Abstract
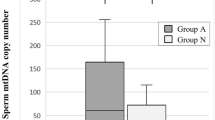
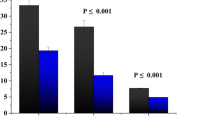
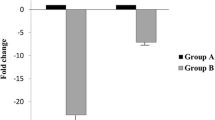
Sperm contain a complex population of coding and noncoding RNA, and the utility of sperm RNA in fertility research is currently being explored. The aim of this study was to estimate the content of transcripts of protamines 1 and 2 in human ejaculated spermatozoa in relation to semen quality and sperm DNA fragmentation between fertile and infertile patients. Human ejaculates were obtained from 33 patients and semen analyzes were assessed by WHO criteria (2010). We evaluated the sperm DNA fragmentation measured by TUNEL assay. The ejaculates of patients were purified by density-gradient centrifugation, sperm cells were lysed, and mRNA was extracted, reverse transcribed, and subjected to real-time qPCR using specific primer pairs for protamine-1, protamine-2 RNA. The sperm protamine mRNA ratio in normozoospermic men (n = 19; 2.86 ± 0.16) differed significantly from that of patozoospermic patients (n = 14; 3.43 ± 0.22; p < 0.05). A significant correlation was shown between sperm DNA fragmentation and the PRM2/PRM1 mRNA ratio (r = 0.33; p < 0.05). In the group of patients with an increased sperm DNA fragmentation (n = 14; 2.74 ± 0.18), the PRM2/PRM1 ratio was significantly higher than in the group of patients with normal rates (n = 19; 3.26 ± 0.19; p < 0.05). An abnormal sperm protamine ratio was associated with poor semen quality and DNA fragmentation. Finding sperm-quality markers would help to understand the causes of male infertility and to improve male reproductive health.



Similar content being viewed by others
REFERENCES
Oliva, R., Protamines and male infertility, Hum. Reprod. Update., 2006, vol. 12, no. 4, pp. 417–435. https://doi.org/10.1093/humupd/dml009
Jodar, M., Selvaraju, S., Sendler, E., et al., The presence, role and clinical use of spermatozoal RNAs, Hum. Reprod. Update., 2013, vol. 19, no. 6, pp. 604–624. https://doi.org/10.1093/humupd/dmt031
Sendler, E., Johnson, G.D., Mao, S., et al., Stability, delivery and functions of human sperm RNAs at fertilization, Nucleic Acids Res., 2013, vol. 41, no. 7, pp. 4104–4117. https://doi.org/10.1093/nar/gkt132
Jodar, M., Sendler, E., Moskovtsev, S.I., et al., Absence of sperm RNA elements correlates with idiopathic male infertility, Sci. Transl. Med., 2015, vol. 7, p. 295. https://doi.org/10.1126/scitranslmed.aab1287
Godia, M., Swanson, G., and Krawetz, S.A., A history of why fathers’ RNA matters, Biol. Reprod., 2018, vol. 99, no. 1, pp. 147–159. https://doi.org/10.1093/biolre/ioy007
Krawetz, S.A., Paternal contribution: new insights and future challenges, Nat. Rev. Genet., 2005, vol. 6, no. 8, pp. 633–642. https://doi.org/10.1038/nrg1654
Carrell, D.T., Epigenetics of the male gamete, Fertil. Steril., 2012, vol. 97, no. 2, pp. 267–274. https://doi.org/10.1016/j.fertnstert.2011.12.036
Rando, O.J., Daddy issues: paternal effects on phenotype, Cell, 2012, vol. 151, no. 4, pp. 702–708. https://doi.org/10.1016/j.cell.2012.10.020
Castillo, J., Estanyol, J.M., Ballescà, J.L., and Oliva, R., Human sperm chromatin epigenetic potential: genomics, proteomics, and male infertility, Asian J. Androl., 2015, vol. 17, pp. 601–609. https://doi.org/10.4103/1008-682X.153302
Chen, Q., Yan, W., and Duan, E., Epigenetic inheritance of acquired traits through sperm RNAs and sperm RNA modifications, Nat. Rev. Genet., 2016, vol. 17, no. 12, pp. 733–743. https://doi.org/10.1038/nrg.2016.106
Ammer, H., Henschen, A., and Lee, C.H., Isolation and amino-acid sequence analysis of human sperm protamines P1 and P2: occurrence of two forms of protamine P2, Biol. Chem. Hoppe Seyler, 1986, vol. 367, no. 1, pp. 515–522. https://doi.org/10.1515/bchm3.1986.367.1.515
Steger, K., Klonisch, .T, Gavenis, K., et al., Expression of mRNA and protein of nucleoproteins during human spermiogenesis, Mol. Hum. Reprod., 1998, vol. 4, no. 10, pp. 939–945. https://doi.org/10.1093/molehr/4.10.939
Steger, K., Pauls, K., Klonisch, T., et al., Expression of protamine-1 and -2 mRNA during human spermiogenesis, Mol. Hum. Reprod., 2000, vol. 6, no. 3, pp. 219–225. https://doi.org/10.1093/molehr/6.3.219
Aoki, V.W., Emery, B.R., Liu, L., and Carrell, D.T., Protamine levels vary between individual sperm cells of infertile human males and correlate with viability and DNA integrity, J. Androl., 2006, vol. 27, no. 6, pp. 890–898. https://doi.org/10.2164/jandrol.106.000703
Morales, C.R., Kwon, Y.K., and Hecht, N.B., Cytoplasmic localization during storage and translation of the mRNAs of transition protein 1 and protamine 1, two translationally regulated transcripts of the mammalian testis, J. Cell Sci., 1991, vol. 100, no. 1, pp. 119–131. http://www.ncbi.nlm.nih.gov/pubmed/1795020.
Balhorn, R., Cosman, M., Thornton, K., et al., Protamine mediated condensation of DNA in mammalian sperm, in The Male Gamete: From Basic Science to Clinical Applications, Salt Lake City, Utah: American Society of Andrology, 1999, pp. 707–907.
Simon, L., Murphy, K., Shamsi, M.B., et al., Paternal influence of sperm DNA integrity on early embryonic development, Hum. Reprod., 2014, vol. 29, no. 11, pp. 2402–2412. https://doi.org/10.1093/humrep/deu228
Mengual, L., Ballescà, J.L., Ascaso, C., and Oliva, R., Marked differences in protamine content and P1/P2 ratios in sperm cells from percoll fractions between patients and controls, J. Androl., 2003, vol. 24, no. 3, pp. 438–447. https://doi.org/10.1002/j.1939-4640.2003.tb02692.x
Wright, C., Milne, S., and Leeson, H., Sperm DNA damage caused by oxidative stress: modifiable clinical, lifestyle and nutritional factors in male infertility, Reprod. Biomed. Online, 2014, vol. 28, no. 6, pp. 684–703. https://doi.org/10.1016/j.rbmo.2014.02.004
Miller, D., Briggs, D., Snowden, H., et al., A complex population of RNAs exists in human ejaculate spermatozoa: implications for understanding molecular aspects of spermiogenesis, Gene, 1999, vol. 237, no. 2, pp. 385–392. https://doi.org/10.1016/s0378-1119(99)00324-8
Ostermeier, G.C., Dix, D.J., Miller, D., et al., Spermatozoal RNA profiles of normal fertile men, Lancet, 2002, vol. 360, no. 9335, pp. 772–777. https://doi.org/10.1016/S0140-6736(02)09899-9
Kempisty, B., Depa-Martynow, M., Lianeri, M., et al., Evaluation of protamines 1 and 2 transcript contents in spermatozoa from asthenozoospermic men, Folia Histochem. Cytobiol., 2007, vol. 45, no. 1, pp. 109–113. http://www.ncbi.nlm.nih.gov/pubmed/18292846.
González-Marín, C., Gosálvez, J., and Roy, R., Types, causes, detection and repair of DNA fragmentation in animal and human sperm cells, Int. J. Mol. Sci., 2012, vol. 13, no. 11, pp. 14026–14052. https://doi.org/10.3390/ijms131114026
WHO Laboratory Manual for the Examination and Processing of Human Semen, 2010.
Efimova, O.A., Pendina, AA., Tikhonov, A.V., et al., Genome-wide 5-hydroxymethylcytosine patterns in human spermatogenesis are associated with semen quality, Oncotarget, 2017, vol. 8, no. 51, pp. 88294–88307. https://doi.org/10.18632/oncotarget.18331
Virro, M.R., Larson-Cook, K.L., Evenson, D.P., et al., Sperm chromatin structure assay (scsa®) parameters are related to fertilization, blastocyst development, and ongoing pregnancy in in vitro fertilization and intracytoplasmic sperm injection cycles, Fertil. Steril., 2004, vol. 81, no. 5, pp. 1289–1295. https://doi.org/10.1016/j.fertnstert.2003.09.063
Evenson, D. and Wixon, R., Meta-analysis of sperm DNA fragmentation using the sperm chromatin structure assay, Rep. BioMed Online, 2006, vol. 12, no. 4, pp. 466–472. https://doi.org/10.1016/S1472-6483(10)62000-7
Hecht, N.B., Regulation of “haploid expressed genes” in male germ cells, J. of Reprod. Fertil., 1990, vol. 88, pp. 679–693. https://doi.org/10.1530/jrf.0.0880679
Grunewald, S., Paasch, U., Glander, H.J., and Anderegg, U., Mature human spermatozoa do not transcribe novel RNA, Andrologia, 2005, vol. 37, no. 2, pp. 69–71. https://doi.org/10.1111/j.1439-0272.2005.00656.x
Steger, K., Transcriptional and translational regulation of gene expression in haploid spermatids, Anat. Embryol. (Berlin), 1999, vol. 199, no. 6, pp. 471–487. https://doi.org/10.1007/s004290050245
Ahmadi, A. and Ng, S.C., Destruction of protamine in human sperm inhibits sperm binding and penetration in the zona-free hamster penetration test but increases sperm head decondensation and male pronuclear formation in the hamster-ICSI assay, J. Assist. Reprod. Genet., 1999, vol. 16, no. 3, pp. 128–132. https://doi.org/10.1023/a:1022527714175
Nanassy, L., Liu, L., Griffin, J.T., and Carrell, D., The clinical utility of the protamine 1/protamine 2 ratio in sperm, Protein Pept. Lett., 2012, vol. 18, no. 8, pp. 772–777. https://doi.org/10.2174/092986611795713934
Depa-Martynow, M., Kempisty, B., Jagodziński, P.P., et al., Impact of protamine transcripts and their proteins on the quality and fertilization ability of sperm and the development of preimplantation embryos, Reprod. Biol., 2012, vol. 12, no. 1, pp. 57–72. https://doi.org/10.1016/s1642-431x(12)60077-1
Rogenhofer, N., Dansranjavin, T., Schorsch, M., et al., The sperm protamine mRNA ratio as a clinical parameter to estimate the fertilizing potential of men taking part in an ART programme, Hum. Reprod., 2013, vol. 28, no. 4, pp. 969–978. https://doi.org/10.1093/humrep/des471
Platts, A.E., Dix, D.J., Chemes, H.E., et al., Success and failure in human spermatogenesis as revealed by teratozoospermic RNAs, Hum. Mol. Genet., 2007, vol. 16, no. 7, pp. 763–773. https://doi.org/10.1093/hmg/ddm012
Savadi-Shiraz, E., Edalatkhah, H., Talebi, S., et al., Quantification of sperm specific mRNA transcripts (PRM1, PRM2, and TNP2) in teratozoospermia and normozoospermia: new correlations between mRNA content and morphology of sperm, Mol. Reprod. Dev., 2015, vol. 82, no. 1, pp. 26–35. https://doi.org/10.1002/mrd.22440
Miyagawa, Y., Nishimura, H., Tsujimura, A., et al., Single-nucleotide polymorphisms and mutation analyses of the TNP1 and TNP2 genes of fertile and infertile human male populations, J. Androl., 2005, vol. 26, no. 6, pp. 779–786. https://doi.org/10.2164/jandrol.05069
Evenson, D.P., Larson, K.L., and Jost, L.K., Sperm chromatin structure assay: its clinical use for detecting sperm DNA fragmentation in male infertility and comparisons with other techniques, J. Androl., 2002, vol. 23, no. 1, pp. 25–43. http://www.ncbi.nlm.nih. gov/pubmed/11780920.
Seli, E., Spermatozoal nuclear determinants of reproductive outcome: implications for ART, Hum. Reprod. Update., 2005, vol. 11, no. 4, pp. 337–349. https://doi.org/10.1093/humupd/dmi011
Shamsi, M.B., Kumar, R., and Dada, R., Evaluation of nuclear DNA damage in human spermatozoa in men opting for assisted reproduction, Indian J. Med. Res., 2008, vol. 127, no. 2, pp. 115–123. http://www.ncbi.nlm.nih.gov/pubmed/18403788.
Simon, L., Castillo, J., Oliva, R., and Lewis, S.E., Relationships between human sperm protamines, DNA damage and assisted reproduction outcomes, Reprod. Biomed. Online., 2011, vol. 23, no. 6, pp. 724–734. https://doi.org/10.1016/j.rbmo.2011.08.010
Hosen, M.B., Islam, M.R., Begum, F., et al., Oxidative stress induced sperm DNA damage, a possible reason for male infertility, Iran. J. Reprod. Med., 2015, vol. 13, no. 9, pp. 525–532. http://www.ncbi.nlm.nih.gov/ pubmed/26568756.
Simon, L., Zini, A., Dyachenko, A., et al., A systematic review and meta-analysis to determine the effect of sperm DNA damage on in vitro fertilization and intracytoplasmic sperm injection outcome, Asian J. Androl., 2017, vol. 19, no. 1, pp. 80–90. https://doi.org/10.4103/1008-682X.182822
Zheng, W.W., Song, G., Wang, Q.L., et al., Sperm DNA damage has a negative effect on early embryonic development following in vitro fertilization, Asian J. Androl., 2018, vol. 20, no. 1, pp. 75–79. https://doi.org/10.4103/aja.aja_19_17
Pellestor, F., Gatinois, V., Puechberty, J., et al., Chromothripsis: potential origin in gametogenesis and preimplantation cell divisions: a review, Fertil. Steril., 2014, vol. 102, no. 6, pp. 1785–1796. https://doi.org/10.1016/j.fertnstert.2014.09.006
Koltsova, A.S., Pendina, A.A., Efimova, O.A., et al., On the complexity of mechanisms and consequences of chromothripsis: an update, Front. Genet., 2019, vol. 10, no. 4, p. 393. https://doi.org/10.3389/fgene.2019.00393
Agarwal, A. and Allamaneni, S.R., Sperm DNA damage assessment: a test whose time has come, Fertil. Steril., 2005, vol. 84, no. 4, pp. 850–853. https://doi.org/10.1016/j.fertnstert.2005.03.080
Funding
This study was financed by the Russian Science Foundation (grant no. 18-75-10046).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest. The authors declare that they have no conflict of interest.
Statement of compliance with standards of research involving humans as subjects. All procedures performed in a study involving people comply with the ethical standards of the institutional and/or national committee for research ethics and the 1964 Helsinki Declaration and its subsequent changes or comparable ethical standards.
Informed voluntary consent was obtained from each of the participants.
Rights and permissions
About this article
Cite this article
Ishchuk, M.A., Malysheva, O.V., Komarova, E.M. et al. Protamine 1 and 2 mRNA Abundance in Human Spermatozoa and Its Relation to Semen Quality and Sperm DNA Fragmentation among Fertility Clinic Patients. Russ J Genet 57, 213–220 (2021). https://doi.org/10.1134/S1022795421020058
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S1022795421020058