-
PDF
- Split View
-
Views
-
Cite
Cite
Jennifer M. Streit, Judith N. Steenbergen, Grace M. Thorne, Jeffrey Alder, Ronald N. Jones, Daptomycin tested against 915 bloodstream isolates of viridans group streptococci (eight species) and Streptococcus bovis, Journal of Antimicrobial Chemotherapy, Volume 55, Issue 4, April 2005, Pages 574–578, https://doi.org/10.1093/jac/dki032
Close - Share Icon Share
Abstract
Objectives: To evaluate the activity of daptomycin tested against numerous species of viridans group streptococci and Streptococcus bovis, which are associated with wound infections, sepsis, cellulitis, endocarditis, abscesses and dental caries. The incidence of penicillin-resistant (non-susceptible) and MLSB-resistant strains among viridans group streptococci often varies by species.
Methods: The activity of daptomycin was compared with seven other antimicrobial classes using reference broth microdilution and disc diffusion methods tested against 915 bacteraemic isolates of streptococci (815 viridans group strains; 100 S. bovis).
Results: Among all species of viridans group streptococci and S. bovis, 99.9% of isolates were susceptible to daptomycin (MIC values, ≤ 0.016–2 mg/L). In contrast, penicillin, erythromycin and tetracycline susceptibility varied widely between species. Erythromycin susceptibility was in the range 48.6–88.7%, penicillin susceptibility in the range 65.5–98.1% and tetracycline in the range 35.0–93.9%. The inter-method agreement between daptomycin and linezolid resistance (comparison agent) disc diffusion and broth microdilution test results was high, each showing near complete susceptibility (99.9%).
Conclusions: Daptomycin is an active antimicrobial agent that has a usable potency against eight species of viridans group streptococci, as well as S. bovis, with all MIC values at ≤2 mg/L.
Introduction
Daptomycin (formerly LY146032) is a novel cyclic lipopeptide, which has demonstrated bactericidal activity against most Gram-positive organisms.1,2 Daptomycin's mode of killing action includes inhibiting cell wall synthesis and establishing multiple ion gradients across the cytoplasmic membranes—giving it a unique dual mechanism2–4— thus having no cross-resistance with glycopeptides (teicoplanin and vancomycin).2,3 The bactericidal activity of daptomycin is dependent upon physiological levels of free calcium ions, Ca++ (50 mg/L).2–6 Increasing calcium concentration in the Mueller–Hinton agar test media has been demonstrated to produce optimal daptomycin disc diffusion results.6
The daptomycin spectrum of activity includes many multidrug-resistant strains for which there are few therapeutic alternatives, including vancomycin-resistant enterococci, methicillin- or oxacillin-resistant Staphylococcus aureus and penicillin-resistant streptococci.1,2,7,8 The United States Food and Drug Administration (US-FDA) recently approved categorical breakpoints for S. aureus, β-haemolytic streptococci and vancomycin-susceptible Enterococcus faecalis for daptomycin at ≤1, ≤1 and ≤4 mg/L, respectively; these criteria were added to National Committee for Clinical Laboratory Standards (NCCLS) tables9 and modified to include Streptococcus spp. (not Streptococcus pneumoniae) at a breakpoint of ≤1 mg/L. Here we report on the susceptibility profiles using breakpoint criteria promulgated by the NCCLS (see Table 1)9 for each of eight species of viridans group streptococci and Streptococcus bovis tested against daptomycin.
Materials and methods
Bacterial isolates
The study collection of 915 streptococci (target ≥ 100 strains per species) recovered from bloodstream infections included strains of Streptococcus anginosus (106 strains), Streptococcus constellatus (103 strains), Streptococcus intermedius (103 strains), Streptococcus mitis (102 strains), Streptococcus mutans (66 strains), Streptococcus oralis (107 strains), Streptococcus salivarius (101 strains), Streptococcus sanguis (127 strains) and S. bovis (100 strains). S. anginosus, S. constellatus and S. intermedius are often placed in the Streptococcus milleri group. All isolates were non-duplicate, clinical isolates collected as part of international surveillance studies by JMI Laboratories (North Liberty, IA, USA). Twenty-one additional bacteraemic strains of S. mutans were received as a kind gift from Dr M. J. Ferraro (Massachusetts General Hospital, Boston, MA, USA).
Susceptibility testing
All strains were tested using Mueller–Hinton broth supplemented with 2–5% lysed horse blood and to 50 mg/L calcium for daptomycin according to the NCCLS M7-A6 reference broth microdilution method.9,10 Daptomycin and seven comparator agents, including penicillin (0.008–16 mg/L), erythromycin (0.008–16 mg/L), clindamycin (0.008–16 mg/L), vancomycin (0.06–2 mg/L), linezolid (0.12–16 mg/L), quinupristin/dalfopristin (0.06–8 mg/L) and tetracycline (1–8 mg/L) were tested in reference frozen-form broth microdilution panels manufactured by TREK Diagnostics Systems (Cleveland, Ohio, USA). Daptomycin and three comparator agents (penicillin, vancomycin, linezolid) were also tested against all strains using the NCCLS M2-M8 disc diffusion method on 5% sheep blood agar.11 The Mueller–Hinton blood agar was tested to confirm a satisfactory minimum calcium concentration of 25 mg/L; the one lot (Remel #416527) that was used for the disc diffusion studies had an average calcium concentration of 33 mg/L. Susceptibility to daptomycin was defined as an MIC of ≤ 1 mg/L.9
Quality control (QC)
An ATCC QC strain (S. pneumoniae ATCC 49619) was processed in parallel and all susceptibility test results were within published ranges for the MIC method.9 The modal MIC results for the QC strain were: daptomycin (0.12 mg/L), penicillin (0.25 mg/L), erythromycin (0.06 mg/L), clindamycin (0.06 mg/L), linezolid (1 mg/L), quinupristin/dalfopristin (0.25 mg/L), vancomycin (0.12 mg/L) and tetracycline ( ≤ 1 mg/L).
For disc diffusion QC, the same strain (S. pneumoniae ATCC 49619) was utilized and all zone diameters were within NCCLS specified ranges.9 The median zone diameters generated for S. pneumoniae ATCC 49619 during the study were: daptomycin (23 mm), penicillin (25 mm), linezolid (29 mm) and vancomycin (24 mm).
Results
Broth microdilution tests
The results of testing 915 streptococci by reference NCCLS MIC methods9,10 against daptomycin and seven comparison agents are summarized in Table 1. Daptomycin MIC values were in the range ≤ 0.016–2 mg/L with 99.9% of isolates inhibited by ≤ 1 mg/L. One isolate of S. oralis had a reproducible daptomycin MIC of 2 mg/L. The least daptomycin-susceptible species were S. oralis and S. sanguis (MIC90, 1 mg/L); the most susceptible species (MIC90, 0.06 mg/L) was S. bovis (group D) followed by viridans group species, S. mutans and S. salivarius (MIC90, 0.25 mg/L).
All strains of viridans group streptococci were observed to be susceptible to vancomycin at ≤ 1 mg/L. The MIC50 and MIC90 was generally 0.5 mg/L (except S. bovis MIC50, 0.25 mg/L) and only S. constellatus and S. mutans strains had a vancomycin MIC90 of 1 mg/L (breakpoint concentration). Penicillin MIC results were in the range ≤ 0.008– > 16 mg/L, and susceptibility rates varied widely (65.5–98.1%) by species. S. sanguis isolates were least penicillin-susceptible (65.5%) and S. constellatus isolates were highly susceptible (98.1%) at current NCCLS breakpoints.9
Macrolide (erythromycin) susceptibility was lowest among S. oralis strains (48.6%), whereas S. anginosus strains were more susceptible (88.7%). Another MLSB-class agent, clindamycin, had a greater level of activity against these tested viridans group streptococci. Clindamycin susceptibility rates ranged from 74.0% for S. bovis to 97.0% for S. mutans. The streptogramin combination, quinupristin/dalfopristin was very potent (99.0%–100.0% susceptible) against all species except S. bovis, (94.0% susceptible), where six strains had elevated MIC results of 2 (intermediate) or 4 mg/L (resistant).9
Tetracycline HCl, representing the class, had quite variable activities when tested against these viridans group streptococci and only tetracycline HCl among the many tetracycline derivatives has NCCLS susceptibility interpretive criteria.9 Tetracycline MIC results were usually bimodally distributed with the susceptibility rates ranging from only 35.0% (S. bovis) to 93.9% (S. mutans). Lastly, linezolid showed excellent potency versus these streptococci. MIC50 and MIC90 results were all 1 mg/L and the linezolid-susceptibility rate was 99.9%. Only one strain resistant to linezolid was observed (S. oralis, MIC at 16 mg/L).
Disc diffusion tests
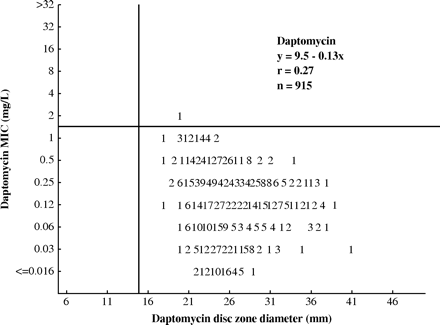
Disc diffusion test11 results were collected for daptomycin and three comparator agents (penicillin, vancomycin, linezolid). Zone diameter results were compared with daptomycin MIC values using scattergram analysis for all 915 isolates (Figure 1). Whereas all strains were daptomycin-susceptible by the disc diffusion method (zone at ≥ 16 mm), one strain (S. oralis) had a reproducible daptomycin MIC at 2 mg/L (non-susceptible) and a zone of 21 mm. The overall inter-method categorical agreement was 99.9% for daptomycin.
The linezolid scattergram comparing MIC results (mg/L) and zone diameter around the 30 μg discs produced a susceptible categorization for 99.9% of results (data not shown). Only the previously noted S. oralis strain was linezolid-non-susceptible (MIC at 16 mg/L; zone diameter at 18 mm). This isolate had a confirmed ribosomal target mutation of G2576U, a common change associated with elevated oxazolidinone MIC values ( ≥ 8 mg/L). The two in vitro linezolid testing methods were 100.0% concordant when testing these 915 streptococcal strains. The penicillin scattergram analyses could only evaluate MIC breakpoints by the NCCLS since no criteria have been recommended for the disc diffusion method.9 Disc diffusion tests poorly discriminate between penicillin-susceptible and -intermediate streptococcal populations.9 Lastly, the uniformly vancomycin-susceptible population of streptococci had vancomycin MIC values at ≤ 1 mg/L, and all zones of inhibition were ≥ 18 mm. No inter-method interpretive error was observed for vancomycin (data not shown).
Discussion
Viridans group streptococci are components of the normal flora, but these species are recognized pathogens in the immunocompromised patient. The neutropenic cancer patient is especially prone to bacteraemia caused by viridans group streptococci.12 In contrast to non-neutropenic patients, these patients are more likely to develop serious complications from the viridans group streptococci bacteraemia.12 Antimicrobial resistance in viridans group streptococci is further complicating patient management, with resistance to penicillin, other β-lactam agents and macrolides being especially problematic.
Daptomycin, although described nearly a decade ago, has recently been approved for clinical use and continues to demonstrate significant in vitro bactericidal activity against a wide spectrum of Gram-positive pathogens.1,2,5,7,8 Physiological calcium ion content of the testing medium has become an important factor in the accurate determination of daptomycin potency.2,5,6,9 Furthermore, daptomycin has demonstrated a long serum half-life (9 h) in Phase I studies, and once-daily dosing trials for 4, 6 and 8 mg/kg have been conducted, displaying evidence that daptomycin remains a safe, efficacious and well-tolerated drug.2,13
Daptomycin was very active against all species of viridans group streptococci (eight species; 815 strains) and S. bovis (100 strains) tested (Table 1). The daptomycin MIC values with appropriate calcium concentrations (50 mg/L) were in the range ≤ 0.016–2 mg/L, with 99.9% of results at ≤ 1 mg/L (MIC90s, 0.06–1 mg/L). Only linezolid and vancomycin showed comparable activity ( ≤ 99.9%) to daptomycin. Quinupristin/dalfopristin was only slightly less effective in vitro (Table 1). Comparing results found in historical studies with the present investigation, there has been little change in daptomycin perceived activity against viridans group streptococci or S. bovis.1,7,8,12 Other studies have reported daptomycin MIC values at ≤ 2 mg/L using calcium supplemented broth when testing viridans group streptococci. In an early study,1 104 streptococcal strains were found to have an MIC range of ≤ 0.016–1 mg/L for daptomycin and an MIC90 of 0.25 mg/L. More recently, Critchley and colleagues7 tested 369 viridans group streptococci and all strains were inhibited by ≤ 2 mg/L of daptomycin, but displayed an elevated MIC90 of 1 mg/L.11 A European study validated Critchley et al.7 by testing a smaller number of viridans group streptococci (51) on both Mueller–Hinton and isotonic agar adjusted to contain 50 mg/L of calcium.8 The NCCLS does not recommend the use of an agar dilution method for testing daptomycin.9
Comparable susceptibility testing results were achieved with the daptomycin disc diffusion test with only one false-susceptible error [MIC at 2 mg/L (non-susceptible); zone at 21 mm (susceptible)] detected. Generally, both the reference broth microdilution (with 50 mg/L calcium) and the disc diffusion method (with media containing at least 25 mg/L of calcium) produced high inter-method accuracy5,6,9 as confirmed here. Such studies should be re-considered when true daptomycin-resistant isolates have been documented.
In conclusion, daptomycin has demonstrated activity against many of the commonly occurring Gram-positive pathogens and has been recently approved by the US-FDA for use in selected staphylococcal and E. faecalis infections. Results from this comparison of two NCCLS in vitro susceptibility test methods using a large, comprehensive streptococcal organism collection demonstrates that daptomycin is a potent antimicrobial agent active against viridans group streptococci, and is an excellent candidate for further clinical trials targeting serious infections produced by these species. The NCCLS has adopted a daptomycin-susceptible breakpoint of ≤ 1 mg/L when testing ‘Streptococcus spp. other than S. pneumoniae (β-haemolytic streptococci only).’9
Scattergram displaying the relationship of daptomycin MIC (mg/L) and the disc inhibitory zone diameter (mm) for 915 viridans group Streptococcus spp.
In vitro activity of daptomycin and seven comparative antimicrobial agents tested against 815 viridans group streptococci and S. bovis (100 strains)
| . | MIC (mg/L) . | . | . | . | ||||
|---|---|---|---|---|---|---|---|---|
| Organism/antimicrobial agent (no. tested) . | 50% . | 90% . | range . | % Susceptiblea . | ||||
| S. anginosus (106) | ||||||||
| daptomycin | 0.25 | 0.5 | ≤ 0.016–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.12 | ≤ 0.008–2 | 93.4 | ||||
| erythromycin | 0.03 | 1 | ≤ 0.008– > 16 | 88.7 | ||||
| clindamycin | 0.03 | 0.03 | ≤ 0.008– > 16 | 94.3 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 72.6 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–1 | 100.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. bovis (100) | ||||||||
| daptomycin | 0.03 | 0.06 | 0.03–0.25 | 100.0b | ||||
| vancomycin | 0.25 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008–1 | 97.0 | ||||
| erythromycin | 0.03 | > 16 | ≤ 0.008– > 16 | 54.0 | ||||
| clindamycin | 0.06 | > 16 | ≤ 0.008– > 16 | 74.0 | ||||
| tetracycline | > 8 | > 8 | ≤ 1– > 8 | 35.0 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–4 | 94.0 | ||||
| linezolid | 1 | 1 | 0.5–2 | 100.0 | ||||
| S. constellatus (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008– > 16 | 98.1 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 86.4 | ||||
| clindamycin | 0.03 | 0.06 | ≤ 0.008– > 16 | 93.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 79.6 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–1 | 100.0 | ||||
| S. intermedius (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008–16 | 87.4 | ||||
| erythromycin | 0.03 | 2 | ≤ 0.008– > 16 | 79.6 | ||||
| clindamycin | 0.016 | 0.03 | ≤ 0.008– > 16 | 92.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 74.8 | ||||
| quinupristin/dalfopristin | 0.5 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mitis (102) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.06 | 2 | ≤ 0.008– > 16 | 68.6 | ||||
| erythromycin | 0.25 | 4 | ≤ 0.008– > 16 | 52.9 | ||||
| clindamycin | 0.016 | 4 | ≤ 0.008– > 16 | 89.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 65.7 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mutans (66) | ||||||||
| daptomycin | 0.12 | 0.25 | 0.03–0.5 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.12–1 | 100.0 | ||||
| penicillin | 0.016 | 0.12 | ≤ 0.008–4 | 90.9 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 83.3 | ||||
| clindamycin | ≤ 0.008 | 0.06 | ≤ 0.008– > 16 | 97.0 | ||||
| tetracycline | ≤ 1 | ≤ 1 | ≤ 1– > 8 | 93.9 | ||||
| quinupristin/dalfopristin | 0.25 | 1 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. oralis (107) | ||||||||
| daptomycin | 0.5 | 1 | 0.03–2 | 99.1b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–0.5 | 100.0 | ||||
| penicillin | 0.06 | 4 | ≤ 0.008– > 16 | 66.4 | ||||
| erythromycin | 0.5 | > 16 | ≤ 0.008– > 16 | 48.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 84.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 69.2 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–2 | 99.1 | ||||
| linezolid | 1 | 1 | 0.25–16 | 99.1 | ||||
| S. salivarius (101) | ||||||||
| daptomycin | 0.06 | 0.25 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008– > 16 | 73.3 | ||||
| erythromycin | 0.016 | 8 | ≤ 0.008– > 16 | 65.3 | ||||
| clindamycin | ≤ 0.008 | 0.03 | ≤ 0.008- > 16 | 92.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.3 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. sanguis (127) | ||||||||
| daptomycin | 0.25 | 1 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 1 | ≤ 0.008– > 16 | 65.5 | ||||
| erythromycin | 0.016 | > 16 | ≤ 0.008– > 16 | 64.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 89.0 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.7 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.2 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| . | MIC (mg/L) . | . | . | . | ||||
|---|---|---|---|---|---|---|---|---|
| Organism/antimicrobial agent (no. tested) . | 50% . | 90% . | range . | % Susceptiblea . | ||||
| S. anginosus (106) | ||||||||
| daptomycin | 0.25 | 0.5 | ≤ 0.016–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.12 | ≤ 0.008–2 | 93.4 | ||||
| erythromycin | 0.03 | 1 | ≤ 0.008– > 16 | 88.7 | ||||
| clindamycin | 0.03 | 0.03 | ≤ 0.008– > 16 | 94.3 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 72.6 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–1 | 100.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. bovis (100) | ||||||||
| daptomycin | 0.03 | 0.06 | 0.03–0.25 | 100.0b | ||||
| vancomycin | 0.25 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008–1 | 97.0 | ||||
| erythromycin | 0.03 | > 16 | ≤ 0.008– > 16 | 54.0 | ||||
| clindamycin | 0.06 | > 16 | ≤ 0.008– > 16 | 74.0 | ||||
| tetracycline | > 8 | > 8 | ≤ 1– > 8 | 35.0 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–4 | 94.0 | ||||
| linezolid | 1 | 1 | 0.5–2 | 100.0 | ||||
| S. constellatus (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008– > 16 | 98.1 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 86.4 | ||||
| clindamycin | 0.03 | 0.06 | ≤ 0.008– > 16 | 93.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 79.6 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–1 | 100.0 | ||||
| S. intermedius (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008–16 | 87.4 | ||||
| erythromycin | 0.03 | 2 | ≤ 0.008– > 16 | 79.6 | ||||
| clindamycin | 0.016 | 0.03 | ≤ 0.008– > 16 | 92.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 74.8 | ||||
| quinupristin/dalfopristin | 0.5 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mitis (102) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.06 | 2 | ≤ 0.008– > 16 | 68.6 | ||||
| erythromycin | 0.25 | 4 | ≤ 0.008– > 16 | 52.9 | ||||
| clindamycin | 0.016 | 4 | ≤ 0.008– > 16 | 89.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 65.7 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mutans (66) | ||||||||
| daptomycin | 0.12 | 0.25 | 0.03–0.5 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.12–1 | 100.0 | ||||
| penicillin | 0.016 | 0.12 | ≤ 0.008–4 | 90.9 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 83.3 | ||||
| clindamycin | ≤ 0.008 | 0.06 | ≤ 0.008– > 16 | 97.0 | ||||
| tetracycline | ≤ 1 | ≤ 1 | ≤ 1– > 8 | 93.9 | ||||
| quinupristin/dalfopristin | 0.25 | 1 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. oralis (107) | ||||||||
| daptomycin | 0.5 | 1 | 0.03–2 | 99.1b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–0.5 | 100.0 | ||||
| penicillin | 0.06 | 4 | ≤ 0.008– > 16 | 66.4 | ||||
| erythromycin | 0.5 | > 16 | ≤ 0.008– > 16 | 48.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 84.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 69.2 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–2 | 99.1 | ||||
| linezolid | 1 | 1 | 0.25–16 | 99.1 | ||||
| S. salivarius (101) | ||||||||
| daptomycin | 0.06 | 0.25 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008– > 16 | 73.3 | ||||
| erythromycin | 0.016 | 8 | ≤ 0.008– > 16 | 65.3 | ||||
| clindamycin | ≤ 0.008 | 0.03 | ≤ 0.008- > 16 | 92.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.3 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. sanguis (127) | ||||||||
| daptomycin | 0.25 | 1 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 1 | ≤ 0.008– > 16 | 65.5 | ||||
| erythromycin | 0.016 | > 16 | ≤ 0.008– > 16 | 64.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 89.0 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.7 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.2 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
Susceptible percentages were established using NCCLS criteria (M100-S15).9
A breakpoint of ≤ 1 mg/L was utilized to determine susceptibility rates for comparative purposes only. NCCLS interpretive criteria have not been established for the viridans group of streptococci, however, breakpoints used for staphylococci ( ≤ 1 mg/L), enterococci ( ≤ 4 mg/L) and β-haemolytic streptococci ( ≤ 1 mg/L) have been approved for publication.9
In vitro activity of daptomycin and seven comparative antimicrobial agents tested against 815 viridans group streptococci and S. bovis (100 strains)
| . | MIC (mg/L) . | . | . | . | ||||
|---|---|---|---|---|---|---|---|---|
| Organism/antimicrobial agent (no. tested) . | 50% . | 90% . | range . | % Susceptiblea . | ||||
| S. anginosus (106) | ||||||||
| daptomycin | 0.25 | 0.5 | ≤ 0.016–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.12 | ≤ 0.008–2 | 93.4 | ||||
| erythromycin | 0.03 | 1 | ≤ 0.008– > 16 | 88.7 | ||||
| clindamycin | 0.03 | 0.03 | ≤ 0.008– > 16 | 94.3 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 72.6 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–1 | 100.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. bovis (100) | ||||||||
| daptomycin | 0.03 | 0.06 | 0.03–0.25 | 100.0b | ||||
| vancomycin | 0.25 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008–1 | 97.0 | ||||
| erythromycin | 0.03 | > 16 | ≤ 0.008– > 16 | 54.0 | ||||
| clindamycin | 0.06 | > 16 | ≤ 0.008– > 16 | 74.0 | ||||
| tetracycline | > 8 | > 8 | ≤ 1– > 8 | 35.0 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–4 | 94.0 | ||||
| linezolid | 1 | 1 | 0.5–2 | 100.0 | ||||
| S. constellatus (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008– > 16 | 98.1 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 86.4 | ||||
| clindamycin | 0.03 | 0.06 | ≤ 0.008– > 16 | 93.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 79.6 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–1 | 100.0 | ||||
| S. intermedius (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008–16 | 87.4 | ||||
| erythromycin | 0.03 | 2 | ≤ 0.008– > 16 | 79.6 | ||||
| clindamycin | 0.016 | 0.03 | ≤ 0.008– > 16 | 92.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 74.8 | ||||
| quinupristin/dalfopristin | 0.5 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mitis (102) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.06 | 2 | ≤ 0.008– > 16 | 68.6 | ||||
| erythromycin | 0.25 | 4 | ≤ 0.008– > 16 | 52.9 | ||||
| clindamycin | 0.016 | 4 | ≤ 0.008– > 16 | 89.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 65.7 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mutans (66) | ||||||||
| daptomycin | 0.12 | 0.25 | 0.03–0.5 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.12–1 | 100.0 | ||||
| penicillin | 0.016 | 0.12 | ≤ 0.008–4 | 90.9 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 83.3 | ||||
| clindamycin | ≤ 0.008 | 0.06 | ≤ 0.008– > 16 | 97.0 | ||||
| tetracycline | ≤ 1 | ≤ 1 | ≤ 1– > 8 | 93.9 | ||||
| quinupristin/dalfopristin | 0.25 | 1 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. oralis (107) | ||||||||
| daptomycin | 0.5 | 1 | 0.03–2 | 99.1b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–0.5 | 100.0 | ||||
| penicillin | 0.06 | 4 | ≤ 0.008– > 16 | 66.4 | ||||
| erythromycin | 0.5 | > 16 | ≤ 0.008– > 16 | 48.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 84.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 69.2 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–2 | 99.1 | ||||
| linezolid | 1 | 1 | 0.25–16 | 99.1 | ||||
| S. salivarius (101) | ||||||||
| daptomycin | 0.06 | 0.25 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008– > 16 | 73.3 | ||||
| erythromycin | 0.016 | 8 | ≤ 0.008– > 16 | 65.3 | ||||
| clindamycin | ≤ 0.008 | 0.03 | ≤ 0.008- > 16 | 92.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.3 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. sanguis (127) | ||||||||
| daptomycin | 0.25 | 1 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 1 | ≤ 0.008– > 16 | 65.5 | ||||
| erythromycin | 0.016 | > 16 | ≤ 0.008– > 16 | 64.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 89.0 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.7 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.2 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| . | MIC (mg/L) . | . | . | . | ||||
|---|---|---|---|---|---|---|---|---|
| Organism/antimicrobial agent (no. tested) . | 50% . | 90% . | range . | % Susceptiblea . | ||||
| S. anginosus (106) | ||||||||
| daptomycin | 0.25 | 0.5 | ≤ 0.016–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.12 | ≤ 0.008–2 | 93.4 | ||||
| erythromycin | 0.03 | 1 | ≤ 0.008– > 16 | 88.7 | ||||
| clindamycin | 0.03 | 0.03 | ≤ 0.008– > 16 | 94.3 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 72.6 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–1 | 100.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. bovis (100) | ||||||||
| daptomycin | 0.03 | 0.06 | 0.03–0.25 | 100.0b | ||||
| vancomycin | 0.25 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008–1 | 97.0 | ||||
| erythromycin | 0.03 | > 16 | ≤ 0.008– > 16 | 54.0 | ||||
| clindamycin | 0.06 | > 16 | ≤ 0.008– > 16 | 74.0 | ||||
| tetracycline | > 8 | > 8 | ≤ 1– > 8 | 35.0 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–4 | 94.0 | ||||
| linezolid | 1 | 1 | 0.5–2 | 100.0 | ||||
| S. constellatus (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.25–1 | 100.0 | ||||
| penicillin | 0.03 | 0.06 | ≤ 0.008– > 16 | 98.1 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 86.4 | ||||
| clindamycin | 0.03 | 0.06 | ≤ 0.008– > 16 | 93.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 79.6 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–1 | 100.0 | ||||
| S. intermedius (103) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008–16 | 87.4 | ||||
| erythromycin | 0.03 | 2 | ≤ 0.008– > 16 | 79.6 | ||||
| clindamycin | 0.016 | 0.03 | ≤ 0.008– > 16 | 92.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 74.8 | ||||
| quinupristin/dalfopristin | 0.5 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mitis (102) | ||||||||
| daptomycin | 0.25 | 0.5 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.12–0.5 | 100.0 | ||||
| penicillin | 0.06 | 2 | ≤ 0.008– > 16 | 68.6 | ||||
| erythromycin | 0.25 | 4 | ≤ 0.008– > 16 | 52.9 | ||||
| clindamycin | 0.016 | 4 | ≤ 0.008– > 16 | 89.2 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 65.7 | ||||
| quinupristin/dalfopristin | 0.25 | 0.5 | ≤ 0.06–2 | 99.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. mutans (66) | ||||||||
| daptomycin | 0.12 | 0.25 | 0.03–0.5 | 100.0b | ||||
| vancomycin | 0.5 | 1 | 0.12–1 | 100.0 | ||||
| penicillin | 0.016 | 0.12 | ≤ 0.008–4 | 90.9 | ||||
| erythromycin | 0.016 | 2 | ≤ 0.008– > 16 | 83.3 | ||||
| clindamycin | ≤ 0.008 | 0.06 | ≤ 0.008– > 16 | 97.0 | ||||
| tetracycline | ≤ 1 | ≤ 1 | ≤ 1– > 8 | 93.9 | ||||
| quinupristin/dalfopristin | 0.25 | 1 | 0.12–1 | 100.0 | ||||
| linezolid | 1 | 1 | ≤ 0.12–2 | 100.0 | ||||
| S. oralis (107) | ||||||||
| daptomycin | 0.5 | 1 | 0.03–2 | 99.1b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–0.5 | 100.0 | ||||
| penicillin | 0.06 | 4 | ≤ 0.008– > 16 | 66.4 | ||||
| erythromycin | 0.5 | > 16 | ≤ 0.008– > 16 | 48.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 84.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 69.2 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | ≤ 0.06–2 | 99.1 | ||||
| linezolid | 1 | 1 | 0.25–16 | 99.1 | ||||
| S. salivarius (101) | ||||||||
| daptomycin | 0.06 | 0.25 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 0.5 | ≤ 0.008– > 16 | 73.3 | ||||
| erythromycin | 0.016 | 8 | ≤ 0.008– > 16 | 65.3 | ||||
| clindamycin | ≤ 0.008 | 0.03 | ≤ 0.008- > 16 | 92.1 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.3 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.0 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
| S. sanguis (127) | ||||||||
| daptomycin | 0.25 | 1 | 0.03–1 | 100.0b | ||||
| vancomycin | 0.5 | 0.5 | 0.25–1 | 100.0 | ||||
| penicillin | 0.06 | 1 | ≤ 0.008– > 16 | 65.5 | ||||
| erythromycin | 0.016 | > 16 | ≤ 0.008– > 16 | 64.6 | ||||
| clindamycin | 0.016 | > 16 | ≤ 0.008– > 16 | 89.0 | ||||
| tetracycline | ≤ 1 | > 8 | ≤ 1– > 8 | 71.7 | ||||
| quinupristin/dalfopristin | 0.5 | 1 | 0.12–2 | 99.2 | ||||
| linezolid | 1 | 1 | 0.25–2 | 100.0 | ||||
Susceptible percentages were established using NCCLS criteria (M100-S15).9
A breakpoint of ≤ 1 mg/L was utilized to determine susceptibility rates for comparative purposes only. NCCLS interpretive criteria have not been established for the viridans group of streptococci, however, breakpoints used for staphylococci ( ≤ 1 mg/L), enterococci ( ≤ 4 mg/L) and β-haemolytic streptococci ( ≤ 1 mg/L) have been approved for publication.9
We express our gratitude to the following JMI Laboratories staff for their contributions to this submission: Drs T. R. Fritsche and H. S. Sader; and D. J. Biedenbach, P. Rhomberg, K. Meyer and M. Stilwell.
References
Jones, R. N. & Barry, A. L. (
Thorne, G. M. & Alder, J. (
Silverman, J. A., Perimutter, N. G. & Shapiro, H. M. (
Laganas, V., Alder, J. S. & Werman, J. A. (
Fuchs, P. C., Barry, A. L. & Brown, S. D. (
Fuchs, P. C., Barry, A. L. & Brown, S. D. (
Critchley, I. A., Blosser-Middleton, R. S., Jones, M. E. et al. (
King, A. & Phillips, I. (
National Committee for Clinical Laboratory Standards. (
National Committee for Clinical Laboratory Standards. (
National Committee for Clinical Laboratory Standards. (
Diekema, D. J., Beach, M. L., Pfaller, M. A. et al. (
Author notes
1The JONES Group/JMI Laboratories, North Liberty, IA; 2Cubist Pharmaceuticals, Lexington, MA; 3Tufts University School of Medicine, Boston, MA, USA