Abstract
Aims
To assess the correlation between macular morphology and visual acuity in retinitis pigmentosa (RP) patients with cystoid macular oedema (CME).
Design
Retrospective cross-sectional study.
Patients and methods
Forty-one eyes of 25 RP patients with CME. Patients underwent cross-sectional scans with optical coherence tomography (Stratus OCT). Age, total retinal thickness, photoreceptor thickness, and the transverse and vertical lengths of the cystoid space were measured. Correlation between visual acuity and each of the measurements were examined. Additionally, the status of the inner segment/outer segment junction (IS/OS) was classified as being absent, discontinuous, or distinct. Measurements were then compared among the three groups.
Results
Total retinal thickness or photoreceptor thickness was not correlated with visual acuity. There was a correlation between the transverse length of the cystoid space and visual acuity, although the correlation coefficient was weak (r=0.30). The logMAR visual acuity in the IS/OS absent group (0.67±0.43) was worse than that seen in the IS/OS discontinuous (0.22±0.19) or IS/OS distinct groups (0.07±0.16) (P<0.001).
Conclusions
When monitoring CME associated with RP, the status of IS/OS is the essential parameter that needs to be examined.
Similar content being viewed by others
Introduction
Cystoid macular oedema (CME) is a common complication of retinitis pigmentosa (RP) and can compromise the visual acuity of RP patients even in the less advanced stages. Several therapies are used to treat CME in RP patients and include topical or oral administration of carbonic anhydrase inhibitor,1, 2, 3, 4 periocular or intravitreal injection of steroid,5, 6, 7, 8, 9 intravitreal injection of bevacizumab,10 photocoagulation,11, 12 or vitrectomy.13 Although each of these therapeutic measures provides a benefit for some of the patients, there is little information on the pathophysiology, prevalence, or natural course of CME that is associated with RP. Furthermore, because of the nature of the pathological and clinical characteristics of RP, it can be quite difficult to assess the involvement of CME in the visual impairment of RP patients as compared to that for other retinal vascular diseases.
Optical coherence tomography (OCT) is now widely used to study retinal pathologies and has also been used for the diagnosis and monitoring of RP. The OCT device is safe and has been shown to be more sensitive or at least as sensitive as fluorescein angiography when detecting CME in RP.14, 15, 16 Meanwhile, owing to imaging resolution limitations, the parameters that are used to monitor CME have been limited to the retinal thickness or the size of the cystoid space.
In addition to examining the retinal thickness or the gross morphologic changes, a recent OCT model has made it possible to obtain a much more detailed evaluation of the retinal layer, which includes the third high reflectance band. This third high reflectance band is depicted as the outer boundary of the retina, and it has been suggested that it represents the photoreceptor inner segment/outer segment junction (IS/OS).17 As OCT can observe the status of IS/OS, it has been used to study various aetiologies, including those of central serous chorioretinopathy,18, 19, 20 retinal vein occlusion,21, 22, 23 macular hole,24 retinal detachment,25 and multiple evanescent white dot syndrome.26 All of the reports have consistently shown that the status of IS/OS is closely correlated with the visual function and/or the pathological change.
To investigate whether OCT can be used for better assessment of CME in RP patients, we performed a detailed evaluation of the retinal measures. We examined IS/OS in the fovea as well as the size of the cystoid space, the total retinal thickness, and the photoreceptor layer thickness. We also investigated which of these measures were best correlated with visual acuity.
Patients and methods
Clinical records of 652 eyes of 326 RP patients who underwent macular scanning with OCTs (Stratus model 3000, Carl-Zeiss, Dublin, CA, USA; OCT ophthalmoscope C7, Nidek, Gamagori, Japan; or 3D-OCT 1000 Topcon, Tokyo, Japan) at Kyoto University Hospital between September 2004 and October 2007 were retrospectively reviewed. Diagnosis of RP was made by the presence of night blindness, characteristic fundus appearance, visual field defect, and a subnormal or non-recordable electroretinogram. CME was confirmed in 49 eyes of 30 patients, and those examined with Stratus OCT (41 eyes of 25 patients) were included in the study. Another 48 eyes had cystoid space elsewhere than the foveola (Figure 1) but were not included in the study, as the lesion was unlikely to affect visual acuity.
OCT images of the eyes included at the initial examination were further analysed as has been reported.21 Briefly, we measured total foveal thickness, the transverse and vertical lengths of the foveal cystoid space, and the photoreceptor layer thickness (Figure 2). Total foveal thickness was defined as the distance between the vitreoretinal interface and the retinal pigment epithelium, whereas the photoreceptor layer thickness was defined as the distance between the posterior surface of the cystoid space and the pigment epithelium. The transverse lengths of the cystoid spaces were determined in such a way as to include all of the cystoid spaces within the image. The status of the foveal IS/OS was further divided into distinct, blurred/discontinuous, and absent groups. The definition of IS/OS was determined using monochromatic images (Figure 3). One of the authors who was unaware of the patients' visual acuity or any other clinical information performed all of the measurements.
Statistical analysis
The statistical program SPSS was used to analyse the sample data.
Descriptive analyses are reported as means±SD unless otherwise specified. Visual acuities were measured with Landolt C and were converted to the logarithm of the minimum angle of resolution (logMAR) equivalents. Bivariate relationships were examined using Pearson's correlation coefficient. Measurement values of the three groups that were classified on the basis of the status of IS/OS were compared using an analysis of variance, with post hoc comparisons tested by the Bonferroni procedure. When the P-value was less than 0.05, this was taken to indicate a significant statistical difference.
Results
We first reviewed the clinical records of 652 eyes of 326 RP patients, with CME identified in 49 eyes. In addition, we found that other macular pathologies existed frequently in the patients, including epiretinal membrane (ERM, 126 eyes), choroidal neovascular membrane-like lesion (four eyes), macular hole (one eye), and retinoschisis (two eyes).
Subsequently, we examined patients with CME. Demographics of the patients are shown in Table 1. The average age of the patients was 44.0±17.1 years and the average logMAR was 0.30±0.35. Gender preponderance was not evident and it was not clear how long the patients had had CME. Bilateral involvement was seen in 16 patients and nine patients had unilateral CME. There was an autosomal dominant inheritance pattern in five patients, an autosomal recessive pattern in five patients, and there were 15 sporadic patients. ERM was found in 11 eyes, whereas 30 eyes did not have ERM detectable with OCT.
The correlation between visual acuity and each measurement is shown in Table 2. No correlations between visual acuity and age, vertical length of the cystoid space, total foveal thickness, and photoreceptor thickness were noted. Although the transverse length of the cystoid space did show a statistical significance, the correlation coefficient was weak (r=0.30, P=0.03).
To further assess the influence of IS/OS on visual acuity, the eyes were divided into absent, discontinuous, and distinct groups based on the status of IS/OS. Table 3 shows the demographics for each of the groups. Although the patients belong to IS/OS distinct group tended to be younger and have smaller cystoid spaces, there was no significant difference in age, total thickness, and the size of the cystoid space among the three groups. In the IS/OS absent group, the photoreceptor layer was thinner as compared with the IS/OS distinct group, and in addition the logMAR visual acuity was worse than that seen for the other two groups. In fact, the logMAR of the IS/OS distinct group was 0.07, which was much better than the 0.67 value of the IS/OS absent group.
Discussion
In this study, foveal thickness, photoreceptor layer thickness, and the vertical length of the cystoid space exhibited no correlation with visual acuity. Although the transverse length of the cystoid space affected visual acuity, the correlation coefficient was weak. However, it should be noted that IS/OS was the most significant factor for visual acuity in RP patients with CME.
Some authors have reported earlier a negative correlation between visual acuity and foveal thickness3 or the transverse length of the cystoid space.16 In contrast to these previous papers, this study found no factors that had any correlation, weak or otherwise, with visual acuity. We assume that the difference lies partly in the selection of patients between various studies. The report by Chung et al3 was primarily conducted to examine the effect of acetazolamide, and thus might have included patients with conditions that were much more severe. Our study included patients with CME, regardless of the extent of oedema or visual acuity, and therefore our study population might have consisted of a group of patients with less severe conditions. The study of Hirakawa et al16 was conducted using OCT 2000, which is an earlier version, and thus may partly explain the differing results.
In RP patients without CME, IS/OS has been shown to be correlated with visual acuity.27 We also showed in an earlier study that the shortening or disappearance of IS/OS was associated with the deterioration of visual acuity and the amplitude of the focal macular electroretinogram.28 In this study, the status of IS/OS was correlated with visual acuity similar to that seen for the cases without CME. The IS/OS absent group had a thinner photoreceptor layer, and therefore these factors might very well have been confounded. However, the photoreceptor layer thickness was not an independent factor for visual acuity, and thus we consider the confounding effect to have been minimal.
Concerning the prevalence of CME in RP patients, a very recent article has reported that up to 49% of patients with a moderate stage of RP had CME.29 However, in this study, the prevalence rate of CME was only 49 out of a total of 652 eyes, that is, 7.5%. This is far fewer than has been reported earlier. In addition, these other studies have all reported similar prevalence rates that ranged from 10 to 15%.27, 30 As this study included non-consecutive and non-population-based data, we were not able to determine the exact prevalence rate, although it is unlikely that the frequency of CME would be as high as 40% in our population. One possible explanation for these differences might very well be how CME was defined. In this study, we observed 48 eyes that had small cystoid spaces that were found elsewhere than in the foveola without foveal thickening (Figure 1). These eyes were not included in this study, as it was assumed that they would not affect visual acuity. If, in fact, we were to count these patients, the frequency of CME would be doubled. Another possible reason for the differences observed might be related to the phenotypic difference seen for the different patient cohorts. The genetics of RP patients are complex, with more than 45 genes having been identified in RP patients. However, in about 40% of the patients, it is still unclear as to what the causative genes are.31 Additionally, the distribution of the causative genes and the phenotypic patterns noted are quite possibly different in a Japanese patient cohort.
Although there is a possibility that ERM impairs visual acuity in RP patients, we did not exclude eyes with ERM from the analysis. The ERM seen in the population was not all that severe, and therefore we did not think that it would affect the visual acuity. In addition, because ERM was a common complication within the studied population, by excluding all these patients with ERM, it would lessen the clinical implications that might possibly be obtained from this study. The exact influence of ERM on visual acuity or the formation of CME should be elucidated in further studies.
The limitation of the image-based definition should be kept in mind. The patients were divided into three groups based on the appearance of OCT images. Although the grouping was made in blinded fashion and the result was well correlated with visual acuity, the process was essentially subjective. Quantitative parameters, for example, length, area, or signal intensity, would enable more objective assessments. It should also be noted that exactly what IS/OS represents remains to be elucidated.
Another limitation of this study involves the examination device. The OCT device that was used in our study was much better than the previous versions, but it is not the latest one that is currently available. Resolution of the Stratus OCT is still limited to 10 μm and it is inferior to the next generation spectral-domain OCT, which has resolutions as high as 2.5 μm. Thus, with more detailed observations using the latest OCT, this might have helped us to better elucidate the pathology and provide a better understanding of CME in RP patients.32
In conclusion, we investigated the correlation between macular morphology and visual acuity in the CME in RP patients. Although in general, there is a correlation between central macular thickness and visual acuity in various pathologies, but in this study, this relationship was less evident in the RP patients as compared with previous reports.16, 33 In fact, we found that all measurements other than the IS/OS status were not distinct factors involved with visual acuity. Thus, when monitoring CME associated with RP, the IS/OS status should be the designated parameter that is used rather than either the foveal thickness or the size of the cystoid space.
References
Wolfensberger TJ . The role of carbonic anhydrase inhibitors in the management of macular edema. Doc Ophthalmol 1999; 97 (3–4): 387–397.
Grover S, Apushkin MA, Fishman GA . Topical dorzolamide for the treatment of cystoid macular edema in patients with retinitis pigmentosa. Am J Ophthalmol 2006; 141 (5): 850–858.
Chung H, Hwang JU, Kim JG, Yoon YH . Optical coherence tomography in the diagnosis and monitoring of cystoid macular edema in patients with retinitis pigmentosa. Retina 2006; 26 (8): 922–927.
Fishman GA, Apushkin MA . Continued use of dorzolamide for the treatment of cystoid macular oedema in patients with retinitis pigmentosa. Br J Ophthalmol 2007; 91 (6): 743–745.
Saraiva VS, Sallum JM, Farah ME . Treatment of cystoid macular edema related to retinitis pigmentosa with intravitreal triamcinolone acetonide. Ophthalmic Surg Lasers Imaging 2003; 34 (5): 398–400.
Ozdemir H, Karacorlu M, Karacorlu S . Intravitreal triamcinolone acetonide for treatment of cystoid macular oedema in patients with retinitis pigmentosa. Acta Ophthalmol Scand 2005; 83 (2): 248–251.
Kim JE . Intravitreal triamcinolone acetonide for treatment of cystoid macular edema associated with retinitis pigmentosa. Retina 2006; 26 (9): 1094–1096.
Wang C, Hu J, Bernstein PS, Teske MP, Payne M, Yang Z et al. Intravitreal injection of triamcinolone acetonide for macular edema due to retinitis pigmentosa and other retinal diseases. Adv Exp Med Biol 2006; 572: 309–314.
Scorolli L, Morara M, Meduri A, Reggiani LB, Ferreri G, Scalinci SZ et al. Treatment of cystoid macular edema in retinitis pigmentosa with intravitreal triamcinolone. Arch Ophthalmol 2007; 125 (6): 759–764.
Melo GB, Farah ME, Aggio FB . Intravitreal injection of bevacizumab for cystoid macular edema in retinitis pigmentosa. Acta Ophthalmol Scand 2007; 85 (4): 461–463.
Newsome DA, Blacharski PA . Grid photocoagulation for macular edema in patients with retinitis pigmentosa. Am J Ophthalmol 1987; 103 (2): 161–166.
Heckenlively JR . Grid photocoagulation for macular edema in patients with retinitis pigmentosa. Am J Ophthalmol 1987; 104 (1): 94–95.
Garcia-Arumi J, Martinez V, Sararols L, Corcostegui B . Vitreoretinal surgery for cystoid macular edema associated with retinitis pigmentosa. Ophthalmology 2003; 110 (6): 1164–1169.
Apushkin MA, Fishman GA, Janowicz MJ . Monitoring cystoid macular edema by optical coherence tomography in patients with retinitis pigmentosa. Ophthalmology 2004; 111 (10): 1899–1904.
Stanga PE, Downes SM, Ahuja RM, Chong NH, Antcliff R, Reck AC et al. Comparison of optical coherence tomography and fluorescein angiography in assessing macular edema in retinal dystrophies: preliminary results. Int Ophthalmol 2001; 23 (4–6): 321–325.
Hirakawa H, Iijima H, Gohdo T, Tsukahara S . Optical coherence tomography of cystoid macular edema associated with retinitis pigmentosa. Am J Ophthalmol 1999; 128 (2): 185–191.
Costa RA, Calucci D, Skaf M, Cardillo JA, Castro JC, Melo Jr LA et al. Optical coherence tomography 3: automatic delineation of the outer neural retinal boundary and its influence on retinal thickness measurements. Invest Ophthalmol Vis Sci 2004; 45 (7): 2399–2406.
Eandi CM, Chung JE, Cardillo-Piccolino F, Spaide RF . Optical coherence tomography in unilateral resolved central serous chorioretinopathy. Retina 2005; 25 (4): 417–421.
Piccolino FC, de la Longrais RR, Ravera G, Eandi CM, Ventre L, Abdollahi A et al. The foveal photoreceptor layer and visual acuity loss in central serous chorioretinopathy. Am J Ophthalmol 2005; 139 (1): 87–99.
Ojima Y, Hangai M, Sasahara M, Gotoh N, Inoue R, Yasuno Y et al. Three-dimensional imaging of the foveal photoreceptor layer in central serous chorioretinopathy using high-speed optical coherence tomography. Ophthalmology 2007; 114 (12): 2197–2207.
Ota M, Tsujikawa A, Murakami T, Yamaike N, Sakamoto A, Kotera Y et al. Foveal photoreceptor layer in eyes with persistent cystoid macular edema associated with branch retinal vein occlusion. Am J Ophthalmol 2008; 145 (2): 273–280.
Ota M, Tsujikawa A, Murakami T, Kita M, Miyamoto K, Sakamoto A et al. Association between integrity of foveal photoreceptor layer and visual acuity in branch retinal vein occlusion. Br J Ophthalmol 2007; 91 (12): 1644–1649.
Murakami T, Tsujikawa A, Ohta M, Miyamoto K, Kita M, Watanabe D et al. Photoreceptor status after resolved macular edema in branch retinal vein occlusion treated with tissue plasminogen activator. Am J Ophthalmol 2007; 143 (1): 171–173.
Scholda C, Wirtitsch M, Hermann B, Unterhuber A, Ergun E, Sattmann H et al. Ultrahigh resolution optical coherence tomography of macular holes. Retina 2006; 26 (9): 1034–1041.
Schocket LS, Witkin AJ, Fujimoto JG, Ko TH, Schuman JS, Rogers AH et al. Ultrahigh-resolution optical coherence tomography in patients with decreased visual acuity after retinal detachment repair. Ophthalmology 2006; 113 (4): 666–672.
Nguyen MH, Witkin AJ, Reichel E, Ko TH, Fujimoto JG, Schuman JS et al. Microstructural abnormalities in MEWDS demonstrated by ultrahigh resolution optical coherence tomography. Retina 2007; 27 (4): 414–418.
Sandberg MA, Brockhurst RJ, Gaudio AR, Berson EL . The association between visual acuity and central retinal thickness in retinitis pigmentosa. Invest Ophthalmol Vis Sci 2005; 46 (9): 3349–3354.
Oishi A, Nakamura H, Tatsumi I, Sasahara M, Kojima H, Kurimoto M et al. Optical coherence tomographic pattern and focal electroretinogram in patients with retinitis pigmentosa. Eye 2008. in press.
Adackapara CA, Sunness JS, Dibernardo CW, Melia BM, Dagnelie G . Prevalence of cystoid macular edema and stability in OCT retinal thickness in eyes with retinitis pigmentosa during a 48-week lutein trial. Retina 2008; 28 (1): 103–110.
Coscas G, Gaudric A . Natural course of nonaphakic cystoid macular edema. Surv Ophthalmol 1984; 28 (Suppl): 471–484.
Hartong DT, Berson EL, Dryja TP . Retinitis pigmentosa. Lancet 2006; 368 (9549): 1795–1809.
Witkin AJ, Ko TH, Fujimoto JG, Chan A, Drexler W, Schuman JS et al. Ultra-high resolution optical coherence tomography assessment of photoreceptors in retinitis pigmentosa and related diseases. Am J Ophthalmol 2006; 142 (6): 945–952.
Catier A, Tadayoni R, Paques M, Erginay A, Haouchine B, Gaudric A et al. Characterization of macular edema from various etiologies by optical coherence tomography. Am J Ophthalmol 2005; 140 (2): 200–206.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests: NoneFunding: None
Rights and permissions
About this article
Cite this article
Oishi, A., Otani, A., Sasahara, M. et al. Photoreceptor integrity and visual acuity in cystoid macular oedema associated with retinitis pigmentosa. Eye 23, 1411–1416 (2009). https://doi.org/10.1038/eye.2008.266
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2008.266
Keywords
This article is cited by
-
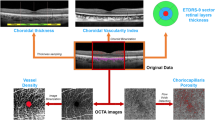
Characterizing macular edema in retinitis pigmentosa through a combined structural and microvascular optical coherence tomography investigation
Scientific Reports (2023)
-
Swept-source optical coherence tomography changes and visual acuity among Palestinian retinitis Pigmentosa patients: a cross-sectional study
BMC Ophthalmology (2021)
-
Impacts of intravitreal anti-VEGF therapy on retinal anatomy and neurophysiology in diabetic macular edema
International Ophthalmology (2021)
-
Short-term outcomes of subtenon triamcinolone acetonide injections in patients with retinitis pigmentosa-associated cystoid macular edema unresponsive to carbonic anhydrase inhibitors
International Ophthalmology (2020)
-
Demonstration of anatomical development of the human macula within the first 5 years of life using handheld OCT
International Ophthalmology (2019)