Abstract
Clinical evidence has linked intrauterine compromise such as fetal hypoxemia to poor neurologic outcome in the newborn. In this study we examined the effects of inducing chronic fetal hypoxemia by impairment of placental function on brain development in fetal sheep. Placental insufficiency was induced from 120 to 140 d of gestation (term = 145-148 d) by injection of microspheres into the umbilical circulation in five fetal sheep. Fetal partial pressure of oxygen, Pao2, was reduced from 24.1 ± 0.5 mm Hg before embolization to 14.8 ± 0.4 mm Hg after embolization (p< 0.05). In another three fetuses a similar level of hypoxemia(Pao2, 13.8 ± 0.4 mm Hg) occurred spontaneously. At 140 d of gestation the fetal brains were perfused with fixatives and compared with five control fetuses for the assessment of structural and immunohistochemical alterations. Hypoxemic fetuses demonstrated severe gliosis in the cerebral cortex and reduced myelination of subcortical white matter as visualized by glial fibrillary acidic protein and myelin basic protein staining, respectively (p < 0.05). White matter lesions were observed in two fetuses. The diameter of cerebral capillaries was increased in hypoxemic fetuses (p < 0.05), but there was no change in the number of nitric oxide synthase immunoreactive cells. Growth of neuronal processes was affected in the cerebellum, where there was also a reduction in the number of Purkinje neurons (p < 0.05). These results show that a prolonged period of placental insufficiency, resulting in moderate fetal hypoxemia during the last third of gestation, can affect neurodevelopmental processes that occur late in gestation such as myelination and growth of the cerebellum. This prenatal damage could affect neural connectivity and have functional consequences after birth.
Similar content being viewed by others
Main
Prolonged intrauterine stresses, such as those associated with placental insufficiency, can lead to chronic fetal hypoxemia and altered fetal endocrine status(1). In the human, such situations are thought to be associated with poor growth of the fetus and an increased risk of permanent neurologic disability(2). Previous experimental studies have shown detrimental effects on the fetal brain, such as selective neuronal loss and cerebral infarction, after severe acute episodes of either intrauterine asphyxia or cerebral hypoxia-ischemia(3–6). Other studies have shown that longer periods of fetal hypoxemia (8 h) in the sheep result in white matter injury with some cortical necrosis(7). A 12-h episode of placental underperfusion in the fetal sheep at midgestation results in mild focal damage in the cortical white matter and a reduction in the number of cerebellar Purkinje neurons and pyramidal cells in the hippocampus(8). However, few studies have examined the effects of hypoxemia through sustained periods of gestation on fetal brain development. Restriction of placental growth in sheep leads to chronic fetal hypoxemia, hypoglycemia, and intrauterine growth retardation(9). Affected fetuses demonstrate a reduction in the growth of neural processes in the cerebellum, motor and visual cortices, and the hippocampal formation, but show no white matter damage or cell loss(10). In the fetal guinea pig, growth-restricted as a result of reduced uterine blood flow, there is a delay in the initiation and extent of myelination in the corticospinal tract and an increase in gliosis(11).
The aim of this study was to examine the effects of chronic placental insufficiency on several aspects of brain development in fetal sheep. To induce placental insufficiency and fetal hypoxemia, the placental circulation was embolized for 20 d during the last third of gestation(12, 13). In fetal sheep, during this period of gestation, the brain is still growing, with the cerebellum in particular undergoing a period of accelerated growth(14). Other major developmental processes occurring during this gestational period include glial proliferation, myelination, and synaptogenesis(15). We used histologic and immunohistochemical techniques to describe structural and neurochemical changes in the brain after placental insufficiency. In particular, structural changes such as neuronal death and growth of neuronal processes were examined. The immunoreactivity of MBP and GFAP were investigated to demonstrate effects on myelination and the glial response, respectively. It has recently been suggested that NO produced by NOS containing neurons might play a role in the control of cerebral blood flow(16), which in the fetus, is known to be altered in response to prolonged hypoxemia(17). Therefore, we also examined cerebral vasculature and the expression of NOS immunoreactive cells in the cortex and striatum.
METHODS
Surgical Preparation
Thirteen pregnant sheep were subjected to aseptic surgery (halothane, 1-2% in O2) at 115 ± 2 d after mating (term = 145-148 d) as described in a companion study(12). Briefly, the uterus was exposed via a midline abdominal incision, and the fetal hindquarters were delivered through a uterine incision. A polyvinyl catheter was inserted into a fetal femoral artery so that its tip lay in the descending abdominal aorta below the level of the renal arteries but above the common umbilical artery. This catheter was used for both injection of microspheres and sampling of fetal blood. The correct position of the arterial catheter was confirmed at postmortem examination. Depomycin (procaine penicillin 20 mg/mL and dihydrostreptomycin 250 mg/mL) was administered (2 mL, i.m.) to the fetus before returning it to the uterus and closure of surgical incisions. After surgery, ewes were housed in individual cages with free access to food and water. Animals were allowed to recover for 5 ± 2 d after surgery before any experiments commenced.
Experimental Protocol
At 120 d of gestation in five randomly assigned fetuses we commenced the injections of microspheres into the aortic catheter to achieve umbilicoplacental embolization(12). Nonradiolabeled mucopolysaccharide microspheres (40-70 μm, Sephadex G-25, Superfine) 1% wt/vol were suspended in sterile heparinized saline containing 0.02% Tween 80(≈1 million spheres/mL) and injected into the femoral artery catheter. Injections were performed each day from 120 to 140 d of gestation, and the number of microspheres injected was adjusted to reduce the fetal Pao2 by approximately 8 mm Hg compared with preembolization and control values. Microspheres were injected only if the fetal Pao2 was greater than this value. Three other fetuses were found to be hypoxemic (Pao2 14.2± 1.3 mm Hg) immediately after surgery, and Pao2 remained low throughout the study period (120-140 d) without injection of microspheres, presumably as a result of placental insufficiency; these three fetuses have been described separately. Fetal arterial blood was sampled daily before, and after, each microsphere injection for the measurement of Pao2, Paco2, pH, O2 saturation (Radiometer, Denmark, ABL 510), as well as glucose and lactate concentrations (Yellow Springs Instruments, Yellow Springs, OH). Five control fetuses (five ewes) were subjected to surgery and blood gas sampling but no microspheres were injected; control fetuses were subjected to the same sampling regime as the experimental group. These experiments were approved by the Animal Ethical Committees of the University of Melbourne and Monash University.
Histology and Immunohistochemistry
At 140 d of gestation ewes and fetuses were killed by a maternal overdose of sodium pentobarbitone (130 mg/kg, i.v.). The fetal brains were perfused in situ with 4% paraformaldehyde in 0.1 M PB, removed, and weighed. Brains were post-fixed in 4% paraformaldehyde for 4 h and then transferred into 20% sucrose in 0.1 M PB overnight.
Serial coronal sections (40 μm) of the forebrain, including the cerebral cortex immediately posterior to the ansate sulcus, underlying white matter and striatum, and the ventral hippocampus and sagittal sections of the cerebellar vermis were cut on a freezing microtome. Every fifth section was mounted and stained with thionine (0.01%). The remaining sections were used for immunohistochemical analysis. Adjacent tissue blocks were processed for paraffin embedding. Sections from these blocks were cut at 8 μm and stained with acid fuchsin/thionine to demonstrate dying neurons(5). Small blocks of lobule 6 from the cerebellum and cortical white matter were collected and fixed in 1% glutaraldehyde and 4% paraformaldehyde in 0.1 M PB (pH 7.4) for 2 d and then postfixed in 1% osmium tetroxide for 4 h, stained with 2% (wt/vol) uranyl acetate, dehydrated in graded alcohols and epoxypropane, and embedded in Araldite. Semithin (1 μm) sections of the cerebellar tissue blocks were cut on an Ultra S microtome and stained with toluidine blue (1%) in 1% sodium tetraborate for light microscopic examination. Ultrathin sections (80 nm) were cut from cortical white matter and stained with uranyl acetate and lead citrate for electron microscopic analysis.
Immunoreactivity for MBP, GFAP, and NOS was localized on free-floating sections using the avidin-biotin peroxidase complex (Vector Laboratories) as previously described(11). Briefly, the sections were washed in 0.1 M PB, three time for 10 min each). To block for endogenous peroxidase activity, sections were incubated in 0.3% hydrogen peroxidase(H2O2) in methanol for 20 min. After washing in 0.1 M PB (three times, 10 min each), sections were placed in 10% BSA in 0.1 M PB (30 min) followed by incubation in an appropriate dilution of antisera and 0.1 M PB/2% BSA/0.3% Triton X-100 overnight at 4°C. The primary antibodies were obtained from the following sources and used at the following dilutions: mouse anti-monkey MBP (Boehringer Mannheim, 1:500) and rabbit anti-cow glial fibrillary acidic protein (DAKO, 1:1000). The rabbit anti-rat neuronal NOS antibody (amino acid sequence 1409-1429)(18), was used at 1:1000 dilution (kindly donated by Dr. Colin Anderson). The secondary antibody (biotinylated anti-rabbit IgG or anti-mouse IgG, 1:400) was added to the sections for 45 min followed by incubation in a 1:200 dilution of the avidin-biotin peroxidase complex for 45 min. After thorough washing, the sections were reacted with 0.05% 3,3′-diaminobenzidine solution for 10 min, after which 0.01% H2O2 was added for 6 min to produce a brown reaction product. Control and experimental material was stained at the same time to avoid procedural variation. To show nonspecific binding, additional control sections were processed as above except the primary antibody was omitted from the incubation solution.
Structural and Immunohistochemical Analysis
Cerebral cortex and underlying white matter. Five sections comprising the cerebral cortex and underlying white matter were viewed under both light and dark field illumination. Thionine-stained sections were examined for gross structural damage, with injury ranging from areas of pallor to necrosis and infarction. In adjacent paraffin sections stained with acid fuchsin/thionine, the presence or absence of dying neurons was noted. Qualitative analysis of the white matter was performed on thin Araldite sections using electron microscopy (Phillips CM12 transmission electron microscope).
White matter/gray matter ratios were determined in the cerebral cortex by projecting coronal sections at ×9 magnification using a microfiche reader and outlining the cortex. The white matter within this area was also traced. The respective areas were then digitized (measuring program V2.0, Kurta Graphic Tablet), and the white matter/gray matter ratio was calculated. The average from five measurements per animal was used for statistical comparison between experimental and control animals.
The number and diameter of cerebral capillaries were determined on sections comprising frontal cortex and underlying white matter. Four sections were chosen from each animal and projected at ×150 magnification, and every third field of view was selected for sampling. Blood vessel diameter was determined by measuring the smallest diameter of transected vessel profiles; thereby accounting for vessels cut tangentially. Approximately 1000 measurements were made per animal. To determine a density value of blood vessels, the total area sampled was determined by projecting sections at×9 under a microfiche reader and outlining the sections. The density of blood vessels (vessels/mm2) was calculated as total number of vessels counted ×3 (for every third field)/total area sampled.
NOS-positive neurons were counted in the cerebral cortex and subcortical white matter dorsal to the striatum and in the striatum, comprising both the caudate and putamen nuclei. Five subserial sections were selected from each animal, the area of interest was projected at ×300 magnification, and the number of NOS-positive cells was counted within an area of 0.4 mm2. Cell densities were calculated from an average of 20 measurements per section and expressed as number of NOS-positive cells/mm2.
The intensity of immunohistochemical staining of GFAP and MBP was determined by quantitative density measurements using the Optimas image analysis system (Optimas Corporation, Edmonds, WA). Before measuring, the image analysis system was calibrated using neutral density filters, dark field(infinite OD) and bright field (background lighting). All measurements were adjusted for uneven lighting and for background staining. Four sections stained with GFAP or MBP were selected from each animal, and 10 measurements of GFAP and five measurements of MBP were made randomly on each section throughout the cerebral cortex and white matter, respectively. The average density was determined per animal. The results are expressed as mean“log inverse gray values” within the area measured, which is proportional to the mean OD.
Hippocampus. To measure dendritic and axonal growth in the hippocampus, the width of the stratum oriens was measured on 10 thionine-stained sections of the CA1 and CA2 regions of the hippocampus from each animal. This layer contains apical dendrites of pyramidal cells. Sections were projected at ×300 magnification, and 10 evenly distributed sites along the CA1 and CA2 regions were sampled in each section, resulting in 100 measurements per animal.
Cerebellum. To determine the growth of neuronal processes in the cerebellum, the width of the molecular layer, which contains the dendrites of the Purkinje neurons, was measured in lobule 6. Lobule 6 was chosen as this region of the cerebellum matures later in development and has previously been shown to be affected in growth-restricted fetal sheep(10, 19). Thionine-stained sections of lobule 6 taken from around the midline of the cerebellar vermis were projected at×600 magnification. An automatic stage was used to select, in a raster fashion, about 30 sampling points in each section where the full width of the molecular layer was projected and measured. Seven sections were selected from each animal, resulting in a total of approximately 200 sampling points per animal.
The width of the external granule layer was measured on semithin Araldite sections. Ten sections per animal, at least 10 μm apart, were selected for measurements. Sections were projected at ×600, and 10 evenly spaced sites along the layer were selected. The width of the external granule layer was determined by measuring the length and area at each site and dividing the area by the length of each segment. The Purkinje cell body area was measured on the same sections by tracing around 20 randomly selected Purkinje cells per section. Purkinje cell densities in lobule 6 were determined on 10 thioninestained sections per animal. Sections were projected at ×150 magnification, and 10 evenly spaced lengths of transected Purkinje cell line were selected per section; Purkinje cells with a clearly defined nucleus were counted and the length determined. Cell densities per unit surface area(mm2) of Purkinje cell layer were determined by dividing the number of Purkinje cells/mm Purkinje cell line by the slab thickness (=mean diameter of Purkinje cell nucleus plus section thickness). In both experimental and control groups the mean diameter of the cell nucleus was approximately 14μm. Mitotic cells in the external granule layer were counted in semithin sections. Four sections from each animal were projected at ×60 magnification, and the mitotic cell densities per unit surface area(mm2) were calculated by multiplying the number of cells/mm by the width of the external granule layer.
Calculation of tissue shrinkage. Untreated fixed blocks of cerebral cortex and striatum from both control and hypoxemic fetuses were placed on slides and mounted on the stage of a projection microscope. The image of the block was projected onto a measuring tablet, and the surface area of the block was measured. Tissue blocks were then cut on a freezing microtome and mounted onto slides. The surface areas of the sections were remeasured and shrinkage was calculated. The average shrinkage was 1.9%. Because this change in surface area was negligible and there was a similar degree of shrinkage in all groups of animals, no corrections were made for shrinkage in morphometric analysis.
Statistical Analysis
All quantitative measurements were made on coded slides, and the codes were not disclosed until the measurements were completed. Statistical significance of differences between treatment groups was determined by the Mann-Whitney U test. No attempt was made to compare statistically the spontaneously hypoxemic animals with the other groups due to the small number of animals in that group. All data are presented as mean ± SEM.
RESULTS
All 13 fetuses entered into this study survived to 140 d of gestation and were available for histologic analysis. Values of fetal arterial pH, Paco2, Pao2, O2, saturation, glucose, and lactate concentrations and mean arterial pressure are summarized in Table 1; data are described in more detail in a companion study(12). Placental embolization resulted in fetal hypoxemia and hypoglycemia, and a small reduction in mean arterial pressure at 140 d, compared with control fetuses (Table 1). The three spontaneously hypoxemic fetuses were hypoxemic and hypoglycemic throughout the study period (Table 1). Body weights were reduced and brain weight/body weight ratios increased in embolized fetuses, but there was no change in either the total brain weight or cerebellar weight(Table 2).
Cerebral cortex and underlying white matter. No histologic damage was observed in control animals. Similarly, the majority of the embolized fetuses demonstrated no gross structural brain damage as visualized in thionine-stained sections (Fig. 1,A-C). Two embolized fetuses showed a poorly developed cortical gyral pattern compared with controls, resulting in wider than normal sulci. No significant difference in the white/gray matter ratio was observed between control and embolized fetuses(Table 3).
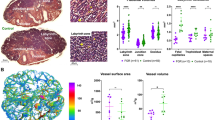
Photomicrographs of thionine-stained coronal sections of cerebral cortex, underlying white matter, and striatum in control(A and D), embolized (B and E), and spontaneously hypoxemic (C and F) fetal sheep at 140 d of gestation. Note white matter lesion indicated by arrows in(C). (D-F) Cerebral capillaries (arrows) in the white matter at a higher magnification. Vessels in the white matter from embolized (E) and spontaneously (F) hypoxemic fetuses appear dilated compared with control (D). White matter in(F) appears vacuolated and shows signs of degeneration. WM, white matter; Str, striatum. (A-C) bar = 5 mm; (D-F) bar = 130 μm.
Cerebral capillaries were distributed throughout the cortex and underlying white matter in all fetuses (Fig 1,A-C). There was no significant change in the number of cerebral capillaries, but the average diameter of the vessels was increased in embolized fetuses(Table 3 and Fig. 1, D-F). There was evidence of macrophages in some of the capillaries in one of the spontaneously hypoxemic animals.
In one of the spontaneously hypoxemic animals, selective acid fuchsin-positive cells were scattered throughout the cortex with the majority of dying cells in layer II (Fig. 2,A and B). In the same animal, two distinct areas of focal infarction were noted within layers III-VI of the cerebral cortex (Fig. 2C). Areas of pallor were also noted throughout the cortex indicating prior cell loss. Thionine-stained sections showed focal injuries to the white matter in one spontaneously hypoxemic fetus (Figs. 1C and 2D) and one embolized fetus (data not shown). In this spontaneously hypoxemic fetus, the presence of hemorrhage was noted in association with two areas of focal white matter lesions underlying the medial parietal cortex.
Photomicrographs of acid fuchsin/thionine-stained paraffin sections in a spontaneously hypoxemic animal. (A) The distribution of pyknotic cells (arrows) in layer II of the cerebral cortex is shown; these cells (arrows) are shown at higher magnification in (B). A focal cortical infarction (arrows) as observed in layers III-IV (C). (D) Lesion in the white matter (arrows) with associated hemorrhage (*). I-III cortical layers. (A) bars = 90 μm; (B) bar = 30 μm,(C) bar = 140 μm, (D) bar = 300 μm.
NOS-positive neurons were sparsely scattered throughout layers II-VI of the cortex and underlying white matter in control animals. The density of cells was higher in the striatum compared with the cortex (Table 3). Striatal cells were evenly distributed throughout the matrix with no cells observed in striosomes (Fig. 3,A and B). Immunoreactive cells were large and darkly stained with either multiple or bipolar processes as previously described in other species(16, 20, 21). The morphologic appearance and distribution of NOS cells in hypoxemic animals was similar to that observed in control animals (Fig. 3,C and D). There was no change in the number of NOS-positive neurons in either the cerebral cortex or the striatum in hypoxemic animals (Table 3). In both control and hypoxemic animals a proportion of the NOS-positive cells could be seen in the vicinity of cerebral capillaries (Fig 3,C and D).
Photomicrographs of nitric oxide synthase (NOS) immunoreactive cells in the striatum in control (A and C) and embolized hypoxemic (B and D) fetal sheep. The distribution and density of NOS-positive cells were similar in both groups. Note the presence of NOS-positive cells in the vicinity of cerebral capillaries. (A and B) Bar = 240 μm; (C and D) bar = 24 μm.
In control animals, the immunoreactivity for GFAP was most intense in layer I of the cortex, with only a few labeled cells scattered throughout the other cortical layers and around some blood vessels (Fig. 4A). There was moderate GFAP staining in the underlying white matter. In the embolized animals there was a marked increase in GFAP staining, which extended throughout all cortical layers (Fig. 4B). The spontaneously hypoxemic animals showed the most extreme GFAP reaction and the staining was very intense throughout the cortex (Fig. 4C). The underlying white matter also showed an increased GFAP immunoreactivity in the hypoxemic animals. Quantitative density measurements confirmed an increase in cortical GFAP staining in hypoxemic animals(Table 3).
Dark field photomicrographs of GFAP immunoreactivity(A-C) in the cerebral cortex and MBP immunoreactivity(D-F) in a cortical gyrus in control (A and D), embolized (B and E), and spontaneously hypoxemic(C and F) fetal sheep. Note the marked increase in GFAP staining in the hypoxemic animals and the reduction in intensity and extent of MBP staining. (A-C) bar = 120 μm; (D-F) bar = 320μm.
At 140 d of gestation, myelination was well advanced in the cortical white matter in control fetuses as judged by the intensity and extent of MBP immunoreactivity (Fig. 4D). In all regions examined, there was a dense core of immunoreactive fibers that extended into the gyri. In each gyrus, individual fibers branched off into the gray matter. In contrast, embolized (Fig. 4E) and spontaneously hypoxemic fetuses (Fig. 4F) in particular showed a reduction in the intensity of staining in the white matter; the length of the fibers extending toward the gray matter was shorter, and fibers were often fragmented. In some cases only a core of immunoreactive staining could be observed in the central white matter, and no fibers could be identified that extended into the gray matter. Quantitative density measurements confirmed that there was significantly less MBP in hypoxemic animals (Table 3). These results were further supported by qualitative electron microscopic examination, which revealed that, for a similar axon diameter, myelination was disproportionally thinner in the hypoxemic fetuses compared with controls (Fig. 5,A and B). In spontaneously hypoxemic fetuses myelination was severely affected; in addition to thin myelin sheaths there was evidence of degeneration and disorganization of myelin, and in some cases large vacuoles had formed between axon and the myelin sheaths (Fig. 5,C-E). The myelin around the vacuoles usually consisted of several lamellae and some of the unmyelinated axons of the surrounding neuropil also appeared swollen.
Electron micrographs of myelinated axons (A and B). Note that for a similar axon diameter the myelin sheath is thinner in the hypoxemic (B) compared with control (A) fetal sheep. (C-E) Severely affected myelin sheaths in a spontaneously hypoxemic animal are shown; vacuoles have formed between the axon sheaths (C) and abnormal loops of myelin (D), and degenerating myelin (E) was observed. (A and B) bar = 1.2 μm; (C) bar = 0.6 μm; (D) bar = 2.0 μm;(E) bar = 0.6 μm.
Cerebellum. The cerebellum showed no gross structural changes in either control or hypoxemic fetuses. The widths of the molecular layer and the external granule layer in lobule 6 of the cerebellum were significantly reduced in hypoxemic animals compared with controls (Fig. 6,A and B; Table 4). The number of Purkinje neurons was also reduced, but there was no change in the Purkinje cell body area. In the external granule layer there was a reduction in the number of mitotic cells.
Photomicrograph of semithin Araldite sections(toluidine blue) of the cerebellum (A-D) and paraffin sections(thionin/acid fuchsin) of the hippocampus (E and F) in control (A, C, and E) and hypoxemic (B, D, and F) fetal sheep. Comparison of control (A) and hypoxemic(B) illustrates the decrease in the width of the molecular layer in hypoxemic fetuses. The width of the external granular layer was also reduced in embolized fetuses (C, control; D, hypoxemic). Note mitosing granule cells (arrow in C). There was no difference in the width of the stratum oriens in the hippocampus between control (E) and hypoxemic (F) fetuses. Blood vessels appeared more dilated in the hypoxemic (F) compared with control(E) fetus. ML, molecular layer; EGL, external granule layer; PL, purkinje cell line; SO, stratum oriens;PL, pyramidale cell layer. (A and B) bar = 30μm; (C and D) bar = 14 μm; (E and F) bar = 90 μm.
Hippocampus. There were no gross morphologic changes, and no acidophilic neurons were observed in acid fuchsinstained sections of the hippocampus in any of the hypoxemic fetuses (Fig. 6,E and F). There was no difference in the width of the stratum oriens layer in the hippocampus in embolized (236 ± 10 μm) and spontaneously hypoxemic(235 ± 4 μm) fetuses compared with control fetuses (252 ± 16μm).
DISCUSSION
This study demonstrates that a period of sustained placental insufficiency and moderate fetal hypoxemia during the last third of gestation affects the developing sheep brain. The degree of fetal hypoxemia in this study was similar to that seen in the human growth-restricted fetus(22). Although there was a sparing of the brain in hypoxemic fetuses, such that there was no reduction in brain weight compared with controls, several aspects of brain development were affected. In particular, the growth of the cerebellum and myelination of cortical white matter showed changes after fetal hypoxemia. Furthermore, marked cortical gliosis and dilatation of blood vessels occurred in hypoxemic animals.
In general, there was no gross structural neuropathology in embolized fetuses, except for one animal that demonstrated a white matter lesion. However, an interesting observation in the most affected spontaneously hypoxemic fetus was the distribution of brain damage. This animal demonstrated frank lesions in the cerebral white matter, cortical infarctions, and selective neuronal loss throughout the cortex. In contrast, no dying neurons were observed in the hippocampus. Similar results have been seen after 8 h of fetal hypoxia(7). In contrast, after severe acute episodes of asphyxia in the fetal sheep, the hippocampus or basal ganglia appear to be the most vulnerable brain regions(4, 23). The brain injury after these acute insults is strongly correlated with the systemic hypotension that develops during the insult and the presumed concurrent cerebral underperfusion(24). In the present study a mild hypotension was present in embolized fetuses only at the end of the 20-d treatment period (Table 1), and the injury observed was likely to be related to hypoxemia. Axonal damage in the white matter after hypoxemia has been suggested to be mediated by excess entry of Ca2+, possibly via the Na+-Ca2+ exchanger(25). White matter, by virtue of the arrangement of its vascular supply, might also be particularly vulnerable to reductions in tissue oxygenation. In addition, the role of endocrine factors, such as cortisol, corticotropin, and noradrenaline, which are known to be altered in this experimental model of placental insufficiency, cannot be excluded(1). This finding emphasizes the importance of the insult paradigm in influencing the distribution of brain damage, and it suggests that, in at least the more mature fetus, chronic hypoxemic insults may be associated with cortical necrosis and white matter injury.
In addition to white matter lesions, a reduction in the staining of MBP was observed in the hypoxemic fetuses, suggesting that myelination was affected in this group. This was supported by the electron microscopic analysis showing thinner myelin sheaths. Furthermore, in two animals there were frank lesions in the white matter. Neuropathologic examination after intrauterine or neonatal death has shown an association between prenatal hypoxia-ischemia and cerebral white matter damage(26, 27). In the growth-retarded fetal guinea pig, myelination is both retarded and reduced(11). Similar results have been observed in the intrauterine growth-retarded rat(28). Several factors may play a role in the effects of placental insufficiency on myelination. Hypoxia is known to inhibit the synthesis of MBP in immature oligodendrocytes in vitro(29). Oligodendrocyte precursor cells are also known to be particularly vulnerable to reactive oxygen species after hypoxia(30) and glutamate toxicity(31). Furthermore, oligodendrocytes are known to be under the support of neurotrophic agents such as IGF-I(32). IGF-1 was not measured in the present study, but previous studies have found an association between fetal growth restriction after carunclectomy in sheep and low circulating concentrations of IGF-I and increased IGF binding protein 1 levels(33). Whether the systemic levels reflect the brain concentrations of these factors is not known, but it is possible that reduced brain IGF-I concentrations play a role in the reduction in myelination observed in the present study.
Reactive astrocytosis, as indicated by increased GFAP staining, was observed in the cerebral cortex in hypoxemic animals. This is in agreement with a number of previous studies that have found increased concentrations of GFAP in the cerebrospinal fluid in asphyxiated infants(34) and increased expression of reactive astrocytosis after hypoxic-ischemic insults in both neonatal(35) and adult animals(36), and after chronic hypoxia in adult rats(37). The intensity of the GFAP staining was increased and extended throughout all the cortical layers in hypoxemic animals. It is not clear whether this represents a proliferation or increased migration of cells or an up-regulation of the protein in resident astrocytes. The reactive astrocytosis appears to be a long-term effect(38); however, the exact role of astrocytosis after hypoxia remains unclear(39). Reactive astrocytes have been suggested to benefit injured neurons by a number of processes. For example, up-regulation of GFAP expression has been found in brain regions that show neuronal survival after hypoxia-ischemia(40, 41). Neurotrophic factors such as IGF-I(42), which is a neuronal rescue agent(43, 44), and basic fibroblast growth factor(45) are expressed in reactive astrocytes after transient forebrain ischemia. On the other hand, reactive astrocytes produce glial scarring after injury, which is likely to impair functional recovery(46). Furthermore, a recent study showed evidence of NOS in reactive astrocytes after hypoxia-ischemia(47). This may be beneficial as it could increase cerebral blood flow, or alternatively it could contribute to neuronal death as NO can be neurotoxic in high concentrations.
Nitric oxide-producing neurons are believed to play an important role in the regulation of cerebral blood flow. Anatomically, NOS-immunoreactive neurons are closely associated with the vasculature in rat and human retina(48). Similarly, neuronal NOS-labeled perivascular processes have been observed in both the human and rat brain(16, 49, 50). Inhibition of NOS prevents dilatation of cerebral microvessels(51) and reduces the hypoxemia-induced cerebral hyperemia in fetal sheep(52, 53). Therefore, we hypothesized that the cerebral vascular changes we saw may be associated with an increase in neuronal NOS staining. However, there was no change in the number of NOS-positive cells in the hypoxemic animals compared with controls, suggesting that other factors were involved. One such factor may be vascular endothelium growth factor. This growth factor has been shown to be induced in response to hypoxia and is thought to be involved in angiogenesis(54).
We found that the width of the molecular layer of the cerebellum was reduced in hypoxemic animals. This cell layer contains axons and dendrites of Purkinje neurons; therefore a reduction in this layer indicates that the growth of the Purkinje cell dendritic tree has been affected. This is in agreement with a previous study in growth-restricted fetal sheep which showed that there was a reduction in the total dendritic field size and in the branching density of the Purkinje neurons(14). There was also a reduction in the number of Purkinje neurons in hypoxemic animals compared with controls. This is likely due to the death of postmitotic cells, because Purkinje cell neurogenesis is complete at this stage of development. We also noted a reduction in the width of the external granular layer and a reduction in the number of cells undergoing mitosis. Under normal conditions the granule cells in this region migrate to the inner granule cell layer and form synapses with the Purkinje cell dendrites(55). Granule cell neurogenesis is at its peak at 100-120 d of gestation(14); therefore a reduction in the width of this layer in hypoxemic fetuses probably occurs as a result of both cell death and a decrease in mitotic activity. Thus our results indicate both cell death and impeded growth of processes in the cerebellum. In contrast to the cerebellum, in the hippocampus there was no evidence of attenuated growth of neuronal processes as determined by the lack of a change in the width of the stratum oriens layer, which contains the apical dendrites of the pyramidal neurons. There was also an absence of acidophilic neurons in the hippocampus. The cerebellum is a brain structure that develops later in gestation in relation to the hippocampus. In the fetal sheep, the most rapid expansion of the Purkinje cell dendritic tree occurs between 100 and 120 d of gestation, but it continues to grow until at least 3 months after birth(14). In contrast, the major growth period of the hippocampus occurs earlier in the sheep (S. Rees, unpublished observation). Therefore it can be expected that, owing to the hypoxemic insult occurring during late gestation, the cerebellum would be more affected in the present study.
In summary, we have shown that a period of chronic placental insufficiency, resulting in fetal hypoxemia and growth restriction, during the latter third of gestation can affect several aspects of brain development. In particular myelination in the cerebral white matter was reduced, and in the cerebellum there was evidence of cell death and attenuated dendritic growth. In addition severe astrocytosis was observed in hypoxemic fetuses. In general, the spontaneously hypoxemic fetuses appeared more affected in all parameters measured. This is presumably due to a longer period of placental insufficiency and hypoxemia than the 20 d which was induced in embolized fetuses although other underlying causes such as genetic or endocrine factors may also be involved. These prenatal developmental alterations could affect neuronal connectivity and have functional consequences in the newborn.
Abbreviations
- GFAP:
-
glial fibrillary acidic protein
- MBP:
-
myelin basic protein
- NOS:
-
nitric oxide synthase
- Paco2:
-
partial pressure of carbon dioxide
- Pao2:
-
partial pressure of oxygen
- PB:
-
phosphate buffer
References
Gagnon R, Challis J, Johnston L, Fraher L 1994 Fetal endocrine responses to chronic placental embolization in the late-gestation ovine fetus. Am J Obstet Gynecol 170: 929–938.
Marsal K, Ley D 1992 Intrauterine blood flow and postnatal neurological development in growth-retarded fetuses. Biol Neonate 62: 258–264.
Gunn AJ, Parer JT, Mallard EC, Williams CE, Gluckman PD 1992 Cerebral histologic and electrocorticographic changes after asphyxia in fetal sheep. Pediatr Res 31: 486–491.
Mallard EC, Gunn AJ, Williams CE, Johnston BM, Gluckman PD 1992 Transient umbilical cord occlusion causes hippocampal damage in the fetal sheep. Am J Obstet Gynecol 167: 1423–1430.
Williams C, Gunn AJ, Mallard C, Gluckman P 1992 Outcome after ischaemia in the developing sheep brain: an electroencephalographic and histological study. Ann Neurol 31: 14–21.
Mallard EC, Williams CE, Gunn AJ, Gunning MI, Gluckman PD 1993 Frequent episodes of brief ischemia sensitize the fetal sheep brain to neuronal loss and induce striatal injury. Pediatr Res 33: 61–65.
Penning DH, Grafe MD, Hammond R, Matsuda Y, Patrick J, Richardson B 1994 Neuropathology of the near-term and midgestation ovine fetal brain after sustained in utero hypoxemia. Am J Obstet Gynecol 170: 1425–1432.
Rees S, Harding R 1995 The effects of experimentally induced placental insufficiency on prenatal brain development. Dev Brain Dysfunct 8: 152–166.
Robinson JS, Kingston EJ, Jones CT, Thorburn GD 1979 Studies on experimental growth retardation in sheep. The effect of removal of endometrial caruncles on fetal size and metabolism. J Dev Physiol 1: 379–398.
Rees S, Bocking AD, Harding R 1988 Structure of the fetal sheep brain in experimental growth retardation. J Dev Physiol 10: 211–225.
Nitsos I, Rees S 1990 The effects of intrauterine growth retardation on the development of neuroglia in fetal guinea pigs. An immunohistochemical and an ultrastructural study. Int J Dev Neurosci 8: 233–244.
Cock ML, Harding R 1997 Renal and amniotic fluid responses to umbilicoplacental embolization for 20 days in fetal sheep. Am J Physiol 273:R1094–R1102.
Murotsuki J, Gagnon R, Matthews SG, Challis JR 1996 Effects of long-term hypoxemia on pituitary-adrenal function in fetal sheep. Am J Physiol 271:E678–E685.
Rees S, Harding R 1988 The effects of intrauterine growth retardation on the development of the Purkinje cell dendritic tree in the cerebellar cortex of fetal sheep: a note on the ontogeny of the Purkinje cell. Int J Dev Neurosci 6: 461–469.
Reynolds ML, Mollgard K 1985 The distribution of plasma protein in the neocortex and early allocortex of the developing sheep brain. Anat Embryol 171: 41–60.
Tomimoto H, Nishimura M, Suenaga T, Nakamura S, Akiguchi I, Wakita H, Kimura J, Mayer B 1994 Distribution of nitric oxide synthase in the human cerebral blood vessels and brain tissues. J Cereb Blood Flow Metab 14: 930–938.
Richardson BS, Carmichael L, Homan J, Patrick JE 1993 Cerebral oxidative metabolism in fetal sheep with prolonged and graded hypoxemia. J Dev Physiol 19: 77–83.
Anderson CR, Furness JB, Woodman HL, Edwards SL, Crack PJ, Smith AI 1995 Characterisation of neurons with nitric oxide synthase immunoreactivity that project to prevertebral ganglia. J Auton Nerv Syst 52: 107–116.
Altman J 1969 Autoradiographic and histological studies of postnatal neurogenesis. II. Dating the time of the production and onset of differentiation of cerebellar microneurons in rats. J Comp Neurol 136: 269–294.
Vincent SR, Kimura H 1992 Histochemical mapping of nitric oxide synthase in the rat brain. Neurosciences 46: 755–784.
Mizukawa K, Vincent SR, McGeer PL, McGeer EG 1989 Distribution of reduced-nicotinamide-adenine-dinucleotide-phosphate diaphorase-positive cells and fibers in the cat central nervous system. J Comp Neurol 279: 281–311.
Soothill PW, Nicolaides KH, Campbell S 1987 Prenatal asphyxia, hyperlacticaemia, hypoglycaemia, and erythroblastosis in growth retarded fetuses. Br Med J Clin Res Ed 294: 1051–1053.
Mallard EC, Waldvogel HJ, Williams CE, Faull RL, Gluckman PD 1995 Repeated asphyxia causes loss of striatal projection neurons in the fetal sheep brain. Neurosciences 65: 827–836.
Mallard EC, Williams CE, Johnston BM, Gunning MI, Davis S, Gluckman PD 1995 Repeated episodes of umbilical cord occlusion in fetal sheep lead to preferential damage to the striatum and sensitize the heart to further insults. Pediatr Res 37: 707–713.
Stys PK, Steffensen I 1996 Na(+)-Ca2+ exchange in anoxic/ischemic injury of CNS myelinated axons. Ann NY Acad Sci 779: 366–378.
Gaffney G, Squier MV, Johnson A, Flavell V, Sellers S 1994 Clinical associations of prenatal ischaemic white matter injury. Arch Dis Child Fetal Neonatal Ed 70: F101–106.
Squier M, Keeling JW 1991 The incidence of prenatal brain injury. Neuropathol Appl Neurobiol 17: 29–38.
Chanez C, Privat A, Flexor MA, Drian MJ 1985 Effect of intrauterine growth retardation on developmental changes in DNA and[14C]thymidine metabolism in different regions of the rat brain: Histological and biochemical correlations. Brain Res Dev Brain Res 21: 283–292.
Qi Y, Dawson G 1993 Effects of hypoxia on oligodendrocyte signal transduction. J Neurochem 61: 1097–1104.
Husain J, Juurlink BH 1995 Oligodendroglial precursor cell susceptibility to hypoxia is related to poor ability to cope with reactive oxygen species. Brain Res 698: 86–94.
Oka A, Belliveau MJ, Rosenberg PA, Volpe JJ 1993 Vulnerability of oligodendroglia to glutamate: pharmacology, mechanisms, and prevention. J Neurosci 13: 1441–1453.
McMorris FA, Smith TM, DeSalvo S, Furlanetto R 1986 Insulin like growth factor I/somatomedin C: A potent inducer of oligodendrocyte development. Proc Natl Acad Sci USA 83: 822–826.
Jones CT, Gu W, Harding JE, Price DA, Parer JY 1988 Studies on the growth of fetal sheep. Effect of surgical reduction in placental size or experimental manipulation of uterine blood flow on plasma sulphation promoting activity on the concentration of insulin like growth factors I and II. J Dev Physiol 10: 179–189.
Blennow M, Hagberg H, Rosengren L 1995 Glial fibrillary acidic protein in the cerebrospinal fluid: a possible indicator of prognosis in full-term asphyxiated newborn infants?. Pediatr Res 37: 260–264.
Burtrum D, Silverstein FS 1994 Hypoxic-ischemic brain injury stimulates glial fibrillary acidic protein mRNA and protein expression in neonatal rats. Exp Neurol 126: 112–118.
Kindy MS, Bhat AN, Bhat NR 1992 Transient ischemia stimulates glial fibrillary acid protein and vimentin gene expression in the gerbil neocortex, striatum and hippocampus. Brain Res Mol Brain Res 13: 199–206.
Zimmer C, Sampaolo S, Sharma HS, Cervos Navarro J 1991 Altered glial fibrillary acidic protein immunoreactivity in rat brain following chronic hypoxia. Neurosciences 40: 353–361.
Romijn HJ, Janszen AW, Van den Bogert C 1994 Permanent increase of immunocytochemical reactivity for γ-aminobutyric acid(GABA), glutamic acid decarboxylase, mitochondrial enzymes, and glial fibrillary acidic protein in rat cerebral cortex damaged by early postnatal hypoxia-ischemia. Acta Neuropathol 87: 612–627.
Eddleston M, Mucke L 1993 Molecular profile of reactive astrocytes-implications for their role in neurologic disease. Neurosciences 54: 15–36.
Li Y, Chopp M, Zhang ZG, Zhang RL 1995 Expression of glial fibrillary acidic protein in areas of focal cerebral ischemia accompanies neuronal expression of 72-kDa heat shock protein. J Neurol Sci 128: 134–142.
Kato H, Kogure K, Araki T, Itoyama Y 1994 Astroglial and microglial reactions in the gerbil hippocampus with induced ischemic tolerance. Brain Res 664: 69–76.
Gluckman P, Klempt N, Guan J, Mallard C, Sirimanne E, Dragunow M, Klempt M, Singh K, Williams C, Nikolics K 1992 A role for IGF-1 in the rescue of CNS neurons following hypoxic-ischemic injury. Biochem Biophysiol Res Commun 182: 593–599.
Guan J, Williams C, Gunning M, Mallard C, Gluckman P 1993 The effects of IGF-1 treatment after hypoxic-ischemic brain injury in adult rats. J Cereb Blood Flow Metab 13: 609–616.
Johnston BM, Mallard EC, Williams CE, Gluckman PD 1996 Insulin-like growth factor-1 is a potent neuronal rescue agent after hypoxic-ischemic injury in fetal lambs. J Clin Invest 97: 300–308.
Takami K, Iwane M, Kiyota Y, Miyamoto M, Tsukuda R, Shiosaka S 1992 Increase of basic fibroblast growth factor immunoreactivity and its mRNA level in rat brain following transient forebrain ischemia. Exp Brain Res 90: 1–10.
Reier PJ, Stensaas LJ, Guth L 1983 The astrocytic scar as an impediment to regeneration in the central nervous system. In: Kao CC, Bunge RP, Reier PJ (eds) Spinal Cord Reconstruction. Raven Press, New York, pp 163–195.
Endoh M, Maiese K, Pulsinelli WA, Wagner JA 1993 Reactive astrocytes express NADPH diaphorase in vivo after transient ischemia. Neurosci Lett 154: 125–128.
Roufail E, Stringer M, Rees S 1995 Nitric oxide synthase immunoreactivity and NADPH diaphorase staining are co-localised in neurons closely associated with the vasculature in rat and human retina. Brain Res 684: 36–46.
Iadecola C, Beitz AJ, Renno W, Xu X, Mayer B, Zhang F 1993 Nitric oxide synthase-containing neural processes on large cerebral arteries and cerebral microvessels. Brain Res 606: 148–155.
Minami Y, Kimura H, Aimi Y, Vincent SR 1994 Projections of nitric oxide synthase-containing fibers from the sphenopalatine ganglion to cerebral arteries in the rat. Neurosciences 60: 745–759.
Kobari M, Fukuuchi Y, Tomita M, Tanahashi N, Konno S, Takeda H 1994 Dilatation of cerebral microvessels mediated by endothelin ETB receptor and nitric oxide in cats. Neurosci Lett 176: 157–160.
Marks KA, Mallard EC, Roberts I, Williams CE, Gluckman PD, Edwards AD 1996 Nitric oxide synthase inhibition attenuates delayed vasodilation and increases injury after cerebral ischemia in fetal sheep. Pediatr Res 40: 185–191.
McCrabb GJ, Harding R 1996 Role of nitric oxide in the regulation of cerebral blood flow in the ovine foetus. Clin Exp Pharmacol Physiol 23: 855–860.
Shweiki D, Itin A, Soffer D, Keshet E 1992 Vascular endothelial growth factor induced by hypoxia may mediate hypoxia-initiated angiogenesis. Nature 359: 843–845.
Rakic P 1969 Neuron-glia relationship during granule cell migration in developing cerebellar cortex. A Golgi and electronmicroscopic study in Macacus Rhesus. J Comp Neurol 141: 283–312.
Acknowledgements
The authors thank Dr. R. Dilley for his helpful advice on image analysis.
Author information
Authors and Affiliations
Additional information
Supported by the National SIDS Foundation of Australia and the National Health and Medical Research Council of Australia.
Rights and permissions
About this article
Cite this article
Mallard, E., Rees, S., Stringer, M. et al. Effects of Chronic Placental Insufficiency on Brain Development in Fetal Sheep. Pediatr Res 43, 262–270 (1998). https://doi.org/10.1203/00006450-199802000-00018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199802000-00018
This article is cited by
-
Environmental Enrichment Protects Offspring of a Rat Model of Preeclampsia from Cognitive Decline
Cellular and Molecular Neurobiology (2023)
-
Neuroplacentology in congenital heart disease: placental connections to neurodevelopmental outcomes
Pediatric Research (2022)
-
Volumetric MRI study of the intrauterine growth restriction fetal brain
European Radiology (2017)
-
Vigour in West African Dwarf kids within the first 24 h post-partum
Tropical Animal Health and Production (2017)
-
White matter injury in the preterm infant: pathology and mechanisms
Acta Neuropathologica (2017)