Abstract
Background
Skeletal muscle depletion (sarcopenia) is closely associated with limited physical ability and high mortality. This study was performed to evaluate the prognostic significance of skeletal muscle depletion in patients with resectable stage I–III colorectal cancer (CRC).
Methods
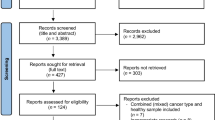
We conducted a retrospective analysis of 220 consecutive patients with stage I–III CRC who underwent curative resection. The skeletal muscle cross-sectional area was measured by preoperative computed tomography. The lowest sex-specific quartile of skeletal muscle mass was classified as sarcopenia. Factors contributing to recurrence-free survival (RFS) were analyzed by univariate and multivariate Cox proportional hazard models.
Results
Of 220 patients who met our inclusion criteria, 55 (25 %) had sarcopenia. The median follow-up duration was 41.4 months. Patients with sarcopenia were younger and had higher carcinoembryonic antigen levels than patients without sarcopenia. RFS and overall survival (OS) were significantly shorter in patients with sarcopenia than those without (5-year RFS, 56 vs. 79 %, log-rank p = 0.006; 5-year OS, 68 vs. 85 %, log-rank p = 0.015). Multivariate Cox regression analysis revealed that sarcopenia was independently associated with shorter RFS (hazard ratio [HR] 2.176; 95 % confidence interval [CI] 1.200–3.943; p = 0.010) and OS (HR 2.270; 95 % CI 1.147–4.494; p = 0.019). The influence of sarcopenia on patient outcome was modified by age at surgery (p value for interaction = 0.026); sarcopenia was associated with a poor prognosis, especially in young patients (log-rank p < 0.001).
Conclusions
Sarcopenia negatively impacts survival in patients undergoing curative resection for stage I–III CRC.



Similar content being viewed by others
References
Fearon K, Arends J, Baracos V. Understanding the mechanisms and treatment options in cancer cachexia. Nat Rev Clin Oncol. 2013;10:90-99.
Fearon K, Strasser F, Anker SD, et al. Definition and classification of cancer cachexia: an international consensus. Lancet Oncol. 2011;12:489-495.
Evans WJ. Skeletal muscle loss: cachexia, sarcopenia, and inactivity. Am J Clin Nutr. 2010;91:1123S-1127S.
Muscaritoli M, Anker SD, Argiles J, et al. Consensus definition of sarcopenia, cachexia and pre-cachexia: joint document elaborated by Special Interest Groups (SIG) “cachexia-anorexia in chronic wasting diseases” and “nutrition in geriatrics”. Clin Nutr. 2010;29:154-159.
van Vledder MG, Levolger S, Ayez N, et al. Body composition and outcome in patients undergoing resection of colorectal liver metastases. Br J Surg. 2012;99:550-557.
Prado CM, Lieffers JR, McCargar LJ, et al. Prevalence and clinical implications of sarcopenic obesity in patients with solid tumours of the respiratory and gastrointestinal tracts: a population-based study. Lancet Oncol. 2008;9:629-635.
Iritani S, Imai K, Takai K, et al. Skeletal muscle depletion is an independent prognostic factor for hepatocellular carcinoma. J Gastroenterol. doi:10.1007/s00535-014-0964-92014.
Voron T, Tselikas L, Pietrasz D, et al. Sarcopenia impacts on short- and long-term results of hepatectomy for hepatocellular carcinoma. Ann Surg. doi:10.1097/SLA.0000000000000743.
Sabel MS, Lee J, Cai S, et al. Sarcopenia as a prognostic factor among patients with stage III melanoma. Ann Surg Oncol. 2011;18:3579-3585.
Tan BH, Birdsell LA, Martin L, et al. Sarcopenia in an overweight or obese patient is an adverse prognostic factor in pancreatic cancer. Clin Cancer Res. 2009;15:6973-6979.
Lieffers JR, Bathe OF, Fassbender K, et al. Sarcopenia is associated with postoperative infection and delayed recovery from colorectal cancer resection surgery. Br J Cancer. 2012;107:931-936.
Hasselager R, Gögenur I. Core muscle size assessed by perioperative abdominal CT scan is related to mortality, postoperative complications, and hospitalization after major abdominal surgery: a systematic review. Langenbecks Arch Surg. 2014;399:287-295.
Baumgartner RN, Koehler KM, Gallagher D, et al. Epidemiology of sarcopenia among the elderly in New Mexico. Am J Epidemiol. 1998;147:755-763.
Dodson S, Baracos VE, Jatoi A, et al. Muscle wasting in cancer cachexia: clinical implications, diagnosis, and emerging treatment strategies. Annu Rev Med. 2011;62:265-279.
Richards CH, Roxburgh CS, MacMillan MT, et al. The relationships between body composition and the systemic inflammatory response in patients with primary operable colorectal cancer. PLoS One. 2012;7:e41883.
Richards CH, Leitch EF, Horgan PG, et al. The relationship between patient physiology, the systemic inflammatory response and survival in patients undergoing curative resection of colorectal cancer. Br J Cancer. 2010;103:1356-1361.
Roxburgh CS, Platt JJ, Leitch EF, et al. Relationship between preoperative comorbidity, systemic inflammatory response, and survival in patients undergoing curative resection for colorectal cancer. Ann Surg Oncol. 2011;18:997-1005.
McMillan DC, Canna K, McArdle CS. Systemic inflammatory response predicts survival following curative resection of colorectal cancer. Br J Surg. 2003;90:215-219.
Aleman MR, Santolaria F, Batista N, et al. Leptin role in advanced lung cancer. A mediator of the acute phase response or a marker of the status of nutrition? Cytokine. 2002;19:21-26.
Mitsiopoulos N, Baumgartner RN, Heymsfield SB, et al. Cadaver validation of skeletal muscle measurement by magnetic resonance imaging and computerized tomography. J Appl Physiol (1985). 1998;85:115-122.
Disclosure
Yuji Miyamoto, Yoshifumi Baba, Yasuo Sakamoto, Mayuko Ohuchi, Ryuma Tokunaga, Junji Kurashige, Yukiharu Hiyoshi, Shiro Iwagami, Naoya Yoshida, Megumi Yoshida, Masayuki Watanabe, and Hideo Baba declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Miyamoto, Y., Baba, Y., Sakamoto, Y. et al. Sarcopenia is a Negative Prognostic Factor After Curative Resection of Colorectal Cancer. Ann Surg Oncol 22, 2663–2668 (2015). https://doi.org/10.1245/s10434-014-4281-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-014-4281-6