Abstract
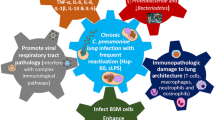
Asthma aetiology is complex, involving interactions between genetic susceptibility, allergen exposure and external aggravating factors such as air pollution, smoking and respiratory tract infections. Available evidence supports a role for acute Chlaymdia pneumoniae or Mycoplasma pneumoniae respiratory tract infection as a trigger for 5 to 30% of wheezing episodes and asthma exacerbations. It also appears that acute infections with C. pneumoniae and M. pneumoniae can initiate asthma in some previously asymptomatic patients; however, the quantitative role for these atypical bacteria as asthma initiators is unknown at the present time. Whether chronic infections with these agents play an important role in persistent asthma symptoms and/or to asthma severity is unclear and additional information should be acquired before definite conclusions can be reached. Improvement in asthma symptoms after antimicrobial therapy active against C. pneumoniae and M. pneumoniae has been observed. In some studies C. pneumoniae seems to be more important for asthma pathogenesis and exacerbations than M. pneumoniae; in other reports the role of M. pneumoniae appears to be more significant. However, a number of questions remain unanswered. Carefully controlled randomised trials are clearly warranted to determine whether infection with atypical bacteria is really associated with asthma and to define the appropriate role of antimicrobial treatment.

Similar content being viewed by others
References
Weiss KB, Wagener DK. Changing patterns of asthma mortality: identifying target populations at high risk. JAMA 1990; 264: 683–5
National Institutes of Health, National Heart, Lung, and Blood Institute. Expert Panel Report II: guidelines for the diagnosis and management of asthma. Bethesda (MD): US Department of Health and Human Services, Public Health Service, 1997 Feb
Silverman M, Wilson NM. Wheezing disorders in infancy. In: Silverman M, editor. Childhood asthma and other wheezing disorders. London: Chapman & Hall Medical, 1995: 141–74
Rusconi F, Galassi C, Corbo GM, et al. Risk factors for early, persistent, and late-onset wheezing in young children. Am J Respir Crit Care Med 1999; 160: 1617–22
The International Study of Asthma and Allergies in Childhood (ISAAC) Steering Committee. Worldwide variation in prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and atopic eczema. Lancet 1998; 351: 1225–32
Burr ML. Is asthma increasing? J Epidemiol Community Health 1987; 41: 185–9
Lewis S. ISAAC: a hypothesis generator for asthma? Lancet 1998; 351: 1220–1
Larsen GL. Asthma in children. N Engl J Med 1992; 326: 1540–5
Holgate ST. Asthma: past, present and future. Eur Respir J 1993; 6: 1507–20
Duff AL, Pomeranz ES, Gelber LE, et al. Risk factors for acute wheezing in infants and children: viruses, passive smoke, and IgE antibodies to inhalant allergens. Pediatrics 1993; 92: 535–40
Nelson HS, Szefler SJ, Jacobs J, et al. The relationships among environmental allergen sensitization, allergen exposure, pulmonary function, and bronchial hyperresponsiveness in the childhood asthma management program. J Allergy Clin Immunol 1999; 104: 775–85
Rona RJ, Duran-Tauleria E, Chinn S. Family size, atopic disorders in parents, asthma in children, and ethnicity. J Allergy Clin Immunol 1997; 99: 454–60
Jirapongsananuruk O, Leung DYM. Clinical applications of cytokines: new directions in the therapy of atopic disease. Ann Allergy Asthma Immunol 1997; 79: 5–16
Leung DYM. Immunologic basis of chronic allergic diseases: clinical messages from the laboratory bench. Pediatr Res 1997; 42: 559–68
McKenzie S. Clinical features and their assessment. In: Silverman M, editor. Childhood asthma and other wheezing disorders. London: Chapman & Hall Medical, 1995: 174–85
Martinez FD, Helms PJ. Types of asthma and wheezing. Eur Resp J 1998; 12Suppl. 27: 3–8S
Martinez FD, Wright AL, Taussig LM, et al. Asthma and wheezing in the first six years of life. N Engl J Med 1995; 332: 133–8
Nystad W, Stensrud T, Rijcken B, et al. Wheezing in school children is not always asthma. Pediatr Allergy Immunol 1999; 10: 58–65
Sigurs N, Bjanarson R, Sigurbergsson F, et al. Asthma and immunoglobulin E antibodies after respiratory syncytial virus bronchiolitis: a prospective cohort study with matched controls. Pediatrics 1995; 95: 500–5
Bjorcksten B, Borres MP, Einarsson R. Interleukin-4, soluble CD23 and interferon gamma levels in serum during the first 18 months of life. Int Arch Allergy Immunol 1995; 107: 34–6
Martinez FD. Viral infections and the development of asthma. Am J Respir Crit Care Med 1995; 151: 1644–8
Hahn DL. Infectious asthma: a reemerging clinical entity? J Fam Pract 1995; 41: 153–7
Newson R, Strachan D, Archibald E, et al. Acute asthma epidemics, weather and pollen in England, 1987–1994. Eur Resp J 1998; 11: 694–701
Busse WW. Role and contribution of viral respiratory infections to asthma. Allergy 1993; 48: 57–64
Hammerschlag MR. Atypical pneumonias in children. Adv Pediatr Infect Dis 1995; 10: 1–39
Blasi F, Cosentini R, Denti F, et al. Two family outbreaks of chlamydia pneumoniae infection. Eur Resp J 1994; 7: 102–4
Layani-Milon MP, Gras I, Valette M, et al. Incidence of upper respiratory tract mycoplasma pneumoniae infections among outpatients in Rhone-Alpes, France, during five successive winter periods. J Clin Microbiol 1999; 36: 1721–6
File TM, Tan JS, Plouffe JF. The role of atypical pathogens: mycoplasma pneumoniae, chlamydia pneumoniae, and legion-ella pneumophila in respiratory infection. Infect Dis Clin North Am 1998; 12: 569–92
Normann E, Gnarpe J, Gnarpe H, et al. Chlamydia pneumoniae in children with acute respiratory tract infections. Acta Paediatr 1998; 87: 23–7
Hahn DL, Dodge RW, Goulgjatnikov R. Association of chlamydia pneumoniae (strain TWAR) infection with wheezing, asthmatic bronchitis, and adult-onset asthma. JAMA 1991; 266: 225–30
Denny FW, Clyde WA, Glezen WP. Mycoplasma pneumoniae disease: clinical spectrum, pathophysiology, epidemiology, and control. J Infect Dis 1971; 123: 74–92
Hahn DL. Chlamydia pneumoniae, asthma, and COPD: what is the evidence? Ann Allergy Asthma Immunol 1999; 83: 271–92
Leinonen M. Pathogenetic mechanisms and epidemiology of chlamydia pneumoniae. Eur Heart J 1993; 14Suppl. K: 56–71
Redecke V, Dalhoff K, Bohnet S, et al. Interaction of chlamydia pneumoniae and human alveolar macrophages: infection and inflammatory response. Am J Respir Cell Mol Biol 1998; 19: 721–7
Grayston JT. Chlamydia pneumoniae (TWAR) infections in children. Pediatr Infect Dis J 1994; 13: 675–85
Ieven M, Ursi D, Van Bever H, et al. Detection of mycoplasma pneumoniae by two polymerase chain reactions and role of M. pneumoniae in acute respiratory tract infections in pediatric patients. J Infect Dis 1996; 173: 1445–52
Block S, Hedrick J, Hammerschlag MR, et al. Mycoplasma pneumoniae and chlamydia pneumoniae in pediatric community-acquired pneumonia: comparative efficacy and safety of clarithromycin vs erythromycin ethylsuccinate. Pediatr Infect Dis J 1995; 14: 471–7
Esposito S, Blasi F, Arosio C, et al. Lower respiratory tract infections in children: role of atypical pathogens. TIERS Annual Congress: 1999 9–13; Madrid, Spain. Eur Resp J 1999; 14Suppl. 30: 450S
Principi N, Esposito S. Comparative tolerability of erythromycin and newer macrolide antibacterials in paediatric patients. Drug Saf 1999; 20: 25–41
Roblin PM, Montalban G, Hammerschlag MR. Susceptibilities to clarithromycin and erythromycin of isolates of chlamydia pneumoniae from children with pneumonia. Antimicrob Agents Chemother 1994; 38: 1588–9
Taylor-Robinson D, Bebear C. Antibiotic susceptibilities of mycoplasmas and treatment of mycoplasmal infections. J Antimicrob Chemother 1997; 40: 622–30
Allegra L, Blasi F, Centanni S, et al. Acute exacerbations of asthma in adults: role of chlamydia pneumoniae infection. Eur Resp J 1994; 7: 2165–8
Resta O, Monno R, Saracino A, et al. Chlamydia pneumoniae infection in Italian patients. Monaldi Arch Chest Dis 1995; 50: 173–6
Dierckx JP, Gillard C. The results of pulmonary function tests in patients infected with mycoplasma pneumoniae. Infection 1976; 4Suppl. 1: 68–70
Huhti E, Mokka T, Nikoskelainen J, et al. Association of viral and mycoplasma infections with exacerbations of asthma. Ann Allergy 1974; 33: 145–9
Seggev JS, Lis I, Siman-Tou R, et al. Mycoplasma pneumoniae is a frequent cause of exacerbation of bronchial asthma in adults. Ann Allergy 1986; 57: 263–5
Berkovich S, Millian SJ, Snyder RD. The association of viral and mycoplasma infections with recurrence of wheezing in the asthmatic child. Ann Allergy 1970; 28: 43–9
Tipirneni P, Moore BS, Hyde JS, et al. IgE antibodies to mycoplasma pneumoniae in asthma and other atopic disease. Ann Allergy 1980; 45: 1–7
Gil JC, Mayagoitia BG, Paz MD. Isolation of mycoplasma pneumoniae from asthmatic patients. Ann Allergy 1993; 70: 23–5
Kraft M, Cassell GH, Henson JE, et al. Detection of mycoplasma pneumoniae in the airways of adults with chronic asthma. Am J Respir Crit Care Med 1998; 158: 998–1001
Kraft M, Cassell GH, Duffy LB, et al. Mycoplasma and chlamydia are present in the airways of chronic, stable asthmatics. American Thoracic Society International Conference; 1999 Apr 23–28; San Diego (CA). Am J Respir Crit Care Med 1999; 159Suppl. 3 (Pt 2): A517
Emre U, Roblin PM, Gelling M, et al. The association of chlamydia pneumoniae infection and reactive airway disease in children. Arch Pediatr Adolesc Med 1994; 148: 727–32
Cunningham AF, Johnston SL, Julious SA, et al. Chronic chlamydia pneumoniae infection and asthma exacerbations in children. Eur Resp J 1998; 11: 345–9
Johnston SL. Influence of viral and bacterial respiratory infections on exacerbations and symptom severity in childhood asthma. Pediatr Pulmonol 1997; 16: 88–9
Priickl PM, Aspock C, Makristathis A, et al. Polymerase chain reaction for detection of chlamydia pneumoniae in gargled-water specimens of children. Eur J Clin Microbiol Infect Dis 1995; 14: 141–4
Emre U, Sokolovskaya N, Roblin PM, et al. Detection of anti-chlamydia pneumoniae IgE in children with reactive airway disease. J Infect Dis 1995; 172: 265–7
Gnarpe J, Gnarpe H, Normann E, et al. Chlamydia pneumoniae, mycoplasma pneumoniae and mycoplasma fermentans PCR in children with acute respiratory tract infections. Proceedings of the 96th General Meeting of the American Society for Microbiology; 1996 May 19–23; New Orleans (LA)
Emre U, Bernius M, Roblin P, et al. Chlamydia pneumoniae infection in patients with cystic fibrosis. Clin Infect Dis 1996; 22: 819–23
Esposito S, Blasi F, Arosio C, et al. Importance of mycoplasma pneumoniae and chlamydia pneumoniae acute infection in children with recurrent wheezing. Proceedings of the 39th Interscience Conference on Antimicrobial Agents and Chemotherapy; 1999 Sep 26–29; San Francisco (CA)
Freymuth F, Vabret A, Brouard J, et al. Detection of viral, chlamydia pneumoniae and mycoplasma pneumoniae infections in exacerbations of asthma in children. J Clin Virol 1999; 13: 131–9
Sabato AR, Martin AJ, Marmion BP, et al. Mycoplasma pneumoniae: acute illness, antibiotics, and subsequent pulmonary function. Arch Dis Child 1984; 59: 1034–7
Mok JYQ, Waugh P, Simpson H. Mycoplasma pneumoniae infection: a follow-up study of 50 children with respiratory illness. Arch Dis Child 1979; 54: 506–11
Nagayama Y, Sakurai N. Clinical observations on lower respiratory tract infections with special reference to serum IgE levels. Pediatr Pulmonol 1991; 11: 44–8
Aldous MB, West S, Kimaro DN, et al. Chlamydia pneumoniae (TWAR) infection in Tanzanian children. Trop Doct 1996; 26: 18–9
Normann E, Gnarpe J, Gnarpe H, et al. Chlamydia pneumoniae in children attending day-care-centers in Gavle, Sweden. Pediatr Infect Dis J 1998; 17: 474–8
Hahn DL. Treatment of chlamydia pneumoniae infection in adult asthma: abefore-after trial. J Fam Pract 1995; 141: 345–51
Hahn D, Bukstein D, Luskin A, et al. Evidence for chlamydia pneumoniae infection in steroid-dependent asthma. Ann Allergy Asthma Immunol 1998; 80: 45–9
Kraft M, Hamid O, Cassell GH, et al. Mycoplasma and chlamydia cause increased airway inflammation that is responsive to clarithromycin. American Thoracic Society International Conference; 1999 Apr 23–28: San Diego (CA). Am J Respir Crit Care Med 1999; 1593 Suppl. (Pt 2): A517
Blasi F, Esposito S, Arosio C, et al. Association between intra-cellular pathogen infection and wheezing in children. American Thoracic Society International Conference; 1999 Apr 23–28; San Diego (CA). Am J Respir Crit Care Med 1999; 1593 Suppl. (Pt 2): A431
Hammerschlag MR, Chirgwin K, Roblin PM, et al. Persistent infection with chlamydia pneumoniae following acute respiratory illness. Clin Infect Dis 1992; 14: 178–82
Gendrel D, Raymond J, Moulin F, et al. Etiology and response to antibiotic therapy of community-acquired pneumonia in French children. Eur J Clin Microbiol Infect Dis 1997; 16: 388–91
Black PN. Anti-inflammatory effects of macrolide antibiotics. Eur Resp J 1997; 10: 971–2
Scaglione F, Rossoni G. Comparative anti-inflammatory effects of roxithromycin, azithromycin and clarithromycin. J Antimicrob Chemother 1998; 41Suppl. B: 47–50
Wales D, Woodhead M. The anti-inflammatory effects of macrolides. Thorax 1999; 54Suppl. 2: 58–62S
Thomson RJ. Laboratory diagnosis of respiratory infections. Curr Opin Infect Dis 1999; 12: 115–9
Heiskanen-Kosma T, Korppi M, Jokinen C, et al. Etiology of childhood pneumonia: serologic results of a prospective, population-based study. Pediatr Infect Dis J 1998; 17: 986–91
Ieven M, Goossens H. Relevance of nucleic acid amplification techniques for diagnosis of respiratory tract infections in the clinical laboratory. Clin Microbiol Rev 1997; 10: 242–56
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Esposito, S., Principi, N. Asthma in Children. Paediatr Drugs 3, 159–168 (2001). https://doi.org/10.2165/00128072-200103030-00001
Published:
Issue Date:
DOI: https://doi.org/10.2165/00128072-200103030-00001