Abstract
Background/Objectives:
We aimed to assess the effects on mild morbidity of a richly micronutrient-fortified complementary/replacement food given to Zambian infants aged 6-18 months. Previous results (The Chilenje Infant Growth, Nutrition and Infection Study Team, 2010) showed an increase in the rate of hospital referral for pneumonia in the same cohort.
Subject/Methods:
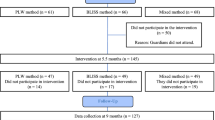
A total of 743 six-month-old healthy Zambian infants were randomised to receive either a richly or a basal micronutrient-fortified porridge for 12 months. Mild morbidity was defined as an illness that did not cause death or require hospitalisation and was diagnosed on clinical examination at scheduled visits.
Results:
There was no evidence of an effect of trial arm on overall mild morbidity during the study (odds ratio (OR)=1.04, 95% confidence interval (CI)=0.90, 1.20, P=0.62). Infants in the richly fortified arm had significantly more visits in which they were diagnosed with lower respiratory tract infections/pneumonia (OR=1.65, 95% CI=1.06, 2.59, P=0.03) and fewer visits in which a diagnosis of urinary tract infection was made (OR=0.43, 95% CI=0.21, 0.87, P=0.02). Maternally reported symptoms were similar between trial arms.
Conclusion:
Compared with the basal diet, the richly micronutrient-fortified food was associated with more episodes of lower respiratory infections/pneumonia diagnosed at scheduled visits, which reinforces our previously reported findings of a higher incidence in hospital referral for pneumonia.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Black RE, Allen LH, Bhutta ZA, Caulfield LE, de Onis M, Ezzati M et al. (2008). Maternal and child undernutrition: global and regional exposures and health consequences. Lancet 371, 243–260.
Dewey K, Brown K (2003). Update on technical issues concerning complementary feeding of young children in developing countries and implications for intervention programs. Special issue based on a World Health Organization expert consultation on complementary feeding. Food Nutr Bull 24: 5–28.
Head KA (2008). Natural approaches to prevention and treatment of infections of the lower urinary tract. Altern Med Rev 3, 227–244.
International Zinc Nutrition Consultative Group (2004). Assessment of the risk of zinc deficiency in populations and options for its control. Food Nutr Bull 25: 94S–203S.
Moody AH, Chiodini PL (2000). Methods for the detection of blood parasites. Clin Lab Haematol 22, 189–201.
Rabe-Hesketh S, Skrondal A (2008). Dichotomous or binary response. In: Rabe-Hesketh S, Skrondal A (eds). Multilevel and Longitudinal Modeling Using Stata, 2nd edn. Stata Press: College Station, TX, pp 231–285.
Sazawal S, Black RE, Ramsan M, Chwaya HM, Stoltzfus RJ, Dutta A et al. (2006). Effects of routine prophylactic supplementation with iron and folic acid on admission to hospital and mortality in preschool children in a high malaria transmission setting: Community-based, randomised, placebo-controlled trial. Lancet 367, 133–143.
The Chilenje Infant Growth, Nutrition and Infection (CIGNIS) Study Team (2010). Micronutrient fortification to improve growth and health of maternally HIV-unexposed and exposed Zambian infants: a randomised controlled trial. PloS One 5, e11165. http://www.plosone.org/article/info%3Adoi%2F10.1371%2Fjournal.pone.0011165.
Wang D, Fox D (2006). Repeated measurements. In: Wang D, Bakhai A (eds). Clinical Trials: A Practical Guide to Design, Analysis and Reporting. Remedica: London, UK, pp 317–328.
WHO (1998). IMCI Information Packet. Department of Child and Adolescent Health and Development, WHO document WHO/CHS/CAH/98.1D: Geneva.
WHO (2005). Urinary tract infections in infants and children in developing countries in the context of IMCI. WHO document WHO/FCH/CAH/05.11.
WHO (2006). Iron supplementation of young children in regions where malaria transmission is intense and infectious disease highly prevalent. http://www.who.int/nutrition/publications/WHOStatement_%20iron%20suppl.pdf.
Acknowledgements
We are grateful to the Bill and Melinda Gates Foundation for funding the study; to DSM, South Africa, for preparing and supplying free of charge the micronutrient premixes; to Mr Chongo of Quality Commodities, Lusaka, for preparing and storing the flours; to the Data Safety and Monitoring Board—Dr Paul Kelly, Dr Jim Todd and Dr Nigel Rollins—for their efforts to monitor and support the trial; to Max Katubulushi, UTH, for audit of the diet randomisation and distribution processes, and to Gabi Meineke, LSHTM, for help with financial management. We are particularly grateful to the mothers and children who participated in the study and to all the other members of the CIGNIS Study Team.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Manno, D., Siame, J., Larke, N. et al. Effect of multiple micronutrient-fortified food on mild morbidity and clinical symptoms in Zambian infants: results from a randomised controlled trial. Eur J Clin Nutr 65, 1163–1166 (2011). https://doi.org/10.1038/ejcn.2011.103
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2011.103
Keywords
This article is cited by
-
Oral iron acutely elevates bacterial growth in human serum
Scientific Reports (2015)