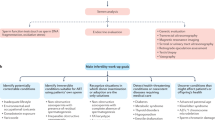
Abstract
Male infertility affects 10% of couples of reproductive age worldwide, and is treatable in many cases. In addition to well-established etiologies, genetic causes of male infertility are now diagnosed more commonly, as our knowledge of genomic medicine advances. Using principles of evidence-based medicine, this review outlines diagnostic and treatment algorithms that guide clinical management. In order of importance, randomized controlled clinical trials, basic scientific studies, meta-analyses, case-controlled cohort studies, best-practice policy recommendations and reviews from peer-reviewed literature were incorporated into algorithms that provide organized and timely guidelines to the current management of male infertility. The strength of the evidence for treatment recommendations is also classified when appropriate.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Abma J et al. (1997) Fertility, Family Planning, and Women's Health: New Data from the 1995 National Survey of Family Growth. In: Vital and Health Statistics Series 23 (No. 19) Atlanta: National Center for Health Statistics
Thonneau P et al. (1991) Incidence and main causes of infertility in a resident population (1,850,000) of three French regions (1988-89). Hum Reprod 6: 811–816
Honig SC et al. (1994) Significant medical pathology uncovered by a comprehensive male infertility evaluation. Fert Steril 62: 1028–1034
WHO (1999) The Semen Analysis WHO Laboratory Manual for the Examination of Human Semen and Sperm–Cervical Mucus Interaction. New York: Cambridge University Press
Guzick DS et al. (2001) National Cooperative Reproductive Medicine Network. Sperm morphology, motility, and concentration in fertile and infertile men. N Engl J Med 345: 1388–1393
Kruger TF et al. (1988) Predictive value of abnormal sperm morphology in in vitro fertilization. Fertil Steril 49: 112–117
Jarow JP et al. (2002) Male Infertility Best Practice Policy Committee of the American Urological Association Inc. Best practice policies for male infertility. J Urol 167: 2138–2144
Gui YL et al. (2004) Male hormonal contraception: suppression of spermatogenesis by injectable testosterone undecanoate alone or with levonorgestrel implants in chinese men. J Androl 25: 720–727
Sigman M and Jarow JP (1997) Endocrine evaluation of infertile men. Urology 50: 659–664
Purohit R et al. (2004) A prospective comparison of 3 diagnostic methods to evaluate ejaculatory duct obstruction. J Urol 171: 232–236
Master VA and Turek PJ (2001) Ejaculatory Physiology and Dysfunction. Urol Clin N Am 28: 363–375
McConnell JD (1997) Abnormalities in sperm motility: techniques of evaluation and treatment. In: Infertility in the Male, edn 3, 249–267 (Eds LI Lipshultz and SS Howards) New York: Mosby
Aitken RJ and Marshall Graves JA (2002) The future of sex. Nature 415: 963
Sigman M and Lopes L (1993) The correlation between round cells and white blood cells in the semen. J Urol 149 (Pt 2): 1338–1340
Eggert-Kruse W et al. (1992) Microbial colonization and sperm–mucus interaction: results in 1000 infertile couples. Hum Reprod 7: 612–620
Turek PJ and Pera RA (2002) Current and future genetic screening for male infertility. Urol Clin North Am 29: 767–792
Cayan S et al. (2001) Response to varicocelectomy in oligospermic men with and without defined genetic infertility. Urology 57: 530–535
Jaffe TM et al. (1998) Sperm pellet analysis: a technique to detect the presence of sperm in men considered to have azoospermia by routine semen analysis. J Urol 159: 1548–1550
Danziger K et al. (2004) Improved detection of cystic fibrosis mutations in infertility patients with DNA sequence analysis. Hum Reprod 19: 540–546
Jarvi K et al. (1995) Cystic fibrosis transmembrane conductance regulator and obstructive azoospermia. Lancet 345: 1578
Zini A et al. (2002) Prevalence of abnormal sperm DNA denaturation in fertile and infertile men. Urology 60: 1069–1072
Turek PJ (1997) Immunopathology and Infertility. In: Infertility in the Male, edn 3, 305–325 (Eds LI Lipshultz and SS Howards) New York: Mosby
Macleod J and Hotchkiss RS (1941) The effect of hyperpyrexia upon spermatozoa counts in men. Endocrinology 28: 780–784
Branigan EF and Muller CH (1994) Efficacy of treatment and recurrence rate of leukocytospermia in infertile men with prostatitis. Fertil Steril 62: 580–584
Haas GG Jr and Manganiello P (1987) A double-blind, placebo-controlled study of the use of methylprednisolone in infertile men with sperm-associated immunoglobulins. Fertil Steril 47: 295–301
Hendry WF et al. (1990) Comparison of prednisolone and placebo in subfertile men with antibodies to spermatozoa. Lancet 335: 85–88
Kamischke A and Nieschlag E (2001) Varicocele treatment in the light of evidence-based andrology. Hum Reprod Update 7: 65–69
Evers JL and Collins JA (2003) Assessment of efficacy of varicocele repair for male subfertility: a systematic review. Lancet 361: 1849–1852
Madgar I et al. (1995) Controlled trial of high spermatic vein ligation for varicocele in infertile men. Fertil Steril 63: 120–124
Nieschlag E et al. (1998) Update on treatment of varicocele: counseling as effective as occlusion of the vena spermatica. Hum Reprod 13: 2147–2150
Pryor JL and Howards SS (1987) Varicocele. Urol Clin North Am 14: 499–513.
Cayan S et al. (2002) Can varicocelectomy significantly change the way couples use assisted reproductive technologies? J Urol 167: 1749–1752
Schlegel PN (1997) Is assisted reproduction the optimal treatment for varicocele-associated male infertility? A cost-effectiveness analysis. Urology 49: 83–90
Turek PJ et al. (1996) Semen parameters before and after transurethral surgery for ejaculatory duct obstruction. J Urol 155: 1291–1293
Belker AM et al. (1991) Results of 1,469 microsurgical vasectomy reversals by the Vasovasostomy Study Group. J Urol 145: 505–511
Sharlip ID (1993) What is the best pregnancy rate that may be expected from vasectomy reversal? J Urol 149: 1469–1471
Kolettis PN and Thomas AJ Jr (1997) Vasoepididymostomy for vasectomy reversal: a critical assessment in the era of intracytoplasmic sperm injection. J Urol 158: 467–470
Kolettis PN et al. (2003) Pregnancy outcomes after vasectomy reversal for female partners 35 years old or older. J Urol 169: 2250–2252
Kolettis PN et al. (2002) Outcomes for vasectomy reversal performed after obstructive intervals of at least 10 years. Urology 60: 885–888
Matsumiya K et al. (1994) A clinical study of azoospermia. Int J Androl 17: 140–142
Guzick DS et al. (1999) Efficacy of superovulation and intrauterine insemination in the treatment of infertility. National Cooperative Reproductive Medicine Network. N Engl J Med 340: 177–183
Palermo G et al. (1992) Pregnancies after intracytoplasmic injection of single spermatozoon into an oocyte. Lancet 340: 17–18
Correa-Villasenor A et al. (2003) The Metropolitan Atlanta Congenital Defects Program: 35 years of birth defects surveillance at the Centers for Disease Control and Prevention. Birth Defects Res A Clin Mol Teratol 67: 617–624
Bonduelle M et al. (1998) Incidence of chromosomal aberrations in children born after assisted reproduction through intracytoplasmic sperm injection. Hum Reprod 13: 781–782
Schroder A and Ludwig M (2002) Congenital malformations after ART. In: Pregnancy and Birth after Assisted Reproductive Technologies, 85–100 New York: Springer
DeBaun MR et al. (2003) Association of in vitro fertilization with Beckwith–Wiedemann syndrome and epigenetic alterations of LIT1 and H19. Am J Hum Genet 72: 156–160
Cox G et al. (2002) Intracytoplasmic sperm injection may increase the risk of imprinting defects. Am J Hum Genet 71: 162–164
Stromberg B et al. (2002) Neurological sequelae in children born after in-vitro fertilization: A population-based study. Lancet 359: 461–465
Van Perperstraten AM et al. (2001) Techniques for surgical retrieval of sperm prior to ICSI for azoospermia Cochrane Database Syst Rev, Issue 4, CD002807
Tournaye H et al. (1997) Are there any predictive factors for successful testicular sperm recovery in azoospermic patients? Hum Reprod 12: 80–86
Mulhall JP et al. (1997) Presence of mature sperm in testicular parenchyma of men with nonobstructive azoospermia: prevelance and predictive factors. Urology 49: 91–96
Schlegel PN (1999) Testicular sperm extraction: microdissection improves sperm yield with minimal tissue excision. Hum Reprod 14: 131–135
Turek PJ et al. (2000) Diagnostic Findings From Testis Fine Needle Aspiration Mapping in Obstructed and Non-Obstructed Azoospermic Men. J Urol 163: 1709–1716
Tsujimura A et al. (2004) Prediction of successful outcome of microdissection testicular sperm extraction in men with idiopathic nonobstructive azoospermia. J Urol 172 (Pt 1): 1944–1947
Guyatt GH et al. (1995) Users' guides to the medical literature. IX: A method for grading health care recommendations. JAMA 274: 1800–1804
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing financial interests.
Glossary
- ORCHIDOPEXY
-
Surgery to place an undescended testis into a more normal position in the scrotum or to untwist a testis that has undergone torsion
- CHORDEE
-
Congential curvature of the penis
- VARICOCELE
-
Dilated plexus of veins draining the testis
- IN VITRO FERTILIZATION (IVF)
-
A method of assisted reproduction in which female eggs are fertilized in vitro after controlled stimulation of egg development with gonadotropins, with subsequent transfer of embryos to the uterus for pregnancy
- HYPOANDROGENISM
-
A low-testosterone state
- INTRAUTERINE INSEMINATION (IUI)
-
The process whereby ejaculated sperm are washed, concentrated and then carefully placed with a syringe past the female cervix and into the uterus to facilitate pregnancy
- Y MICRODELETIONS
-
Regions on the long arm of the Y chromosome that harbor genes important for normal sperm production. These regions have been grouped as azoospermia factor regions AZFa, AZFb and AZFc
- INTRACYTOPLASMIC SPERM INJECTION (ICSI)
-
A micromanipulation strategy used in assisted reproduction in which a single spermatozoa is injected past the egg shell (zona pellucida) directly into the cytoplasm of the egg to facilitate fertilization
- NONOBSTRUCTIVE AZOOSPERMIA
-
No sperm in the ejaculate due to testis failure and atrophy
- OBSTRUCTIVE AZOOSPERMIA
-
No sperm in the ejaculate due to congenital or acquired blockage in the excurrent ductal system of the male reproductive tract
- VASOVASOSTOMY
-
Directly suturing two ends of the vas deferens together using microsurgery to bypass congenital or acquired blockages and facilitate pregnancy
- FNA MAPPING
-
Fine-needle aspiration of the testis performed systemically to acquire information about sperm presence and location for future sperm retrieval
Rights and permissions
About this article
Cite this article
Turek, P. Practical approaches to the diagnosis and management of male infertility. Nat Rev Urol 2, 226–238 (2005). https://doi.org/10.1038/ncpuro0166
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpuro0166
This article is cited by
-
Gel electrophoresis of human sperm: a simple method for evaluating sperm protein quality
Basic and Clinical Andrology (2018)
-
Comparative Proteomics Reveal the Association between SPANX Proteins and Clinical Outcomes of Artificial Insemination with Donor Sperm
Scientific Reports (2018)
-
Microfluidics for sperm analysis and selection
Nature Reviews Urology (2017)
-
Proteomics: a subcellular look at spermatozoa
Reproductive Biology and Endocrinology (2011)