Abstract
Background
To optimize breast cancer care, the American College of Surgeons Commission on Cancer developed quality measures regarding receipt and timing of adjuvant radiotherapy (RT). Nationwide compliance with these measures and its impact on overall survival (OS) are evaluated herein.
Patients and Methods
Patients (n = 285,291) diagnosed with invasive breast cancer from 2004 to 2012 were identified from the National Cancer Database. Compliance with RT administration within 365 days from diagnosis was determined for patients with stage III disease with ≥ 4 positive lymph nodes post mastectomy and stage I–III disease post breast-conserving surgery (BCS). Univariate and multivariate logistic regression and Cox proportional hazard models were used to assess factors associated with compliance and OS, respectively.
Results
In the mastectomy cohort, 66.9% received timely RT, showing improved OS versus no RT patients (HR 0.70, 95% CI 0.67–0.73). Delayed RT patients (≥ 365 days) achieved equivalent OS to those receiving timely RT (HR 1.07, 95% CI 0.93–1.23) and superior OS to no RT patients (HR 0.74, 95% CI 0.65–0.85). In the BCS cohort, 89.4% received timely RT, showing improved OS versus no RT patients (HR 0.47, 95% CI 0.45–0.49). Delayed RT was associated with improved OS versus no RT (HR 0.64, 95% CI 0.56–0.74) and decreased OS versus timely RT (HR 1.37, 95% CI 1.19–1.58). Factors associated with noncompliance included insurance type and distance to hospital.
Conclusions
Quality measure compliance with adjuvant RT improves OS, regardless of timing after mastectomy. However, timeliness does impact OS after BCS. Focus on modifiable factors to improve compliance such as access to care may lead to improved compliance and OS.







Similar content being viewed by others
References
American Cancer Society. Cancer Facts and Figures 2018. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2018/cancer-facts-and-figures-2018.pdf. Accessed 29 Aug 2018.
Berry DA, Cronin KA, Plevritis SK, et al. Effect of screening and adjuvant therapy on mortality from breast cancer. N Enlg J Med. 2005;353:1784–92.
Otto SJ, Fracheboud J, Looman CW, et al. Initiation of population-based mammography screening in Dutch municipalities and effect on breast-cancer mortality: a systematic review. Lancet. 2003;361:1411–7.
Winchester DP. The National Accreditation Program for Breast Centers: quality improvement through standard setting. Surg Oncol Clin N Am. 2011;20:581–6.
Knutson AC, McNamara EJ, McKellar DP, et al. The role of the American College of Surgeons’ cancer program accreditation in influencing oncologic outcomes. J Surg Oncol. 2014;110:611–5.
American College of Surgeons Commission on Cancer. CoC Quality of Care Measures. 2018. https://www.facs.org/quality-programs/cancer/ncdb/qualitymeasures. Accessed 29 Aug 2018.
Berger ER, Wang CE, Kaufman CS, et al. National Accreditation Program for Breast Centers demonstrates improved compliance with post-mastectomy radiation therapy quality measure. J Am Coll Surg. 2017;224:236–44.
Darby S, McGale P, Correa C, et al. Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10,801 women in 17 randomised trials. Lancet. 2011;378:1707–16.
Overgaard M, Hansen PS, Overgaard J, et al. Postoperative radiotherapy in high-risk premenopausal women with breast cancer who receive adjuvant chemotherapy. Danish Breast Cancer Cooperative Group 82b Trial. N Engl J Med. 1997;337:949–55.
Overgaard M, Jensen MB, Overgaard J, et al. Postoperative radiotherapy in high-risk postmenopausal breast-cancer patients given adjuvant tamoxifen: Danish Breast Cancer Cooperative Group DBCG 82c randomised trial. Lancet. 1999;353:1641–8.
Ragaz J, Olivotto IA, Spinelli JJ, et al. Locoregional radiation therapy in patients with high-risk breast cancer receiving adjuvant chemotherapy: 20-year results of the British Columbia randomized trial. J Natl Cancer Inst. 2005;97:116–26.
Bleicher RJ. Timing and delays in breast cancer evaluation and treatment. Ann Surg Oncol. 2018;25:2829–38.
Recht A, Comen EA, Fine RE, et al. Postmastectomy radiotherapy: an American Society of Clinical Oncology, American Society for Radiation Oncology, and Society of Surgical Oncology focused guideline update. J Clin Oncol. 2016;34:4431–42.
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Breast Cancer. 2019. https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf. Accessed 2 Nov 2019.
Froud PJ, Mates D, Jackson JS, et al. Effect of time interval between breast-conserving surgery and radiation therapy on ipsilateral breast recurrence. Int J Radiat Oncol Biol Phys. 2000;46:363–72.
Olivotto IA, Lesperance ML, Truong PT, et al. Intervals longer than 20 weeks from breast-conserving surgery to radiation therapy are associated with inferior outcome for women with early-stage breast cancer who are not receiving chemotherapy. J Clin Oncol. 2009;27:16–23.
Punglia RS, Hughes ME, Edge SB, et al. Factors associated with guideline-concordant use of radiotherapy after mastectomy in the national comprehensive cancer network. Int J Radiat Oncol Biol Phys. 2008;72:1434–40.
Chu QD, Caldito G, Miller JK, Townsend B. Postmastectomy radiation for N2/N3 breast cancer: factors associated with low compliance rate. J Am Coll Surg. 2015;220:659–69.
Noone AM, Lund JL, Mariotto A, et al. Comparison of SEER treatment data with Medicare claims. Med Care. 2016;54:e55–64.
Acknowledgements
This manuscript has been presented in part at the Society of Surgical Oncology Annual Cancer Symposium and in part at the American Society of Breast Surgeons Annual Meeting in 2017. The manuscript is not under consideration for publication at another journal.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
No conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Figure 1
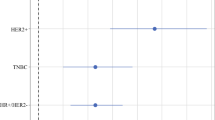
Forest plot. Multivariate Cox proportional hazard analysis of patient, tumor and treatment factors associated with improved overall survival in the BCS cohort – Stage I only (PDF 33 kb)
Supplementary Figure 2
Forest plot. Multivariate Cox proportional hazard analysis of patient, tumor and treatment factors associated with improved overall survival in the BCS cohort – Stage II only (PDF 33 kb)
Supplementary Figure 3
Forest plot. Multivariate Cox proportional hazard analysis of patient, tumor and treatment factors associated with improved overall survival in the BCS cohort – Stage III only (PDF 33 kb)
Rights and permissions
About this article
Cite this article
Zheleva, V., Nelson, R.A., Dumitra, S. et al. Time to Adjuvant Radiotherapy in Breast Cancer Affects Survival: Implications for the American College of Surgeons Commission on Cancer Quality Metrics. Ann Surg Oncol 27, 2614–2625 (2020). https://doi.org/10.1245/s10434-020-08326-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-020-08326-8