-
PDF
- Split View
-
Views
-
Cite
Cite
Thomas F. Kresina, R. Douglas Bruce, Victoria A. Cargill, Laura W. Cheever, Integrating Care for Hepatitis C Virus (HCV) and Primary Care for HIV for Injection Drug Users Coinfected with HIV and HCV, Clinical Infectious Diseases, Volume 41, Issue Supplement_1, July 2005, Pages S83–S88, https://doi.org/10.1086/429502
Close - Share Icon Share
Abstract
Injection drug use accounts for most of the incident infections with hepatitis C virus (HCV) and for at least one-third of new human immunodeficiency virus (HIV) infections. Coinfection with HCV and HIV presents complex and challenging medical conditions. Ensuring access to and maintaining care for HIV and HCV for drug users presents special challenges to the health care team that require a nonjudgmental attitude, experience, and patience. Care for HCV infection, however, can be used as an instrument to engage drug-using persons in ongoing primary care relationships. Common elements to both care for HCV infection and primary care for HIV infection are testing for and counseling about HCV and HIV, substance abuse and mental health services, social support, and subspecialty referral. These elements, in particular treatment for substance abuse, can be focal points for model care systems that provide integrative care for both HCV and HIV infections.
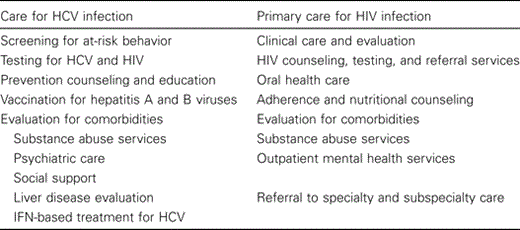
Injection drug users (IDUs) constitute the largest group of persons infected with hepatitis C virus (HCV) and HIV in the United States. The prevalence of HCV antibody among IDUs is 80%–90%, with incidence of HCV infection ranging from 10% to 20% per year [1]. The Centers for Disease Control and Prevention estimates that, during 1999–2002, 22% of men and 28% of women given the diagnosis of HIV/AIDS had an exposure category of injection drug use [2]. Controlling both HCV and HIV epidemics, therefore, requires developing, testing, and implementing prevention, care, and treatment strategies for both HIV and HCV infection that are effective for persons who inject drugs [3]. IDUs are most in need of primary care that comprises elements of care for both HCV and HIV infection. Elements of care for HCV infection for drug users include screening for at-risk behavior, testing for HCV and HIV, prevention counseling and education, vaccination for hepatitis A and B viruses, and evaluation for comorbidities, including the need for substance abuse services, psychiatric care, social support, evaluation of liver disease, and IFN-based treatment for HCV infection. Primary care for HIV infection, as funded by the Ryan White Comprehensive AIDS Resources Emergency (CARE) Act, is a comprehensive continuum of primary cares services, including clinical care and evaluation, HIV counseling, testing and referral services, oral health care, adherence and nutritional counseling, outpatient mental health and substance abuse services, and referral to specialty and subspecialty care (table 1). Barriers to providing care and treatment for HCV and HIV infection to IDUs stem from characteristics of the diseases and their treatments, patients, providers, and the health care system and can be addressed through the integration of care for both HIV and HCV infection.
Elements of care for hepatitis C virus (HCV) infection and primary care for HIV infection.
Injection Drug Use and Coinfection with HCV and HIV
Co-occurring HIV and HCV infections complicate the medical management of either infection. It is well established that HIV infection modifies the natural history of HCV infection [4]. HIV influences the ability to resolve HCV infection: Clearance of HCV viremia occurs less frequently in coinfected patients, and coinfected patients have higher HCV loads and a 3-fold higher rate of progression of cirrhosis to end-stage liver disease and death [5]. Since the advent of effective combination antiretroviral therapy for HIV infection, liver disease, primarily due to HCV coinfection, has been reported to be the major cause of death in several cohort studies of HIV-infected patients [5].
There are also interactions between the 2 diseases and their treatments. Drug-induced hepatotoxicity has been observed in persons coinfected with HCV and HIV undergoing treatment for HIV, and certain antiretrovirals should be avoided when ribavirin-based therapies are used to treat HCV [5, 6]. Patients coinfected with HCV have a worse prognosis with antiretroviral therapy for HIV, a component of which may be contributed by injection drug use and its complications [7]. Given the myriad of interactions between the infections and their treatments, it is critical to the successful medical management of coinfection with HIV and HCV that coinfected patients be maintained in long-term care that promotes a supportive environment and effective clinical outcomes.
Drug Users and Patient-Provider Relationships
Care and treatment of HCV and HIV infection in IDUs is complex, with numerous barriers to providing high-quality care. There are high prevalences of psychiatric diagnoses, such as major depression, anxiety disorder, and bipolar disorder, with some patients using substances in an attempt to self-medicate an underlying mental illness. Such untreated mental illness can increase risk-taking behaviors. This is further complicated by negative experiences of IDUs with the health care system in general and providers more specifically [8, 9]. A trusting relationship with a member of the health care team who can help patients anticipate, plan for, and endure the difficulties that arise in the medical management of coinfection with HIV and HCV is fundamental for IDUs as they seek care. A patient-provider relationship that will encourage a dialogue in which both parties are able to communicate openly about their expectations and frustrations is critical but may not be supported by the health care system.
The extensive experience gained from treating IDUs for medical conditions, especially HIV infection, has led to principles for engaging IDUs in health care relationships. Successful programs have a respectful approach to substance users, understand the medical and behavioral sequelae of addiction, refrain from moralistic judgments, and use a multidisciplinary team [10]. These strategies embody a client-centered approach. Thus, a care provider works with a client to identify changes that the client is motivated to make. These changes will enhance his or her health and well-being. Even if global behavior change (such as ceasing all drug use) is not possible or likely, many other measures can nevertheless reduce the harmful medical consequences of high-risk behavior. In this setting, health care providers will work with the patient to develop a treatment regimen that fits the lifestyle of the patient (e.g., once-daily therapy) rather than attempting to restructure the patient's lifestyle.
Care for HCV Infection in Drug Users
Because of the need to develop a strong patient-provider relationship and the difficult nature of IFN-based treatment regimens for HCV infection, IDUs tested for HCV infection and found to be HCV seropositive need to be presented with a comprehensive health program that constitutes high-quality care for HCV infection [3]. Medical care for IDUs with hepatitis C can begin with strong linkages to prevention services, including community-based HCV testing and counseling programs based on screening for high-risk behavior, so that drug users with HCV infection can be identified, and their entry into care can be facilitated. Patient-centered education and counseling about prevention of HCV infection, based on behavior risk assessment, should be provided, either on-site or by referral [11], in all public programs and institutions serving IDUs, including public health clinics and hospitals, substance abuse treatment programs, correctional institutions, programs for high-risk youth, sites for HIV counseling and testing, sexually transmitted disease clinics, and mental health clinics and psychiatric hospitals. Regardless of where screening and testing for HCV occurs, additional comprehensive medical and social services need to be provided that address important unmet needs, including treatment for substance abuse, mental health treatment, housing, and other social supports.
Primary Care for HIV Infection in Drug Users
Given that substance abuse is a chronic relapsing disorder with serious adverse consequences to patients with HIV/AIDS, the longitudinal model of care, inherent in primary care, is ideal for caring for this patient population, because primary care addresses other chronic medical conditions [12]. Because substance abuse usually continues after diagnosis of HIV infection, caring for HIV-positive IDUs presents unique challenges. It is well documented that IDUs have less access to antiretroviral medications and, therefore, have experienced significantly less gain in disease-free survival than have other HIV-infected populations since the advent of antiretroviral therapy [13]. A dose-response correlation between the number of days of taking illicit drugs in the last 6 months and use of antiretroviral therapy has been documented [14]. Among IDUs making use of antiretroviral therapy, there is also a clear negative association between current injection drug use and/or alcohol use with adherence to antiretrovirals and HIV suppression [15]. Many clinicians are reluctant to prescribe antiretroviral therapy to IDUs, but many active substance abusers undergoing antiretroviral therapy do maintain undetectable HIV loads.
Many interventions are effective in improving outcomes. Patients who receive support services, whether case management, mental health services, substance abuse treatment, or transportation, are more likely to remain in care. Substance abuse treatment also improves adherence to antiretroviral medications [16], and there are several ongoing studies examining the feasibility of modified directly observed therapy in the context of substance abuse treatment [17]. Care systems are needed to meet the unique set of needs of IDUs.
Integrating Care for HIV And HCV Infection with Treatment for Substance Abuse
Substance abuse is a complex disorder composed of multiple physiological, social, and behavioral problems. It is often interrelated with mental illness; thus, providers need to screen for mental illness. It can be difficult to ascertain whether substance abuse, mental illness, or HIV and HCV infection should be addressed first. However, an initial focus on the medical treatment of substance use is often necessary to create sufficient stability from which other treatments can begin. Full stability can likely be achieved with both mental health services and treatment for substance abuse, subsequently enhancing the medical outcomes of treatment for HIV and HCV infections. Because substance abuse is a complex multifactorial disorder, it is appropriate to treat the “whole person.” Such treatment includes behavioral and social rehabilitative components, as well as biological (pharmacological) components (table 2). Behavioral therapy interventions have been extensively researched and are critical components of the treatment of all drug addictions. Social rehabilitative components are also important and may prove to be suited to certain treatment environments.
Components of a comprehensive treatment plan for a patient's particular substance abuse problems and needs.
Pharmacological treatments, both agonists and antagonists, have been developed and approved by the US Food and Drug Administration (FDA) to treat specific drug addictions. Currently, addiction treatment medications are available for nicotine, alcohol, and opiates. Although none are available for stimulants, such as cocaine, methamphetamine, and 3,4-methylenedioxymethamphetamine (ecstasy), many potential medications are now being developed for these addictions and are expected to be available over the next few years.
An effective treatment strategy for drug abuse and dependence is to match a comprehensive treatment plan to the person's particular substance abuse problems and needs. Desired treatment outcomes are to reduce dependence on drug of abuse, reduce morbidity and mortality associated with drugs of abuse, and maximize the patients' abilities to access services and achieve social integration. This latter outcome is a particularly important step in addressing HCV and HIV in a primary care setting (see Clinical Trials Network, National Institute on Drug Abuse).
Pharmacotherapy for substance abuse is a rapidly evolving field, with both old and new effective treatments for substance use. Therapy with opiate agonists (e.g., methadone or buprenorphine) is the mainstay of pharmacological treatment for opiate dependence and has been shown to diminish and often eliminate opiate use and reduce transmission of many infections, including HIV [18, 19]. Until recently, opioid agonist therapy was limited to federally licensed opioid treatment programs. Understanding the need to increase the number of treatment slots, Congress passed the Drug Addiction Treatment Act (DATA) in 2000, which allows for the use of buprenorphine for treatment of opioid dependence by a properly licensed physician. Any physician licensed by the US Drug Enforcement Agency may apply to receive a waiver (termed the “X number”) to prescribe buprenorphine after an 8-h course of training [20]. Primary care physicians can expand the accessibility of treatment while mitigating the stigma associated with drug use and treatment.
Buprenorphine [21] is a pharmacological agent that differs significantly from full agonists (table 2). Buprenorphine is a partial mu-receptor opiate agonist, and, as such, it has a plateau of its agonist properties at higher doses. This limitation on agonist properties results in an improved safety profile. Specifically, buprenorphine has a favorable “ceiling effect” on respiratory depression. Alternate-day dosing is feasible, because buprenorphine has a high binding affinity for the opiate receptor and slowly dissociates. Buprenorphine has 2 features that decrease the favorability of the drug for street diversion. First, buprenorphine has a higher binding affinity for the mu opiate receptor than does heroin and can precipitate opiate withdrawal when it is taken by an opiate-dependent patient. For this reason, buprenorphine induction must occur in patients already in opiate withdrawal. Second, in the United States, buprenorphine is marketed both alone (Subutex) and in combination with naloxone (Suboxone). In the latter formulation, naloxone is minimally bioavailable via sublingual ingestion. If the tablet is crushed and injected, acute opiate withdrawal is precipitated.
A few case reports from France have noted an elevation in liver function test results (especially alanine aminotransferase levels) after the use of buprenorphine given intravenously. One case report demonstrated an increase in liver function test results after starting treatment with buprenorphine, but this report was limited by the small sample size, retrospective analysis, and short time in which buprenorphine was given [22]. Since 2001, no additional reports of hepatotoxic effects with buprenorphine have been reported, despite the large expansion in the number of patients treated with buprenorphine since the medication was approved by the US FDA in 2002. Although monitoring is required when any medication is added to the other medications of a patient coinfected with HIV and HCV, the presence of HIV or HCV is not a contraindication to the use of buprenorphine.
The high level of liver disease in the population coinfected with HIV and HCV requires that alcohol consumption be addressed. All patients with HCV infection should be counseled to refrain from alcohol consumption [23]. HCV loads have been shown to be elevated in patients with HCV infection who consume alcohol, and elevated HCV loads and alcohol use are associated with a decreased therapeutic response to IFN-based treatment regimens. Alcohol consumption is also associated with poor adherence to medications.
Outpatient pharmacotherapy for alcohol addiction is done with either naltrexone or acamprosate. Acamprosate and naltrexone have different mechanisms of action and modify different behavioral aspects of addiction. Acamprosate, a long-acting compound, prolongs periods of abstinence by normalizing glutamateric neurotransmission that is dysregulated during chronic alcohol consumption and withdrawal. Naltrexone is a fast-acting opioid receptor antagonist that reduces heavy drinking through decreasing the rewarding effects of ethanol. Safety and efficacy of treatment with both drugs for alcohol addiction have been shown in double-blind studies [24].
Cocaine abuse by patients coinfected with HIV and HCV has a negative effect on adherence to treatment. A recent clinical trial [25] has shown buprenorphine to be efficacious in reducing use of both opiates and cocaine by addicted patients. Currently, successful treatment modalities for cocaine addiction rely on lifestyle change through cognitive behavioral counseling.
Challenges and Barriers to Care for HCV and HIV Infection for Drug Users
Barriers to care for HCV infection include patient characteristics, provider-associated factors, the health care system, and the social disorganization that often affects IDUs. Poverty, homelessness, addiction, mental health disorders, social marginalization, fear of prosecution, mistrust of the health care system, and inconsistent follow-through represent challenges to effective care for HCV for IDUs. Nonwhites appear to be more vulnerable to the effects of these barriers, because they are less likely to receive testing for HCV and subspecialty referral, even after drug use is controlled for [25]. Social instability associated with drug use, drug use comorbidities, access to HCV expertise, access to liver biopsy, patient acceptance of liver biopsy, and cost of comprehensive care and treatment also serve as barriers to care. Predictably, socially and culturally marginalized populations are particularly vulnerable to these issues, any combination of which may make treatment of HIV and HCV infection seem formidable. Of these, the significant barriers may be perceptions about the seriousness of HCV disease, access to a psychiatrist, and treatment for substance abuse [26, 27].
Providers constitute another barrier for the provision of care for IDUs coinfected with HCV and HIV because of insufficient training. Consequently, the stigma of drug use in conjunction with unrealistic expectations and judgmental attitudes leads to frustration and resentment for both physician and patient. HCV-infected patients commonly report communication problems with their providers. IDUs may fail to follow their physicians' advice, fail to fully and truthfully disclose their lifestyles and behaviors, and/or fail to keep their appointments. Physicians caring for drug users often experience this behavior as frustrating and may respond with aversion, malice, or neglect. Consequently, most physicians defer to addiction specialists or a drug treatment facility, thus avoiding caring for IDUs. As with other chronic medical conditions, providers need education about substance abuse and injection drug use as a disease. The concept that substance abuse is a moral failing requiring condemnation is inappropriate given our present understanding of substance abuse.
Selected Models for Integration of Care for Patients Coinfected with HIV and HCV
Patient-centered care is essential for programs to successfully provide treatment for HIV and HCV, and such an approach follows a multidisciplinary model to provide integrated services rather than using the traditional referral services from the HIV primary care site to an HCV subspecialist.
The HIV/HCV colocated clinics. An HIV/HCV clinic was established at the CARE-funded clinic at Brown University School of Medicine [28]. The clinic serves ∼1000 HIV-seropositive patients, 43% of whom are coinfected with HCV. HCV Coinfection Clinic is held 2 times per month in the same office in which patients receive HIV primary care and gynecologic services. The clinic is staffed by a physician expert in care of HIV who also treats HCV, a consulting hepatologist, a coinfection nurse, and a clinic coordinator. A collaborating community-based mental health agency provides coordinated psychiatric care, counseling, addiction treatment and referral, and intensive home-based case management. The goals of HCV Coinfection Clinic are to provide patient education about HCV, medical evaluation, treatment with pegylated IFN plus ribavirin, evaluation and treatment of drug dependence, and evaluation and treatment of psychiatric disease, as well to conduct clinical research on HIV and HCV infection as medical complications of injection drug use. The advantage of this approach is that patients are already familiar with the clinic location, staff, and policies. Colocation and a single record allow for close coordination and communication between the patient's HIV specialist and the provider of care for HCV infection.
Integrating care for HCV infection into primary care for HIV infection. In the fully integrated clinic model, the HIV specialty clinicians treat HCV infection in their patients rather than referring within the clinic to other specialists. The HIV Alameda County (California) Coordinated Early Services System has established such a program [29]. Critical elements of the program include education of HIV clinicians regarding HCV and its treatment; ongoing consultation and support for an expert in HCV, in this case a gastroenterologist; assignment of a full-time registered nurse for one-on-one patient counseling, monitoring of adverse effects, and support of patients undergoing treatment for HCV infection; and establishment of a weekly peer support and education group for the coinfected patients. In addition, the program facilitates obtaining liver biopsy by providing the service in the clinic's infusion room. Education of patients through the one-on-one nursing and the support group has been critical in assisting patients in making decisions to initiate treatment. This approach has the advantage over colocated clinics in that patients already have a trusting relationship with their HIV care provider, which facilitates their decisions about beginning treatment for HCV infection. However, HIV specialists need to be trained and remain current on treatment for HCV infection.
Substance abuse treatment and integrated care: treatment programs for opioid addiction. Methadone treatment programs provide a comprehensive therapeutic milieu, often including primary medical care, psychosocial counseling, vocational rehabilitation, ongoing performance monitoring, and other vital services. One such program integrates general and HIV-related medical, substance abuse, and mental health services at a single site [30]. The staffing pattern at this site, serving ∼400 patients, includes a full-time physician (internist or family practitioner), a full-time mid-level provider (physician assistant or nurse practitioner), part-time psychiatrist, a social worker, nursing staff, and substance abuse treatment counselors. Weekly interdisciplinary meetings foster communication between staff regarding diverse aspects of patients' care. Subspecialty care, advanced diagnostics, and acute care are provided through a linkage with a nearby tertiary-care system (Montefiore Medical Center, New York, NY). Physicians at methadone treatment sites serve as patients' inpatient attending physicians if the patients are hospitalized for medical care, thereby providing continuity of care. Colocation of care services for HCV and HIV in the substance abuse treatment setting fosters access to care for a high concentration of coinfected patients, many of whom likely would not have access to needed care.
These are 3 examples of integrated approaches to the treatment of patients coinfected with HIV and HCV. To improve outcomes among patients, more programs will need to adopt such integrated models as the standard of care.
Acknowledgments
Potential conflicts of interest. All authors: no conflicts.






Comments