Abstract
Study design
Cohort study. Retrospective analysis of T2-weighted magnetic resonance images (MRIs) and clinical documentation.
Objectives
To evaluate the relationship between the presence/absence and widths of midsagittal tissue bridges and walking ability among veterans with cervical, predominantly chronic SCI.
Setting
University research and hospital setting.
Methods
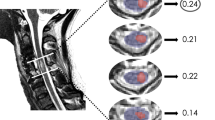
T2-weighted midsagittal MRIs of 22 United States veterans with cervical spinal cord injuries were examined. The presence/absence of midsagittal tissue bridges were determined, and the widths of present ventral and dorsal tissue bridges were measured. Midsagittal tissue bridge characteristics were related to each participant’s ability to walk based off examination of clinical documentation.
Results
Fourteen of the analyzed participant images revealed the presence of midsagittal tissue bridges. Ten of those individuals (71%) possessed overground walking ability. The 8 individuals with no apparent tissue bridges were all unable to walk. There was a significant correlation between walking and widths of ventral midsagittal tissue bridges (r = 0.69, 95%CI: 0.52, 0.92, p < 0.001), as well as dorsal midsagittal tissue bridges (r = 0.44, 95%CI: 0.15, 0.73, p = 0.039).
Conclusion
The evaluation of midsagittal tissue bridges may be useful in various rehabilitation settings to help inform patients’ plan of care, allocation of neuromodulatory resources, and appropriate stratification into research cohorts.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Additional data are available from the corresponding author on reasonable request.
References
Berliner JC, O’Dell DR, Albin SR, Dungan D, Sevigny M, Elliott JM, et al. The influence of conventional T2 MRI indices in predicting who will walk outside one year after spinal cord injury. J Spinal Cord Med. 2023;46:501–7.
David G, Seif M, Huber E, Hupp M, Rosner J, Dietz V, et al. In vivo evidence of remote neural degeneration in the lumbar enlargement after cervical injury. Neurology. 2019;92:e1367–77. https://doi.org/10.1212/wnl.0000000000007137
Huber E, Lachappelle P, Sutter R, Curt A, Freund P. Are midsagittal tissue bridges predictive of outcome after cervical spinal cord injury? Ann Neurol. 2017;81:740–8. https://doi.org/10.1002/ana.24932
O’Dell DR, Weber KA, Berliner JC, Elliott JM, Connor JR, Cummins DP, et al. Midsagittal tissue bridges are associated with walking ability in incomplete spinal cord injury: a magnetic resonance imaging case series. J Spinal Cord Med. 2020;43:268–71. https://doi.org/10.1080/10790268.2018.1527079
Pfyffer D, Huber E, Sutter R, Curt A, Freund P. Tissue bridges predict recovery after traumatic and ischemic thoracic spinal cord injury. Neurology. 2019;93:e1550–60. https://doi.org/10.1212/WNL.0000000000008318
Pfyffer D, Vallotton K, Curt A, Freund P. Tissue bridges predict neuropathic pain emergence after spinal cord injury. J Neurol Neurosurg Psychiatry. 2020;91:1111–7. https://doi.org/10.1136/jnnp-2020-323150
Pfyffer D, Vallotton K, Curt A, Freund P. Predictive value of midsagittal tissue bridges on functional recovery after spinal cord injury. Neurorehabil Neural Repair. 2021;35:33–43. https://doi.org/10.1177/1545968320971787
Smith AC, Angeli CA, Ugiliweneza B, Weber KA, Bert RJ, Negahdar M, et al. Spinal cord imaging markers and recovery of standing with epidural stimulation in individuals with clinically motor complete spinal cord injury. Exp Brain Res. 2022;240:279–88. https://doi.org/10.1007/s00221-021-06272-9
Smith AC, O’Dell DR, Thornton WA, Dungan D, Robinson E, Thaker A, et al. Spinal cord tissue bridges validation study: predictive relationships with sensory scores following cervical spinal cord injury. Top Spinal Cord Inj Rehabil. 2021;28:111–5.
Smith AC, O’Dell DR, Thornton WA, Dungan D, Robinson E, Thaker A, et al. Spinal cord tissue bridges validation study: predictive relationships with sensory scores following cervical spinal cord injury. Top Spinal Cord Inj Rehabil. 2022;28:111–5.
Vallotton K, Huber E, Sutter R, Curt A, Hupp M, Freund P. Width and neurophysiologic properties of tissue bridges predict recovery after cervical injury. Neurology. 2019;92:e2793–e2802. https://doi.org/10.1212/WNL.0000000000007642
Rupp R, Biering-Sørensen F, Burns SP, Graves DE, Guest J, Jones L, et al. International standards for neurological classification of spinal cord injury: revised 2019. Top Spinal Cord Inj Rehabil. 2021;27:1–22.
Hornby TG, Reisman DS, Ward IG, Scheets PL, Miller A, Haddad D, et al. Clinical practice guideline to improve locomotor function following chronic stroke, incomplete spinal cord injury, and brain injury. J Neurol Phys Ther. 2020;44:49–100.
Rowald A, Komi S, Demesmaeker R, Baaklini E, Hernandez-Charpak SD, Paoles E, et al. Activity-dependent spinal cord neuromodulation rapidly restores trunk and leg motor functions after complete paralysis. Nat Med. 2022;28:260–71. https://doi.org/10.1038/s41591-021-01663-5
Rutges JP, Kwon BK, Heran M, Ailon T, Street JT, Dvorak MF. A prospective serial MRI study following acute traumatic cervical spinal cord injury. Eur Spine J. 2017;26:2324–32.
Scivoletto G, Romanelli A, Mariotti A, Marinucci D, Tamburella F, Mammone A, et al. Clinical factors that affect walking level and performance in chronic spinal cord lesion patients. Spine. 2008;33:259–64.
Funding
ACS was supported by NIH Eunice Kennedy Shriver National Institute of Child Health and Human Development – K01HD106928. WAT and ACS were supported by the Boettcher Foundation’s Webb-Waring Biomedical Research Program.
Author information
Authors and Affiliations
Contributions
WAT was responsible for designing the study, assessing the imaging, analyzing imaging data, interpreting the results, and writing the report. GM was responsible for providing access to the images and determining walking ability of the participants. He also contributed to providing participant demographic information and provided feedback on the report. SR was responsible for providing access to the images and determining walking ability of the participants. She also contributed to providing participant demographic information and provided feedback on the report. AB was responsible for providing access to the images and provided feedback on the report. KR was responsible for assisting with the reliability testing for imaging measurements. She also provided feedback on the report. DC provided approval for project collaboration, access to the images, and contributed to determining walking ability of the participants. ACS was responsible for providing funding for the project and training in imaging measurements. He also contributed with collecting images for assessment, data analysis and interpretation, and providing feedback on the report.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The research described in our manuscript was in compliance with the Declaration of Helsinki and approved by COMIRB, the Colorado Multiple Institutional Review Board.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Thornton, W.A., Marzloff, G., Ryder, S. et al. The presence or absence of midsagittal tissue bridges and walking: a retrospective cohort study in spinal cord injury. Spinal Cord 61, 436–440 (2023). https://doi.org/10.1038/s41393-023-00890-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41393-023-00890-6