Abstract
Background
Laparoscopic surgery is increasingly used in the treatment of colorectal cancer and more recently robotic assistance has been advocated. However, the learning curve to achieve surgical proficiency in laparoscopic surgery is ill-defined and subject to many influences. The aim of this review was to comprehensively appraise the literature on the learning curve for laparoscopic and robotic colorectal cancer surgery, and to quantify attainment of surgical proficiency and its implications in surgical clinical trial design.
Methods
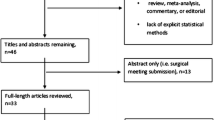
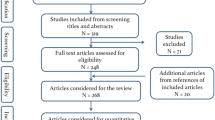
A systematic review using a defined search strategy was performed. Included studies had to state an explicit numerical value of the learning curve evaluated by a single parameter or multiple parameters.
Results
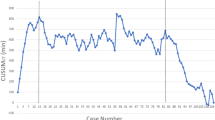
Thirty-four studies were included, 28 laparoscopic and 6 robot assisted. Of the laparoscopic studies, nine defined the learning curve on the basis of a single parameter. Nine studies used more than one parameter to define learning, and 11 used a cumulative sum (CUSUM) analysis. One study used both a multiparameter and CUSUM analysis. The definition of proficiency was subjective, and the number of operations to achieve it ranged from 5 to 310 cases for laparoscopic and 15–30 cases for robotic surgery.
Conclusions
The learning curve in laparoscopic colorectal surgery is multifaceted and often ill-defined, with poor descriptions of mentorship/supervision. Further, the quantification to attain proficiency is variable. The use of a single parameter to quantify this is simplistic. Multidimensional assessment is recommended; as part of this, the CUSUM model, which assesses trends in multiple surgical outcomes, is useful and appropriate when assessing the learning curve in a clinical setting.

Similar content being viewed by others
References
Phillips EH, Franklin M, Carroll BJ, Fallas MJ, Ramos R, Rosenthal D. Laparoscopic colectomy. Ann Surg. 1992;216:703–7.
Guillou P, Quirke P, Thorpe H, Walker J, Jayne D, Smith A, et al. Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet. 2005;365(9472):1718–26.
Lanfranco A, Castellanos A, Desai J, Meyers W. Robotic surgery: a current perspective. Ann Surg. 2004;239:14–21.
Smith A, Smith J, Jayne D. Telerobotics: surgery for the 21st century. Surgery. 2006;24:74–8.
Pigazzi A, Luca F, Patriti A, Valvo M, Ceccarelli G, Casciola L, et al. Multicentric study on robotic tumor-specific mesorectal excision for the treatment of rectal cancer. Ann Surg Oncol. 2010;17:1614–20.
Collinson F, Jayne D, Pigazzi A, Tsang C, Barrie J, Edlin R, et al. An international, multicentre, prospective, randomised, controlled, unblinded, parallel-group trial of robotic-assisted versus standard laparoscopic surgery for the curative treatment of rectal cancer. Int J Colorectal Dis. 2011;27:1–9.
The Clinical Outcomes of Surgical Therapy Study Group. A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med. 2004;350:2050–9.
Buunen M, Veldkamp R, Hop WC, Kuhry E, Jeekel J, Haglind E, et al. Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol. 2009;10:44–52.
Laparoscopic-assisted resection or open resection in treating patients with stage IIA, stage IIIA, or stage IIIB rectal cancer. NCT00726622. http://ClinicalTrials.gov.
Tekkis PP, Senagore AJ, Delaney CP, Fazio VW. Evaluation of the learning curve in laparoscopic colorectal surgery: comparison of right-sided and left-sided resections. Ann Surg. 2005;242:83–91.
Jayne DG, Thorpe H, Copeland J, Quirke P, Brown JM, Guillou PJ. Five-year follow-up of the Medical Research Council CLASICC trial of laparoscopically assisted versus open surgery for colorectal cancer. Br J Surg. 2010;97:1638–45.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med. 2009;151:65–94.
Critical appraisal skills programme: making sense of evidence about clinical effectiveness. http://www.caspinternational.org/mod_product/uploads/CASP_Case_Control_Checklist_14.10.10.pdf (2010). Accessed 1 May 2012.
Simons A, Anthone G, Ortega A. Laparoscopic-assisted colectomy learning curve. Dis Colon Rectum. 1995;38:600–3.
Wishner J, Baker J, Hoffman G, Hubbard G, Gould R, Wohlgemuth S, et al. Laparoscopic assisted colectomy. The learning curve. Surg Endosc. 1995;9:1179–83.
Agachan F, Joo JS, Sher M, Weiss EG, Nogueras JJ, Wexner SD. Laparoscopic colorectal surgery. Do we get faster? Surg Endosc. 1997;11:331–5.
Park JS, Kang SB, Kim SW, Cheon GN. Economics and the laparoscopic surgery learning curve: comparison with open surgery for rectosigmoid cancer. World J Surg. 2007;31:1827–34.
Kim J, Edwards E, Bowne W, Castro A, Moon V, Gadangi P, et al. Medial-to-lateral laparoscopic colon resection: a view beyond the learning curve. Surg Endosc. 2007;21:1503–7.
Akiyoshi T, Kuroyanagi H, Ueno M, Oya M, Fujimoto Y, Konishi T, et al. Learning curve for standardized laparoscopic surgery for colorectal cancer under supervision: a single-center experience. Surg Endosc. 2011;25:1409–14.
Agachan F, Joo JS, Weiss EG, Wexner SD. Intraoperative laparoscopic complications: are we getting better? Dis Colon Rectum. 1996;39:S14–9.
Begos DG, Arsenault J, Ballantyne GH. Laparoscopic colon and rectal surgery at a VA hospital. Surg Endosc. 1996;10:1050–6.
Chen G, Liu Z, Han P, Li JW, Cui BB. The learning curve for the laparoscopic approach for colorectal cancer: a single institution’s experience. J Laparoendosc Adv Surg Tech A. 2013;23:17–21.
Avital S, Hermon H, Greenberg R, Karin E, Skomick Y. Learning curve in laparoscopic colorectal surgery: our first 100 patients. Isr Med Assoc J. 2006;8:683–6.
Schlachta C, Mamazza J, Seshadri P, Cadeddu M, Gregoire R, Poulin E. Defining a learning curve for laparoscopic colorectal resections. Dis Colon Rectum. 2001;44:217–22.
Fukunaga Y, Higashino M, Tanimura S, Takemura M, Osugi H. Laparoscopic colorectal surgery for neoplasm. A large series by a single surgeon. Surg Endosc. 2008;22:1452–8.
Ito M, Sugito M, Kobayashi A, Nishizawa Y, Tsunoda Y, Saito N. Influence of learning curve on short-term results after laparoscopic resection for rectal cancer. Surg Endosc. 2009;23:403–8.
Kayano H, Okuda J, Tanaka K, Kondo K, Tanigawa N. Evaluation of the learning curve in laparoscopic low anterior resection for rectal cancer. Surg Endosc. 2011;25:2972–9.
Bennett CL, Stryker SJ, Ferreira MR, Adams J, Beart RW Jr. The learning curve for laparoscopic colorectal surgery: preliminary results from a prospective analysis of 1194 laparoscopic-assisted colectomies. Arch Surg. 1997;132:41–4.
Son GM, Kim JG, Lee JC, Suh YJ, Cho HM, Lee YS, Lee IK, Chun CS. Multidimensional analysis of the learning curve for laparoscopic rectal cancer surgery. J Laparoendosc Adv Surg Tech A. 2010;20:609–17.
Kuo LJ, Hung CS, Wang W, Tam KW, Lee HC, Liang HH, et al. Intersphincteric resection for very low rectal cancer: clinical outcomes of open versus laparoscopic approach and multidimensional analysis of the learning curve for laparoscopic surgery. J Surg Res. 2013;183:524–30.
Park I, Choi GS, Lim K, Kang B, Jun S. Multidimensional analysis of the learning curve for laparoscopic resection in rectal cancer. J Gastrointest Surg. 2009;13:275–81.
Dinçler S, Koller M, Steurer J, Bachmann L, Christen D, Buchmann P. Multidimensional analysis of learning curves in laparoscopic sigmoid resection. Dis Colon Rectum. 2003;46:1371–8.
Choi D, Jeong W, Lim SW, Chung T, Park JI, Lim SB, et al. Learning curves for laparoscopic sigmoidectomy used to manage curable sigmoid colon cancer: single-institute, three-surgeon experience. Surg Endosc. 2009;23:622–8.
Bege T, Lelong B, Esterni B, Turrini O, Guiramand J, Francon D, et al. The learning curve for the laparoscopic approach to conservative mesorectal excision for rectal cancer: lessons drawn from a single institution’s experience. Ann Surg. 2010;251:249–53.
Maeda T, Tan K, Konishi F, Tsujinaka S, Mizokami K, Sasaki J, et al. Accelerated learning curve for colorectal resection, open versus laparoscopic approach, can be attained with expert supervision. Surg Endosc. 2010;24:2850–4.
Li J, Lo A, Hon S, Ng S, Lee J, Leung K. Institution learning curve of laparoscopic colectomy—a multi-dimensional analysis. Int J Colorectal Dis. 2012;27:527–33.
Kye B, Kim J, Cho H, Kim H, Suh Y, Chun C. Learning curves in laparoscopic right-sided colon cancer surgery: a comparison of first-generation colorectal surgeon to advance laparoscopically trained surgeon. J Laparoendosc Adv Surg Tech A. 2011;21:789–96.
Mackenzie H, Miskovic D, Ni M, Parvaiz A, Acheson A, Jenkins J, et al. Clinical and educational proficiency gain of supervised laparoscopic colorectal surgical trainees. Surg Endosc. 2013;27:2704–11.
Bosker R, Groen H, Hoff C, Totte E, Ploeg R, Pierie JP. Early learning effect of residents for laparoscopic sigmoid resection. J Surg Educ. 2013;70:200–5.
Park I, Choi GS, Lim KH, Kang BM, Jun SH. Multidimensional analysis of the learning curve for laparoscopic colorectal surgery: lessons from 1,000 cases of laparoscopic colorectal surgery. Surg Endosc. 2009;23:839–46.
Jamali FR, Soweid AM, Dimassi H, Bailey C, Leroy J, Marescaux J. Evaluating the degree of difficulty of laparoscopic colorectal surgery. Arch Surg. 2008;143:762–7.
Sng KK, Hara M, Shin JW, Yoo BE, Yang KS, Kim SH. The multiphasic learning curve for robot-assisted rectal surgery. Surg Endosc. 2013;27:3297–307.
D’Annibale A, Pernazza G, Monsellato I, Pende V, Lucandri G, Mazzocchi P, et al. Total mesorectal excision: a comparison of oncological and functional outcomes between robotic and laparoscopic surgery for rectal cancer. Surg Endosc. 2013;27:1887–95.
Bokhari M, Patel C, Ramos-Valadez D, Ragupathi M, Haas E. Learning curve for robotic-assisted laparoscopic colorectal surgery. Surg Endosc. 2011;25:855–60.
Jiménez-Rodríguez R, Díaz-Pavón J, Portilla de Juan F, Prendes-Sillero E, Dussort H, Padillo J. Learning curve for robotic-assisted laparoscopic rectal cancer surgery. Int J Colorectal Dis. 2012;28:815–21.
Park J, Choi GS, Lim K, Jang Y, Jun S. S052: a comparison of robot-assisted, laparoscopic, and open surgery in the treatment of rectal cancer. Surg Endosc. 2011;25:240–8.
Kim YW, Lee HM, Kim NK, Min BS, Lee KY. The learning curve for robot-assisted total mesorectal excision for rectal cancer. Surg Laparosc Endosc Percutaneous Tech. 2012;22:400–5.
Chen W, Sailhamer E, Berger D, Rattner D. Operative time is a poor surrogate for the learning curve in laparoscopic colorectal surgery. Surg Endosc. 2007;21:238–43.
Schlachta CM, Mamazza J, Seshadri PA, Cadeddu MO, Poulin EC. Predicting conversion to open surgery in laparoscopic colorectal resections. Surg Endosc. 2000;14:1114–7.
Hoffman GC, Baker JW, Fitchett CW, Vansant JH. Laparoscopic-assisted colectomy. Initial experience. Ann Surg. 1994;219:732–43.
Pandya S, Murray JJ, Coller JA, Rusin LC. Laparoscopic colectomy: indications for conversion to laparotomy. Arch Surg. 1999;134:471–5.
Schwandner O, Schiedeck THK, Bruch HP. The role of conversion in laparoscopic colorectal surgery. Surg Endosc. 1999;13:151–6.
Marusch F, Gastinger I, Schneider C, Scheidbach H, Konradt J, Bruch H, et al. Experience as a factor influencing the indications for laparoscopic colorectal surgery and the results. Surg Endosc. 2001;15:116–20.
Le Moine MC, Fabre JM, Vacher C, Navarro F, Picot MC, Domergue J. Factors and consequences of conversion in laparoscopic sigmoidectomy for diverticular disease. Br J Surg. 2003;90:232–6.
Bouchard A, Martel G, Sabri E, Schlachta C, Poulin É, Mamazza J, et al. Does experience with laparoscopic colorectal surgery influence intraoperative outcomes? Surg Endosc. 2009;23:862–8.
Akmal Y, Baek JH, McKenzie S, Garcia-Aguilar J, Pigazzi A. Robot-assisted total mesorectal excision: is there a learning curve? Surg Endosc. 2012;26:2471–6.
Acknowledgment
Supported in part by the University of Leeds Flexibility and Sustainability Fund.
Disclosures
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Barrie, J., Jayne, D.G., Wright, J. et al. Attaining Surgical Competency and Its Implications in Surgical Clinical Trial Design: A Systematic Review of the Learning Curve in Laparoscopic and Robot-Assisted Laparoscopic Colorectal Cancer Surgery. Ann Surg Oncol 21, 829–840 (2014). https://doi.org/10.1245/s10434-013-3348-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-013-3348-0