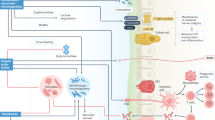
Abstract
One hundred twenty low birth weight infants were enterally fed diets containing fixed differences in protein and energy content. Serial, biweekly measurements were made of metabolizable energy intake, energy expenditure, nitrogen balance, and distribution of states of sleep, from the time the infants were receiving full enteral intakes (180 mL/kg·d) until weight reached 2200 g. Using multiple regression analysis of energy expenditure against protein stored, and metabolizable energy, the energy expended in the deposition of protein was calculated to be 5.5 kcal/g ± 1.1 kcal/g (SE) and the energy cost of fat deposited was 1.6 kcal/g ± 0.3 kcal/g (SE). Estimated maintenance energy expenditure of the nongrowing low birth weight infant was 42.3 ± 3.2 kcal/kg/d. Variations in distribution of sleep state, an assessment of the activity state of the infant, did not explain additional variability in energy expenditure, after adjusting for protein and energy storage.
Similar content being viewed by others
Main
The development of techniques for the accurate determination of energy balance of LBW infants has led to increased interest in the energy requirements for growth. The energy cost of growth is comprised of two components: the energy equivalent of tissue stores of fat, protein, and carbohydrate added during growth, and the energy expended by the body in the process of depositing new tissues of growth.
Although a number of observers have reported estimates of energy stored by the growing LBW infant, there is a paucity of experimental data available concerning the energy expended by infants during the deposition of growth tissues. Since rapid and efficient growth is a major goal of neonatal nutritional support(1), estimates of the energy cost of tissue deposition should prove useful in understanding the physiology of growth in the LBW infant.
The purpose of this investigation was to relate the energy expenditure of growing LBW infants to the amount of protein stored, the amount of fat stored, and the infant's physical activity, and, thereby, to estimate the energy expended in protein and fat deposition.
METHODS
Subjects. The study population consisted of 120 LBW infants. All were participants in a series of four prospective feeding studies investigating the effects of variations in protein and energy intake on the rate and composition of weight gain in LBW infants(2–6). Each of the four studies was similar in design and evaluated the effects of three different diets. The design and methods have been described in detail(2–6) and are summarized below.
The infants' birth weights ranged from 760 to 1770 g (mean = 1387 ± 235 g) and gestational ages ranged from 26 to 37 wk. The postnatal study ages ranged from 2 to 9 wk. At the time of study all infants were medically stable, were on no drugs or other therapies that would influence energy expenditure, and had no serious medical complications from their prematurity. All studies were approved by the IRB of Columbia University, and written informed consent was obtained from the parents of all infants enrolled.
Experimental protocol. Both formula-fed infants and human milk-fed infants were studied. The experimental formulas were manufactured by Ross Laboratories specifically for the feeding studies. The energy content of the intakes ranged from 98 to 159 kcal/kg/d, and the protein intake ranged from 2.2 to 4.2 g/kg/d. All other components of the formulas were identical. The energy and protein content varied independently. Nonprotein energy of the experimental formulas was 50% fat and 50% carbohydrate.
Human milk-fed infants were fed their mothers' milk(4). If the supply was inadequate, they received supplemented pooled banked human donor milk. The composition of both the formulas and the human milk feedings was analyzed serially during the study. An aliquot of breast milk was collected each day during each week of the protocol. The human milk aliquots were pooled and analyzed subsequently in the same manner as the formulas(4). Vitamin supplementation was provided to all infants, and the nutrient content of the vitamins, as described by the manufacturer, was included in measurements of gross energy intake.
Experimental feedings were introduced as soon as the infant commenced enteral feeds. Feedings were advanced according to standard nursery practices. If the infant achieved full intake, defined as an intake of 180 mL/kg/d, by 28-d postnatal age, the infant was enrolled in the study.
Experimental variables. The following variables were measured serially from the time of full enteral intake until a discharge weight of 2200 g was achieved.
Growth. Body weight was measured daily on a Scaletronix 4800 pediatric balance scale to the nearest 5 g. The rate of weight gain, expressed as grams/kg·d was computed from a regression of the daily weight against the infant's age in days, using an exponential model(5).
Energy expenditure. Energy expenditure was estimated by open circuit indirect calorimetry using 6-h (two 3-h epochs) measurements of oxygen consumption and carbon dioxide production(7). From these measurements and 24-h measurements of urinary nitrogen excretion, energy expenditure was calculated using the constants of Lusk(8). The infants' skin temperature was maintained at 36.5°C using a servo-controlled radiant warmer(9, 10).
Measurements of physical activity. Throughout the 6-h studies of energy expenditure, the state of sleep or wakefulness was recorded each minute and coded according to methods developed in our laboratory(11).
Protein stored. Nitrogen balance was determined every 2 wk as the difference between nitrogen intake and the sum of urinary and fecal nitrogen losses. Urinary losses were computed from 48-72-h urinary nitrogen excretion, and stool losses were computed from 48-72-h stool samples. The collection methods have been described in a previous publication(3). Nitrogen content of urine, stool, and formula were measured by the Dumas method using a Coleman model 129 automatic nitrogen analyzer (Perkin-Elmer Corp., Norwalk, CT)(12). Protein stored was computed as 6.25 times nitrogen balance (grams/kg·d).
Metabolizable energy. Gross energy intake and stool energy losses were measured by bomb calorimetry(13). The energy content of urine was calculated as 5.4 kcal/g (the heat of combustion of urea) of urinary urea nitrogen(14). The small amount of carbohydrate lost in the stool was included in the measurement of stool energy content(15). Metabolizable energy was calculated as the difference between gross energy intake and energy losses in the excreta.
Energy stored. Energy stored was computed as the difference between gross energy intake and the sum of excretory losses and energy expenditure.
Fat stored. Fat stored was computed from energy stored and protein stored according to the following equation: where 5.65 and 9.25 represent the energy of combustion for milk protein and fat, respectively(16).

The study consisted of 229 nitrogen balance and energy balance determinations with accompanying 6-h activity assessments. Of the 120 infants studied, 85 had two calorimetry studies performed 2 wk apart. Twenty four infants had one study, nine infants had three studies, and two infants had four studies performed.
Data analysis. To determine the relationship between macronutrient storage and energy expenditure, the following model was formulated: under thermoneutral conditions, the energy expended by growing LBW infants is determined by maintenance energy expenditure, energy expended in protein and fat storage, and energy expended in physical activity, all expressed in kilocalories/kg·d. It is assumed that differences in energy expenditure related to physical activity in the premature infant are largely due to differences in the distribution of states of sleep. Premature infants are known to sleep 80-90% of the time and it is known that during active sleep energy expenditure is approximately 15% greater than during quiet sleep(17, 18).
This model is expressed mathematically as: equation 1 where EE is energy expenditure in kilocalories/kg·d,c is the energy expenditure of nongrowing infants at rest in kilocalories/kg·d, Ps is protein stored in grams/kg·d,Fs is fat stored in grams/kg·d., Act is the percent time spent in active sleep. The coefficient p is kilocalories EE/ g protein stored, f is kilocalories EE/g fat stored, and a is kcal EE/kg·d/% time in active sleep.

To test this regression model, independent measurements of EE, Ps, Fs, and Act are required. However, Fs is not measurable directly but must be computed from measurements of energy stored (ME - EE); hence, Fs is not independent of EE. Thus, it was necessary to transform the regression model algebraically to express EE in terms of an independent experimental measurement,ME. The steps in this transformation are shown below:equation 2 where (ME - EE - 5.65Ps)/9.25 is Fs computed from energy and nitrogen balance data, and the other terms are as in Equation 1 above.Equation 3,Equation 4,Equation 5 Simplifying the equation by substituting single symbols for the more complex functions in Equation 5, the equation becomes: Equation 6 So that: Equation This model was fitted to the data using the REG and NLIN procedures of SAS.






RESULTS
The study subjects, grouped according to dietary group and relevant ages and weights, are described in Table 1. Study weight refers to the infants weight at the time of the energy balance study. Gestational age refers to gestational age at time of birth. Postnatal age is the age expressed in days at the time of the energy balance study. The values used in the calculations are the overall study means.
Means and SD values for weight gain, energy expenditure, metabolizable energy, protein stored, fat stored, and percent active sleep are summarized by diet group in Table 2. Because weight gain is composed primarily of protein stored, fat stored, and water, the relationship between energy expenditure and weight gain was examined by simple linear regression. The slope of the line, 0.45 ± 0.13 kcal/g, is an estimate of the energy expended in the synthesis of a gram of weight gain of infants on mixed intakes of protein and energy. This relationship is plotted in Figure 1.
The results of the regression analysis of the multivariate model, with the precision expressed as SE, are shown below: Equation The coefficients b1 = 3.6 and b2 = 0.14 and the intercept b0 = 31.8 were significant; however, the coefficient b3 for percent active sleep was not significant. Because physical activity did not account for significant additional variability in EE, this independent variable was eliminated from the model, and the analysis was repeated. Equation Transforming the equation back to the original form with Fs replacing ME yields the following equation: Thus, the energy costs of protein and fat deposition are approximately 5.5 and 1.62 kcal/g, respectively, and the energy expended by the nongrowing infant is approximately 42 kcal/kg·d.



The measurements listed in Table 2 were used in the regression model to estimate the two components of the energy cost of growth, that is, the energy cost of deposition (5.5Ps + 1.6Fs) and energy cost of storage (5.65Ps + 9.25Fs). For this group of infants on varying protein and caloric intakes, the mean energy cost of growth was 74 ± 15 kcal/kg·d.
Figure 2A illustrates the regression relationship between energy expenditure and protein storage, adjusted for the effects of metabolizable energy. Figure 2B illustrates the regression relationship between energy expenditure and metabolizable energy, adjusted for protein stored.
(A) Energy expenditure in kilocalories/kg·d is regressed against protein stored expressed in grams/kg·d. Energy expenditure has been adjusted for the effects of metabolizable energy. (B) Energy expenditure in kilocalories/kg·d is regressed against metabolizable energy, expressed in kilocalories/kg·d. Energy expenditure has been adjusted for the effects of protein stored.
DISCUSSION
The energy expended in the deposition of protein and fat has been investigated previously from both a theoretical and an experimental perspective. Using a theoretical approach Hommes et al.(19) and Holmes(20) estimated the energy cost of substrate deposition applying Atkinson's metabolic price system. This system assigns ATP equivalents and, hence, caloric costs, to each step in the digestion and transport of macronutrient substrates as well as to each synthetic step involved in making peptides, proteins, tissue lipids, and so forth. Assuming all processes have been identified and included, the sum of these caloric equivalents represents a minimal estimate of the energy expended in tissue synthesis.
A number of investigators have estimated the energy costs of tissue deposition experimentally. In the pig model, using estimates of fat and protein stored obtained from carcass analysis and predicting ME and net energy stored from intakes, the total energy costs of protein and fat deposition were found to be 15.96 and 12.96 kcal/g, respectively, of which the energy costs of synthesis accounted for 10.31 and 3.71 kcal/g, respectively(21). Other studies in the rat, using direct measurements of protein and fat stored, metabolizable energy and energy expenditure, estimated the energy expended in protein and fat synthesis to be 7.06 and 3.3 kcal/g, respectively(22).
Estimates of the energy cost of synthesis have also been derived from studies of macronutrient storage and energy expenditure in the human LBW infant(23–30). Gross estimates of the relationship between weight gain and energy expenditure indicate that the overall energy cost per g of weight gain ranges from 0.23 to 0.68 kcal/g(25–27). Our data from 120 infants on mixed intakes suggest the energy expended in tissue synthesis is in the range of 0.45 ± 0.13 kcal/g. An analysis of pooled data from a number of studies of LBW infants relating metabolizable energy intake, energy expenditure, and estimates of protein and fat stored from nitrogen balance and energy stored, respectively, concluded that the energy expended in protein and fat synthesis was approximately 7.75 and 1.55 kcal/g, respectively(23). The results of our investigation, using a different regression model, one which used independent measurements of all independent variables, agree rather closely with the data reported in this study. The amount of variability in energy expenditure accounted for by raw weight gain was relatively small (r2 = 0.09). Greater variability could be explained by examining the individual components of weight gain, ie protein and fat (r2 = 0.34).
Several unique features of our experimental design are worth noting. All infants were on prospectively controlled and accurately measured intakes, study intervals were never less than 2 wk, all infants were studied using the same methodologies, and the possible confounding effects of physical activity were investigated. In addition, energy expenditure itself was the dependent variable in the regression model.
In general, estimates of the energy cost of synthesis obtained experimentally are several times greater than the theoretical estimates using the metabolic price system. This is thought to be due to the fact that protein accretion is a dynamic and inefficient process. Tracer studies suggest that net protein synthesis requires a 5-fold turnover of tissue protein,i.e. roughly 5 g of protein are synthesized and catabolized for every gram of protein stored as new tissue(31). The differences between theoretical and experimental estimates of the energy expended in tissue deposition remain largely unexplained. Some uncertainty exists as to the true caloric value of ATP equivalents, and although it may be that the net synthesis is an inefficient process, it is also true that the metabolic price system may not account for all energy expended in tissue synthesis(19). For example, it is known that weight gain and protein storage are associated with increases in heart rate and respiratory rate(32). Because these are energy-requiring processes, it follows that the energy requirements for oxygen transport by the heart and lungs are also influenced by the rate of weight gain. These costs, although small in terms of total energy expenditure, are significant in relation to the energy expended in tissue synthesis. If dietary intake exerted a systematic effect on physical activity and, therefore, altered total energy expenditure, our estimates of the energy cost of synthesis would be biased. Infants receiving low protein intakes or human milk are known to spend less time in active sleep, and active sleep is a time of increased energy expenditure(17, 33). In theory, this could falsely increase our estimates of the energy cost of protein synthesis. Although our results did not indicate an independent effect of activity on energy expenditure, the range of variation in percent active sleep was relatively small, and this measurement represents only one measure of physical activity. Thus the possibility remains that activity may systematically alter physical activity and energy expenditure in ways not accounted for by macronutrient storage.
The energy cost of growth for the LBW infant is substantial. In this series of studies of LBW infants, the mean total energy cost of growth was found to be 74 ± 15 kcal/kg·d, of which 54 ± 12 kcal/kg·d or 73% was stored as fat and protein, and 20 ± 3 kcal/kg·d or 27% was expended in fat and protein deposition. Thus, on average, 45% of caloric intake is stored as new tissue and 32% of the total energy expenditure of the growing infant is related to tissue accretion.
These observations in healthy growing LBW infants may be pertinent to prevailing questions about growth failure in distressed infants, particularly those with cardiorespiratory insufficiency. Growth failure in the presence of limited oxygen availability is poorly understood and fundamental questions remain unanswered. Is the growth failure of the patient with bronchopulmonary dysplasia due to primary limitations of nutrient intake, or are there more fundamental limitations in oxygen available for the bioenergetic functions controlling tissue synthesis? What are the consequences of delivering large amounts of substrates such as amino acids when oxygen transport and cellular energy stores are insufficient? Our data from the LBW infants suggest that the high energy cost of protein accretion might render growth of lean body mass particularly sensitive to limitations in oxygen availability. The mechanisms that control tissue synthesis and balance the rate of tissue synthesis with intracellular energy stores are important clinical issues that remain to be investigated.
Abbreviations
- LBW:
-
low birth weight
References
Committee on Nutrition of the American Academy of Pediatrics 1985 Nutritional needs of the low birth weight infants. Pediatrics 75: 976
Kashyap S, Forsyth MS, Zucker C, Ramakrishnan R, Dell RB, Heird WC 1986 Effects of varying protein and energy intakes on growth and metabolic response in low birth weight infants. J Pediatr 108: 955–963
Kashyap S, Schulze K, Forsyth M, Zucker C, Dell RB, Ramakrishnan R, Heird WC 1988 Growth, nutrient retention and metabolic response in low birth weight infants fed varying intakes of protein and energy. J Pediatr 113: 713–721
Kashyap S, Schulze KF, Forsyth M, Dell RB, Ramakrishnan R, Heird WC 1990 Growth, nutrient retention and metabolic response of low birth weight infants fed supplemented and unsupplemented preterm human milk. Am J Clin Nutr 52: 254–262
Kashyap S, Schulze KF, Ramakrishnan R, Dell R, Heird WC 1994 Evaluation of a mathematical model for predicting the relationship between protein and energy intakes of low-birth-weight infants and the rate and composition of weight gain. Pediatr Res 35: 704–712
Schulze KF, Stefanski M, Masterson J, Spinnazola R, Ramakrishnan R, Dell RB, Heird WC 1987 Energy expenditure, energy balance and composition of weight gain in low birth weight infants fed diets of different protein and energy content. J Pediatr 110: 753–759
Schulze KF, Kairam R, Stefanski M, Sciacca R, James LS 1981 Continuous measurements of minute ventilation and gaseous metabolism of newborn infants. J Appl Physiol 50: 1098–11036
Lusk G. 1961 Basal Metabolism Standards. Scientific Tables, Ed 6. Documenta Geigy, Montreal, pp 628
Mestyan J, Jarai I, Fekete M 1968 The total energy expenditure and its components in premature infants maintained under different nursing and environmental conditions. Pediatr Res 2: 161–171
Hey EN 1971 The care of babies in incubators. In: Recent Advances in Pediatrics, 4th Ed. Churchill, London, pp 171
Stefanski M, Schulze KF, Bateman D, Kairam R, Pedley TA, Masterson J, James LS 1984 A scoring system for states of sleep and wakefulness in term and preterm infants. Pediatr Res 18: 58–62
Ebeling M 1968 The Dumas method for nitrogen in feeds. J Assoc Off Agric Chem 51: 766
Miller DS, Payne PR 1959 A ballistic bomb calorimeter. Br J Nutr 13: 501–508
Kleiber M. 1974 The Fire of Life: An Introduction to Animal Energetics. Krieger, Melbourne, FL, pp 104–130
Ameen VZ, Powell GK 1989 Quantitative fecal carbohydrate excretion in premature infants. Am J Clin Nutr 49: 1238–1242
Report of FAO/WHO Ad Hoc Committee in Energy and Protein Requirements. 1973 FAO Nutritional Series No.7 Rome, Food and Agricultural Organization of the United Nations, pp 102
Stothers JK, Warner RM 1978 Oxygen consumption and neonatal sleep states. J Physiol (Lond) 278: 435–440
Schulze KF, Kairam R, Stefanski M, Sciacca R, Bateman D, Dell RB, James LS 1981 Spontaneous variability in minute ventilation, oxygen consumption and heart rate of low birth weight infants. Pediatr Res 15: 1111–1116
Hommes FA, Drost YM, Geralts XYM, Reijenga MAA 1975 The energy requirement for growth; an application of Atkinson's metabolic price system. Pediatr Res 9: 51–55
Hommes FA 1980 The energy requirement for growth. A reevaluation. Nutr Metab 24: 110–113
Kielanowski J, Kotarbinska M 1970 Energy requirements of growing pigs. Eur Assoc Anim Prod Publ 13: 145
Pullar JD, Webster AJF 1977 The energy cost of fat and protein deposition in the rat. Br J Nutr 37: 355–363
Roberts SB, Young VR 1988 Energy costs of fat and protein deposition in the human infant. Am J Clin Nutr 48: 951–954
Reichman BL, Chessex P, Putet G, Verellan GJE, Smith JM, Heim T, Swyer PR 1982 Partition of energy metabolism and energy cost of growth in the very low-birth weight infant. Pediatrics 69: 446–451
Gudinchet F, Schutz Y, Micheli JL, Stettler E, Jequier E 1982 Metabolic cost of growth in very low birth weight infants. Pediatr Res 16: 1025–1031
Sauer PJJ, Pearse RG, Dane HJ, Visser HKA 1979 The energy cost of growth estimated from simultaneous direct and indirect calorimetry in infants of less than 2500 g. In: Visser HKA (ed) Nutrition and Metabolism of the Fetus and Infant. Martinus Nijhoff, Amsterdam
Reichman BJ, Chessex P, Putet G, Verellen G, Smith JM, Heim T, Swyer PR 1981 Diet, fat accretion and growth in premature infants. N Engl J Med 305: 1495–1500
Brooke OG 1980 Energy balance and metabolic rate in preterm infants fed with standard and high-energy formulas. Br J Nutr 44: 13–23
Brooke OG 1982 Energy requirements and utilization of the low birth infant. Acta Paediatr Scand Suppl 296: 67
Chessex P, Reichman BJ, Verellen GJE, Putet G, Smith JM, Heim T, Swyer PR 1981 Influence of postnatal age, energy intake, and weight gain on energy metabolism in the very low birthweight infant. J Pediatr 99: 761–766
Young VR, Steffee WP, Pencharz PB, Winterer JC, Scrimshaw NS 1975 Total human body protein synthesis in relation to protein requirements at various ages. Nature 253: 192–194
Schulze K, Kashyap S, Ramakrishnan R 1993 Cardiorespiratory costs of growth in low birth weight infants. J Dev Physiol 19: 85–90
Butte NF, Jensen CL, Moon JK, Glaze DG, Frost JD Jr 1992 Sleep organization and energy expenditure of breast-fed and formula-fed infants. Pediatr Res 32: 514–519
Acknowledgements
The authors thank Steve Holleran for his assistance in the statistical analysis.
Author information
Authors and Affiliations
Additional information
Supported by U.S. Public Health Service Grants HD13020, HD13063, HD27564, and RR00645, and by Wyeth-Ayerst Laboratories.
Rights and permissions
About this article
Cite this article
Towers, H., Schulze, K., Ramakrishnan, R. et al. Energy Expended by Low Birth Weight Infants in the Deposition of Protein and Fat. Pediatr Res 41, 584–589 (1997). https://doi.org/10.1203/00006450-199704000-00021
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199704000-00021
This article is cited by
-
Predicting growth of the healthy infant using a genome scale metabolic model
npj Systems Biology and Applications (2017)