Abstract
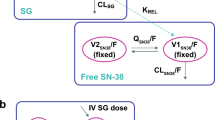
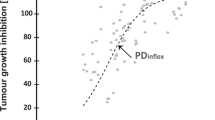
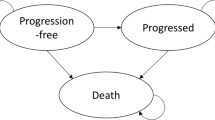
The aim of this evaluation was to predict tumour response to gemcitabine in patients with advanced pancreas or ovarian cancer using pre-clinical data obtained from xenograft tumour-bearing mice. The approach consisted of building a translational model combining pre-clinical pharmacokinetic–pharmacodynamic (PKPD) models and parameters, with dosing paradigms used in the clinics along with clinical PK models to derive tumour profiles in humans driving overall survival. Tumour growth inhibition simulations were performed using drug effect parameters obtained from mice, system parameters obtained from mice after appropriate scaling, patient PK models for gemcitabine and carboplatin, and the standard dosing schedules given in the clinical scenario for both types of cancers. Tumour profiles in mice were scaled by body weight to their equivalent values in humans. As models for survival in humans showed that tumour size was the main driver of the hazard rate, it was possible to describe overall survival in pancreatic and ovarian cancer patients. Simulated tumour dynamics in pancreatic and ovarian cancer patients were evaluated using available data from clinical trials. Furthermore, calculated metrics showed values (maximal tumour regression [0–17%] and tumour size ratio at week 12 with respect to baseline [− 9, − 4.5]) in the range of those predicted with the clinical PKPD models. The model-informed Drug Discovery and Development paradigm has been successfully applied retrospectively to gemcitabine data, through a semi-mechanistic translational approach, describing the time course of the tumour response in patients from pre-clinical studies.





Similar content being viewed by others
References
Kola I, Landis J. Can the pharmaceutical industry reduce attrition rates? Nat Rev Drug Discov. 2004;3:711–6.
Ait-Oudhia S, Mager DE. Array of translational systems pharmacodynamic models of anti-cancer drugs. J Pharmacokinet Pharmacodyn. 2016;43:549–65.
Zhang L, Pfister M, Meibohm B. Concepts and challenges in quantitative pharmacology and model-based drug development. AAPS J. 2008;10:552–9.
Zhang L, Sinha V, Forgue S, Callies S, Ni L, Peck R, et al. Model-based drug development: the road to quantitative pharmacology. J Pharmacokinet Pharmacodyn. 2006;33:369–93.
Rocchetti M, Simeoni M, Pesenti E, De Nicolao G, Poggesi I. Predicting the active doses in humans from animal studies: a novel approach in oncology. Eur J Cancer. 2007;43:1862–8.
Kerbel RS. Human tumor xenografts as predictive preclinical models for anticancer drug activity in humans: better than commonly perceived-but they can be improved. Cancer Biol Ther. 2003;2:S134–9.
Ruggeri BA, Camp F, Miknyoczki S. Animal models of disease: pre-clinical animal models of cancer and their applications and utility in drug discovery. Biochem Pharmacol. 2014;87:150–61.
Wong H, Choo EF, Alicke B, Ding X, La H, McNamara E, et al. Antitumor activity of targeted and cytotoxic agents in murine subcutaneous tumor models correlates with clinical response. Clin Cancer Res. 2012;18:3846–55.
Hui YF, Reitz J. Gemcitabine: a cytidine analogue active against solid tumors. Am J Health Pharm. 1997;54:162–70.
Storniolo AM, AllerheiligenS R, Pearce HL. Preclinical, pharmacologic, and phase I studies of gemcitabine. Semin Oncol. 1997;24:S7–2.
Garcia-Cremades M, Pitou C, Iversen PW, Troconiz IF. Characterizing gemcitabine effects administered as single agent or combined with carboplatin in mice pancreatic and ovarian cancer xenografts: a semimechanistic pharmacokinetic/pharmacodynamics tumor growth-response model. J Pharmacol Exp Ther. 2017;360:445–56.
Garcia-Cremades M, Pitou C, Iversen PW, Troconiz IF. Predicting tumour growth and its impact on survival in gemcitabine-treated patients with advanced pancreatic cancer. Eur J Pharm Sci. 2018;115:296–303.
Zecchin C, Gueorguieva I, Enas NH, Friberg LE. Models for change in tumour size, appearance of new lesions and survival probability in patients with advanced epithelial ovarian cancer. Br J Clin Pharmacol. 2016;82:717–27.
Joerger M, Huitema ADR, Richel DJ, Dittrich C, Pavlidis N, Briasoulis E, et al. Population pharmacokinetics and pharmacodynamics of paclitaxel and carboplatin in ovarian cancer patients: a study by the European organization for research and treatment of cancer-pharmacology and molecular mechanisms group and new drug development group. Clin Cancer Res. 2007;13:6410–8.
Tomayko MM, Reynolds CP. Determination of subcutaneous tumor size in athymic (nude) mice. Cancer Chemother Pharmacol. 1989;24:148–54.
Hahnfeldt P. Tumor development under angiogenic signaling: a dynamical theory of tumor growth, treatment response, and postvascular dormancy. Cancer Res. 1999;59:4770.
Elassaiss-Schaap J. Allometric scaling in oncology disease progression from xenograft tumor growth to human non-small-cell lung cancer. PAGE. 2010:19 Abstr 1907 [www.page-meeting.org/?abstract=1907]%0A.
Johnson JI, Decker S, Zaharevitz D, Rubinstein LV, Venditti JM, Schepartz S, et al. Relationships between drug activity in NCI preclinical in vitro and in vivo models and early clinical trials. Br J Cancer. 2001;84:1424–31.
Spilker ME, Chen X, Visswanathan R, Vage C, Yamazaki S, Li G, et al. Found in translation: maximizing the clinical relevance of nonclinical oncology studies. Clin Cancer Res. 2017;23(4):1080–90.
Lindauer A, Valiathan CR, Mehta K, Sriram V, de Greef R, Elassaiss-Schaap J, et al. Translational pharmacokinetic/pharmacodynamic modeling of tumor growth inhibition supports dose-range selection of the anti-PD-1 antibody pembrolizumab. CPT Pharmacometrics Syst Pharmacol. 2017;6:11–20.
Ouerdani A, Struemper H, Suttle A, Ouellet D, Ribba B. Preclinical modeling of tumor growth and angiogenesis inhibition to describe pazopanib clinical effects in renal cell carcinoma. CPT Pharmacometrics Syst Pharmacol. 2015;4:660–8.
Danhof M, de Lange ECM, Della Pasqua OE, Ploeger BA, Voskuyl RA. Mechanism-based pharmacokinetic-pharmacodynamic (PK-PD) modeling in translational drug research. Trends Pharmacol Sci. 2008;29:186–91.
Mager DE, Jusko WJ. Development of translational pharmacokinetic-pharmacodynamic models. Clin Pharmacol Ther. 2008;83:909–12.
Titze MI, Schaaf O, Hofmann MH, Sanderson MP, Zahn SK, Quant J, et al. An allometric pharmacokinetic/pharmacodynamics model for BI 893923, a novel IGF-1 receptor inhibitor. Cancer Chemother Pharmacol. 2017;79:545–58.
Zhu X, Shen X, Qu J, Straubinger RM, Jusko WJ. Multi-scale network model supported by proteomics for analysis of combined gemcitabine and birinapant effects in pancreatic cancer cells. CPT Pharmacometrics Syst Pharmacol. 2018;7:549–61.
van Kesteren C, Mathôt RAA, Beijnen JH, Schellens JHM. Pharmacokinetic-pharmacodynamic guided trial design in oncology. Investig New Drugs. 2003;21:225–41.
Barrett JS, Gupta M, Mondick JT. Model-based drug development applied to oncology. Expert Opin Drug Discov. 2007;2:185–209.
de Sousa Cavalcante L, Monteiro G. Gemcitabine: metabolism and molecular mechanisms of action, sensitivity and chemoresistance in pancreatic cancer. Eur J Pharmacol. 2014;741:8–16.
Binenbaum Y, Na’ara S, Gil Z. Gemcitabine resistance in pancreatic ductal adenocarcinoma. Drug Resist Updat. 2015;23:55–68.
Parra-Guillen ZP, Mangas-sanjuan V, Garcia-cremades M, Troconiz IF, Mo G, Pitou C, et al. Systematic modeling and design evaluation of unperturbed tumor dynamics in xenografts. J Pharmacol Exp Ther. 2018;366:96–104.
Thiel C, Schneckener S, Krauss M, Ghallab A, Hofmann U, Kanacher T, et al. A systematic evaluation of the use of physiologically based pharmacokinetic modeling for cross-species extrapolation. J Pharm Sci. 2015;104:191–206.
Eissing T, Kuepfer L, Becker C, Block M, Coboeken K, Gaub T, et al. A computational systems biology software platform for multiscale modeling and simulation: integrating whole-body physiology, disease biology, and molecular reaction networks. Front Physiol. 2011;2:4.
Acknowledgements
Support was received from the Innovative Medicines Initiative Joint Undertaking under grant agreement no 115156, resources of which are composed of financial contribution from the European Union’s Seventh Framework Programme (FP7/2007-2013) and the EFPIA companies’ in kind contribution. The DDMoRe project is also financially supported by contributions from the Academic and SME partners.
At the time the research was performed, Iñaki F Troconiz was an employee of the University of Navarra and Maria Garcia-Cremades was a PhD student from the University of Navarra. Celine Pitou and Philip W Iversen were employees of Elli Lilly and Company.
The authors would like to thank Sonya Tate for providing assistance during the writing process.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The first version of this manuscript was part of the thesis of Garcia-Cremades M and appears in dadun.unav.edu, a digital repository of the University of Navarra.
Electronic supplementary material
ESM 1
(PDF 5367 kb)
Rights and permissions
About this article
Cite this article
Garcia-Cremades, M., Pitou, C., Iversen, P.W. et al. Translational Framework Predicting Tumour Response in Gemcitabine-Treated Patients with Advanced Pancreatic and Ovarian Cancer from Xenograft Studies. AAPS J 21, 23 (2019). https://doi.org/10.1208/s12248-018-0291-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12248-018-0291-9