Abstract
Background
When needle core biopsies (NCBs) of the breast reveal radial scar or complex sclerosing lesions (RSLs), excision is often recommended despite a low risk of malignancy in the modern era. The optimal management of NCBs revealing RSLs is controversial, and understanding of the natural history of unresected RSLs is limited.
Methods
We retrospectively analyzed pathology and imaging data from 148 patients with NCB revealing RSL without atypia from 2015 to 2019 to determine the prevalence of malignancy and the behavior of RSLs undergoing active surveillance (AS).
Results
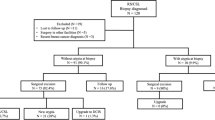
The mean age of patients was 52 years, and most lesions were screen-detected (91%). The median lesion size was 6.0 mm (range 2–39). Most patients (66%, n = 98) underwent immediate surgery, while 34% (n = 50) of patients underwent AS, with a median follow-up of 16 months (range 6–51). Of the excised RSLs, 99% (n = 97) were benign and 1% (n = 1) revealed ductal carcinoma in situ (DCIS). In 17% (n = 17) of cases, additional high-risk lesions were discovered upon excision. Among the 50 patients undergoing AS, no lesions progressed on interval imaging.
Conclusions
In this cohort, 99% of RSLs undergoing excision were benign, 1% revealed DCIS, and there were no invasive cancers. In the first study of patients with RSLs undergoing AS, we found that all lesions either remained stable or resolved. We propose that the vast majority of patients with RSL on NCB can be safely offered AS, and that routine excision is a low-value intervention.


Similar content being viewed by others
References
Davies JD. Diagnostic histopathology of the breast. O. L. Page and T. J. Anderson, with several contributors. Churchill Livingstone, Edinburgh, 1987. No. of pages: 362. Price: £65.00. ISBN: 0 443 02240 2. J Pathol. 1988;156(3):271–72.
Eusebi V, Millis RR. Epitheliosis, infiltrating epitheliosis, and radial scar. Semin Diagn Pathol. 2010;27(1):5–12.
Nielsen M, Jensen J, Andersen JA. An autopsy study of radial scar in the female breast. Histopathology. 1985;9(3):287–95.
Becker L, et al. Management of radial scars found at percutaneous breast biopsy. Can Assoc Radiol J. 2006;57(2):72–8.
Bianchi S, et al. Radial scar without associated atypical epithelial proliferation on image-guided 14-gauge needle core biopsy: analysis of 49 cases from a single-centre and review of the literature. Breast. 2012;21(2):159–64.
El-Sayed ME, et al. Predictive value of needle core biopsy diagnoses of lesions of uncertain malignant potential (B3) in abnormalities detected by mammographic screening. Histopathology. 2008;53(6):650–7.
Rakha EA, et al. Characterization and outcome of breast needle core biopsy diagnoses of lesions of uncertain malignant potential (B3) in abnormalities detected by mammographic screening. Int J Cancer. 2011;129(6):1417–24.
Leong RY, et al. Radial scar at percutaneous breast biopsy that does not require surgery. J Am Coll Surg. 2016;223(5):712–6.
Li Z, Ranade A, Zhao C. Pathologic findings of follow-up surgical excision for radial scar on breast core needle biopsy. Hum Pathol. 2016;48:76–80.
Phantana-Angkool A, et al. Rate of radial scars by core biopsy and upgrading to malignancy or high-risk lesions before and after introduction of digital breast tomosynthesis. Breast cancer research and treatment. 2019;173(1):23–9.
Farshid G, Buckley E. Meta-analysis of upgrade rates in 3163 radial scars excised after needle core biopsy diagnosis. Breast Cancer Res Treat. 2019;174(1):165–77.
The American Society of Breast Surgeons. Consensus guideline on concordance assessment of image-guided breast biopsies and management of borderline or high-risk Lesions. Columbia: American Society of Breast Surgeons; 2016. p. 1–13.
Eisenhauer EA, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45(2):228–47.
Chou WYY, Veis DJ, Aft R. Radial scar on image-guided breast biopsy: is surgical excision necessary? Breast Cancer Res Treat. 2018;170(2):313–20.
Kalife ET, et al. Clinical and radiologic follow-up study for biopsy diagnosis of radial scar/radial Sclerosing lesion without other Atypia. Breast J. 2016;22(6):637–44.
Mesa-Quesada J, et al. Radial scars without atypia in percutaneous biopsy specimens: can they obviate surgical biopsy? Radiologia. 2017;59(6):523–30.
Nakhlis F, et al. Complex sclerosing lesions and radial sclerosing lesions on core needle biopsy: Low risk of carcinoma on excision in cases with clinical and imaging concordance. Breast J. 2018;24(2):133–8.
Resetkova E, et al. Management of radial sclerosing lesions of the breast diagnosed using percutaneous vacuum-assisted core needle biopsy: recommendations for excision based on seven years’ of experience at a single institution. Breast Cancer Res Treat. 2011;127(2):335–43.
Thomas ET, Del Mar C, Glasziou P, Wright G, Barratt A, Bell KJL. Prevalence of incidental breast cancer and precursor lesions in autopsy studies: a systematic review and meta-analysis. BMC Cancer. 2017;17(1):808.
Acknowledgment
We thank our patients and their families, and members of the breast surgery, breast pathology, and breast radiology services at the breast center at New York-Presbyterian/Weill Cornell Medical Center for multidisciplinary care and helpful input into this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Elizabeth Kraft, Jessica N. Limberg, Katerina Dodelzon, Lisa A. Newman, Rache Simmons, Alexander Swistel, Paula S. Ginter, and Jennifer L. Marti declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kraft, E., Limberg, J.N., Dodelzon, K. et al. Radial Scars and Complex Sclerosing Lesions of the Breast: Prevalence of Malignancy and Natural History Under Active Surveillance. Ann Surg Oncol 28, 5149–5155 (2021). https://doi.org/10.1245/s10434-021-09713-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-021-09713-5