-
PDF
- Split View
-
Views
-
Cite
Cite
Åke Hjalmarson, Heart rate: an independent risk factor in cardiovascular disease, European Heart Journal Supplements, Volume 9, Issue suppl_F, September 2007, Pages F3–F7, https://doi.org/10.1093/eurheartj/sum030
Close - Share Icon Share
Abstract
Large epidemiological studies have demonstrated that elevated heart rate is an independent risk factor for mortality and morbidity in healthy individuals with and without hypertension and in patients with coronary artery disease (CAD), myocardial infarction, and congestive heart failure. Elevated heart rate has been found to be a more powerful predictor of later death than depressed left ventricular function. This means that heart rate in patients with congestive heart failure is not only reflecting depressed cardiac function. Heart rate should be viewed in the same light as other risk factors, such as elevated blood pressure or cholesterol, smoking, cardiac dysfunction, or diabetes. It is well documented that interventions against these risk factors improve prognosis, in terms of both primary and secondary prevention. Several large placebo-controlled trials of patients with acute myocardial infarction or congestive heart failure have demonstrated that beta-blocking agents reduce mortality and morbidity. In fact, the effects seem to be more marked in patients with higher pre-treatment heart rates, and these patients also demonstrate a more marked reduction in heart rate. It seems reasonable to believe that heart rate reduction per se is of major importance for the effects of beta-blockers. Beneficial effects on the prognosis after myocardial infarction have also been shown for some calcium antagonists, which also reduce heart rate. Heart rate should be considered as an important risk factor in patients at risk of CAD or with established CAD. Treatment should be started to reduce heart rate to a normal level, similar to the aim in the treatment of patients with hypertension.
Normal population and subjects with hypertension
Epidemiological data on the long-term follow-up of healthy individuals have demonstrated that there is an independent association between elevated heart rate and cardiovascular mortality and morbidity. Published studies on the general population and subjects with hypertension include approximately 180 000 individuals and show that cardiovascular mortality is significantly increased with elevated heart rate.1–3 In the Framingham study (n = 5070), there was a 30-year follow-up of healthy men and women. Although the increase in the overall mortality as a consequence of elevated resting heart rate was more marked among men, it was also found to be significant among women and in both younger and older individuals (Table 1).4 In another American study on healthy subjects aged 25–74 years who were followed for between 6 and 13 years (n = 5995), elevated resting heart rate was found to be an independent risk factor for coronary artery disease (CAD) incidence or death among white and black men and women.5 In several studies of healthy men and women, it has been found that elevated resting heart rate is not only a predictor of all-cause mortality, but also an independent risk predictor of sudden cardiac death.6,7
Coronary artery disease at baseline
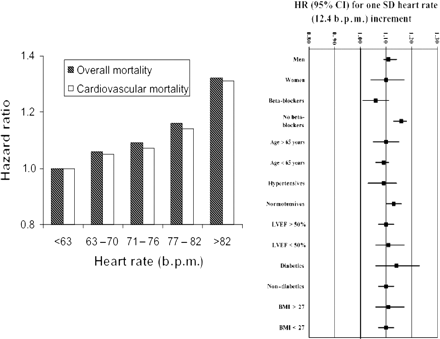
In patients with CAD at baseline, elevated heart rate is an independent risk predictor for major ischaemic coronary events, cardiovascular mortality, and sudden cardiac death, in a manner very similar to that seen in healthy individuals.8–12 In the Coronary Artery Surgery Study (CASS) registry, which included 24 913 men and women with suspected or proven CAD with a median follow-up time of 14.7 years, resting heart rate was found to be a predictor of overall and cardiovascular mortality.11 This study population was large enough to allow subgroup analysis, and the association between heart rate and total mortality held true in all analysed subgroups regardless of sex, age, hypertension, cardiac function, body weight, presence of diabetes, or use of beta-blockers (Figure 1). Heart rate was also a predictor of time to first rehospitalization because of congestive heart failure. In a large British study, heart rate was found to be a predictor of major ischaemic heart disease events, cardiovascular mortality, and sudden cardiac death, both in patients with CAD and in the normal population with or without hypertension.9
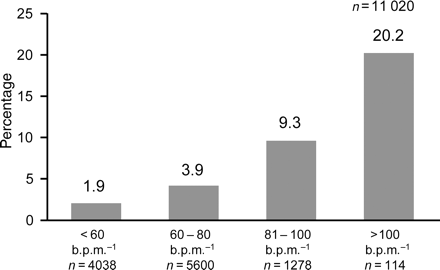
In patients with acute myocardial infarction, the resting heart rate on arrival in the emergency room and the average heart rate during the hospital stay or at the time of discharge are independent and highly significant predictors of later death.8 In this study from hospitals in San Diego (n = 1807), heart rate was found to be a more powerful predictor of later mortality than assessment of left ventricular function after arrival in hospital. This clearly demonstrates that heart rate is not only reflecting depressed cardiac function, which has for long been the general assumption. Very similar observations were made in the Gruppo Italiano per lo Studio della Sopravvivenza nell'Infarto miocardico-3 (GISSI-3) study (n = 11 020) on patients with acute myocardial infarction, which showed that elevated heart rate at discharge was highly significant and independently correlated with 6-month mortality (Figure 2).10
Patients with heart failure
Large trials on patients with congestive heart failure have demonstrated that baseline heart rate is an independent risk predictor of all-cause mortality, cardiovascular mortality, and hospitalization for congestive heart failure.13–15 This was the case in the MEtoprolol CR/XL Randomized Intervention Trial in Heart Failure (MERIT-HF, n = 3991), but only in the placebo-treated patients (Table 2).14 In this study, mean baseline heart rate was analysed by quintiles of heart rate [mean heart rate of the lowest quintile was 71 beats per minute (b.p.m.) and in the highest quintile, it was 98 b.p.m.]. In this trial, with increasing baseline heart rate, age was lower, there were more females, ejection fraction was lower, more patients were in the New York Heart Association Classes III and IV, more patients had a non-ischaemic aetiology, and there was a higher presence of diabetes. This tells us that patients with a higher heart rate are very different from those with a lower heart rate; in general, patients with a higher heart rate have more risk factors. Even when adjusting for these differences, however, heart rate is an independent risk predictor of prognosis. Data from the large Cardiac Insufficiency Bisoprolol Study-II (CIBIS-II, n = 2539), also carried out in patients with chronic heart failure, showed that heart rate was a strong predictor of 1-year mortality, was most marked in the placebo group, and was blunted by beta-blocker treatment.15
Pathophysiological evidence
High resting heart rate reflects an imbalance of the autonomic nervous system, with increased sympathetic activity and/or reduced vagal activity. Heart rate is a major determinant of myocardial oxygen consumption and energy utilization; furthermore, an increase in heart rate reduces the diastolic coronary perfusion time. By way of these two mechanisms, an increase in heart rate may trigger ischaemic events. An increase in sympathetic activity and/or lowering of vagal activity are known to increase the risk of ventricular fibrillation in experimental studies on myocardial ischaemia. It is well known that psychosocial stress-associated increases in heart rate can trigger the onset of acute myocardial infarction, in addition to sudden cardiac death. This has been well documented in the literature, and one example of an increase in attacks of sudden death occurred during the San Francisco earthquake in 1994.16 During the earthquake, there was a seven-fold increase in the risk of sudden cardiac death reported by hospitals in the region. Elevated heart rate during mental stress may play a key role in the development of sudden cardiac death. It is well known that the incidence of sudden cardiac death among patients with hypertension, myocardial infarction, or congestive heart failure is reduced by beta-blockers.17
Experimental data have demonstrated that elevated heart rate has a role in the development of atherosclerosis and plaque disruption. Studies in monkeys have shown that a reduction in heart rate can delay the progression of coronary atherosclerosis.18 In addition, it has been shown that monkeys subjected to sinus node ablation or treatment with beta-blockers have significantly less coronary atherosclerosis than animals not receiving these treatments and with a higher heart rate.19,20 High heart rates have been associated with coronary artery endothelial dysfunction in experimental studies.21,22 These observations are supported by results from the Beta-blocker Cholesterol lowering Asymptomatic Plaque Study (BCAPS), a randomized trial that showed that administration of a beta-blocker reduces the rate of progression of carotid artery intima thickness in asymptomatic subjects.23 Furthermore, in a multivariable analysis, it was shown that elevated heart rate is associated with coronary plaque disruption in patients.24 There is good experimental and clinical evidence that high heart rate is of importance in the development and progression of atherosclerosis, myocardial ischaemia, acute ischaemic events, and sudden cardiac death, and that a reduction in heart rate has beneficial effects.
Effects of heart rate reduction
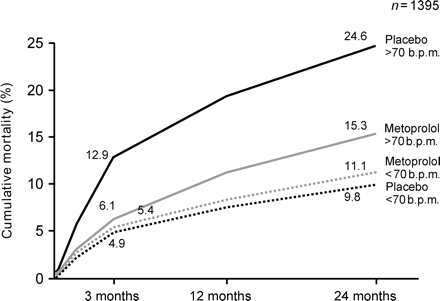
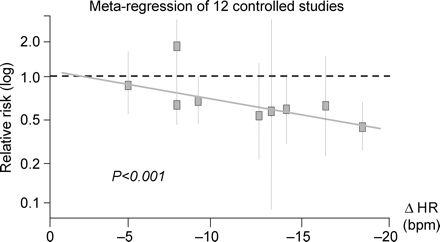
In 1981, three large trials of patients with acute myocardial infarction demonstrated that beta-blockers such as timolol, metoprolol, and propranolol reduced all-cause mortality, cardiovascular and sudden cardiac death, and hospitalization.25–27 In these studies, it was also noted that patients with a heart rate above the median at baseline had a higher mortality during follow-up and that the effect of the beta-blockers was most marked in the patients with the highest heart rate at baseline. In the Göteborg Metoprolol trial, it was also found that all of the beneficial effects of the beta-blocker metoprolol were most marked in patients whose heart rate was above the median at baseline (>70 b.p.m.).26,28 These effects included reduction in all-cause mortality at 3–24 months (Figure 3), sudden cardiac death, ventricular fibrillation, infarct development, and enzyme-estimated infarct size. By analysing all placebo-controlled beta-blocker studies in patients with acute myocardial infarction, it was proposed by Kjekshus and Gullestad29,30 that there was a significant relationship between the reduction in resting heart rate and the decrease in all-cause mortality. Recently new meta-regression of randomized, placebo-controlled trials of long-term β-blocker treatment in patients surviving myocardial infarction has a similar significant reduction in log odds ratio for cardiac death (P = 0.02) (Figure 4), sudden death (P < 0.01), and reinfarction (P < 0.01). The same relationship between changes in heart rate and all-cause mortality in patients with chronic heart failure—not only with the use of beta-blockers, but also, for example, with angiotensin-converting enzyme inhibitors. In the two large trials on patients with chronic heart failure, CIBIS-II and MERIT-HF, patients with a higher heart rate at baseline had the highest mortality, and among these patients, there was a more marked effect of the beta-blockers disoprolol and metoprolol CR/XL.14,15
Conclusion
It can be concluded that heart rate is an independent risk predictor of the onset of acute coronary events, including all-cause mortality, cardiovascular mortality, sudden cardiac death, and acute coronary syndromes, and also the development of myocardial infarction. Measurement of heart rate should be carried out in patients with or without established ischaemic heart disease and should be viewed in the same light as other risk factors, such as high blood pressure and cholesterol, smoking, cardiac dysfunction, and diabetes. Hypertension, smoking, depressed cardiac function, and diabetes are all associated with an elevated heart rate. It is known that interventions against these risk factors improve prognosis. In several large placebo-controlled trials of patients with acute myocardial infarction or chronic heart failure, beta-blocking agents have shown more marked effects on mortality in patients with higher pre-treatment heart rates. It is reasonable to believe that the heart rate reduction per se is of major importance in these effects of beta-blockers. With the introduction of ivabradine, the first selective and specific If inhibitor, heart rate reduction can be obtained without affecting sympathetic activity or contractility. Whether heart rate reduction per se with ivabradine will have the potential not only to reduce anginal attacks and myocardial ischaemia, but also to improve prognosis in patients with CAD and left ventricular dysfunction and in patients with chronic heart failure is presently being tested in the ongoing large-scale studies, BEAUTIfUL31 and SHIfT.32
Conflict of interest: none declared.
Mortality related to heart rate among men and women in the Framingham study4
| Resting heart rate (b.p.m.) . | Age-adjusted annual rate/1000 . | |||
|---|---|---|---|---|
| Men . | Women . | |||
| 36–64 . | 65–94 . | 35–64 . | 65–94 . | |
| 30–67 | 6 | 35 | 3 | 22 |
| 68–75 | 8 | 43 | 4 | 28 |
| 76–83 | 11 | 46 | 6 | 25 |
| 84–91 | 13 | 61 | 8 | 30 |
| 92–220 | 14 | 64 | 9 | 35 |
| Resting heart rate (b.p.m.) . | Age-adjusted annual rate/1000 . | |||
|---|---|---|---|---|
| Men . | Women . | |||
| 36–64 . | 65–94 . | 35–64 . | 65–94 . | |
| 30–67 | 6 | 35 | 3 | 22 |
| 68–75 | 8 | 43 | 4 | 28 |
| 76–83 | 11 | 46 | 6 | 25 |
| 84–91 | 13 | 61 | 8 | 30 |
| 92–220 | 14 | 64 | 9 | 35 |
n = 5070.
Mortality related to heart rate among men and women in the Framingham study4
| Resting heart rate (b.p.m.) . | Age-adjusted annual rate/1000 . | |||
|---|---|---|---|---|
| Men . | Women . | |||
| 36–64 . | 65–94 . | 35–64 . | 65–94 . | |
| 30–67 | 6 | 35 | 3 | 22 |
| 68–75 | 8 | 43 | 4 | 28 |
| 76–83 | 11 | 46 | 6 | 25 |
| 84–91 | 13 | 61 | 8 | 30 |
| 92–220 | 14 | 64 | 9 | 35 |
| Resting heart rate (b.p.m.) . | Age-adjusted annual rate/1000 . | |||
|---|---|---|---|---|
| Men . | Women . | |||
| 36–64 . | 65–94 . | 35–64 . | 65–94 . | |
| 30–67 | 6 | 35 | 3 | 22 |
| 68–75 | 8 | 43 | 4 | 28 |
| 76–83 | 11 | 46 | 6 | 25 |
| 84–91 | 13 | 61 | 8 | 30 |
| 92–220 | 14 | 64 | 9 | 35 |
n = 5070.
Mortality related to heart rate in the Coronary Artery Surgery Study registry, in all patients and in subgroups. Reproduced from Diaz et al.11
Mortality at 6 months of follow-up in patients with acute myocardial infarction: the GISSI experience.10
Mortality related to baseline heart rate among placebo and metoprolol CR/XL subjects in the MERIT-HF trial14
| Endpoint . | Placebo n = 2001 . | Metoprolol CR/XL n = 1990 . | ||
|---|---|---|---|---|
| P-value . | No. of events . | P-value . | No. of events . | |
| All-cause mortality | 0.003 | 217 | ns | 145 |
| CV mortality | 0.006 | 203 | ns | 128 |
| Pts hospitalized (CHF) | <0.0001 | 294 | ns | 200 |
| Endpoint . | Placebo n = 2001 . | Metoprolol CR/XL n = 1990 . | ||
|---|---|---|---|---|
| P-value . | No. of events . | P-value . | No. of events . | |
| All-cause mortality | 0.003 | 217 | ns | 145 |
| CV mortality | 0.006 | 203 | ns | 128 |
| Pts hospitalized (CHF) | <0.0001 | 294 | ns | 200 |
n = 3991 Cox-adjusted. CHF, congestive heart failure; CV, cardiovascular; ns, non-significant; Pts, patients.
Mortality related to baseline heart rate among placebo and metoprolol CR/XL subjects in the MERIT-HF trial14
| Endpoint . | Placebo n = 2001 . | Metoprolol CR/XL n = 1990 . | ||
|---|---|---|---|---|
| P-value . | No. of events . | P-value . | No. of events . | |
| All-cause mortality | 0.003 | 217 | ns | 145 |
| CV mortality | 0.006 | 203 | ns | 128 |
| Pts hospitalized (CHF) | <0.0001 | 294 | ns | 200 |
| Endpoint . | Placebo n = 2001 . | Metoprolol CR/XL n = 1990 . | ||
|---|---|---|---|---|
| P-value . | No. of events . | P-value . | No. of events . | |
| All-cause mortality | 0.003 | 217 | ns | 145 |
| CV mortality | 0.006 | 203 | ns | 128 |
| Pts hospitalized (CHF) | <0.0001 | 294 | ns | 200 |
n = 3991 Cox-adjusted. CHF, congestive heart failure; CV, cardiovascular; ns, non-significant; Pts, patients.
Mortality related to heart rate at baseline (below or above median) in patients with suspected acute myocardial infarction on arrival in the emergency room and in the placebo and metoprolol groups of the Göteborg Metoprolol Trial.28
Relationship between heart rate lowering and benefits on cardiac death observed with β-blockers in postmyocardial infarction.29
References
MERIT-HF Study Group. Effect of metoprolol CR/XL in chronic heart failure: Metoprolol CR/XL Randomised Intervention Trial in Congestive Heart Failure (MERIT-HF).
The Norwegian Multicenter Study Group. Timolol-induced reduction in mortality reinfarction in patients surviving acute myocardial infarction.
The Beta-Blocker Heart Attack Study Group. The beta-blocker heart attack trial preliminary report.
Current Controlled Trials. ISRCTN70429960: effects of ivabradine on cardiovascular events in patients with moderate to severe chronic heart failure: left ventricular systolic dysfunction. A three-year randomised double-blind placebo-controlled international multicentre study [online]. http://www.controlled-trials.com/ISRCTN70429960/ivabradine (1 May 2007).