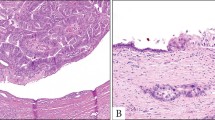
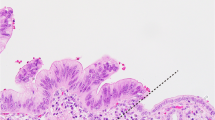
Abstract
Intraductal papillary mucinous neoplasia (IPMN) encompasses a spectrum of neoplastic change in the epithelial lining of the pancreatic duct. As such, it is difficult to predict the presence of malignancy, and pancreatic resection is established as the only effective treatment for IPMN. There is controversy about the natural history, evaluation, surgical management and surveillance of IPMN; as IPMN is being increasingly recognized, this controversy is being brought to the forefront of clinical practice. This review presents pooled surgical data, future directions and a proposed algorithm for the management of patients with IPMN.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Kloeppel G et al. (1996) World Health Organization international histological classification of tumors. In: Histological typing of tumours of the exocrine pancreas, 1–61 edn 2 Berlin: Springer-Verlag
Kimura W et al. (1998) Characteristics and treatment of mucin-producing tumor of the pancreas. Hepatogastroenterology 45: 2001–2008
Yamao K et al. (2000) The prognosis of intraductal papillary mucinous tumors of the pancreas. Hepatogastroenterology 47: 1129–1134
Ohhashi K et al. (1982) Four cases of a mucous secreting pancreatic cancer (in Japanese with English abstract). Prog Dig Endosc 20: 348–351
Tollefson MK et al. (2003) Intraductal papillary mucinous neoplasm: did it exist prior to 1980? Pancreas 26: 55–58
Hruban RH et al. (2000) Progression model for pancreatic cancer. Clin Cancer Res 6: 2969–2972
Shyr YM et al. (1996) Mucin-producing neoplasms of the pancreas. Intraductal papillary and mucinous cystic neoplasms. Ann Surg 223: 141–146
Obara T et al. (1991) Mucin-producing tumor of the pancreas: a unique clinical entity. Am J Gastroenterol 86: 1619–1625
Kubo H et al. (2001) Intraductal papillary-mucinous tumors of the pancreas: differential diagnosis between benign and malignant tumors by endoscopic ultrasonography. Am J Gastroenterol 96: 1429–1434
Tanaka M (2004) Intraductal papillary mucinous neoplasm of the pancreas: diagnosis and treatment. Pancreas 28: 282–288
Hara T et al. (2002) Diagnosis and patient management of intraductal papillary-mucinous tumor of the pancreas by using peroral pancreatoscopy and intraductal ultrasonography. Gastroenterology 122: 34–43
Procacci C et al. (2001) Intraductal papillary mucinous tumors of the pancreas: spectrum of CT and MR findings with pathologic correlation. Eur Radiol 11: 1939–1951
Koito K et al. (1998) Mucin-producing pancreatic tumors: comparison of MR cholangiopancreatography with endoscopic retrograde cholangiopancreatograpy. Radiology 208: 231–237
Aithal GP et al. (2002) Accuracy of EUS for detection of intraductal papillary mucinous tumor of the pancreas. Gastrointest Endosc 56: 701–707
Brandwein SL et al. (2001) Detection and tumor staging of malignancy in cystic, intraductal, and solid tumors of the pancreas by EUS. Gastrointest Endosc 53: 722–727
D'Angelica M et al. (2004) Intraductal papillary mucinous neoplasms of the pancreas: an analysis of clincopathologic features and outcome. Ann Surg 239: 400–408
Salvia R et al. (2004) Main-duct intraductal papillary mucinous neoplasms of the pancreas: clinical predictors of malignancy and long-term survival following resection. Ann Surg 239: 678–685
Sohn TA et al. (2004) Intraductal papillary mucinous neoplasms of the pancreas: an updated experience. Ann Surg 239: 788–797
Wiesenauer CA et al. (2003) Preoperative predictors of malignancy in pancreatic intraductal papillary mucinous neoplasms. Arch Surg 138: 610–617
Irie H et al. (2004) Natural history of pancreatic intraductal papillary mucinous tumor of branch duct type: follow-up study by magnetic resonance cholangiopancreatography. J Comput Assist Tomogr 28: 117–122
Bernard P et al. (2002) Intraductal papillary mucinous tumors of the pancreas: predictive criteria of malignancy according to pathologic examination of 53 cases. Arch Surg 137: 1274–1278
Khalid A et al. (2004) First hit K-ras point mutation followed by tumor suppressor gene allelic loss predicts malignancy in EUS guided pancreatic cyst aspirate. Pancreas 29: 357 [abstract]
Schoedel KE et al. (2005) K-ras and microsatellite marker analysis of fine needle aspirates from intraductal papillary mucinous neoplasms of the pancreas. Mod Pathol 18 (Suppl): 77 [abstract]
Acknowledgements
The authors thank Terri Wetmore for her assistance in the preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Glossary
- AMPULLARY STENOSIS
-
Fibrosis or scarring of the pancreatic sphincter that can lead to increased resistance to the flow of pancreatic juice, resulting in pancreatic duct dilation
- MAGNETIC RESONANCE CHOLANGIOPANCREATOGRAPHY (MRCP)
-
MRI of the biliary tree and pancreatic duct system
- ENDOSCOPIC ULTRASONOGRAPHY (EUS)
-
A staging and diagnostic technique performed via an ultrasound probe mounted at the tip of an endoscope
- ENDOSCOPIC RETROGRADE CHOLANGIOPANCREATOGRAPHY (ERCP)
-
Endoscopic technique of injecting contrast dye into the ampulla of Vater for radiologic visualization of the pancreatic and biliary ducts
Rights and permissions
About this article
Cite this article
McGrath, K., Slivka, A. Diagnosis and management of intraductal papillary mucinous neoplasia. Nat Rev Gastroenterol Hepatol 2, 316–322 (2005). https://doi.org/10.1038/ncpgasthep0213
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpgasthep0213
This article is cited by
-
The Endoscopist's Influence on Endoscopic Test Characteristics
American Journal of Gastroenterology (2011)
-
Technology Insight: applications of MRI for the evaluation of benign disease of the pancreas
Nature Clinical Practice Gastroenterology & Hepatology (2007)