Abstract
Keloid formation is a wound healing response, which fails to resolve and leads to formation of a raised collagen mass extending beyond the original wound margins. Keloids are typically excluded from palms and soles. Therefore we compared keloid and palmar fibroblasts in vitro using fibroblasts from nonaffected individuals as controls. Collagen I, α-smooth muscle actin and thrombospondin-1 were found at higher levels in keloid than in palmar fibroblasts. These differences were ameliorated by addition of TGFβ1. The potential for resolution of the wound healing response was estimated analyzing apoptosis during serum starvation. Annexin V and TUNEL assays showed that palmar fibroblasts underwent faster apoptosis, than did the keloid fibroblasts, and started detaching. Addition of TGFβ1 counteracted this effect. The weak expression of the myofibroblast phenotype and the advanced apoptosis of palmar fibroblasts suggest mechanisms for the exclusion of keloids from palmar sites.
Similar content being viewed by others
Introduction
Keloids occur due to deviations from the normal wound healing process. The defect is found predominantly in individuals of African origin (about 10% incidence in the African-American population) and is excluded from the glabrous tissue of palmar and plantar surfaces. A raised scar forms, which extends beyond the boundaries of the original wound. It contains thick and highly crosslinked collagen bundles and excessive proteoglycan and fibronectin (for recent reviews see1,2,3).
Although there have been many in vitro and in vivo studies on keloids, it is still not known what causes their formation. The particular protein expression pattern in keloids may be related to a specific cytokine environment. Higher (IFN-β, TNF-α, IL-6) and lower (IFN-γ, IFN-α, IL-2, TNF-β) levels were found in the peripheral blood mononuclear-cells (PMNC) of black keloid formers.4 In vitro keloid fibroblasts demonstrate a variety of differences in behaviour compared to normal fibroblasts. Some, but not all cultures of keloid fibroblasts, show higher levels of collagen I than do normal fibroblasts.5,6,7,8,9 In addition, TGFβ1, which is known to enhance matrix production, has been reported to have differential effects on proliferation rates and collagen synthesis of keloid vs normal fibroblasts.10,11,12 TGFβ1 mRNA was detected in fibroblasts and endothelial cells within the expanding borders of the active keloid,7 implicating TGFβ1 in the development of this scar. Decorin, a natural inhibitor of TGFβ,13 was found unaltered in the keloid tissue.14,15
The progression through the different stages of normal wound healing leads to granulation tissue formation and fibroblast differentiation into myofibroblasts. In normal wounds the myofibroblast marker, α-smooth muscle actin (α-SMA), peaks between 7–15 days, when 70% of the wound fibroblasts have the myofibroblast phenotype.16 In vitro, a negative dependence of the myofibroblast phenotype on the plating density has been documented.17 On the other hand, TGβ1 has a strong positive effect on the expression of α-SMA.18 α2β1 integrins are necessary for the TGFβ1 induction of α-SMA.19,20 The presence of the EDA splicing variant of fibronectin21,22,23 and the intracellular tension response to the deformability of the extracellular matrix (ECM)19,20 also appear to be crucial for the TGFβ1 effect on the myofibroblast phenotype.
As wounds close there is a decrease in cellularity due to apoptosis. This ensures the transition between granulation tissue and scar. The myofibroblasts gradually disappear and by day 30 the fibroblast population is indistinguishable from that found in normal dermis.16,24,25 Myofibroblasts can undergo apoptosis. This is seen in Dupuytren fibromatosis, where it coincides with an elevated expression of TGFβ1.26,27,28 However, recent findings in a model of regressing granulation tissue have suggested that differentiation into myofibroblasts might not be a prerequisite for apoptosis.29
Keloids, when studied immunohistochemically show α-SMA only around microvessels. In contrast, cultured keloid fibroblasts have detectable levels of α-SMA.30 When plated on collagen-coated plates or embedded in collagen gels normal and keloid fibroblasts down-regulate their α-SMA synthesis, while upregulating their α2β1 integrins.31
When apoptosis was studied in keloids, the number of apoptotic cells were found to either decrease distally from the keloid lesion edges32 or to decrease near them.33 The delayed apoptosis has been ascribed to the presence of somatic mutations in both p53 alleles of cells within the center of the keloid.34 Irrespective of these conflicting reports on the location of apoptotic cells, delayed apoptosis in keloid fibroblasts could be responsible for the production of vast amounts of ECM prior to the eventual disappearance of the cells, leaving only the acellular collagenous scar.
In an effort to determine the mechanisms whereby keloids form and keloid prone individuals are spared keloid formation on glabrous tissues, an in vitro assessment was carried out. Comparisons were made among fibroblasts isolated from palmar surfaces, from nonpalmar sites and from keloids. Matrix production, myofibroblast expression and apoptosis were monitored in the absence and presence of exogenously supplied TGFβ1. Under a variety of experimental conditions palmar fibroblasts demonstrated a weaker myofibroblast phenotype and higher growth factor requirements.
Results
Differences in the phenotype between palmar and nonpalmar fibroblasts were evaluated using cells isolated from keloid and nonaffected donors. Palmar fibroblasts were smaller and reached confluence 1–2 days earlier than their nonpalmar or keloid counterparts (data not shown). In order to reveal differences between cultures from different sources, cells were maintained with or without serum for 3 days after reaching confluence. Ascorbic acid was present during these 3 days to ensure collagen I secretion.
Collagen I, α-SMA and TSP-1 are upregulated in keloid cultures
The cellular distribution and organization of collagen I, α-SMA, and the TGFβ1-activator thrombospondin-1 (TSP-1) shown in Figure 1, were analyzed in fibroblasts plated on chamber slides at 5 cells/mm2. Keloid fibroblast (K) cultures accumulated the most collagen I (Figure 1a). It was found to be organized into thicker fibers than the rest of the cultures (Nnp, nonpalmar fibroblasts from a nonaffected donor; Pk, palmar fibroblasts from a keloid patient; Pn, palmar fibroblasts from a nonaffected donor) (Figure 1b,e,f). The abundance and thickness of the collagen fibers were not significantly changed when K were cultured in serum-free medium for 72 h (Figure 1c). However, there was some reduction in the collagen content in Nnp (Figure 1d) and much greater reductions in the collagen content in palmar fibroblasts (P) (Figure 1g,h). In the serum-free Pk and Pn cultures all remaining collagen appeared to be intracellular, little or no extracellular collagen was detected.
Collagen I, Thrombospondin-1 and α-smooth muscle actin in fibroblasts from different origin. Fibroblasts derived from a keloid (K) (a, c, i, k, q, s), from the corresponding palm (Pk) (e, g, m, o, u, v), from a nonpalmar site of a nonaffected donor (Nnp) (b, d, j, l, r, t) and from the palm of a nonaffected donor (Pn) (f, h, n, p, v, x) were grown on chamber slides. After confluence the cultures were incubated for an additional 3 days in serum-containing medium (a, b, e, f, i, j, m, n, q, r, u, v) or in serum-free medium (c, d, g, h, k, l, o, p, s, t, w, x). Antibodies against collagen I (a–h), thrombospondin-1 (i–p) and α-smooth muscle actin (q–x) were used and visualized by indirect immunofluorescence the level and organization of the corresponding proteins in the cells. The photographs were taken with an automatic exposure-time adjustment enabling weak fluorescence to show up at the expense of higher background. Note the predominance in K of fluorescence from these three markers in either medium condition
Similar to the results with collagen I, K cultures contained the most TSP-1 (Figure 1i). As TSP-1 colocalized with collagen (data not shown), it was also found in thick fibers. Little difference in abundance was observed in the serum-starved K cultures (Figure 1k). This contrasted with the non-K. In the serum-containing media there were lower levels of extracellular TSP-1 (thin and lower intensity fibers) (Figure 1j,m,n) and in the serum-starved cultures extracellular TSP-1 was no longer detectable (Figure 1l,o,p).
α-SMA was found in the greatest abundance and in stress fibers in K incubated in presence (Figure 1q) or absence (Figure 1s) of serum. This actin was also detected in the non-K cultures, but to a lesser extent (Figure 1r,u,v), being especially low in Pk (Figure 1u). Barely detectable levels were seen in the serum-starved cultures of the non-K strains (Figure 1t,w,x).
α-SMA levels have been reported to depend on the plating density.17 Therefore, FACS analyses were used (Figure 2) to compare the distribution of α-SMA fluorescence among individual fibroblasts in serum-starved cultures when seeded at a low plating density (lpd) of 5 cells/mm2 and at an intermediate density of 50 cells/mm2. As shown in Figure 2 at both plating densities the highest intensities were detected in K cultures, compared to P cultures (Pk and Pn). Nnp had intermediate levels.
FACS analysis of α-smooth muscle actin in fibroblasts. Fibroblasts from keloid patients (e.g. Keloid H), from corresponding palm biopsies (e.g. Palm H) and from nonaffected donors (e.g. Nonpalm w, palm c) were plated either at intermediate 50 cells/mm2 (—-), or at a low density (lpd) 5 cells/mm2 (- - - -). After reaching confluence, they were grown for 3 days in medium without serum. Cultures were then harvested by trypsinization. For FACS, the cells were fixed with Histochoice, permeabilized in 0.3% Triton in PBS and immunolabelled with anti-α-SMA antibody and PE-conjugated secondary antibody. Examples of FACS scans are presented. The average of all experiments is plotted below the scans. The geometrical mean fluorescence of the cells with α-SMA intensities above the background (fluorescence≈percnt;10) was used as a characteristic of the distribution
Protein expression in fibroblasts from keloid formers and nonaffected individuals
Protein extracts from equal numbers of cells of twelve cell cultures (four K, four Pk, two Pk and two Pn) plated at 50 cells/mm2, were analyzed by immunoblotting using antibodies specific to a larger set of proteins known to be modulated during wound healing and apoptosis (Figure 3A–F). Two of these markers, collagen and α-SMA, showed consistent differences between K and to a lesser extent between Nnp and P (Figure 3G). After 72 h of serum-starvation P showed little accumulation of collagen I and α-SMA (Figure 3G). K had consistently higher collagen I levels and variably higher α-SMA levels, perhaps reflecting strain-dependent differences.35,36 Pk grown in serum containing medium, showed similar lower levels of α-SMA and collagen I compared to the other fibroblast cultures (not shown).
Western blot analysis of fibroblasts grown to confluence in serum and then subjected to serum starvation for 3 days. Cell extracts from equal number of keloid fibroblasts (KD, KH, KL, KT), from corresponding palmar fibroblasts (PD, PH, PL, PT), and from controls: Nnp (Nd, Caucasian, Nw, African-American) and Pn (Pc, latin, Pl, African-American)–were resolved on 4–12% SDS-polyacrylamide gels, electroblotted and indirectly immunolabeled using corresponding antibodies and chemiluminescence for detection -A/-F/. Averaged results from a densitometry scan of the Western blots (A–F) for all K, Pk, Nnp and Pn G/. The bars are standard deviations. When keloid fibroblasts were compared with palmar fibroblasts consistent differences (t-test was used) were found for the following markers: fibronectin {P=0.2 for K vs Pk}, collagen {P=0.015 (K vs P) and P=0.035 (K vs Pk)}, and α-SMA {P=0.034 (K vs P) and P=0.1 (K vs Pk)}, but not for integrin, vimentin, p53 and BAX proteins
Less pronounced changes were the 10–50% higher levels of fibronectin (t-test; P=0.2) and vimentin (P=0.38) in K vs Pk cultures. When the general actin antibody was used no significant difference was seen between P and non-P. The levels of integrin β1 and Bax showed no consistent variation among the cultures from different sources. However, we were able to detect more p53 in two out of four Pk (Palm D, Palm H in Figure 3D) compared to their paired K.
When normalization of the immunoblot results was done per protein (e.g. actin) the results of higher collagen I and higher α-SMA in K remained valid. The fibronectin levels became similar amongst cultures and three out of four Pk showed higher p53 than did K. The fourth donor had barely detectable levels of p53 in either K or Pk (data not shown).
As shown in Figure 4, the addition of TGFβ1 to the serum-starved confluent cultures blunted the differences in collagen I and α-SMA content between K and non-K fibroblasts. All cultures (palmar and nonpalmar) showed upregulation of collagen I (Figure 4A) and α-SMA (Figure 4C), when TGFβ1 was present in the media (lanes 2, 4, 6, 8). At the same time little effect was seen on the vimentin levels. Similar conclusions were drawn from immunohistochemical analyses (not shown).
Alpha smooth muscle actin (α-SMA) and type I collagen are upregulated by addition of TGFβ1 to serum starved palmar and keloid fibroblasts. Fibroblasts were grown from keloids (KD, KH) or from palmar biopsies of the corresponding patients (PD, PH). After confluence had been reached, the cultures were serum starved for 3 days either without or with active TGFβ1. Cell extracts were resolved as in Figure 3, electroblotted and indirectly immunolabeled with corresponding antibodies. Nw, nonpalmar fibroblasts from a nonaffected donor were included. + + indicates the procollagen type I bands; * * indicates the mature (processed) collagen I (α1 and α2) bands. Vimentin was used as a reference. At this film exposure the collagen I bands were not apparent for fibroblasts without TGFβ1
Apoptosis in serum starved keloid fibroblasts is low
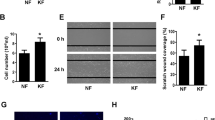
After 72 h of serum withdrawal there was a striking difference between cultures. Those of Pk (Figure 5c) and Pn (data not shown) contained many loosely bound and detaching round vesicles (cells). Few were found in K (Figure 5a) and Nnp (data not shown). The addition of TGFβ1 alleviated this effect of serum withdrawal (Figure 5d). As lactate dehydrogenase (LDH) activity was not detected in the media of any cultures, there was not a significant degree of lysis during starvation (not shown). Pk and Pn maintained in a serum-containing medium did not demonstrate detaching cells (not shown).
Detachment of palmar fibroblasts during serum starvation. After reaching confluence fibroblasts were starved for 3 days. The palmar cultures (Pk)–(c)–contained many vesicles (cells) released into the media or loosely bound to the confluent layer. The keloid fibroblasts (K) from the same patient–(a)–were larger and only a few round cells could be seen floating. When TGFβ1 was present during serum starvation the number of floating cells in the palmar cultures was greatly reduced (d). TGFβ1 had little effect on K (b)
The TUNEL assay for DNA fragmentation was used to ascertain whether the appearance of the palmar cultures following serum withdrawal reflected an enhanced apoptosis. As shown in Figure 6, nuclei were differently stained, with the darkest color (an indication of advanced apoptosis) within the picnotic nuclei (Figure 6). These appear to correspond to cells in the process of detachment (Figure 5). Normally shaped TUNEL-positive cells correspond to a preapoptotic stage.37,38
Slower apoptosis in keloid fibroblasts during serum starvation. The TUNEL assay (In situ cell death detection kit, Boehringer, Mannheim) was used to compare the apoptosis in: (a, b) keloid fibroblasts (K); (c, d) nonpalmar fibroblasts from a nonaffected donor (Nnp); (e, f) palmar fibroblasts of the same keloid patient (Pk); g, h) palmar fibroblasts from a nonaffected donor (Pn). After reaching confluence they were grown either without (a, e, c, g) or with (b, f, d, h) TGFβ1 in medium without serum for 3 days. Arrowheads ‘>’ mark the dark picnotic nuclei
The larger keloid fibroblasts had a regular shape, weak coloration and few picnotic nuclei (Figure 6a). This was not influenced by TGFβ1 (Figure 6b). Both Pk and Pn had fuzzy nuclear membranes and many picnotic nuclei (Figure 6e,g). The addition of TGFβ1 caused improvements in nuclear definition and a decrease in the number of dark picnotic nuclei (Figure 6f,h). Pk had a pronounced granular intranuclear structure (Figure 6f), which was not present in K (Figure 6b). The Nnp nuclei had more staining than did K nuclei (compare Figure 6a and c). Some of the heavily stained cells appeared shrunken and smaller in size than the rest. TGFβ1 showed an effect on Nnp (Figure 6d). Cells were bigger but still stained more than K (Figure 6b). In the presence of serum the preapoptotic state of K and non-K fibroblasts seemed comparable (not shown).
Analysis of TUNEL-stained fibroblasts by FACS revealed distinct differences between K, Nnp and P (Figure 7a). In these experiments, the level of apoptosis was measured by the cell count at corresponding fluorescence intensities. The lowest level of apoptosis was seen in K fibroblasts (e.g. Keloid T) while intermediate (e.g. Nonpalm w) and high levels (e.g. Palm T, Palm l) were found in the rest of the cultures.
Apoptosis in fibroblasts during serum starvation. Typical FACS scans of keloid fibroblasts: Keloid T; corresponding palmar fibroblasts: Palm T; from nonaffected palmar fibroblasts: Palm l, Palm c; from normal nonpalmar fibroblasts: Nonpalm w. The cells were grown to confluence and serum starved for 3 days before harvesting. Bars, standard deviations. (a) FACS–TUNEL assay. Cells were acetone-fixed after harvesting and fluorescein-dUTP was incorporated at DNA strand breaks. Shown is a plot of the percentage of dUTP-fluorescein positive cells (M2) with fluorescence intensities above 102 and the geometrical mean (Geo Mean) of the distribution of such cells, averaged over all the data for culture of the same type. For every pair (keloid vs corresponding palmar fibroblasts) both parameters differed considerably. The overall difference between K and non-K cultures was also significant (t-test; P<0.25). (b) FACS Annexin V/Propidium Iodide assay. The assay was performed according to the Manufacturer's (Clontech) protocol.54FL1, Annexin V-FITC fluorescence, increases with apoptosis; FL2, PI-fluorescence, increases with necrosis. Fluorescence scans: lower left quadrant (LL), live cells (low apoptosis and necrosis; upper left (UL), necrotic cells only; lower right (LR), early apoptosis (pre-apoptotic) cells; upper right (UR), cells in late apoptotic state. A plot is given of the percentage of cells from the corresponding apoptotic stages. Early apoptosis is substantially delayed in K vs Pk (t-test: P=0.006), and in K vs Nnp (P=0.034). Late apoptosis percentage is lower in K vs Pk, although the variation is higher (P=0.25)
When membrane alteration and integrity were evaluated by Annexin V binding and Propidium iodide (PI) uptake (Figure 7b), results were similar to those obtained by TUNEL. K and Nnp had the most live cells; 91±2% of the cells showed low levels of both FITC-Annexin V- and PI-fluorescence. This is significantly different from P, which contained 79±9% live cells (t-test: P=0.075). Pk showed higher early and late apoptosis levels than K. Pn and Nnp were in intermediate states. Pn had the highest amount of necrotic cells. [The terminology and definition for apoptosis and necrosis are as previously described.]39 It is possible that the Pk had already lost necrotic cells by detachment into the media (cf. Figure 5c).
Discussion
Keloid fibroblasts differ in phenotype from palmar fibroblasts
Individuals prone to keloid formation are spared aberrant wound healing on their palmar and plantar surfaces, suggesting either that the resident fibroblasts differ in phenotype or in microenvironment. Fibroblasts grown on plastic in submerged culture are under conditions resembling a fresh wound, thus revealing features that may not be detectable in an already formed keloid. The experiments that are presented herein revealed intrinsic differences in the phenotypes of Pn/Pk and K fibroblasts. The Nnp showed characteristics intermediate between Pk/Pn and K. The differences between palmar and nonpalmar fibroblasts may serve as clues about the development of keloids and about the reason for their exclusion from glabrous tissue.
Fibroblasts from keloids accumulated the most α-SMA, collagen I and TSP-1 under all culture conditions (Figures 1,2,3). Their α-SMA stress-fibers were more prominent–thicker and abundant. There were also thicker collagen I and TSP-1 positive fibers in the keloid cultures (Figure 1a,c,i,k). This correlates with reports demonstrating a higher lysyl oxidase (the enzyme catalyzing collagen crosslinking) expression in myofibroblasts.40
The differences between K and non-K were more pronounced when cells were deprived of serum for 3 days. The keloid cultures were the least influenced by the serum withdrawal (Figure 1c vs g; k vs o; s vs w, etc). Palmar fibroblasts, especially Pk, had low levels of α-SMA, collagen and TSP-1 (Figures 1,2,3). The predominance of the myofibroblast phenotype (i.e. expression of α-SMA) in the K cultures remained even when we took into account the effect of plating density17 (Figure 2). This suggests that this phenotype is an intrinsic feature of keloid fibroblasts.
However, addition of TGFβ1 during serum starvation blunted the differences between fibroblast cultures by causing an increase in the expression of α-SMA, collagen I (Figure 4) and TSP-1 (not shown) in all cultures. This cytokine has previously been demonstrated in vivo and in vitro to determine the expression of collagen I7,9,41 and α-SMA.42
The transient appearance of myofibroblasts in a healing wound is a prerequisite for proper wound healing and correlates with TGFβ1 activity.43 Although the amount of TGFβ1 present in the conditioned media of normal skin fibroblasts was found equal to that in keloid fibroblasts embedded in a fibrin maxtrix gel,44 our data (Figure 4) suggest that requirements for and levels of TGFβ1 might still determine the difference between palmar and nonpalmar fibroblasts (see ‘Note added in proof’ at the end). In addition, TGFβ1 activity may be greater in keloids as K expressed higher levels of the TGFβ1-activator TSP-1 (Figure 1i, k vs j, l–p).45 Alternatively, in keloid formers, the higher level of TNFα and lower level of γ-interferon, secreted by activated PMNs at the growing margins of the keloids,4 may also lead to increased collagen I and α-SMA expression.42 These cytokine differences may be sufficient to explain the occurrence of keloids.
Delay of apoptosis in keloid cultures
The effect of serum withdrawal on confluent fibroblasts in submerged culture demonstrated yet another aspect of palmar fibroblast behavior. Their behavior correlated with previous reports of confluence and starvation as factors that may lead to apoptosis.46,47,48,49 In contrast to Nnp and K, the serum starved Pk and Pn became increasingly dysadherent (Figure 5)–a landmark of late stage apoptosis.47 Using TUNEL (Figure 6) and Annexin V (Figure 7) apoptosis assays to further specify the apoptotic stage, it was found that K were delayed in apoptosis compared to Pk, Pn, and Nnp, especially Pk from the corresponding keloid patients (Figures 5,6,7). This correlated with the predominance of myofibroblast stress-fibers in K cultures (Figures 1,2,3) and is consistent with the observed reduction of myofibroblast markers in wounds prior to apoptosis16 and with other reports33 showing delayed apoptosis in subconfluent keloid fibroblasts. Although there have been reports of p53 in keloids (in vivo and in vitro),33 our immunoblots (Figure 3D,G) showed higher levels of p53 in non-keloid cultures. In the two cases (Palm D and Palm H, Figure 3D) this correlated with a higher apoptosis (actual FACS scans not shown).
Similar to our results, a negative correlation between α-SMA levels and apoptosis has been found by treatment of fibroblasts with IL-1β. This cytokine causes induction of apoptosis mainly in fibroblasts with higher α-SMA expression.50 Other data51 have shown that the basic fibroblast growth factor (bFGF) leads to decrease in α-SMA and induction of apoptosis.
Using model systems for different stages of wound healing it has been found that a stressed ECM delays apoptosis.29,52,53 At nonpalmar, keloid-prone sites, continued expression of α-SMA and collagen I could generate such a stressed ECM. The delay in keloid fibroblast apoptosis as demonstrated in our experiments (Figures 5,6,7) would give time for excess fibroblast proliferation and further ECM synthesis. After this one might imagine fibroblasts being discarded by apoptosis leaving a large acellular collagenous mass. Not surprisingly, at the time biopsies are typically taken, the keloid has usually been formed for more than several weeks and we should not expect to detect any α-SMA30 (and data not shown). Although it may not be the myofibroblasts that undergo apoptosis in normal wound healing,29 a pronounced myofibroblast phenotype may lead to a delay in apoptosis, as the one observed in our experiments.
In summary, in the absence of TGFβ1, we found a stronger myofibroblast phenotype and lower apoptosis level in K compared to Pk, Pn and Nnp. Differences between Nnp and Pk, Pn were also observed especially in response to serum withdrawal. Thus the absence of keloids from the palmar surface of keloid formers may be due to particular exogenous/endogenous TGFβ1 availability and specific palmar fibroblast requirements for higher TGFβ1 levels to promote growth and protection against apoptosis. As TGFβ1 levels are transient, collagen and α-SMA production could be down-regulated at palmar sites where a quicker resolution of fibrosis by apoptosis might occur. Further in vivo and in vitro studies on the levels of vitamins, cytokines and other growth factors, as well as their receptors, in keloids and nonkeloid (P, Nnp) tissues will be necessary to advance our knowledge of the etiology of keloids and provide clues for improved therapies.
Materials and Methods
Keloid patients
Fibroblasts were isolated from biopsies of keloids and palms of four keloid patients. In three keloid cases (marked KD, KH, KL) fibroblasts were grown from keloid subjacent to the epidermis, and in one keloid case (KT) fibroblasts were grown from the keloid deeper in the dermis. In both cases the biopsies were taken away from the lesion boundaries in order to avoid mixing of fibroblast populations from the keloid and the adjacent tissue. As control, fibroblasts were isolated from biopsies of the nonpalmar regions of two nonaffected individuals (African-American and Caucasian) and from the palms of two other nonaffected individuals (African-American and Hispanic). For experimentation cells were used between the second and fifth passage. No consistent differences were found with passage.
Cell cultures
Cells were plated either at 105 cells per p100 plate (50 cells/mm2) or 104 cells per p100 (5 cells/mm2, low plating density (lpd)). Cultures were grown to confluence at 37°C and 7.5% CO2 in low glucose DMEM (Gibco, BRL) supplemented with 10% fetal bovine serum (HyClone), 100 units/ml penicillin and streptomycin. The serum-starved samples were grown in the same medium without serum for 72 h. (The 10% serum-containing medium has 14 μg/ml ascorbic acid and less than 0.5 ng/ml TGFβ). At confluence L-ascorbic acid-sodium salt (Sigma) was added to 50 μg/ml. When indicated the medium was supplemented with recombinant TFGβ1 (R&D Systems) to 5 ng/ml. For protein analysis the cells were harvested in phosphate-buffered saline (PBS) by scraping with a Teflon scraper. Aliquots were taken for measurements of protein and DNA. The cocktail of proteinase inhibitors included 1 mM EDTA, 5 mM benzimide, 5 ng/μl leupeptin, 1 μg/ml pepstatin, 0.5 μg/ml aprotinin and 0.1 mM PMSF.
Protein electrophoresis
1.5 mm Precast NOVEX (San Diego, CA) gradient 4–12% Tris-Glycine polyacrylamide SDS gels were used according to the conditions specified by the manufacturer. Samples were sonicated, appropriate volumes of 10× sample buffer (0.6 M Tris-HCL, pH 6.8, 1.4(v/v) β-mercaptoethanol, 0.1% bromphenol-blue, 50%(w/v) SDS) were added and the samples were heated to 95°C for 5 min before loading. Equal numbers of cells, according to nucleic acid content were loaded (approximately 2–4 μg nucleic acids per lane). SeeBlue™ prestained protein molecular weight standards (NOVEX) were used together with 2 μg of rat-tail collagen type I (Upstate Biotechnology, NY, USA) as markers.
Nucleic acid and protein concentration
Protein contents were determined using the Bradford reagent with BSA as standard. Nucleic acid contents were estimated by measuring the absorption at 260 nm.
Primary antibodies
Primary antibodies were as set out in Table 1.
Secondary antibodies
Anti-[mouse/rabbit IgG (H+L)]-peroxidase conjugates (Boehringer, Mannheim) were used for the Western blots at 1 : 2500–5000. R-Phycoerythrin (PE) conjugated anti-mouse IgG (whole molecule) (Sigma) were used at 1 : 100; affinity purified fluorescein (FITC)-conjugated goat anti-mouse IgG (H+L) (Jackson Immunoresearch Labs) and anti-rabbit F9(ab’)2 (G+L) IgG (TAGO, Burlingame, CA, USA) were diluted 1 : 100 prior to application.
Immunohistochemistry
Acetone-fixed cells on chamber slides were treated with universal blocking solution Power Block (Biogenex) or FBS 10% in PBS for 10 min. Primary antibodies were used at dilutions specified above. Incubations with secondary FITC- or PE-conjugated mouse/rabbit IgGs were for 60 min at room temperature. After washes with PBS the chamber slides were mounted with Vectashield plus DAPI (Vector Laboratories, Burlingame, CA, USA), visualized and photographed using a Nikon Optiphot microscope with automatic exposure adjustment at 50× magnification on Kodak Gold Max 800 film.
Western blotting
Gels were electroblotted at 4 V DC overnight in a Semiphor apparatus TE70 (Hoefer/Pharmacia). The blots were blocked in 5% nonfat dry milk, 1% BSA in PBS with 0.05% Tween (PBS/Tween). Primary antibodies were diluted in 5% nonfat milk-PBS and blots were incubated for 1 h at room temperature or overnight at 4°C. After three PBS/Tween washes, the blots were incubated with peroxidase-conjugated secondary antibody (diluted in PBS/Tween with 5% nonfat milk) for 30 min to 1 h. Detection was with the SuperSignal CL-HRP Substrate System (Pierce) for 5 min followed by exposure on X-ray film for seconds to minutes. Scanning of the X-ray films was performed using ScanMaker Et (Mikrotek) and Adobe Photoshop 4.0 software. Densitometry was carried out with the automatic digitizing system Un-SCAN-IT gel version 4.1 for Windows (Silk Sci. Corp., 1996) and Microsoft Excel 97 SR-1. To reprobe blots, antibodies were removed with a 30 min incubation at 60°C in 2% SDS, 62.5 mM Tris-HCL, pH 7, 100 mM β-mercaptoethanol. Blots were then blocked for 15 min.
Apoptosis (chamber slides)
Cells grown on chamber slides were acetone fixed and microwave pretreated for 5 min. This approach proved to be very efficient in revealing most cells in a preapoptotic or apoptotic state.38 After fixation the In Situ Cell Death Detection Kit, POD (Boehringer, Mannheim) was used according to the manufacturer's protocol, with peroxidase as the detecting reagent. The antibody conjugate was diluted 1 : 2. The enzyme was omitted in the negative controls.
FACS analysis
Cells were harvested by incubation with trypsin (0.05%) and EDTA (0.02%). About 1×106 cells were used per sample. When needed cells were fixed for 5 min with ice-cold acetone at −20°C, and washed twice in PBS afterwards. Alternatively, fixation was performed using a 20 min incubation in HistoChoice (Amresco, Solon, Ohio) at room temperature, followed by a 5 min permeabilization on ice in 0.3% Triton in PBS with two subsequent washes in PBS. The samples were filtered through 35 μm cell strainer caps of Falcon polystryrene tubes before being applied to the FACS machine.
α-Smooth muscle actin analyses
The cells were resuspended in 100 μl PBS and incubated for 1 h at room temperature with the 1 : 100 diluted antibody. After two PBS washes, the secondary antibody (FITC conjugated mouse IgG, or, alternatively PE conjugated mouse IgG) was applied for 1 h at room temperature and later removed by PBS washes. Control cells for each fibroblast culture, incubated only with the secondary antibody were used to define the background.
TUNEL assay (Boehringer, In Situ Cell Death detection Kit, Fluorescein)
The samples were resuspended in 50 μl TUNEL reaction mix and incubated for 1 h at 37°C with agitation. A control sample incubated without the enzyme was prepared for each fibroblast culture. A PBS wash was performed at the end of the reaction.
Annexin V-FITC/Propidium Iodide (PI) analyses
The ApoAlert Annexin V Apoptosis kit (Clontech) was used according to the manufacturer's procedure.54 Cells incubated only in the binding buffer (without Annexin V and Propidium iodide) served as control for each fibroblast culture. After 15 min of dark incubation the samples were analyzed by FACS. Cells with high Annexin V-FITC fluorescence (FL1) and low PI-fluorescence (FL2) (Figure 7b, lower right quadrant of the histogram) are considered in early apoptosis (or preapoptotic); the ones with high FL2 and low FL1 (Figure 7b, upper left quadrant) as necrotic (the PI is able to enter the nuclei), the ones with high FL1 and FL2 (Figure 7b, upper right quadrant) as late apoptotic (kit's manual). The position of the lines defining these four regions is determined using control cells incubated without Annexin V and PI.
Flow cytometry
Flow cytometry was performed on a Becton Dickinson FACScan with CellQuest software Version 3.2.
Light microscopy
An Olympus VANOX-T microscope with an LBT filter model AHBT on 160T Kodak slide film was used together with an inverted microscope Carl Zeiss IM 35.
Statistical analysis
The effects reported were found in at least three independent experiments with several keloid patient cultures, as well as with cultures of cells from several non-affected individuals. The Student t-test was used for comparison of the means.
Abbreviations
- ECM:
-
extracellular matrix
- FACS:
-
fluorescence aided cell sorting
- K:
-
keloid fibroblasts
- lpd:
-
low plating density
- Nnp:
-
nonaffected nonpalmar fibroblasts
- P:
-
palmar fibroblasts
- P :
-
the probability that you are incorrect in stating that the two means are different according to Student's t-test
- PBS:
-
phosphate buffered saline
- PI:
-
propidium iodide
- Pk:
-
palmar fibroblasts from a keloid patient
- Pn:
-
palmar fibroblasts from a nonaffected individual
- TSP-1:
-
thrombospondin-1
- TUNEL:
-
terminal deoxynucleotidyl transferase (TdT)-mediated dUTP nick end-labeling
References
Berman B and Bieley HC . (1995) Keloids. J. Am. Acad. Derm. 33: 117–123
Tredget EE, Nedelec B, Scott PG and Ghahary A . (1997) Hypertrophic scars, keloids and contractures. Surg. Clin. North Am. 77: 701–730
Tuan T-l and Nichter LS . (1998) The molecular basis of keloid and hypertrophic scar formation. Molec. Med. Today 4: 19–23
McCauley RL, Chopra V, Li Y-Y, Herndon DN and Robson MC . (1992) Altered cytokine production in black patients with keloids. J. Clin. Immunol. 12: 300–308
Abergel RP, Pizzuro D, Meeker CA, Lask G, Matsuoka LY, Minor RR, Chu M-L and Uitto J . (1985) Biochemical composition of the connective tissue in keloids and analysis of collagen metabolism in keloid fibroblast cultures. J. Invest. Dermatol. 84: 384–390
Ala-Kokko L, Rintala A and Savolainen E-R . (1987) Collagen gene expression in keloids: Analysis of collagen metabolism and type I, II, IV and V procollagen mRNA in keloid tissue and keloid fibroblast cultures. J. Invest. Dermatol. 89: 238–244
Peltonen J, Hsiao LL, Jaakkola S, Sollberg S, Aumailley M, Timpl R, Chu M-L and Uitto J . (1991) Activation of collagen gene expression in keloids: Co-localization of type I and VI collagen and transforming growth factor-β1 mRNA. J. Invest. Dermatol. 97: 240–248
Friedman DW, Boyd CD, Mackenzie JW, Norton P, Olson RM and Deak SB . (1993) Regulation of collagen gene expression in keloids and hypertrophic scars. J. Surg. res. 55: 214–222
Bettinger DA, Yager DR, Diegelman RF and Cohen IK . (1996) The effect of TGF-β on keloid fibroblasts proliferation and collagen synthesis. Plastic Reconstr. Surg. 98: 827–833
Sato H, Suzuki A, Funahashi M, Takezawa T, Ogawa Y and Yoshizato K . (1996) Characteristics of growth, morphology, contractility and protein expression of fibroblasts derived from keloid. Wound Repair Regener. 4: 103–114
Younai S, Nichter LS, Wellisz T, Reinisch J, Nimni ME and Tuan T-L . (1994) Modulation of collagen synthesis by transforming growth factor-β in keloid and hypertrophic scar fibroblasts. Ann. Plast. Surg. 33: 148–154
Kikuchi K, Kadono T and Takehara K . (1995) Effects of various growth factors and histamine on cultured keloid fibroblasts. Dermatol. 190: 4–8
Yamaguchi Y, Mann DM and Ruoslahti E . (1990) Negative regulation of the transforming growth factor-β by the proteoglycan decorin. Nature 346: 281–284
Tan EML, Hoffren J, Rouda S, Greenbaum S, Fox JW, Moore JH and Dodge GR . (1993) Decorin, versican and biglycan gene expression by keloid and normal dermal fibroblasts: Differential regulation by basic fibroblast growth factor. Exp. Cell Res. 209: 200–207
Hunzelmann N, Anders S, Sollberg S, Schonherr E and Krieg T . (1996) Coordinate induction of collagen type I and biglycan expression in keloids. Br. J. Dermatol. 135: 94–399
Darby I, Skalli O and Gabbiani G . (1990) α-Smooth muscle actin is transiently expressed by myofibroblasts during experimental wound healing. Lab. Investig. 63: 21–29
Masur SK, Dewal HS, Dinh TT, Ehrenburg I and Petridou S . (1996) Myofibroblasts differentiate from fibroblasts when plated at low density. Proc. Natl. Acad. Sci. 93: 4219–4223
Desmoulière A, Geinoz A, Gabbiani F and Gabbiani G . (1993) Transforming factor-β1 induces α-smooth muscle actin expression in granulation tissue myofibroblasts and in quiescent and growing cultured fibroblasts. J. Cell Biol. 122: 103–111
Narani N, Arora PD, Lew A, Luo M, Glogauer M, Ganss B and McCuloch CAG . (1997) Transforming growth factor-β induction of α-smooth muscle actin is dependent on the deformability of the collagen matrix. Curr. Top. Pathol. 93: 47–60
Arora PD, Narani N and McCulloch CAG . (1999) The compliance of collagen gels regulates transforming growth factor-β induction of α-smooth muscle action in fibroblasts. Am. J. Pathol. 154: 871–882
Serini G, Bochaton-Piallat M-L, Ropraz P, Geinoz A, Borsi L, Zardi L and Gabbiani G . (1998) The fibronectin domain ED-A is crucial for myofibroblastic phenotype induction by transforming factor-β1. J. Cell Biol. 142: 873–881
Balza E, Borsi L, Allemanni G and Zardi L . (1988) Transforming growth factor β regulates the level of different fibronectin isoforms in normal human cultured fibroblasts. FEBS Lett. 228: 42–44
Bürger A, Wagner C, Viedt C, Reis B, Hug F and Hänsch GM . (1998) Fibronectin synthesis by human tubular epithelial cells in culture: Effects of PDGF and TGF-β on synthesis and splicing. Kidney Int. 54: 407–415
Clark RAF . (1993) Regulation of fibroplasia in cutaneous wound repair. Am. J. Med. Sci. 306: 42–48
Desmoulière A, Redard M, Darby I and Gabbiani . (1995) Apoptosis mediates the decrease in cellularity during the transition between granulation tissue and scar. Am. J. Pathol. 146: 56–66
Berndt A, Koshmehl H, Mandel U, Gabler U, Luo X, Celeda D, Zardi L and Katenkamp D . (1995) TGFβ and bFGF synthesis and localization in Dupuytren's disease (nodular palmar fibromatosis) relative to cellular activity, myofibroblast phenotype and oncofetal variants of fibronectin. Histochem. J. 27: 1014–1020
Wilutzky B, Berndt A, Katenkamp D and Koshmehl H . (1998) Programmed cell death in nodular palmar fibromatosis (Morbus Dupuytren). Histol. Histopathol. 13: 67–72
Desmoulière A, Geinoz A, Gabbiani F and Gabbiani G . (1993) Transforming factor-β1 induces α-smooth muscle actin expression in granulation tissue myofibroblasts and in quiescent and growing cultured fibroblasts. J. Cell Biol. 122: 103–111
Grinnell F, Zhu M, Carlson MA and Abrams JM . (1999) Release of mechanical tension triggers apoptosis of human fibroblasts in a model of regressing granulation tissue. Exp. Cell Res. 248: 608–619
Ehrlich HP, Desmoulière A, Diegelman RF, Cohen IK, Compton CC, Garner WL, Kapanci Y and Gabbiani G . (1994) Morphological and immunochemical differences between keloid and hypertrophic scar. Am. J. Pathol. 145: 105–113
Ehrlich HP, Cremona O and Gabianni G . (1998) The expression of alpha 2 beta 1 integrin and alpha smooth muscle actin in fibroblasts grown on collagen. Cell Biochem. Funct. 16: 129–137
Appleton I, Brown NJ and Willoughby DA . (1996) Apoptosis, necrosis and proliferation. Possible implications in the etiology of keloids. Am. J. Pathol. 149: 1441–1447
Ladin DA, Hou Z, Patel D, McPhail M, Olson JC, Saed GM and Fivenson DP . (1998) p53 and apoptosis alterations in keloids and keloid fibroblasts. Wound Repair Regen. 6: 28–37
Saed GM, Ladin D, Olson J, Han X, Hou Z and Fivenson D . (1998) Analysis of p53 gene mutations in keloids using polymerase chain reaction-based single strand conformational polymorphism and DNA sequencing. Arch. Dermatol. 134: 963–967
Moulin V, Castilloux G, Jean A, Garrel DR, Auger FA and Germain L . (1996) In vitro models to study wound healing fibroblasts. Burns 22: 359–362
Moulin V, Castilloux G, Auger FA, Garrel D, O'Connor-McCourt MD and Germain L . (1998) Modulated response to cytokines of human wound healing myofibroblasts compared to dermal fibroblasts. Exp. Cell Res. 238: 283–293
Gorczyca W, Gong J and Darzynkiewicz Z . (1993) Detection of DNA strand breaks in individual apoptotic cells by the in situ terminal deoxynucleotidyl transferase and nick translation assays. Cancer Res. 53: 1945–1951
Negoiescu A, Lorimier P, Labat-Moleur F, Drouet C, Robert C, Guillermet C, Brambilla C and Brambilla E . (1996) In situ apoptotic cell labeling by the TUNEL method: improvement and evaluation of cell preparations. J. Histochem. Cytochem. 44: 959–968
Trump BF and Berezesky IK . (1998) The reaction of cells to lethal injury: Oncosis and necrosis–the role of calcium. In: When Cells Die. Lockshin RA, Zakeri Z and Tilly JL eds. (New York: J Wiley & Sons) pp. 57–97
Peyrol S, Raccurt M, Gerard F, Gleyzal C, Grimaud JA and Sommer P . (1997) Lysyl oxidase gene expression in the stromal reaction to in situ and invasive ductal breast carcinoma. Am. J. Pathol. 150: 497–507
Babu M, Diegelman R and Oliver N . (1992) Keloid fibroblasts exhibit an altered response to TGF-β. J. Invest. Dermatol. 99: 650–655
Desmoulière A . (1995) Factors influencing myofibroblast differentiation during wound healing and fibrosis. Cell. Biol. Intern. 19: 471–476
Frank S, Madlener M and Werner S . (1996) Transforming growth factors β1, β2, β3 and their receptors are differentially regulated during normal and impaired wound healing. J. Biol. Chem. 271: 10188–10193
Younai S, Venters G, Vu S, Nichter L, Nimni ME and Tuan T-L . (1996) Role of growth factors in scar contraction: An in vitro analysis. Ann. Plast. Surg. 36: 495–502
Crawford SE, Stellmach V, Murphy-Ullrich JE, Ribeiro SMF, Lawler JH, Hynes RO, Boivin GP and Bouck N . (1998) Thrombospondin-1 is the major activator of TGFβ-1 in vivo. Cell 93: 1159–1170
Mymric J, Shire K and Bayley ST . (1994) Induction of apoptosis by adenovirus type 5 E1A in rat cells requires a proliferation block. Oncogene 9: 1187–1193
Desjardins LM and MacManus JP . (1995) An adherent cell model to study different stages of apoptosis. Exp. Cell Res. 216: 380–387
Ishizaki Y, Cheng L, Mudge AW and Raff MC . (1995) Programmed cell death by default in embryonic cells, fibroblasts, and cancer cells. Exp. Cell Res. 216: 380–387
Brezden CB and Rauth AM . (1996) Differential cell death in immortalized and nonimmortalized cells at confluency. Oncogene 12: 201–206
Zhang H-Y, Gharaee-Kermani M and Phan SH . (1997) Regulation of lung fibroblast α-smooth muscle actin expression, contractile phenotype and apoptosis by IL-1β. J. Immunol. 158: 1392–1399
Funato N, Moriyama K, Shimokawa H and Kuroda T . (1997) Basic fibroblast growth factor induces apoptosis in myofibroblastic cells isolated from rat palatal mucosa. Biochem. Biophys. Res.Commun. 240: 21–26
Grinnell F . (1994) Fibroblasts, myofibroblasts and wound contraction. J. Cell Biol. 124: 401–404
Fluck J, Querfeld C, Cremer A, Niland S, Krieg T and Solverg S . (1998) Normal human primary fibroblasts undergo apoptosis in three-dimensional contractile gels. J. Invest. Dermatol. 110: 153–157
Martin SJ, Reutelingsperger CPM, McGahon AJ, Rader JA, van Schie RCAA, LaFace DM and Green DR . (1995) Early distribution of plasma membrane phosphatidylserine is a general feature of apoptosis regardless of the initiating stimulus: Inhibition by overexpression of Bcl-2 and Abl. J. Exp. Med. 182: 1545–1556
Acknowledgements
We thank Dr. C Pullis for the FACS analysis, Dr. N Ramamurthy and the members of the Simon group for helpful discussions and advice. This work was partially funded by a grant to AE Katz from the American Association of Plastic and Reconstructive Surgery.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Edited by P Cohen
Rights and permissions
About this article
Cite this article
Chipev, C., Simman, R., Hatch, G. et al. Myofibroblast phenotype and apoptosis in keloid and palmar fibroblasts in vitro. Cell Death Differ 7, 166–176 (2000). https://doi.org/10.1038/sj.cdd.4400605
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4400605
Keywords
This article is cited by
-
Atypische, Myofibroblasten-reiche Keloide im Rahmen einer Acne vulgaris
Der Hautarzt (2022)
-
The effect of 5α-oleandrin on keloid fibroblast activities
BMC Proceedings (2019)
-
Transforming growth factor-β in stem cells and tissue homeostasis
Bone Research (2018)
-
Mortalin deficiency suppresses fibrosis and induces apoptosis in keloid spheroids
Scientific Reports (2017)
-
3D modeling of keloid scars in vitro by cell and tissue engineering
Archives of Dermatological Research (2017)