Abstract
NKG2D is an important immunosurveillance receptor that responds to stress-induced ligand expression on tumors and virus-infected cells. Human natural killer cells express NKG2D and require the transmembrane adaptor DAP10 to initiate their full cytotoxic activation. However, DAP10 has no immunoreceptor tyrosine-based activation motif and thus the mechanism of recruiting 'downstream' effector proteins is unclear. We show here that binding of the p85 subunit of phosphatidylinositol-3- kinase to DAP10 could not by itself trigger cell-mediated cytotoxicity and that binding of an intermediate consisting of the DAP10 binding partner Grb2 and the effector molecule Vav1 (Grb2-Vav1) to DAP10 was sufficient to initiate tyrosine-phosphorylation events. For full calcium release and cytotoxicity to occur, both Grb2-Vav1 and p85 had to bind to DAP10. These findings identify a previously unknown mechanism by which NKG2D-DAP10 mediates cytotoxicity and provides a framework for evaluating activation by other receptor complexes that lack immunoreceptor tyrosine-based activation motifs.
Similar content being viewed by others
Main
The cytotoxic lymphocyte-activating receptor NKG2D recognizes ligands such as MICA (in human) and Rae-1 (in mouse) that are upregulated by DNA damage and replication inhibition–induced DNA-repair pathways such as those initiated during tumorigenesis and viral infection1,2,3,4. The importance of NKG2D in immunosurveillance has been emphasized by data detailing the importance of NKG2D-mediated signaling in downregulating carcinogen-induced tumor incidence and tumor progression5. In addition, protective interleukin 12 and interleukin 21 tumor therapies require functional NKG2D5,6, and a DNA vaccine that induces NKG2D ligands has been shown to increase the efficacy of an established tumor vaccination protocol7. Moreover, NKG2D function is recognized as an important factor in transplantation: bone marrow graft cells have been shown to express an NKG2D ligand and treatment with an NKG2D blocking antibody prevents graft rejection8. Finally, NKG2D is also important in the pathogenesis of autoimmune diseases. For example, patients with celiac disease express the NKG2D ligand MICA on the surface of their intestinal cells, and CD8+ T cells that normally only costimulate through NKG2D9 can be fully cytotoxic in those patients10.
Despite advances in understanding the clinical importance of NKG2D, little is known about the intracellular signals mediating NKG2D-initiated activation. In humans, NKG2D couples to the transmembrane adaptor DAP10 for intracellular signaling and can deliver a full cytotoxic response when triggered11,12,13,14. However, DAP10 does not have an immunoreceptor tyrosine-based activation motif (ITAM) but instead contains a 'traditional' costimulatory phosphatidylinositol-3-kinase (PI(3)K) binding motif, YINM11. DAP10 also does not use the kinase Syk or the adaptor Lat, yet other effector proteins such as SLP-76, PLC-γ2 and Vav1 are still recruited and activated during the cytotoxic response13,14. Exactly how this recruitment occurs remains unclear.
The NKG2D receptor complex is hexameric in structure, containing two NKG2D and four DAP10 molecules15. With four potential YINM binding sites, the NKG2D-DAP10 receptor complex could potentially recruit a combination of different 'downstream' adaptors that might coordinate initiation of the cytotoxic signaling pathway. Two potential DAP10 binding partners have been described, one of which is the p85 regulatory subunit of PI(3)K11,16. Because the DAP10 YINM motif closely resembles the YMNM motif of the costimulatory CD28 receptor, it has been assumed that only p85 binds to DAP10 during an NKG2D-mediated cytotoxic response and that this is sufficient to recruit downstream effectors for directed granule release. That assumption is supported by data showing that the PI(3)K inhibitor wortmannin completely abrogates NKG2D-mediated cytotoxicity13. However, those data indicate only that PI(3)K is necessary at some point in the pathway and do not address the issue of whether p85 must be directly recruited to DAP10 or whether this recruitment would be sufficient for initiating a cytotoxic response.
The other potential DAP10 binding partner that has been described is growth factor receptor–bound protein 2 (Grb2)16. The main function of Grb2 in T cell receptor signaling seems to be recruiting and activating the Ras-Sos pathway; thus, its potential involvement in granule-dependent cell-mediated cytotoxicity remains unclear. Also, although a Grb2-Vav1 interaction has been described and characterized in a crystal structure17,18,19, the functional relevance of such an interaction has not yet been examined in cytotoxic lymphocyte activation. Thus, binding of neither Grb2 nor p85 to DAP10 has actually been explored for functional effects in NKG2D signaling.
Here we explore the individual contributions of Grb2 and p85 to the NKG2D-mediated cytotoxic response. We found that binding of DAP10 to p85 alone did not lead to phosphorylation of downstream effectors or trigger calcium release or cytotoxicity. In contrast, binding of DAP10 to Grb2 alone resulted in phosphorylation of SLP-76, PLC-γ2 and Vav1 as well as reduced calcium release and cytotoxicity. Full calcium release and cytotoxicity only occurred when both adaptors were recruited to the signaling complex. Furthermore, we compared wild-type Vav1 with a mutant that eliminates the Grb2-Vav1 interaction and found that the Grb2-Vav1 interaction was necessary for SLP-76 and PLC-γ2 phosphorylation as well as calcium release and cytotoxicity. Thus, we propose a model in which stimulated and aggregated NKG2D-DAP10 complexes recruit a Grb2-Vav1 intermediate and the p85 subunit of PI(3)K. The Grb2-Vav1 intermediate is responsible for coupling the receptor to SLP-76 and PLC-γ2, whereas both Grb2-Vav1 and PI(3)K are required for optimal calcium release and cytotoxicity.
Results
Binding of p85 to DAP10 is not sufficient for cytotoxicity
Although an association between phosphorylated DAP10 and both p85 and Grb2 has been documented11,16, the traditional view that only p85 is required for DAP10-mediated cytotoxicity has remained. We first verified the stimulation-dependent DAP10 recruitment of Grb2 (Supplementary Fig. 1 online). Then, to test the hypothesis that the DAP10-p85 interaction is sufficient for DAP10-mediated cytotoxicity, we sought to independently disrupt the binding of DAP10 to the two adaptors. The YINM motif in DAP10 contains both a p85 binding site (YxxM) and a Grb2 binding site (YxNx; where 'x' is any amino acid). Studies have shown that altering the '+2' position to any amino acid, including Asp or Glu, does not affect the binding of p85 to its motif, but altering the '+3' position from Met to any other amino acid abrogates p85 binding20. In contrast, altering the '+2' position from Asp to any other amino acid abrogates the binding of Grb2 to its motif, whereas Grb2 binding is unaffected by changes in the '+3' position, including Met or Glu20,21,22. Thus, we created a DAP10-M88Q point mutant to disrupt p85 but not Grb2 binding and a DAP10-N87Q point mutant to disrupt Grb2 but not p85 binding. We created phosphorylated and unphosphorylated fusion proteins of glutathione S-transferase (GST) and DAP10 (GST.DAP10; Fig. 1a), and by both protein-protein immunoblot analysis and precipitation assay, Grb2 interacted directly and comparably with phosphorylated wild-type DAP10 and DAP10-M88Q but not with DAP10-N87Q (Fig. 1b,c). In multiple experiments using both endogenous and overexpressed p85 in protein-protein immunoblots and precipitation assays, the DAP10-p85 interaction was difficult to detect sensitively in human natural killer (NK) clones (data not shown). However, we were able to detect equivalent association of p85 with phosphorylated wild-type DAP10 and DAP10-N87Q but not with DAP10-M88Q in a precipitation assay (Fig. 1c). These data indicate that both p85 and Grb2 can directly associate with phosphorylated DAP10 and that the binding sites can be independently disrupted.
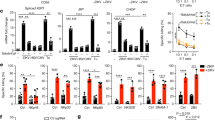
(a) Immunoblot for phosphorylated tyrosine (p-Tyr; top) and amido black staining (bottom) of 1 μg (top) or 10 μg (bottom) of GST.DAP10 fusion proteins resolved by SDS-PAGE and transferred to a membrane. (b) Protein-protein immunoblot analysis of 3.5 × 107 Jurkat cells expressing Flag-tagged Grb2 immunoprecipitated with anti-Flag. Immunoprecipitates were loaded equally onto seven different lanes and resolved by SDS-PAGE, and separate membrane strips were probed with the various GST.DAP10 fusion proteins. The membrane strip that had been blotted with GST.DAP10-Y85F was then reblotted with anti-Flag. (c) Immunoblots (bottom) of lysates from primary NK cells that were incubated with phosphorylated or nonphosphorylated GST.DAP10 fusion proteins and precipitated (IP) with GSH-agarose beads. Above, densitometry of the relative band darkness for each blot. (d) Flow cytometry for CD4 surface expression on Jurkat cells or NK clones expressing various chimeric receptors (above histograms) and stained with fluorescein isothiocyanate–labeled anti-CD4. Shaded histograms represent CD4 surface expression on cells infected with nonrecombinant control vaccinia. (e) Redirected cytotoxicity assay of NK cell killing. NK clones expressing NKG2D or various chimeric receptors were incubated with P815 cells coated with anti-NKG2D or anti-CD4 at various effector/target ratios (horizontal axis). WT, wild-type; YF, DAP10-Y85F; NQ, DAP10-N87Q; MQ, DAP10-M88Q; p-, phosphorylated. Data are representative of seven separate experiments.
Direct interaction between DAP10 and p85 is consistent with involvement of PI(3)K in NKG2D-initiated activation. To determine whether an association between DAP10 and p85 is sufficient to trigger NK cell–mediated cytotoxicity, we made chimeric Flag-tagged receptors with the extracellular and transmembrane portions of CD4 linked to the intracellular portion of DAP10 (F.CD4-DAP10; Supplementary Fig. 2 online). We expressed the chimeric receptors using recombinant vaccinia virus. In addition, we made Flag-tagged chimeric receptors with specific DAP10 substitutions (Fig. 1a–c). The CD4-DAP10 chimeric receptors were equivalently expressed on cell surfaces (Fig. 1d, top and middle). We tested NK clones infected with recombinant vaccinia expressing the chimeric receptors for their ability to lyse P815 tumor cells coated with antibody to NKG2D (anti-NKG2D) or anti-CD4 in a redirected cytotoxicity assay. Expression of the chimeric receptors did not affect killing initiated by the endogenous NKG2D receptor (data not shown). Interrupting the association of DAP10 with p85 (F.CD4-DAP10-M88Q) abrogated killing (Fig. 1e), supporting published data showing that NKG2D-mediated cytotoxicity is inhibited by the PI(3)K inhibitor wortmannin13. Notably, the F.CD4-DAP10-N87Q chimeric receptor, which does not bind Grb2 but can bind p85 (Fig. 1b,c), also could not trigger cytotoxicity (Fig. 1e). These results suggest that binding of DAP10 to either p85 or Grb2 alone is not sufficient to trigger DAP10-mediated cytotoxicity and that both binding sites are necessary for NKG2D-initiated killing.
Grb2 positively regulates DAP10-mediated cytotoxicity
Because a requirement for Grb2 has not been documented for NKG2D-mediated cytotoxicity, we sought to assess killing in a cellular environment in which Grb2 expression was suppressed. We introduced control small interfering RNA (siRNA) or Grb2-specific siRNA into NK clones, resulting in partial Grb2 suppression, as determined by immunoblot (Fig. 2a, inset); the specificity of the Grb2-specific siRNA was demonstrated by the lack of suppression of the adaptor GADS, Vav1, SLP-76, PLC-γ and dynamin-2 (data not shown). We then incubated the siRNA-expressing clones with anti-NKG2D-coated P815 cells in a redirected cytotoxicity assay. Partial Grb2 suppression partially inhibited NKG2D-mediated cytotoxicity (Fig. 2a) and, in a series of similar experiments, Grb2 expression directly correlated with NKG2D-initiated cytolytic activity (r = 0.92, P = 0.0012; two-tailed, one-sample t-test for correlation coefficients; Fig. 2b). NK cells with 75% Grb2 suppression (the greatest suppression attained) still had residual NKG2D function (about 50%; Fig. 2b). Although that could indicate functional redundancy of Grb2 with another molecule, a more likely explanation was that residual Grb2 was sufficient to mediate some cytotoxicity through NKG2D. Nevertheless, these results show that Grb2 is involved in NKG2D-initiated cytotoxicity and, along with the data reported above (Fig. 1), suggest that Grb2 directly binds to DAP10 and thereby positively regulates NKG2D-mediated cytotoxicity.
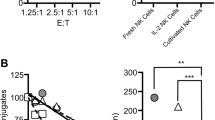
(a) Redirected cytotoxicity assay of NKG2D-mediated cytotoxicity. NK clones expressing control siRNA (Neg) or Grb2-specific siRNA (siGrb2) were incubated with P815 cells coated with anti-NKG2D at various effector/target ratios (horizontal axis). Inset, immunoblot of Grb2 protein expression. (b) Grb2 expression by NK clones and ability of NK clones to kill anti-NKG2D-coated P815 cells. NK clones expressing control siRNA or Grb2-specific siRNA were evaluated in a series of experiments. The results for each sample were normalized to those of the control siRNA sample for both lytic units and Grb2 expression. Grb2 expression was determined by immunoblot and densitometry.
Grb2 couples DAP10 to proximal phosphorylation events
To 'dissect' the individual functions of Grb2 and p85 in NKG2D-mediated cytotoxicity, we first examined the ability of the DAP10 mutant chimeric receptors to initiate phosphorylation of the proximal effectors SLP-76, PLC-γ2 and Vav1. We stimulated NK clones infected with recombinant vaccinia expressing the mutant DAP10 chimeric receptors (F.CD4-DAP10-M88Q and F.CD4-DAP10-N87Q) with anti-CD4 followed by goat anti-mouse IgG F(ab′)2 (secondary antibody). We then immunoprecipitated cell lysates for SLP-76, PLC-γ2 and Vav1, resolved the immunoprecipitates by SDS-PAGE and probed for tyrosine phosphorylation. DAP10-mediated phosphorylation of SLP-76, PLC-γ2 and Vav1 was completely abrogated when the Grb2 binding site on DAP10 was disrupted (although p85 could still bind; Fig. 3a). However, when the p85 binding site was disrupted (but Grb2 could still bind), tyrosine phosphorylation of SLP-76, PLC-γ2 and Vav1 occurred to a degree that varied depending on the specific NK clone tested but was nevertheless consistently comparable to phosphorylation induced by wild-type DAP10 (Fig. 3a). This is consistent with published data showing that wortmannin treatment does not inhibit NKG2D-initiated proximal tyrosine-phosphorylation events13. These results suggest that binding of Grb2 but not p85 to DAP10 is necessary for specific DAP10-initiated proximal tyrosine-phosphorylation events.
We next tested if recruitment of Grb2 to a signaling complex (a 'signalosome') is sufficient to initiate the tyrosine phosphorylation of SLP-76, PLC-γ2 and Vav1. We made Flag-tagged chimeric receptors directly linking the extracellular and transmembrane portions of CD4 to either Grb2 or p85 (F.CD4-Grb2 and F.CD4-p85; Supplementary Fig. 2). There was approximately equivalent expression of the CD4-Grb2 chimeric receptor and CD4-DAP10 chimeric receptor on the surface (Fig. 1d, bottom). We stimulated NK cell clones infected with recombinant vaccinia expressing F.CD4-Grb2 and treated them as described above. Crosslinking of F.CD4-Grb2 alone at the surface was sufficient to initiate tyrosine phosphorylation of SLP-76, PLC-γ2 and Vav1 (Fig. 3b) and the phosphorylation at 1 min was as robust as that initiated by F.CD4-DAP10, but by 5 min, the phosphorylation induced by F.CD4-Grb2 was much less. These data indicate that recruitment of Grb2 to a signalosome could initiate phosphorylation of SLP-76, PLC-γ2 and Vav1. It thus follows that binding of DAP10 to Grb2 (thereby recruiting it to the NKG2D signalosome) would be sufficient to initiate DAP10-mediated phosphorylation of SLP-76, PLC-γ2 and Vav1.
In a parallel experiment, we infected NK clones with recombinant vaccinia expressing the F.CD4-p85 chimeric receptor. Crosslinking F.CD4-p85 at the surface did not initiate phosphorylation events (Fig. 3c). In addition, the F.CD4-DAP10-N87Q chimeric receptor (which bound p85 but did not bind Grb2) did not cause tyrosine phosphorylation of SLP-76, PLC-γ2 and Vav1 (Fig. 3a). Thus, these results suggest that p85 is not involved sufficient for proximal effector tyrosine phosphorylation during DAP10-initiated signaling.
DAP10-initiated proximal phosphorylations require Grb2-Vav1
We next explored how Grb2 couples to SLP-76, PLC-γ2 and Vav1 during NKG2D-initiated signal transduction. Although a constitutive Grb2-Vav1 complex has been described and crystallized17,18,19, the physiological importance of this interaction in the activation of cytotoxic lymphocytes has not yet been assessed. To explore the function of this intermediate in NKG2D-mediated signaling, we first assessed whether Vav1 is required for the coupling of DAP10 to SLP-76 and PLC-γ. We infected a Vav1-deficient 'subline' of the Jurkat T cell line (J.Vav1) with recombinant vaccinia expressing F.CD4-DAP10 or a Flag-tagged chimeric receptor linking the extracellular and transmembrane portions of CD4 to the cytoplasmic tail of the CD3ζ chain (F.CD4-ζ; Supplementary Fig. 2). We then stimulated cells with anti-CD4. In the absence of Vav1, neither SLP-76 nor PLC-γ phosphorylation occurred after DAP10 crosslinking (Fig. 4a). In contrast, parallel experiments using SLP-76- or PLC-γ-deficient 'sublines' of Jurkat cells had almost wild-type amounts of Vav1 tyrosine phosphorylation (data not shown). Also, ITAM-mediated SLP-76 and PLC-γ tyrosine phosphorylation occurred in the absence of Vav1 (Fig. 4b). These data indicate that in contrast to ITAM-mediated signaling, Vav1 is 'upstream' of and is necessary for SLP-76 and PLC-γ tyrosine phosphorylation during DAP10 signaling.
(a) Immunoblot of lysates of Vav1-deficient Jurkat cells (J.Vav1) expressing F.CD4-DAP10 and either a Vav1 construct (above blots) or control (WR), stimulated with anti-CD4 (time, above lanes). Lysates were treated as described in Figure 3. (b) Immunoblot of J.Vav1 cells as described in a, except cells express the chimeric receptor F.CD4-ζ instead of F.CD4-DAP10. (c) Immunoblot of immunoprecipitated lysates from J.Vav1 cells. Cells expressing various Vav1 constructs (above blot) were immunoprecipitated with anti-Flag bound to goat anti-mouse agarose beads. Beads were washed and GST fusion protein (below blot) was added, followed by overnight incubation. Beads were then washed again and precipitates were resolved by SDS-PAGE, followed by immunoblot with anti-GST.
The next step in evaluating the importance of a potential Grb2-Vav1 intermediate in NKG2D-mediated signaling was to determine if the Grb2-Vav1 interaction was necessary for coupling of DAP10 to downstream effectors. The Grb2-Vav1 interaction described is unique, occurring through the Grb2 C-terminal Src homology 3 (SH3) domain and the Vav1 N-terminal SH3 domain17. A pivotal residue in this interaction is Pro 657 of Vav1 (ref. 18). We thus made a Vav1-P657A point mutant and then determined the consequences of this substitution on interaction of the Grb2 C-terminal SH3 domain with Vav1. We infected J.Vav1 cells with recombinant vaccinia expressing Flag-tagged wild-type Vav1 (F.Vav1-WT) or mutant Vav1 (F.Vav1-P657A). We immunoprecipitated lysates for Flag and washed them thoroughly, then incubated the immunoprecipitates with GST alone or GST fused to the C-terminal SH3 domain of Grb2. After washing the samples a second time, we resolved the remaining protein complexes by SDS-PAGE and probed with anti-GST. The Grb2 C-terminal SH3 domain specifically associated with wild-type Vav1 but not Vav1-P657A (Fig. 4c). In some experiments, residual interaction between Grb2 and Vav1-P657A could be detected, but it was much less than the Grb2–wild-type Vav1 interaction (data not shown). We verified equal wild-type and mutant Vav1 loading and purity by Coomassie staining (data not shown). These data confirmed that the Grb2-Vav1 interaction was constitutive and could be disrupted17,18.
We then assessed whether disrupting the Grb2-Vav1 interaction affected DAP10-mediated signaling. We infected J.Vav1 cells with recombinant vaccinia expressing F.CD4-DAP10 or F.CD4-ζ plus F.Vav1-WT, F.Vav1-P657A or control vaccinia. We stimulated cells with anti-CD4 followed by a goat anti-mouse IgG F(ab′)2. We immunoprecipitated lysates for SLP-76, PLC-γ and Vav1, resolved the immunoprecipitates by SDS-PAGE and probed for tyrosine phosphorylation. Both wild-type and mutant Vav1 were recruited to the signaling complex and were phosphorylated after ITAM receptor crosslinking (Fig. 4b), indicating that the mutant Vav could be phosphorylated. However, expression of only wild-type (not mutant) Vav1 could fully restore DAP10-mediated SLP-76, PLC-γ2 and Vav1 phosphorylation in J.Vav1 cells (Fig. 4a). In some experiments, minimal residual phosphorylation of PLC-γ could be detected with Vav-P657A, which was probably due to residual interaction of Grb2 with Vav1-P657A. These results suggest that a specific Grb2-Vav1 interaction is necessary for DAP10-mediated phosphorylation of SLP-76 and PLC-γ.
Lack of Grb2-Vav1 or p85 binding abrogates calcium flux
Because the DAP10-Grb2 interaction alone initiated tyrosine phosphorylation of PLC-γ2 (Fig. 3a,b), we next tested its ability to initiate calcium release. We used Jurkat cells for calcium experiments because of their greater utility than primary cells in sensitively detecting calcium signaling; moreover, DAP10-mediated calcium flux has been shown to be similar if not increased in Jurkat cells versus NK cells23. We stimulated Jurkat cells infected with recombinant vaccinia expressing the F.CD4-DAP10 chimeric receptors (or a control virus) with anti-CD4 followed by goat anti-mouse IgG F(ab′)2 and analyzed calcium flux by flow cytometry. Expression of the F.CD4-DAP10 chimeric receptors on the surface of Jurkat cells was similar to that on NK cells (Fig. 1d). Despite the ability of F.CD4-DAP10-M88Q to initiate PLC-γ2 tyrosine phosphorylation (Fig. 3a), however, calcium signaling was much less than that with wild-type DAP10 (Fig. 5a). Additionally, F.CD4-DAP10-N87Q could not initiate calcium signaling, consistent with its inability to activate SLP-76, PLC-γ2 or Vav1 (Figs. 3a and 5a). Thus, whereas coupling of Grb2 to DAP10 is sufficient to initiate downstream phosphorylation events, neither DAP10-Grb2 alone nor DAP10-p85 alone is sufficient to initiate an optimal calcium signal.
Jurkat cells expressing various chimeric receptors (in graph; a) or J.Vav1 cells expressing F.CD4-DAP10 (b, top) or F.CD4-ζ (b, bottom) and various Vav1 constructs (in graphs; b) were stimulated with anti-CD4 and calcium release was measured. Inset (b, top), representative immunoblot of Vav1 expression in J.Vav1 cells: left lane, control vaccinia; center lane, F.Vav1-WT; right lane, F.Vav1-P657A. WR, control vaccinia; NS, no stimulation.
Because the Grb2-Vav1 interaction was required for DAP10-mediated phosphorylation of SLP-76, PLC-γ and Vav1, we next tested the involvement of this intermediate in DAP10-mediated calcium flux. We coinfected J.Vav1 cells with recombinant vaccinia expressing F.CD4-DAP10 or F.CD4-ζ plus F.Vav1-WT, F.Vav1-P657A or control vaccinia virus. We then stimulated cells with anti-CD4 followed by a goat anti-mouse F(ab′)2 and analyzed calcium flux by flow cytometry. In the absence of Vav1, F.CD4-DAP10 could not initiate calcium release, whereas wild-type Vav1 fully restored that ability (Fig. 5b, top). However, calcium release in the presence of the mutant Vav1 was diminished substantially (Fig. 5b, top). In contrast, F.CD4-ζ was able to initiate calcium release in the absence of Vav1, and reconstitution with wild-type or mutant Vav1 equally enhanced the calcium signal (Fig. 5b, bottom). Thus, the defect in the activity of mutant Vav1 was specific to DAP10-mediated signaling and did not affect other Vav1 functions (such as cytoskeletal rearrangement) that may have potentially contributed to calcium release. Those data were consistent with the PLC-γ phosphorylation data (Fig. 4a,b) and suggest that the Grb2-Vav1 intermediate is also uniquely necessary for DAP10-mediated calcium flux.
The Grb2-Vav1 intermediate is necessary for cytotoxicity
To confirm the functional importance of the Grb2-Vav1 intermediate in a more physiological setting, we first examined whether Grb2 and Vav1 associate in NK cells. We immunoprecipitated lysates from untreated primary NK clones with a Vav1 specific antibody or with normal rabbit serum. We then resolved immunoprecipitates by SDS-PAGE, transferred them to a membrane and probed with a Grb2-specific antibody. Grb2 was present in the Vav1 immunoprecipitate but not the normal rabbit serum immunoprecipitate (Fig. 6a). Thus, endogenous Grb2 and Vav1 can constitutively associate in primary human NK cells.
(a) Immunoblot of immunoprecipitated lysates from primary NK clones. Clones left untreated (−) or expressing Flag-tagged Grb2 were immunoprecipitated with antibodies specific for Vav1 or Flag, respectively; immunoprecipitates were resolved by SDS-PAGE, transferred to a membrane and probed with anti-Grb2. NRS, normal rabbit serum. (b) NKG2D-mediated killing (top) and FcR-mediated killing (bottom). Left, NK clones expressing various Vav1 constructs (key) were incubated with P815 cells coated with anti-NKG2D (top) or anti-FcR (bottom). Right, pooling of data from several experiments (top, n = 5; bottom, n = 9). In each experiment, the lytic units for each sample were compared with lytic units for cells infected with vacccinia control (WR). Error bars represent s.e.m. Inset (top left), representative immunoblot of Vav1 expression in NK clones: left lane, vacccinia control; center lane, F.Vav1-WT; right lane, F.Vav1-P657A. (c) Redirected cytotoxicity assay of killing by NK clones expressing various constructs (below graph). Clones were incubated with P815 cells coated with anti-NKG2D or anti-CD4. Data are representative of seven separate experiments.
Next we investigated the function of the Grb2-Vav1 intermediate in NK cell–mediated cytotoxicity initiated by NKG2D. We infected NK clones with recombinant vaccinia viruses expressing F.Vav1-WT or F.Vav1-P657A (or with control virus). We then incubated the NK clones with P815 tumor cells coated with anti-NKG2D or anti–Fc receptor (anti-FcR) in a redirected cytotoxicity assay. Overexpression of wild-type Vav1 enhanced baseline NKG2D-mediated cytotoxicity approximately threefold (Fig. 6b, top). However, overexpression of mutant Vav1 did not enhance NKG2D-mediated cytotoxicity (Fig. 6b, top). In five independent experiments, the lytic units for cells overexpressing wild-type but not mutant Vav1 were significantly different from the lytic units for baseline NKG2D-initiated cytotoxicity (P < 0.0001, wild-type Vav1; P = 0.1069, Vav1-P657A; Dunnett's method with WR vaccinia control as the control group; Fig. 6b, top). In contrast, in nine independent experiments assessing FcR-mediated cytotoxicity, overexpression of both wild-type and mutant Vav1 significantly increased lytic units compared with baseline (P = 0.0004, wild-type Vav1; P = 0.0391, Vav1-P657A; Dunnett's Method with WR vaccinia control as the control group), and the 'fold increases' mediated by the two Vav1 constructs did not differ significantly from each other (P = 0.1269, two-tailed t-test assuming unequal variances; Fig. 6b, bottom). These data indicated that the Vav1-P657A substitution did not broadly affect the Vav1 functions initiated by multiple and different kinds of activating receptors. Instead, the direct interaction between Grb2 and Vav1 was uniquely necessary for optimal NKG2D-initiated cytotoxicity, consistent with the requirement for this intermediate in DAP10-mediated phosphorylation events and calcium release (Figs. 4a and 5b).
Membrane Grb2 and p85 is sufficient to initiate cytotoxicity
As reported above, whereas binding of DAP10 to Grb2 alone was sufficient for tyrosine phosphorylation events (Fig. 3a,b), both Grb2 and p85 were necessary for DAP10-mediated calcium release (Fig. 5a) and cytotoxicity (Fig. 1e). We next tested if recruitment of both Grb2 and p85 to the NKG2D signalosome was sufficient to initiate cytotoxicity. To avoid any interference from other potential DAP10 adaptors, we used the F.CD4-Grb2 and F.CD4-p85 chimeric receptors. We infected NK clones with various combinations of recombinant vaccinia viruses expressing the Grb2 chimeric receptor, the p85 chimeric receptor or a control virus. We then incubated the clones with P815 tumor targets coated with anti-NKG2D or anti-CD4 in a redirected cytotoxicity assay. Neither F.CD4-p85 nor F.CD4-Grb2 was able to initiate cytotoxicity (Fig. 6c). However, when stimulated in combination, F.CD4-Grb2 and F.CD4-p85 acted in synergy (Fig. 6c) to initiate considerable cell-mediated cytotoxicity despite the lower F.CD4-p85 expression at the cell surface (Fig. 1d). This synergy was not due to the presence of additional CD4 on the surface, because F.CD4-DAP10-Y85F did not act in synergy with F.CD4-Grb2 (data not shown). Those data indicated that recruitment of Grb2 and p85 to the receptor complex was sufficient to initiate the signaling events that culminated in NK cell killing of a tumor target. More broadly, the data suggest a model in which YINM motifs in the hexameric structure of the NKG2D receptor complex recruit some combination of Grb2-Vav1 and p85, leading to signal propagation and cytotoxicity (Supplementary Figure 3 online).
Discussion
Here we have demonstrated mechanistically how NKG2D initiates a cytotoxic response in the absence of an ITAM signaling motif. Many (if not most) activating immune-recognition receptor complexes (such as T cell receptors, B cell receptors, Fc receptors and killer immunoglobulin receptors) contain ITAMs in their intracellular signaling domains and thus use the well studied signaling pathways that couple proximal activation of Src family and Syk family tyrosine kinases to downstream effector molecules via specific adaptor molecules (such as Lat, SLP-76 and BLNK). Stimulation of ITAM-coupled receptors initiates rapid proximal tyrosine phosphorylation and increases in calcium flux. In contrast, human NKG2D signals through the non-ITAM-containing transmembrane adaptor DAP10 (refs. 11,12) and the tyrosine phosphorylation and calcium kinetics of this pathway are somewhat delayed13,23. Although Src family kinases are involved in initiating NKG2D signaling13, Syk family kinases are not recruited to the NKG2D signalosome, and without Syk family kinases, Lat is not phosphorylated13,14. Consequently, the longstanding assumption has been that the DAP10 YINM motif recruits the PI(3)K regulatory subunit p85 and thereby couples to necessary downstream effectors to initiate cytotoxicity.
We have demonstrated that that is not the case. Instead, because PI(3)K is not sufficient to fully affect downstream signaling molecules, DAP10 must also directly recruit a Grb2-Vav1 intermediate to initiate the further required downstream tyrosine phosphorylation of both SLP-76 and PLC-γ2. Binding of DAP10 to both p85 and Grb2, furthermore, is necessary for full calcium release and cytotoxicity, and recruitment of those two adaptors is sufficient to initiate the cytotoxic response. Thus, given the hexameric structure of the NKG2D receptor complex (two NKG2D molecules and four DAP10 molecules)15, it seems likely that the four YINM motifs recruit some combination of Grb2-Vav1 and p85, leading to signal propagation and cytotoxicity.
Because DAP10 has no canonical ITAM but instead has a 'costimulatory-like' YINM motif (because it is similar to the YMNM motif of the CD28 costimulatory molecule)11, NKG2D was first assumed to initiate signals mainly through PI(3)K activation. The involvement of PI(3)K in NKG2D signaling was supported by data showing an association of DAP10 with the p85 regulatory subunit11. Subsequently, data using the PI(3)K inhibitor wortmannin have shown that PI(3)K activity is essential for NKG2D-mediated cytotoxicity but not for phosphorylation of PLC-γ2 (ref. 13). The NKG2D signaling studies so far have not definitively shown whether p85 must directly bind DAP10, nor have those studies challenged the critical assumption that p85 is solely involved in initiating the DAP10 signal. We have shown here that disrupting the YxxM motif in DAP10 abrogated the association with p85, indicating that it binds directly to DAP10. We have also demonstrated that the DAP10-p85 interaction was necessary for calcium release and cytotoxicity. More notably, we have shown that p85 was not sufficient for cytotoxicity but that Grb2 (another adaptor) had to bind to DAP10 and recruit downstream effector molecules. One notable observation was that whereas binding of p85 to DAP10 was not necessary for PLC-γ2 tyrosine phosphorylation, it was necessary for full calcium release. Perhaps proteins with pleckstrin homology domains, such as Vav1 and PLC-γ2, are stabilized at (but not necessarily recruited to) the membrane as a result of PI(3)K activity, which might explain why the F.CD4-DAP10-M88Q and F.CD4-Grb2 chimeric receptors demonstrated robust but nonsustainable phosphorylation events and why calcium release was diminished despite near-normal initial tyrosine phosphorylation. Alternatively, PI(3)K activity could regulate the function of another molecule that can fully activate PLC-γ2 (such as ITK) and thereby promote calcium release24.
Despite the many studies demonstrating the importance of PI(3)K in NKG2D-mediated signaling, the mechanism by which SLP-76, PLC-γ2 and Vav1 are recruited to DAP10 have remained unclear. One study indicated that Grb2 can associate with phosphorylated DAP10 (ref. 16), but neither the nature (direct versus indirect) nor the functional relevance of that interaction were explored. A constitutive Grb2-Vav1 interaction has also been described in various studies17,18,19, but again the functional importance of the interaction in activating lymphocyte-mediated cytotoxicity was not addressed. Another study showed that cytoplasmic Grb2 is mainly an inhibitory molecule and that recruitment to the membrane serves merely to sequester it from activating effectors25.
We have shown not only that Grb2 could bind directly to DAP10 but also that this direct interaction was necessary for NKG2D-mediated cytotoxicity. Many Grb2 binding partners have been described, and although we have not explored all of those potential interactions in NKG2D-DAP10–initiated cytotoxicity, we have demonstrated that a Grb2-Vav1 complex formed in NK cells and that the interaction of DAP10 with Grb2-Vav1 was necessary and sufficient for recruitment and activation of Vav1, SLP-76 and PLC-γ2, which addresses the longstanding issue of how NKG2D, without coupling to Lat, recruits downstream effectors. We have also shown that the Grb2-Vav1 intermediate was necessary for DAP10-mediated (but not ITAM-mediated) calcium flux and cytotoxicity. Studies have shown that NKG2D 'preferentially' couples to specific isoforms of downstream effectors, whereas receptors using ITAM are not restricted to such isoform specificities23,26. Perhaps the unique Grb2-Vav1–mediated recruitment of molecules necessitates these isoform 'preferences', whereas Lat-mediated recruitment does not.
The prototypical T cell coreceptor CD28 also contains a YxNM motif that binds both p85 (refs. 27–29) and Grb2 (ref. 30). Binding of Grb2 to CD28 is also necessary for CD28-initiated Vav tyrosine phosphorylation in T cells21. CD28 might also activate NK cell cytotoxicity by a mechanism similar to the one NKG2D uses. Mouse NK cells express CD28 and can be activated by the CD28 ligand B7 (refs. 31–33), and a 'subline' of the human NK leukemia YT triggers cytotoxicity through CD28 stimulation alone34. Additionally, ectopic expression of B7 on tumor targets enhances cell-mediated cytotoxicity in untransformed human NK cells35,36, although it is unclear whether normal human NK cells express CD28, as one study has demonstrated surface expression35, whereas others have not36,37,38. Thus, further studies are necessary to fully elucidate the potential function of CD28 stimulation in normal human NK cells.
No studies so far have shown whether cytoplasmic proteins are first recruited to the membrane and are sufficient to initiate cell-mediated cytotoxicity independently of their cognate receptor complex. In the ITAM signaling pathway, recruitment of the kinase Syk to glycolipid-enriched microdomains is necessary but not sufficient to initiate downstream events without concurrent aggregation of the ITAM-containing receptor complex39. In contrast, for NKG2D, we have shown that mere recruitment of the two adaptor proteins Grb2 and p85 to the signaling complex was sufficient to initiate an alternative signaling pathway that culminated in cell-mediated cytotoxicity. Presumably, then, this is the minimum essential function of DAP10 phosphorylation in initiating NKG2D-mediated killing.
Thus, NKG2D uses a signaling pathway that differs fundamentally from receptors that couple to ITAM-containing transmembrane adaptors. Instead of recruiting a cytoplasmic kinase and using a 'super adaptor' to recruit other effectors, NKG2D-DAP10 directly recruits downstream effectors (SLP-76, PLC-γ2 and Vav1) and PI(3)K to initiate cytotoxicity; this 'shortcut' seems to eliminate a potentially important regulatory step (the step from Syk to Lat). However, in contrast to ITAM-containing receptors, which are always activating, human NKG2D has different functional effects depending on the cellular environment. For example, NKG2D stimulation has no observable effect in naive or (some) recently activated CD8+ T cells40, whereas in resting NK cells and other activated CD8+ T cells it is costimulatory9,41,42,43,44. Alternatively, NKG2D stimulation alone is fully activating and can initiate cytotoxicity in activated NK cells and CD8+ T cells from patients with some autoimmune diseases10,13,14,41,42. Perhaps the various outcomes of NKG2D stimulation are a result of its need to couple to multiple specific binding partners. Nevertheless, each activating immune receptor has a slightly different function in immunity and immune modulation, and each differential signaling pathway that is identified provides potential pharmacological targets for selective therapeutic intervention.
Methods
Reagents, cells and antibodies.
All reagents were obtained from Sigma unless stated otherwise. The human T cell leukemia line Jurkat and the Vav1-deficient Jurkat subline J.Vav1 were provided by R.T. Abraham (Wyeth Research, Pearl River, New York). The mouse mastocytoma P815 was obtained from American Type Culture Collection. Human NK cells were cloned and passaged as described45. Rabbit polyclonal antibodies to PLC-γ1, PLC-γ2, SLP-76 and Vav1 have been described46,47,48. Monoclonal anti-NKG2D (R&D Systems), monoclonal anti-GST (Pierce Biotechnology), monoclonal anti-Grb2 (Upstate Signaling Solutions), anti-DAP10 (Santa Cruz), monoclonal anti-p85α (Upstate), anti–phosphorylated tyrosine (4G10; Upstate) and monoclonal anti-CD4 (BD Biosciences) were also used. Goat anti-mouse IgG F(ab′)2 was obtained from MP Biomedicals.
Chimeric receptors, point mutations and recombinant vaccinia.
Flag-tagged chimeric receptors were generated using extracellular and transmembrane CD4 and the intracellular portions of either the 20–amino acid intracellular DAP10 tail, various mutants of the DAP10 tail, full-length Grb2, full-length p85 or the intracellular portion of CD3ζ. Flag-tagged CD4-DAP10 and CD4-DAP10-Y85F chimeric receptors were generated by PCR and standard molecular biology techniques as described13. Human p85α was provided by E. Leof (Mayo Clinic College of Medicine, Rochester, Minnesota). Full-length Grb2 and p85α were cloned into a pSP11.F.CD4(tm) construct that has been described13. DAP10-N87Q, DAP10-M88Q and Vav1-P657A point mutants were generated with the QuikChange Site-Directed Mutagenesis Kit (Stratagene) according to the kit instructions. All constructs were sequenced and verified for accuracy. Recombinant vaccinia viruses were generated with the pSP11.F or pSP11.F.CD4 cloning vectors as described13,49.
Calcium mobilization assays.
Intracellular calcium flux was measured by flow cytometry in cells 'loaded' with the calcium indicator Indo-1 as described23,50.
Cytotoxicity assays.
The 51Cr-release assays were done as described45. In redirected cytotoxicity assays, the FcR+ P815 tumor targets bind the Fc portion of the antibodies and thus are 'coated' by the triggering antibody. The antigen-binding portion of the antibody then binds the specific NK cell–activating receptor and thereby triggers cytotoxicity. These target cells were lysed only in the presence of the triggering antibody and only if the NK cell expressed the appropriate receptor on the surface. Lytic units per 1 × 106 cells were calculated on the basis of 20% cytotoxicity.
Cell stimulation and immunoblot assays.
Vaccinia infection of NK cells, cell stimulation, protein immunoprecipitation and detection of tyrosine phosphorylation were done as described23.
GST fusion proteins.
For construction of GST.DAP10, amino acids 73–92 of DAP10 were cloned into the pGEX-KG cloning vector using PCR and standard molecular biology techniques. For construction of GST.Grb2-SH3-C, amino acids 151–217 of Grb2 were cloned into the pGEX-KG cloning vector by standard molecular biology techniques. GST.DAP10-Y85F, GST.DAP10-N87Q and GST.DAP10-M88Q either were cloned from the pSP11 constructs generated as described above or were mutated in the pGEX-KG vector by site-directed mutagenesis as described above. The pGEX-KG vectors were then cloned into BL21 competent cells (for nonphosphorylated proteins) or TKB1 competent cells (for phosphorylated proteins; both from Stratagene). GST proteins were purified over glutathione-agarose columns and were stored in 50% (volume/volume) glycerol at −20 °C. For phosphorylated proteins, 184 μg/ml of sodium orthovanadate was also added. All constructs were sequenced and verified for accuracy, and all fusion proteins were checked for purity by SDS-PAGE and Coomassie staining.
GST protein precipitation.
For association of DAP10 with Grb2 or p85, 1.4 × 108 NK cells were lysed on ice for 15 min in 7 ml of buffer containing 50 mM Tris, 20 mM EDTA and 1% (volume/volume) Nonidet-P40, pH 8.0. Cellular debris were removed by centrifugation at 20,800g for 5 min at 4 °C. The lysate was then divided into 1-ml aliquots and was added to 20 μg of a GST fusion protein bound to glutathione-agarose beads. Fusion proteins and lysates were rotated at 4 °C for a period of 30 min to overnight and then protein complexes were eluted with 40 μl SDS sample buffer, were resolved by SDS-PAGE and were transferred to Immobilon-P membranes (Millipore). Specific proteins were detected with primary antibodies followed by goat-anti mouse IgG coupled to horseradish peroxidase (Santa Cruz Biotechnology) and were visualized with the Super Signal detection system (Pierce Biotechnology). Optical density was determined by measurement of band darkness and subtraction of the background darkness of an equal area directly below the band.
For detection of the Grb2-Vav1 interaction, 2 × 107 Jurkat T cells infected for 3 h with recombinant vaccinia (multiplicity of infection, 10:1) encoding F.Vav1-WT or F.Vav1-P657A were lysed in 2 ml Nonidet-P40 buffer and were centrifuged as described above, were divided into 1-ml aliquots and were immunoprecipitated for 1 h with anti-Flag bound to goat anti-mouse agarose beads. Beads were washed thoroughly and then 5 μg of a GST fusion protein was added, followed by rotation at 4 °C overnight. After another thorough washing, protein complexes were eluted, resolved and detected as described above.
Protein-protein immunoblot analysis.
Jurkat T cells (3.5 × 107) infected for 3 h with recombinant vaccinia virus (multiplicity of infection, 10:1) encoding F.Grb2 were lysed for 10 min on ice in 350 μl of a solution of 10 mM Tris base, 50 mM NaCl, 5 mM EDTA, 50 mM NaF, 30 mM Na2P2O7 and 1% (volume/volume) Triton-X100, pH 7.4. Cellular debris were removed by centrifugation as described above and lysate was added to 175 μl SDS sample buffer. Equal amounts of lysate were loaded onto seven different lanes and were resolved by SDS-PAGE. After transfer of proteins onto membranes, individual lanes were separated and were simultaneously blotted with 4 μg/ml of a GST fusion protein in 50 mM Tris HCl, 150 mM NaCl, 0.1% (volume/volume) Tween, 2% (weight/volume) BSA and 0.05% (weight/volume) sodium azide, pH 7.4. Overnight incubation with the GST fusion protein solution was followed by incubation with an anti-GST solution and then goat anti-mouse IgG coupled to horseradish peroxidase. Individual bands were visualized as described above.
Grb2 suppression.
The following Grb2-specific siRNA construct was obtained from Dharmacon: 5′-TCAGCCAATTTGTCTCCTA-3′. On day 4 after passage, actively dividing NK cells were 'nucleofected' using the Amaxa Cell Line Kit V, program O-17. NK clones (4 × 106) were nucleofected with 300 pmol of negative control siRNA (AF488, Qiagen) or Grb2 siRNA and then were resuspended at a density of 7 × 105 cells/ml in RPMI medium (Invitrogen) plus 10% human serum, 1% L-glutamine (Mediatech), 1% sodium pyruvate (Invitrogen) and 10 U/ml of interleukin 2 (Chiron). Typically, nucleofection results in 50% cell death with a nucleofection efficiency of about 80% in the viable cells. Relative Grb2 suppression was determined by cell lysis, immunoblot and densitometry.
Statistics.
In cytotoxicity assays in which the percent 51Cr release is plotted, error bars represent s.d. of triplicate wells. Where lytic units are plotted, error bars represent s.d. obtained from nonlinear regression analysis to the exponential fit y = A × (1 − e−kx) as described51.
Note: Supplementary information is available on the Nature Immunology website.
References
Lanier, L.L. NK cell recognition. Annu. Rev. Immunol. 23, 225–274 (2005).
Bauer, S. et al. Activation of NK cells and T cells by NKG2D, a receptor for stress-inducible MICA. Science 285, 727–729 (1999).
Cerwenka, A. et al. Retinoic acid early inducible genes define a ligand family for the activating NKG2D receptor in mice. Immunity 12, 721–727 (2000).
Gasser, S., Orsulic, S., Brown, E.J. & Raulet, D.H. The DNA damage pathway regulates innate immune system ligands of the NKG2D receptor. Nature 436, 1186–1190 (2005).
Smyth, M.J. et al. NKG2D function protects the host from tumor initiation. J. Exp. Med. 202, 583–588 (2005).
Takaki, R. et al. IL-21 enhances tumor rejection through a NKG2D-dependent mechanism. J. Immunol. 175, 2167–2173 (2005).
Zhou, H. et al. DNA-based vaccines activate innate and adaptive antitumor immunity by engaging the NKG2D receptor. Proc. Natl. Acad. Sci. USA 102, 10846–10851 (2005).
Ogasawara, K., Benjamin, J., Takaki, R., Phillips, J.H. & Lanier, L.L. Function of NKG2D in natural killer cell-mediated rejection of mouse bone marrow grafts. Nat. Immunol. 6, 938–945 (2005).
Groh, V. et al. Costimulation of CD8alphabeta T cells by NKG2D via engagement by MIC induced on virus-infected cells. Nat. Immunol. 2, 255–260 (2001).
Meresse, B. et al. Coordinated induction by IL15 of a TCR-independent NKG2D signaling pathway converts CTL into lymphokine-activated killer cells in celiac disease. Immunity 21, 357–366 (2004).
Wu, J. et al. An activating immunoreceptor complex formed by NKG2D and DAP10. Science 285, 730–732 (1999).
Rosen, D.B. et al. A structural basis for the association of DAP12 with mouse, but not human, NKG2D. J. Immunol. 173, 2470–2478 (2004).
Billadeau, D.D., Upshaw, J.L., Schoon, R.A., Dick, C.J. & Leibson, P.J. NKG2D–DAP10 triggers human NK cell-mediated killing via a Syk-independent regulatory pathway. Nat. Immunol. 4, 557–564 (2003).
Zompi, S. et al. NKG2D triggers cytotoxicity in mouse NK cells lacking DAP12 or Syk family kinases. Nat. Immunol. 4, 565–572 (2003).
Garrity, D., Call, M.E., Feng, J. & Wucherpfennig, K.W. The activating NKG2D receptor assembles in the membrane with two signaling dimers into a hexameric structure. Proc. Natl. Acad. Sci. USA 102, 7641–7646 (2005).
Chang, C. et al. Cutting edge: KAP10, a novel transmembrane adapter protein genetically linked to DAP12 but with unique signaling properties. J. Immunol. 163, 4651–4654 (1999).
Nishida, M. et al. Novel recognition mode between Vav and Grb2 SH3 domains. EMBO J. 20, 2995–3007 (2001).
Ogura, K. et al. Solution structure of N-terminal SH3 domain of Vav and the recognition site for Grb2 C-terminal SH3 domain. J. Biomol. NMR 22, 37–46 (2002).
Ramos-Morales, F. et al. The proline-rich region of Vav binds to Grb2 and Grb3–3. Oncogene 11, 1665–1669 (1995).
Songyang, Z. et al. SH2 domains recognize specific phosphopeptide sequences. Cell 72, 767–778 (1993).
Kim, H.H., Tharayil, M. & Rudd, C.E. Growth factor receptor-bound protein 2 SH2/SH3 domain binding to CD28 and its role in co-signaling. J. Biol. Chem. 273, 296–301 (1998).
Skolnik, E.Y. et al. The SH2/SH3 domain-containing protein GRB2 interacts with tyrosine-phosphorylated IRS1 and Shc: implications for insulin control of ras signalling. EMBO J. 12, 1929–1936 (1993).
Upshaw, J.L., Schoon, R.A., Dick, C.J., Billadeau, D.D. & Leibson, P.J. The isoforms of phospholipase C-gamma are differentially used by distinct human NK activating receptors. J. Immunol. 175, 213–218 (2005).
Yang, W.C., Ching, K.A., Tsoukas, C.D. & Berg, L.J. Tec kinase signaling in T cells is regulated by phosphatidylinositol 3-kinase and the Tec pleckstrin homology domain. J. Immunol. 166, 387–395 (2001).
Stork, B. et al. Grb2 and the non-T cell activation linker NTAL constitute a Ca(2+)-regulating signal circuit in B lymphocytes. Immunity 21, 681–691 (2004).
Cella, M. et al. Differential requirements for Vav proteins in DAP10- and ITAM-mediated NK cell cytotoxicity. J. Exp. Med. 200, 817–823 (2004).
August, A. & Dupont, B. CD28 of T lymphocytes associates with phosphatidylinositol 3-kinase. Int. Immunol. 6, 769–774 (1994).
Truitt, K.E., Hicks, C.M. & Imboden, J.B. Stimulation of CD28 triggers an association between CD28 and phosphatidylinositol 3-kinase in Jurkat T cells. J. Exp. Med. 179, 1071–1076 (1994).
Prasad, K.V. et al. T-cell antigen CD28 interacts with the lipid kinase phosphatidylinositol 3-kinase by a cytoplasmic Tyr(P)-Met-Xaa-Met motif. Proc. Natl. Acad. Sci. USA 91, 2834–2838 (1994).
Schneider, H., Cai, Y.C., Prasad, K.V., Shoelson, S.E. & Rudd, C.E. T cell antigen CD28 binds to the GRB-2/SOS complex, regulators of p21ras. Eur. J. Immunol. 25, 1044–1050 (1995).
Geldhof, A.B. et al. Expression of B7–1 by highly metastatic mouse T lymphomas induces optimal natural killer cell-mediated cytotoxicity. Cancer Res. 55, 2730–2733 (1995).
Yeh, K.Y. et al. B7–1 enhances natural killer cell-mediated cytotoxicity and inhibits tumor growth of a poorly immunogenic murine carcinoma. Cell. Immunol. 165, 217–224 (1995).
Hunter, C.A. et al. The role of the CD28/B7 interaction in the regulation of NK cell responses during infection with Toxoplasma gondii. J. Immunol. 158, 2285–2293 (1997).
Azuma, M., Cayabyab, M., Buck, D., Phillips, J.H. & Lanier, L.L. Involvement of CD28 in MHC-unrestricted cytotoxicity mediated by a human natural killer leukemia cell line. J. Immunol. 149, 1115–1123 (1992).
Galea-Lauri, J. et al. Expression of a variant of CD28 on a subpopulation of human NK cells: implications for B7-mediated stimulation of NK cells. J. Immunol. 163, 62–70 (1999).
Wilson, J.L. et al. NK cell triggering by the human costimulatory molecules CD80 and CD86. J. Immunol. 163, 4207–4212 (1999).
Lang, S., Vujanovic, N.L., Wollenberg, B. & Whiteside, T.L. Absence of B7.1–CD28/CTLA-4-mediated co-stimulation in human NK cells. Eur. J. Immunol. 28, 780–786 (1998).
Goodier, M.R. & Londei, M. CD28 is not directly involved in the response of human CD3- CD56+ natural killer cells to lipopolysaccharide: a role for T cells. Immunology 111, 384–390 (2004).
Sada, K., Zhang, J. & Siraganian, R.P. SH2 domain-mediated targeting, but not localization, of Syk in the plasma membrane is critical for FcepsilonRI signaling. Blood 97, 1352–1359 (2001).
Ehrlich, L.I. et al. Engagement of NKG2D by cognate ligand or antibody alone is insufficient to mediate costimulation of human and mouse CD8+ T cells. J. Immunol. 174, 1922–1931 (2005).
Ho, E.L. et al. Costimulation of multiple NK cell activation receptors by NKG2D. J. Immunol. 169, 3667–3675 (2002).
Jamieson, A.M. et al. The role of the NKG2D immunoreceptor in immune cell activation and natural killing. Immunity 17, 19–29 (2002).
Maasho, K., Opoku-Anane, J., Marusina, A.I., Coligan, J.E. & Borrego, F. NKG2D is a costimulatory receptor for human naive CD8+ T cells. J. Immunol. 174, 4480–4484 (2005).
Markiewicz, M.A. et al. Costimulation through NKG2D enhances murine CD8+ CTL function: similarities and differences between NKG2D and CD28 costimulation. J. Immunol. 175, 2825–2833 (2005).
Windebank, K.P. et al. Signal transduction during human natural killer cell activation: inositol phosphate generation and regulation by cyclic AMP. J. Immunol. 141, 3951–3957 (1988).
Ting, A.T., Karnitz, L.M., Schoon, R.A., Abraham, R.T. & Leibson, P.J. Fc gamma receptor activation induces the tyrosine phosphorylation of both phospholipase C (PLC)-γ1 and PLC-γ2 in natural killer cells. J. Exp. Med. 176, 1751–1755 (1992).
Binstadt, B.A. et al. SLP-76 is a direct substrate of SHP-1 recruited to killer cell inhibitory receptors. J. Biol. Chem. 273, 27518–27523 (1998).
Billadeau, D.D., Mackie, S.M., Schoon, R.A. & Leibson, P.J. The Rho family guanine nucleotide exchange factor Vav-2 regulates the development of cell-mediated cytotoxicity. J. Exp. Med. 192, 381–392 (2000).
Billadeau, D.D. et al. The Vav-Rac1 pathway in cytotoxic lymphocytes regulates the generation of cell-mediated killing. J. Exp. Med. 188, 549–559 (1998).
Billadeau, D.D., Mackie, S.M., Schoon, R.A. & Leibson, P.J. Specific subdomains of Vav differentially affect T cell and NK cell activation. J. Immunol. 164, 3971–3981 (2000).
Rubin, P., Pross, H.F. & Roder, J.C. Studies of human natural killer cells. II. Analysis at the single cell level. J. Immunol. 128, 2553–2558 (1982).
Acknowledgements
We thank E. Leof (Mayo Clinic College of Medicine, Rochester, Minnesota) for providing a human p85α construct, and R.T. Abraham (Wyeth Research, Pearl River, New York) for providing the Jurkat cells and the signaling-defective Jurkat 'sublines'. Supported by the Mayo Foundation and the National Institutes of Health (CA-47752 to P.J.L.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Figure 1
DAP10 recruitment of Grb2 upon NKG2D stimulation. (PDF 333 kb)
Supplementary Figure 2
Flag-tagged chimeric receptors with extracellular and transmembrane CD4 and the indicated cytoplasmic tails. (PDF 197 kb)
Supplementary Figure 3
Model of NKG2D-DAP10 coupling to downstream effectors. (PDF 222 kb)
Rights and permissions
About this article
Cite this article
Upshaw, J., Arneson, L., Schoon, R. et al. NKG2D-mediated signaling requires a DAP10-bound Grb2-Vav1 intermediate and phosphatidylinositol-3-kinase in human natural killer cells. Nat Immunol 7, 524–532 (2006). https://doi.org/10.1038/ni1325
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni1325
This article is cited by
-
Leveraging CD16 fusion receptors to remodel the immune response for enhancing anti-tumor immunotherapy in iPSC-derived NK cells
Journal of Hematology & Oncology (2023)
-
Natural killer cells strengthen antitumor activity of cisplatin by immunomodulation and ameliorate cisplatin-induced side effects
International Urology and Nephrology (2023)
-
Chimeric antigen receptor- and natural killer cell receptor-engineered innate killer cells in cancer immunotherapy
Cellular & Molecular Immunology (2021)
-
Natural killer group 2D receptor and its ligands in cancer immune escape
Molecular Cancer (2019)
-
Hexamethylene bisacetamide impairs NK cell-mediated clearance of acute T lymphoblastic leukemia cells and HIV-1-infected T cells that exit viral latency
Scientific Reports (2019)