 1990; 78 (3): 154–7.
Ijsselmuiden CB, De Beer C. Reducing health care costs: potential and limitations of local authority health services. S Afr Med J 1990; 78 (3): 161–4.
Chigwedere P, Seage 3rd GR, Gruskin S, et al. Estimating the lost benefits of antiretroviral drug use in South Africa. J Acq Immun Def Synd 2008; 49 (4): 410–5.
Benatar SR, van Rensburg HC. Health care services in a new South Africa. Hastings Cent Rep 1995; 25 (4): 16–21.
Pillans PI, Conry I, Gie BE. Drug cost containment at a large teaching hospital. Pharmacoeconomics 1992; 1 (5): 377–82.
Adam MA, Johnson LF. Estimation of adult antiretroviral treatment coverage in South Africa. S Afr Med J 2009; 99 (9): 661–7.
Naidoo LC, Stephen LX. Oral health finance and expenditure in South Africa. J Dent Assoc S Afr 1997; 52 (12): 727–32.
Harling G, Wood R. The evolving cost of HIV in South Africa: changes in health care cost with duration on antiretroviral therapy for public sector patients. J Acq Immun Def Synd 2007; 45 (3): 348–54.
Parrish A, Blockman M. Clinical excellence and the NIC-Eties of value-based priority setting. S Afr Med J 2008; 98 (10): 758, 760–1.
Jinabhai CC, Ramdas PD, Govender V. Cost analysis of the basic package, resource utilisation and financing of health services at Halley Stott Health Centre and Umbumbulu Clinic in KwaZulu-Natal. S Afr Med J 1997; 87(10): 1359–64.
Broomberg J, Rees H. Delivering at the right price: the costs of primary maternity care at the Diepkloof Community Health Centre, Soweto. S Afr Med J 1993; 83 (4): 272–5.
Deghaye N, Pawinski RA, Desmond C. Financial and economic costs of scaling up the provision of HAART to HIV-infected health care workers in KwaZulu-Natal. S Afr Med J 2006; 96 (2): 140–3.
Cleary SM, McIntyre D, Boulle AM. The cost-effectiveness of antiretroviral treatment in Khayelitsha, South Africa: a primary data analysis. Cost Eff Resour Alloc 2006; 4: 20.
Cleary SM, McIntyre D. Affordability: the forgotten criterion in health-care priority setting. Health Econ 2009; 18(4): 373–5.
Gavaza P, Rascati KL, Oladapo AO, et al. The state of health economic evaluation research in Nigeria: a systematic review. Pharmacoeconomics 2010; 28 (7): 539–53.
Gavaza P, Rascati KL, Lawson K, et al. The state of health economics and pharmacoeconomics research in Zimbabwe. Curr Ther Res 2008; 69 (3): 268–85.
Sullivan SD, Lyles A, Luce BR, et al. AMCP guidance for submission of clinical and economic evaluation data to support formulary listing in US health plans and pharmacy benefits management organizations. J Man Care Pharm 2001; 7 (4): 272–82.
Zarnke K, Levine M, O’Brien B. Cost-benefit analysis in the health care literature: don’t judge a study by its label. J Clin Epidemiol 1997; 50 (7): 817–22.
Offman J, Sullivan S, Neumann P, et al. Examining the value and quality of health economic analyses: implications of utilizing the QHES. J Man Care Pharm 2003; 9 (1): 53–61.
Drummond MF, Sculpher MJ, Torrance GW, et al. Methods for the economic evaluation of health care programmes. 3rd rev. ed. Oxford: Oxford University Press, 2005.
Rascati KL. Essentials of pharmacoeconomics. Philadelphia (PA): Lippincott Williams & Wilkins, 2009.
PASW® Statistics [computer program]. Version 18. Chicago (IL): SPSS Inc, 2009.
Coetzee D, Hildebrand K, Boulle A, et al. Outcomes after two years of providing antiretroviral treatment in Khayelitsha, South Africa. AIDS 2004; 18 (6): 887–95.
Decosas J. HIV prevention and treatment in South Africa: affordable and desirable. Lancet 2003; 361 (9364): 1146–7.
Geffen N. Beyond HAART: scientists and activists need to work together. Lancet 2009; 374 (9693): 860–1.
Haile B. Affordability of home-based care for HIV/AIDS. S Afr Med J 2000; 90 (7): 690–1.
Jeena PM, McNally LM, Stobie M, et al. Challenges in the provision of ICU services to HIV infected children in resource poor settings: a South African case study. J Med Ethics 2005; 31 (4): 226–30.
O’Farrell N. Cost-effectiveness of services for sexually transmitted diseases in prevention of HIV-1. Lancet 1998; 351 (9103): 681–2.
Sidley P. South African drug companies are found guilty of price fixing. BMJ 2008; 336 (7641): 413.
Song C. Infection and the impact on cost effectiveness in wound care. Adv Wound Care 1995; 8 (5): 58–9.
Taylor S, Kuhn L, Dupree W, et al. Direct comparison of liquid-based and conventional cytology in a South African screening trial. Int J Cancer 2006; 118 (4): 957–62.
White RG, Glynn JR, Orroth KK, et al. Male circumcision for HIV prevention in sub-Saharan Africa: who, what and when? AIDS 2008; 22 (14): 1841–50.
Hanass-Hancock J. Disability and HIV/AIDS: a systematic review of literature on Africa. J Int AIDS Soc 2009; 2 (1): 9.
Health slips as the financial crisis grips [editorial]. Lancet 2009; 373 (9672): 1311.
Bateman C. Cash without capacity: the AIDS dilemma. S Afr Med J 2002; 92 (7): 488–9.
Bekker LG, Wood R. Blood safety: at what cost? JAMA 2006; 295 (5): 557–8.
Braithwaite RS, Tsevat J. Is antiretroviral therapy cost-effective in South Africa? PLoS Med 2006; 3 (1): e60.
Burns DG. Responsible use of scarce health care benefits. S Afr Med J 2007; 97 (1): 38–9.
Jaros GG, Boonzaier DA. Cost escalation in health-care technology: possible solutions. S Afr Med J 1993; 83 (6): 420–2.
Jaros GG, Muller JH. The cost and appropriateness of health care technology in South Africa: a plea for the development of a local medical equipment industry. S Afr Med J 1986; 69 (10): 625–7.
Kumaranayake L, Watts C. Economic costs of HIV/AIDS prevention activities in sub-Saharan Africa. AIDS 2000; 14 Suppl. 3: S239–52.
Leiman A, Standish B, Boting A, et al. Reducing the healthcare costs of urban air pollution: the South African experience. J Environ Manage 2007; 84 (1): 27–37.
McCoy D, Barron P. Cytological screening for cervical cancer: what are its opportunity costs? S Afr Med J 1996; 86 (8): 935–6.
Mooney G, Gilson L. The economic situation in South Africa and health inequities. Lancet 2009; 374 (9693): 858–9.
Nattrass NJ. The (political) economics of antiretroviral treatment in developing countries. Trends Microbiol 2008; 16 (12): 574–9.
Scotland GS, van Teijlingen ER, van der Pol M, et al. A review of studies assessing the costs and consequences of interventions to reduce mother-to-child HIV transmission in sub-Saharan Africa. AIDS 2003; 17 (7): 1045–52.
Walters L, Valodia B. Balancing access with cost and quality. S Afr Med J 2004; 94 (3): 173–4.
Worrall E, Morel C, Yeung S, et al. The economics of malaria in pregnancy: a review of the evidence and research priorities. Lancet Infect Dis 2007; 7 (2): 156–68.
Terris-Prestholt F, Vyas S, Kumaranayake L, et al. The costs of treating curable sexually transmitted infections in low- and middle-income countries: a systematic review. Sex Transm Dis 2006; 33 (10 Suppl.): S153–66.
Newell ML, Dabis F, Tolley K, et al. Cost-effectiveness and cost-benefit in the prevention of mother-to-child transmission of HIV in developing countries. Ghent International Working Group on Mother-to-Child Transmission of HIV. AIDS 1998; 12 (13): 1571–80.
Vassall A, Compernolle P. Estimating the resource needs of scaling-up HIV/AIDS and tuberculosis interventions in sub-Saharan Africa: a systematic review for national policy makers and planners. Health Policy 2006; 79 (1): 1–15.
Bremer JK. The cost of medical services: set the facts right [in Afrikaans]. S Afr Med J 1977; 52 (13): 508–9.
Geyer NM, Swanevelder JP, de Wit PW. Cost estimation of an intensive care unit [in Afrikaans]. S Afr Med J 1991; 80 (10): 491–3.
van de Wal BW. Expenditures on medicines at provincial hospitals in the Cape: a comparative analysis from 1982–1989 [in Afrikaans]. S Afr Med J 1991; 80 (11–12): 553–7.
Hotez PJ, Molyneux DH, Fenwick A, et al. Incorporating a rapid-impact package for neglected tropical diseases with programs for HIV/AIDS, tuberculosis, and malaria. PLoS Med 2006; 3 (5): e102.
Hensher M, Jefferys E. Financing blood transfusion services in sub-Saharan Africa: a role for user fees? Health Policy Plan 2000; 15 (3): 287–95.
Mock C, Nguyen S, Quansah R, et al. Evaluation of trauma care capabilities in four countries using the WHO-IATSIC Guidelines for Essential Trauma Care. World J Surg 2006; 30 (6): 946–56.
Eisler MC, Magona JW, Jonsson NN, et al. A low cost decision support tool for the diagnosis of endemic bovine infectious diseases in the mixed crop-livestock production system of sub-Saharan Africa. Epidemiol Infect 2007; 135 (1): 67–75.
Adam T, Lim SS, Mehta S, et al. Cost effectiveness analysis of strategies for maternal and neonatal health in developing countries. BMJ 2005; 331 (7525): 1107–13.
Bovier PA, Wyss K, Au HJ. A cost-effectiveness analysis of vaccination strategies against N. meningitidis meningitis in sub-Saharan African countries. Soc Sci Med 1999; 48 (9): 1205–20.
Brown N, Landon J. Antivenom: the most cost-effective treatment in the world? Toxicon 2010; 55 (7): 1405–7.
Chisholm D, Gureje O, Saldivia S, et al. Schizophrenia treatment in the developing world: an interregional and multinational cost-effectiveness analysis. B World Health Organ 2008; 86 (7): 542–51.
Coleman PG, Morel C, Shillcutt S, et al. A threshold analysis of the cost-effectiveness of artemisinin-based combination therapies in sub-saharan Africa. Am J Trop Med Hyg 2004; 71 (2 Suppl.): 196–204.
Ekwueme DU, Weniger BG, Chen RT. Model-based estimates of risks of disease transmission and economic costs of seven injection devices in sub-Saharan Africa. B World Health Organ 2002; 80 (11): 859–70.
Goodman CA, Coleman PG, Mills AJ. Changing the first line drug for malaria treatment: cost-effectiveness analysis with highly uncertain inter-temporal trade-offs. Health Econ 2001; 10 (8): 731–49.
Goodman CA, Coleman PG, Mills AJ. The cost-effectiveness of antenatal malaria prevention in sub-Saharan Africa. Am J Trop Med Hyg 2001; 64 (1–2 Suppl.): 45–56.
Guyatt HL, Snow RW, Evans DB. Malaria epidemiology and economics: the effect of delayed immune acquisition on the cost-effectiveness of insecticide-treated bednets. Philos Trans R Soc Lond B Biol Sci 1999; 354 (1384): 827–35.
Kirigia JM, Snow RW, Fox-Rushby J, et al. The cost of treating paediatric malaria admissions and the potential impact of insecticide-treated mosquito nets on hospital expenditure. Trop Med Int Health 1998; 3 (2): 145–50.
Marseille E, Kahn JG, Mmiro F, et al. The cost effectiveness of a single-dose nevirapine regimen to mother and infant to reduce vertical HIV-1 transmission in sub-Saharan Africa. Ann NY Acad Sci 2000; 918: 53–6.
Motala AA, Pirie FJ, Rauff S, et al. Cost-effective management of diabetes mellitus. Ethn Dis 2006; 16 (2 Suppl. 2): S2–79–84.
Patil AP, Okiro EA, Gething PW, et al. Defining the relationship between Plasmodium falciparum parasite rate and clinical disease: statistical models for disease burden estimation. Malar J 2009; 8: 186.
Shillcutt S, Morel C, Goodman C, et al. Cost-effectiveness of malaria diagnostic methods in sub-Saharan Africa in an era of combination therapy. B World Health Organ 2008; 86 (2): 101–10.
Stringer JS, Rouse DJ, Vermund SH, et al. Cost-effective use of nevirapine to prevent vertical HIV transmission in sub-Saharan Africa. J Acq Immun Def Synd 2000; 24 (4): 369–77.
Tediosi F, Maire N, Smith T, et al. An approach to model the costs and effects of case management of Plasmodium falciparum malaria in sub-Saharan Africa. Am J Trop Med Hyg 2006; 75 (2 Suppl.): 90–103.
Mansergh G, Haddix AC, Steketee RW, et al. Cost-effectiveness of short-course zidovudine to prevent perinatal HIV type 1 infection in a sub-Saharan African developing country setting. JAMA 1996; 276 (2): 139–45.
Marseille E, Kahn JG, Mmiro F, et al. Cost effectiveness of single-dose nevirapine regimen for mothers and babies to decrease vertical HIV-1 transmission in sub-Saharan Africa. Lancet 1999; 354 (9181): 803–9.
Affinnih YH. Revisiting sub-Saharan African countries’ drug problems: health, social, economic costs, and drug control policy. Subst Use Misuse 2002; 37 (3): 265–90.
Bell C, Devarajan S, Gersbach H. The long-run economic costs of AIDS: a model with an application to South Africa. World Bank Econ Rev 2006; 20 (1): 55–89.
Du Toit JP. A cost-effective but safe protocol for the staging of invasive cervical carcinoma in a third world country. Int J Gynecol Obstet 1988; 26 (2): 261–4.
Dyer SJ. The conflict between effective and affordable health care: a perspective from the developing world. Hum Reprod 2002; 17 (7): 1680–3.
Dirks JH, Levin NW. Dialysis rationing in South Africa: a global message. Kidney Int 2006; 70 (6): 982–4.
Gaziano TA. The South African Hypertension Guideline 2006 is evidence-based but not cost-effective. S Afr Med J 2006; 96 (11): 1170–3.
Goudge J, Gilson L, Russell S, et al. Affordability, availability and acceptability barriers to health care for the chronically ill: longitudinal case studies from South Africa. BMC Health Serv Res 2009; 9 (75): 1–19.
Goudge J, Gumede T, Gilson L, et al. Coping with the cost burdens of illness: combining qualitative and quantitative methods in longitudinal, household research. Scand J Public Health Suppl 2007; 69: 181–5.
Helleringer S, Kohler HP, Frimpong JA, et al. Increasing uptake of HIV testing and counseling among the poorest in sub-Saharan countries through home-based service provision. J Acq Immun Def Synd 2009; 51 (2): 185–93.
Koch S, Alaba O. On health insurance and household decisions: a treatment effect analysis. Soc Sci Med 2010; 70 (2): 175–82.
Maydell AT, Andronikou S, Ackermann C, et al. Comparison of paper print and soft copy reading in plain paediatric radiographs. J Med Imag Rad Oncol 2009; 53 (5): 459–66.
Schneider M, Norman R, Steyn N, et al. Estimating the burden of disease attributable to low fruit and vegetable intake in South Africa in 2000. S Afr Med J 2007; 97 (8 Pt 2): 717–23.
Stein DJ, Roberts M, Hollander E, et al. Quality of life and pharmaco-economic aspects of obsessive-compulsive disorder: a South African survey. S Afr Med J 1996; 86 (12 Suppl.): 1579, 1582–5.
Wilkinson D, Gouws E, Sach M, et al. Effect of removing user fees on attendance for curative and preventive primary health care services in rural South Africa. B World Health Organ 2001; 79 (7): 665–71.
Cotton MF. Antiretroviral therapy in children: increased benefit from increased complexity. S Afr Med J 2000; 90 (10): 985–8.
Bell E, Bell H, Socrates C, et al. A low-cost thermochromic thermometer to replace glass and mercury thermometers. Trop Doct 2002; 32 (3): 168–71.
van Walbeek C. A simulation model to predict the fiscal and public health impact of a change in cigarette excise taxes. Tob Control 2010; 19 (1): 31–6.
Benatar SR. Economics of health in South Africa: past, present and future. Med Law 1989; 8 (2): 111–7.
Lundkvist J, Kastang F, Kobelt G. The burden of rheumatoid arthritis and access to treatment: health burden and costs. Eur J Health Econ 2008; 8 Suppl. 2: S49–60.
Allard D, Burch VC. The cost of treating serious abdominal firearm-related injuries in South Africa. S Afr Med J 2005; 95 (8): 591–4.
Auvert B, Marseille E, Korenromp EL, et al. Estimating the resources needed and savings anticipated from rollout of adult male circumcision in Sub-Saharan Africa. PLoS One 2008; 3 (8): e2679.
Bachmann MO, Booysen FL. Health and economic impact of HIV/AIDS on South African households: a cohort study. BMC Public Health 2003; 3: 14.
Bachmann MO, Booysen FL. Economic causes and effects of AIDS in South African households. AIDS 2006; 20 (14): 1861–7.
Badri M, Maartens G, Mandalia S, et al. Cost-effectiveness of highly active antiretroviral therapy in South Africa. PLoS Med 2006; 3 (1): e4.
Bendavid E, Wood R, Katzenstein DA, et al. Expanding antiretroviral options in resource-limited settings: a cost-effectiveness analysis. J Acq Immun Def Synd 2009; 52(1): 106–13.
Biccard BM, Sear JW, Foex P. The pharmaco-economics of peri-operative beta-blocker and statin therapy in South Africa. S Afr Med J 2006; 96 (11): 1199–202.
Bradley SE, Prata N, Young-Lin N, et al. Cost-effectiveness of misoprostol to control postpartum hemorrhage in low-resource settings. Int J Gynecol Obstet 2007; 97 (1): 52–6.
Carabin H, Krecek RC, Cowan LD, et al. Estimation of the cost of Taenia solium cysticercosis in Eastern Cape Province, South Africa. Trop Med Int Health 2006; 11 (6): 906–16.
Clarke M, Dick J, Bogg L. Cost-effectiveness analysis of an alternative tuberculosis management strategy for permanent farm dwellers in South Africa amidst health service contraction. Scand J Public Health 2006; 34 (1): 83–91.
Collins DL, Leibbrandt M. The financial impact of HIV/AIDS on poor households in South Africa. AIDS 2007; 21 Suppl. 7: S75–81.
Dalvie MA, Sinanovic E, London L, et al. Cost analysis of ELISA, solid-phase extraction, and solid-phase micro-extraction for the monitoring of pesticides in water. Environ Res 2005; 98 (1): 143–50.
Dowdy DW, O’Brien MA, Bishai D. Cost-effectiveness of novel diagnostic tools for the diagnosis of tuberculosis. Int J Tuberc Lung Dis 2008; 12 (9): 1021–9.
Dyer JJ. Comparative costs of mobile and fixed-clinic primary health care services. S Afr Med J 1996; 86 (5): 528–30.
Dowdy DW, Sweat MD, Holtgrave DR. Country-wide distribution of the nitrile female condom (FC2) in Brazil and South Africa: a cost-effectiveness analysis. AIDS 2006; 20 (16): 2091–8.
Drennan G. Counting the cost of language services in psychiatry. S Afr Med J 1996; 86 (4): 343–5.
Edwards PR, Lunt DW, Fehrsen GS, et al. Improving cost-effectiveness of hypertension management at a community health centre. S Afr Med J 1998; 88 (5): 549–54.
Fairall L, Bachmann MO, Zwarenstein M, et al. Cost-effectiveness of educational outreach to primary care nurses to increase tuberculosis case detection and improve respiratory care: economic evaluation alongside a randomised trial. Trop Med Int Health 2010; 15 (3): 277–86.
Gaziano TA, Steyn K, Cohen DJ, et al. Cost-effectiveness analysis of hypertension guidelines in South Africa: absolute risk versus blood pressure level. Circulation 2005; 112 (23): 3569–76.
Geerts LT, Brand EJ, Theron GB. Routine obstetric ultrasound examinations in South Africa: cost and effect on perinatal outcome — a prospective randomised controlled trial. Br J Obstet Gynaecol 1996; 103 (6): 501–7.
Gillis LS, Koch A, Joyi M. The value and cost-effectiveness of a home-visiting programme for psychiatric patients. S Afr Med J 1990; 77 (6): 309–10.
Goldhaber-Fiebert JD, Denny LA, De Souza M, et al. Program spending to increase adherence: South African cervical cancer screening. PLoS One 2009; 4 (5): e5691.
Goldhaber-Fiebert JD, Denny LE, De Souza M, et al. The costs of reducing loss to follow-up in South African cervical cancer screening. Cost Eff Resour Alloc 2005; 3 (11): 1–9.
Goldie SJ, Gaffikin L, Goldhaber-Fiebert JD, et al. Cost-effectiveness of cervical-cancer screening in five developing countries. New Engl J Med 2005; 353 (20): 2158–68.
Goodman CA, Mnzava AE, Dlamini SS, et al. Comparison of the cost and cost-effectiveness of insecticide-treated bednets and residual house-spraying in KwaZulu-Natal, South Africa. Trop Med Int Health 2001; 6 (4): 280–95.
Goudge J, Gilson L, Russell S, et al. The household costs of health care in rural South Africa with free public primary care and hospital exemptions for the poor. Trop Med Int Health 2009; 14 (4): 458–67.
Griffiths UK, Botham L, Schoub BD. The cost-effectiveness of alternative polio immunization policies in South Africa. Vaccine 2006; 24 (29–30): 5670–8.
Gow JA. The adequacy of policy responses to the treatment needs of South Africans living with HIV (1999–2008): a case study. J Int AIDS Soc 2009; 12: 37.
Guerriero C, Cairns J, Jayaraman S, et al. Giving tranexamic acid to reduce surgical bleeding in sub-Saharan Africa: an economic evaluation. Cost Eff Resour Alloc 2010; 8 (1): 1.
Harling G, Bekker LG, Wood R. Cost of a dedicated ART clinic. S Afr Med J 2007; 97 (8): 593–6.
Hausler HP, Sinanovic E, Kumaranayake L, et al. Costs of measures to control tuberculosis/HIV in public primary care facilities in Cape Town, South Africa. B World Health Organ 2006; 84 (7): 528–36.
Hukins G, Boyce D. Containing medicines costs in the private sector: the example of a medical benefit scheme. S Afr Med J 1990; 78 (3): 152–4.
Hussey GD, Lasser ML, Reekie WD. The costs and benefits of a vaccination programme for Haemophilus influenzae type B disease. S Afr Med J 1995; 85 (1): 20–5.
Johnston K, Kennedy C, Murdoch I, et al. The cost-effectiveness of technology transfer using telemedicine. Health Policy Plan 2004; 19 (5): 302–9.
Kahn JG, Marseille E, Auvert B. Cost-effectiveness of male circumcision for HIV prevention in a South African setting. PLoS Med 2006; 3 (12): e517.
Kay BJ, Katzenellenbogen J, Fawcus S, et al. An analysis of the cost of incomplete abortion to the public health sector in South Africa: 1994. S Afr Med J 1997; 87 (4): 442–7.
Ker JA, Oosthuizen H, Rheeder P. Decision-making using absolute cardiovascular risk reduction and incremental cost-effectiveness ratios: a case study. Cardiovasc J Afr 2008; 19 (2): 97–101.
Kevany S, Meintjes G, Rebe K, et al. Clinical and financial burdens of secondary level care in a public sector antiretroviral roll-out setting (G. F. Jooste Hospital). S Afr Med J 2009; 99 (5): 320–5.
Lutge EE, Muirhead D. The epidemiology and cost of trauma to the orthopaedic department at a secondary-level hospital. S Afr J Surg 2005; 43 (3): 74–7.
Le Feuvre D, Taylor A. Endovascular treatment of cerebral aneurysms: a cost analysis. S Afr Med J 2004; 94 (12): 981–3.
Leisegang R, Cleary S, Hislop M, et al. Early and late direct costs in a Southern African antiretroviral treatment programme: a retrospective cohort analysis. PLoS Med 2009; 6 (12): e1000189.
Long L, Fox M, Sanne I, et al. The high cost of second-line antiretroviral therapy for HIV/AIDS in South Africa. AIDS 2010; 24 (6): 915–9.
Marseille E, Kahn JG, Billinghurst K, et al. Cost-effectiveness of the female condom in preventing HIV and STDs in commercial sex workers in rural South Africa. Soc Sci Med 2001; 52 (1): 135–48.
Marseille E, Kahn J, Saba J. Cost-effectiveness of antiviral drug therapy to reduce mother-to-child HIV transmission in sub-Saharan Africa. AIDS 1998; 12 (8): 939–48.
Marseille E, Dandona L, Marshall N, et al. HIV prevention costs and program scale: data from the PANCEA project in five low and middle-income countries. BMC Health Serv Res 2007; 7: 108.
Martinson N, Mohapi L, Bakos D, et al. Costs of providing care for HIV-infected adults in an urban HIV clinic in Soweto, South Africa. J Acq Immun Defic Syndr 2009; 50 (3): 327–30.
McConnel CE, Stanley N, du Plessis JA, et al. The cost of a rapid-test VCT clinic in South Africa. S Afr Med J 2005; 95 (12): 968–71.
McIntyre D, Valentine N, Cornell J. Private sector health care expenditure in South Africa. S Afr Med J 1995; 85 (3): 133–5.
Muheki C, McIntyre D, Barnes KI. Artemisinin-based combination therapy reduces expenditure on malaria treatment in KwaZulu Natal, South Africa. Trop Med Int Health 2004; 9 (9): 959–66.
Moodley I. Analysis of a medical aid administrator database for costs and utilisation of benefits by patients claiming for lipid-lowering agents. Cardiovasc J S Afr 2006; 17 (3): 140–5.
Norberg J, Nilsson T, Eriksson A, et al. The costs of a bullet: inpatient costs of firearm injuries in South Africa. S Afr Med J 2009; 99 (6): 442–4.
Olukoga A. Cost analysis of road traffic crashes in South Africa. Int J Injury Control Safe Promot 2004; 11 (1): 59–62.
Parrish A. Where does all the money go? An audit of cost and waste distribution in a second-tier peri-urban hospital. S Afr Med J 1997; 87 (10): 1365–70.
Price MR. A comparison of prescribing patterns and consequent costs at Alexandra Health Centre and in the private fee-for-service medical aid sector. S Afr Med J 1990; 78 (3): 158–60.
Rosen S, Long L, Fox M, et al. Cost and cost-effectiveness of switching from stavudine to tenofovir in first-line antiretroviral regimens in South Africa. J Acq Immun Def Synd 2008; 48 (3): 334–44.
Rosen S, Long L, Sanne I. The outcomes and outpatient costs of different models of antiretroviral treatment delivery in South Africa. Trop Med Int Health 2008; 13 (8): 1005–15.
Rydzak CE, Goldie SJ. Cost-effectiveness of rapid point-of-care prenatal syphilis screening in sub-Saharan Africa. Sex Transm Dis 2008; 35 (9): 775–84.
Schapera R. The economics of caring for the aged. S Afr Med J 1977; 51 (13): 431–3.
Sinanovic E, Moodley J, Barone MA, et al. The potential cost-effectiveness of adding a human papillomavirus vaccine to the cervical cancer screening programme in South Africa. Vaccine 2009; 27 (44): 6196–202.
Sinanovic E, Kumaranayake L. Financing and cost-effectiveness analysis of public-private partnerships: provision of tuberculosis treatment in South Africa. Cost Eff Resour Alloc 2006; 4: 11.
Sinanovic E, Kumaranayake L. Sharing the burden of TB/HIV? Costs and financing of public-private partnerships for tuberculosis treatment in South Africa. Trop Med Int Health 2006; 11 (9): 1466–74.
Smit J, Gray A, McFadyen L, et al. Counting the costs: comparing depot medroxyprogesterone acetate and norethisterone oenanthate utilisation patterns in South Africa. BMC Health Serv Res 2001; 1 (1): 4.
Soderlund N, Zwi K, Kinghorn A, et al. Prevention of vertical transmission of HIV: analysis of cost effectiveness of options available in South Africa. BMJ 1999; 318 (7199): 1650–6.
Soorapanth S, Sansom S, Bulterys M, et al. Cost-effectiveness of HIV rescreening during late pregnancy to prevent mother-to-child HIV transmission in South Africa and other resource-limited settings. J Acq Immun Def Synd 2006; 42 (2): 213–21.
Sherman GG, Matsebula TC, Jones SA. Is early HIV testing of infants in poorly resourced prevention of mother to child transmission programmes unaffordable? Trop Med Int Health 2005; 10 (11): 1108–13.
Skordis J, Nattrass N. Paying to waste lives: the affordability of reducing mother-to-child transmission of HIV in South Africa. J Health Econ 2002; 21 (3): 405–21.
Taylor SP, Klopper JM. South African health care expenditure, 1975–1984. S Afr Med J 1987; 72 (11): 802–4.
Thomas LS, Manning A, Holmes CB, et al. Comparative costs of inpatient care for HIV-infected and uninfected children and adults in Soweto, South Africa. J Acq Immun Def Synd 2007; 46 (4): 410–6.
Uys L, Hensher M. The cost of home-based terminal care for people with AIDS in South Africa. S Afr Med J 2002; 92 (8): 624–8.
Valli A, Ferrinho PD, Broomberg J, et al. Costs of primary health care at the Alexandra Health Centre. S Afr Med J 1991; 80 (8): 396–9.
Ferrinho P, Valli A. Cost of drugs at an urban primary health care centre in Alexandra, South Africa. Ann Soc Belg Med Trop 1994; 74 (4): 327–38.
van Wyk PJ, Kroon J, Holtshousen WS. Cost evaluation for the implementation of water fluoridation in Gauteng. SADJ 2001; 56 (2): 71–6.
Vickerman P, Terris-Prestholt F, Delany S, et al. Are targeted HIV prevention activities cost-effective in high prevalence settings? Results from a sexually transmitted infection treatment project for sex workers in Johannesburg, South Africa. Sex Transm Dis 2006; 33 (10 Suppl.): S122–32.
Vijayaraghavan A, Efrusy MB, Mazonson PD, et al. Cost-effectiveness of alternative strategies for initiating and monitoring highly active antiretroviral therapy in the developing world. J Acq Immun Def Synd 2007; 46 (1): 91–100.
Whittaker DE, le Roux I, Disler P. The cost effectiveness of the Philani Nutrition Day Centre in Crossroads squatter camp, Cape Town. S Afr Med J 1985; 68 (3): 174–6.
Wessels F, Green R, Luyt D. Cost of therapy for allergic rhinitis. S Afr Med J 1997; 87 (2): 141–5.
Wilkinson D, Floyd K, Gilks CF. Costs and cost-effectiveness of alternative tuberculosis management strategies in South Africa: implications for policy. S Afr Med J 1997; 87 (4): 451–5.
Wilkinson D, Floyd K, Gilks CF. Antiretroviral drugs as a public health intervention for pregnant HIV-infected women in rural South Africa: an issue of cost-effectiveness and capacity. AIDS 1998; 12(13): 1675–82.
Wilkins JJ, Folb PI, Valentine N, et al. An economic comparison of chloroquine and sulfadoxine-pyrimethamine as first-line treatment for malaria in South Africa: development of a model for estimating recurrent direct costs. Trans R Soc Trop Med Hyg 2002; 96 (1): 85–90.
Day K, Booyens S. The cost-effectiveness of managed care regarding chronic medicine prescriptions in a selected medical scheme. Curationis 1998; 21 (4): 65–70.
Anderson AN, Moodley I, Kropman K. A South African pharmaco-economic analysis of the Acute lnfarction Ramipril Efficacy (AIRE) study. Cardiovasc J S Afr 2000; 11 (2): 89–94.
Blecher MS, McIntyre D. Expenditure on health research in South Africa, 1991/1992. S Afr Med J 1995; 85 (5): 365–70.
Holtshousen WS, van Wyk PJ. Medical scheme expenditure on dental care: a smaller slice of the pie. J Dent Assoc S Afr 1997; 52 (10): 597–9.
Morris CN, Cheevers EJ. The direct costs of HIV/AIDS in a South African sugar mill. AIDS Anal Afr 2000; 10 (5): 7–8.
Sinanovic E, Floyd K, Dudley L, et al. Cost and cost-effectiveness of community-based care for tuberculosis in Cape Town, South Africa. Int J Tuberc Lung D 2003; 7 (9 Suppl. 1): S56–62.
Roux P, Henley L, Cotton M, et al. Burden and cost of inpatient care for HIV-positive paediatric patients: status in the Cape Town metropole during the second week of March 1999 — Paediatric HIV Census Group. S Afr Med J 2000; 90 (10): 1008–11.
Mickenautsch S, Munshi I, Grossman ES. Comparative cost of ART and conventional treatment within a dental school clinic. SADJ 2002; 57 (2): 52–8.
Holtshousen WS, Smit A. A cost-efficiency analysis of a mobile dental clinic in the public services. SADJ 2007; 62 (8): 334, 336–8, 340.
Yach D. Economic aspects of smoking in South Africa. S Afr Med J 1982; 62 (6): 167–70.
Patel DN, Lambert EV, da Silva R, et al. The association between medical costs and participation in the vitality health promotion program among 948,974 members of a South African health insurance company. Am J Health Promot 2010; 24 (3): 199–204.
Wessels F. Is fenofibrate a cost-saving treatment for middle-aged individuals with type 2 diabetes? A South African private-sector perspective. Cardiovasc J Afr 2010; 21 (1): 43–6.
Verguet S, Walsh J. Vaginal microbicides save money: a model of cost-effectiveness in South Africa and the USA. Sex Transm Infect 2010; 86 (3): 212–6.
Cleary SM, McIntyre D, Boulle AM. Assessing efficiency and costs of scaling up HIV treatment. AIDS 2008; 22 Suppl. 1: S35–42.
Lombard CJ, Stegman JC, Barnard A. Modelling net expenditure of hospitals in the Cape Province. S Afr Med J 1991; 80 (10): 508–10.
Wilkinson D, Sach ME. Cost-effective on-site screening for anaemia in pregnancy in primary care clinics. S Afr Med J 1997; 87 (4): 463–5.
Gavaza P, Shepherd M, Shcherbakova N, et al. The state of health economics and pharmaceoconomics research in Russia: a systematic review. J Pharm Health Serv Res 2010; 1(3): 113–21.
Teerawattananon Y, Russell S, Mugford M. A systematic review of economic evaluation literature in Thailand: are the data good enough to be used by policy-makers? Pharmacoeconomics 2007; 25 (6): 467–79.
Elixhauser A, Luce BR, Taylor WR, et al. Health care CBA/CEA: an update on the growth and composition of the literature. Med Care 1993; 31 (7 Suppl.): JS1–11, JS18–149.
Neumann PJ, Stone PW, Chapman RH, et al. The quality of reporting in published cost-utility analyses, 1976–1997. Ann Intern Med 2000; 132 (12): 964–72.
Elixhauser A, Halpern M, Schmier J, et al. Health care CBA and CEA from 1991 to 1996: an updated bibliography. Med Care 1998; 36 (5 Suppl.): MS1–9, MS18–147.
Lee KS, Brouwer WB, Lee SI, et al. Introducing economic evaluation as a policy tool in Korea: will decision makers get quality information? A critical review of published Korean economic evaluations. Pharmacoeconomics 2005; 23 (7): 709–21.
Walker D, Fox-Rushby JA. Economic evaluation of communicable disease interventions in developing countries: a critical review of the published literature. Health Econ 2000; 9 (8): 681–98.
Abt Associates, LoveLife. The impending catastrophe revisted: an update on the HIV/AIDS epidemic in South Africa. Parklands: LoveLife, Foundation HJKF, 2001.
Hensher M. Health sector impacts of HIV/AIDS: key issues for planning. Johannesburg: Department of Health Directorate of Health Financing and Economics, 2001.
Korenromp EL, Scano F, Williams BG, et al. Effects of human immunodeficiency virus infection on recurrence of tuberculosis after rifampin-based treatment: an analytical review. Clin Infect Dis 2003; 37 (1): 101–12.
Mqoqi N, Kellet P, Sitas F, et al. Incidence of histologically diagnosed cancer in South Africa 1998–1999. Johannesburg: National Cancer Registry of South Africa, 2004.
Drummond MF, Iglesias CP, Cooper NJ. Systematic reviews and economic evaluations conducted for the National Institute for Health and Clinical Excellence in the United Kingdom: a game of two halves? Int J Technol Assess Health Care 2008; 24 (2): 146–50.
Hopewell S, Loudon K, Clarke MJ, et al. Publication bias in clinical trials due to statistical significance or direction of trial results. Cochrane Database Syst Rev 2009 Jan 21; 1: MR000006.
Acknowledgements
The authors acknowledge the help rendered by The University of Texas at Austin library in accessing the articles used in the study. Some of the articles were accessed through the university’s inter-library loan facility. The authors have no conflicts of interest relevant to the content of this paper.
P. Gavaza and A.O. Oladapo reviewed and summarized all the articles included in the systematic review. S. Khoza acted as the tiebreaker for areas where P. Gavaza and A.O. Oladapo had conflicting views. P. Gavaza took the lead role in writing the manuscript with support from A.O. Oladapo. S. Khoza and K.L. Rascati helped to review and edit the manuscript. P. Gavaza came up with the idea to conduct the study and is the guarantor for the overall content of the article.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Gavaza, P., Rascati, K.L., Oladapo, A.O. et al. The State of Health Economic Research in South Africa. PharmacoEconomics 30, 925–940 (2012). https://doi.org/10.2165/11589450-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11589450-000000000-00000