Abstract
The gp130 receptor and its binding partners play a central role in cytokine signalling. Ciliary neurotrophic factor (CNTF) is one of the cytokines that signals through the gp130 receptor complex. CNTF has previously been shown to be a negative regulator of trabecular bone remodelling and important for motor neuron development. Since haematopoietic cell maintenance and differentiation is dependent on the bone marrow (BM) microenvironment, where cells of the osteoblastic lineage are important regulators, we hypothesised that CNTF may also have important roles in regulating haematopoiesis. Analysis of haematopoietic parameters in male and female Cntf−/− mice at 12 and 24 weeks of age revealed altered B lymphopoiesis. Strikingly, the B lymphocyte phenotype differed based on sex, age and also the BM microenvironment in which the B cells develop. When BM cells from wildtype mice were transplanted into Cntf−/− mice, there were minimal effects on B lymphopoiesis or bone parameters. However, when Cntf−/− BM cells were transplanted into a wildtype BM microenvironment, there were changes in both haematopoiesis and bone parameters. Our data reveal that haematopoietic cell-derived CNTF has roles in regulating BM B cell lymphopoiesis and both trabecular and cortical bone, the latter in a sex-dependent manner.
Similar content being viewed by others
Introduction
Cytokines that signal through the gp130 receptor play important roles in bone biology and neuronal survival1. One of these factors, ciliary neurotrophic factor (CNTF), binds with high affinity to a receptor complex consisting of the CNTF receptor (CNTFR), the gp130 receptor and leukemia inhibitory factor (LIF) receptor (LIFR). It can also bind with lower affinity to a complex consisting of the interleukin-6 receptor, GP130 and LIFR2.
Mice that lack Cntfr are perinatal lethal, surviving less than 24 hours after birth3. The Cntfr−/− mice displayed significant loss of motor neurons and were unable to suckle, which likely resulted in their premature death3. In contrast, Cntf−/− mice are viable, although they displayed significant reductions in motor neurons from 8 weeks of age4. Studies of the Cntf−/− mice have also revealed that CNTF regulates normal bone structure in a sex-dependent manner5. While both male and female Cntf−/− mice have shorter femur lengths compared to wildtype (WT) littermates, they showed different phenotypes in other bone parameters. Female Cntf−/− mice had increased trabecular bone volume, caused by an increase in osteoblast number and bone formation rate. In contrast, male Cntf−/− mice had normal trabecular bone but significantly reduced cortical bone5.
The bone marrow (BM) within the bone cavity is central for blood cell development. Structural or functional alterations to the BM microenvironment, which includes cells of the osteoblastic lineage6, have previously been shown to affect haematopoietic cell development. In particular, changes in osteoblast numbers have been associated with alterations in haematopoietic stem cell (HSC) numbers and function7,8.
B lymphopoiesis is also finely regulated by cells of the BM microenvironment. Tokoyoda et al. showed that B cell progenitors are in contact with stromal cells in the BM that express either chemokine (C-X-C motif) ligand 12 (CXCL12) or interleukin-7 (IL-7), two cytokines that are important for B cell differentiation9. Specifically, pre-pro B cells co-localised with CXCL12-expressing stromal cells while pro-B cells were in contact with IL-7-expressing stromal cells. Maturation beyond pro-B cells requires the developing B cells to migrate away from IL-7 and CXCL12-positive cells and pre-B cells and immature IgM-expressing B cells were not found in contact with either of these cell types in the BM9.
Furthermore, in vitro culture studies showed that primary osteoblasts support B cell development10 and in vivo changes in osteoblast numbers altered the numbers of different subsets of B-lymphocytes10,11,12. However, the exact mechanism for the involvement of osteoblasts in the regulation of B cell development is not known. The level of osteoblasts does not correlate to the number of B cells, indicating that other, more complex mechanisms are involved12.
Despite the proven effect of CNTF on osteoblast numbers and function, nothing is known about the effects of CNTF on haematopoiesis. Here we have investigated the role of CNTF in haematopoiesis by analysing the haematopoietic cell phenotypes of Cntf-−/− mice. Our analyses revealed that Cntf−/− mice have altered B lymphopoiesis, however, the B cell phenotype differs based on sex, age and also the BM microenvironment in which the B cells develop.
Results
Female mice lacking Cntf have reductions of immature B cells in the bone marrow
As previously shown, 12-week-old Cntf−/− mice have a sex-dependent bone phenotype, where female mice have increased bone volume accompanied by increased osteoblast numbers5. The lack of Cntf did not affect osteoclasts and culture studies confirmed that CNTF directly inhibits osteoblast differentiation5. To investigate whether the bone phenotype was accompanied by changes to haematopoiesis, we analysed haematopoietic cell content in peripheral blood (PB), bone marrow (BM), spleen and thymus of female Cntf−/− mice at 12 and 24 weeks of age. There were no significant differences in the numbers of leukocytes or erythrocytes in PB, BM or thymus, PB platelets, total body, or thymus weights (Supplementary Fig. 1). In contrast, spleen weights, spleen leukocytes, erythrocytes and platelets were significantly reduced in 12-week-old, but not 24-week-old, female Cntf−/− mice (Supplementary Fig. 1).
Interestingly, analysis of specific haematopoietic lineages using flow cytometry revealed an effect on B cell development in 12- and 24-week-old female Cntf−/− mice, where we observed reduced proportions of immature B220+IgM+ B cells in the BM of 12-week-old Cntf−/− mice and B220+IgM− B cells in the BM of 24-week-old Cntf−/− mice (Fig. 1a,b). However, although there were trends to reductions in pro-B cells in 24-week-old Cntf−/− mice (P = 0.11 vs. 24-week-old Cntf+/+ females), BM progenitor B cells were not significantly affected (Fig. 1b–e). The decreases in the immature B cell populations in the BM were not reflected in PB or spleen (Supplementary Fig. 2). Furthermore, 12-week-old male Cntf−/− mice had significantly increased B220+IgM+ cells in their BM (Fig. 1f). Aside from this, male Cntf−/− mice at either 12 or 24 weeks of age did not have any obvious B cell phenotype (Fig. 1f–j and Supplementary Fig. 2). The effects on other haematopoietic lineages were modest in both female (Supplementary Fig. 3) and male (Supplementary Fig. 4) mice. Female mice displayed a slight disruption of T cell development as shown by an increase of CD8+ T cells in the spleen at 12 weeks (Supplementary Fig. 3) and a reduction of CD4+ T cells in the BM at 24 weeks (Supplementary Fig. 3).
Analysis of BM B cell populations in female and male Cntf−/− and Cntf+/+ mice.
Shown are BM B cell populations in 12 and 24-week-old female (a–e) and male (f–j) Cntf−/− (KO) and Cntf+/+ (WT) mice. The following populations were analysed: B220+IgM+ immature B cells (a,f), B220+IgM− B cells (b,g), pre-pro B cells (c,h), pro-B cells (d,i) and pre-B cells (e,j). Data are shown as mean ± SEM, n = 3–9. The unpaired Student’s T-test was used for statistical comparisons between age- and sex-matched mice. *P < 0.05, **P < 0.01.
The trabecular and cortical bone phenotypes have previously been described for 12-week-old, but not 24-week-old mice. As shown in Fig. 2, 24-week-old female Cntf−/− mice have increased trabecular bone volume, trabecular number and reduced trabecular separation (Fig. 2a–d,i,j), similar to that shown for 12-week-old female Cntf−/− mice5. In contrast and consistent with that observed in 12-week-old male Cntf−/− mice, while the bone volume was slightly reduced in 24-week-old Cntf−/− mice (P = 0.11 vs. Cntf+/+ males, Fig. 2e), trabecular bone parameters in 24-week-old male knock-out (KO) mice were not significantly affected by the loss of Cntf (Fig. 2e–h,k,l). Furthermore, the loss of Cntf did not affect cortical bone parameters in 24-week-old female or male mice (Supplementary Fig. 5 and 6), consistent with the phenotype observed in 12-week-old female Cntf−/− mice, but different to that reported in 12-week-old male Cntf−/− mice5.
Analysis of trabecular bone in female and male Cntf−/− and Cntf+/+ mice.
The secondary spongiosa of the proximal femur was assessed by micro-computed tomography in femurs from 24-week-old female (a–d,i,j) and male (e–h,k,l) Cntf−/− (KO) and Cntf+/+ (WT) mice. The following parameters were assessed: bone volume/total volume (BV/TV) (a,e), trabecular thickness (b,f), trabecular number (c,g) and trabecular separation (d,h). Representative micro-CT images of the femurs of (i) female Cntf+/+ mice or (j) female Cntf−/− mice and femurs of (k) male Cntf+/+ mice or (l) male Cntf−/− mice are shown at 24 weeks of age. Data are shown as mean ± SEM, n = 4–6. The unpaired Student’s T-test was used for statistical comparisons. *P < 0.05, **P < 0.01.
Il-7 expression is deregulated in Cntf−/− female mice in both osteoblastic and pro-B cells
To determine the potential mechanisms resulting in reduced B cell populations in the BM of female Cntf−/− mice we performed further studies using female Cntf+/+ and Cntf−/− mice. There were no differences in the proportions of long-term repopulating haematopoietic stem cells [lineage negative, c-kit+, Sca-1+ (LKS+) CD150+ cells] or common lymphoid progenitor cells (CLPs) in the BM of the 12- or 24-week-old female Cntf−/− mice (Fig. 3a,b). Furthermore, the LKS+ CD150- cells consisting of short-term repopulating stem cells and multipotent progenitors were not altered in the Cntf−/− mice compared to their wildtype littermates [LKS+CD150- cells (% of total BM, mean ± SEM, n = 4–5 mice): Cntf+/+: 0.139 ± 0.026%; Cntf−/−: 0.107 ± 0.030%]. We next analysed the level of apoptosis in B cell populations in 12-week-old females but could not detect any changes that could explain the reduction of the immature B cells (Fig. 3c). We determined that Cntf was expressed by developing B lymphocytes sorted from WT BM, especially by pro-B, pre-B and immature B220+IgM+ B cells (Fig. 3d), suggesting potential intrinsic roles for CNTF in regulating B lymphopoiesis. In contrast, none of the B cell populations expressed CNTFR (data not shown).
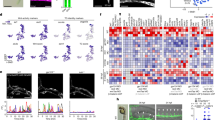
Il7 and Cxcl12 expression in sorted BM osteoblastic cells and B cell populations from 12-week- and 24-week-old female Cntf−/− and Cntf+/+ mice.
Proportions of (a) lineage negative, c-kit+, Sca-1+ CD150+ (LKS+CD150+) haematopoietic stem cells and (b) common lymphoid progenitors in BM. Analysis of apoptosis (c) and Cntf expression (d) in BM B cell populations from Cntf−/− (KO) and Cntf+/+ (WT) 12-week-old mice. Osteoblast progenitors (e,g) and osteoblasts (f,h) were sorted from 12-week-old female Cntf−/− (KO) and Cntf+/+ (WT) mice and the expression of Il7 (c,d) and Cxcl12 (d,f) was analysed (n = 3 separate sort experiments but within each experiment, 3–4 mice were pooled). BM was also sorted into B cell populations and analysed for the expression of Cxcl12 (i) and Il7 (j). Data are shown as mean ± SEM, n = 3–4. One-way analysis of variance followed by post-hoc testing or the unpaired Student’s T-test was used for statistical comparisons. *P < 0.05.
Osteoblasts have previously been shown to express CNTFR, but not CNTF5. To determine if there might be extrinsic changes in the BM microenvironment supporting B lymphopoiesis, we first examined the expression of B cell regulatory factors in whole BM obtained from 12-week-old female Cntf−/− and Cntf-+/+ mice, focusing on extrinsic factors that have been shown to be essential in regulating B lymphopoiesis13. There were no changes in the expression of Flt3 ligand, or Rankl (receptor activator of nuclear factor-κβ ligand) observed in whole bone marrow mRNA obtained from Cntf−/− or Cntf+/+ mice (data not shown). In contrast, we observed trends to increased expression of Il7 and Cxcl12 transcripts in BM from 12-week-old female Cntf−/− compared to Cntf+/+ mice (data not shown). We therefore purified osteoblast progenitors (lineage, CD45 and CD31 negative, Sca-1+, CD51+) and relatively mature osteoblast cell (lineage, CD45 and CD31 negative, Sca-1 negative, CD51+) populations from 12-week-old female Cntf−/− and Cntf+/+ mice using fluorescence activated cell sorting (FACS)14,15 and analysed the expression of Il7 and Cxcl12 in these populations. The expression of Il7 was significantly reduced in osteoblast progenitors (Fig. 3e) and increased in osteoblasts sorted from Cntf−/− mice (Fig. 3f). In contrast, the expression of Cxcl12 was unchanged in both populations (Fig. 3g,h). We also sorted B cell populations from the same mice and analysed the expression levels of Cxcl12 and Il7. Cxcl12 expression was very low and unchanged in B cells isolated from Cntf−/− mice compared to Cntf+/+ mice (Fig. 3i). Intriguingly, while the different B cell populations sorted from Cntf+/+ mice had undetectable expression of Il7 (Fig. 3j), we detected Il7 expression exclusively in pro-B cells sorted from Cntf−/− mice (Fig. 3j).
Deregulated B cell differentiation and altered bone parameters observed in Cntf−/− mice are partly due to haematopoietic cell-intrinsic effects on Cntf in haematopoietic cells
The mice used for this study are complete knockouts, hence Cntf expression is lacking from all cells. The effects observed in B cell development could thus be a result of indirect stimulation from the surrounding microenvironment or from intrinsic effects in the haematopoietic system. To delineate whether the observed changes are intrinsic to the haematopoietic cells or whether they are induced by the microenvironment, we transplanted either Cntf+/+ or Cntf−/− BM cells into WT mice or WT BM cells into Cntf+/+ or Cntf−/− mice. Given the differences observed between the female and male sexes, we performed female into female and male into male BM transplants.
There were no changes in PB, BM, spleen or thymus cellularities or spleen or thymus weights in WT recipients of Cntf−/− BM cells of either sex (Supplementary Fig. 7). However, transplantation of female Cntf−/− BM cells into a female WT microenvironment resulted in a more profound, but intriguingly different, haematopoietic phenotype than that observed in full Cntf−/− female mice. There were significant increases in immature B220+IgM+ B cells (Fig. 4a) and B220+IgM− B cells (Fig. 4b). Fractionation of the B220+IgM- cells revealed significant increases in pre-pro and pro-B cell populations (Fig. 4c,d). Furthermore, a trend towards an increase in pre-B cells was observed (Fig. 4e). Analysis of myeloid cells in the BM (Fig. 4f–h) showed a significant reduction of mature granulocytes (Fig. 4g). No other changes were observed in any of the haematopoietic cells in the female WT recipients (Fig. 4f,h and data not shown).
Haematopoietic lineage analysis of BM from WT mice following transplantation of Cntf−/− and Cntf+/+ BM.
Female (a–h) or male WT mice (i–p) were transplanted with Cntf−/− (KO) and Cntf+/+ (WT) BM cells (female cells into female mice and male cells into male mice) and the BM content was analysed using FACS at 12 weeks post-transplantation. Presented here is the analysis of B220+IgM+ immature B cells (a,i), B220+IgM- B cells (b,j), pre-pro B cells (c,k), pro-B cells (d,l), pre-B cells (e,m), CD11b+Gr-1low immature granulocytes (f,n), CD11b+Gr-1br mature granulocytes (g,o) and F4/80+CD11b− pre-osteoclasts (h,p). Data are shown as mean ± SEM, n = 5–10. The unpaired Student’s T-test was used for statistical comparisons. *P < 0.05, **P < 0.01, *** P < 0.005.
Similar haematopoietic changes were observed in male WT recipients transplanted with male Cntf−/− BM cells (Fig. 4i–p). These recipients also had significantly increased pre-pro B and pro-B cells (Fig. 4k,l). Furthermore and also similar to the female WT recipients, the male WT recipients of Cntf−/− BM cells had significant reductions in mature granulocytes (Fig. 4o) in their BM. Furthermore, the proportions of F4/80+CD11b− pre-osteoclasts were increased in the BM of the WT male recipients (Fig. 4p).
There were also significant differences observed in the female and male bone parameters when Cntf−/− BM cells were transplanted into WT recipients. In female recipients, there was a trend to decreased trabecular bone volume (Fig. 5a), no changes to trabecular thickness (Fig. 5b), significant increases in trabecular number (Fig. 5c) and significant reductions in trabecular separation (Fig. 5d) in WT recipients transplanted with Cntf−/− BM cells (Fig. 5j) compared to WT recipients transplanted with Cntf-+/+ BM cells (Fig. 5i). These phenotypes were similar to those observed in 12-week5 and 24-week-old female Cntf−/− mice (Fig. 2). In contrast and also the same as that observed in 12-week and 24-week-old female Cntf−/− mice, female WT recipients transplanted with female Cntf−/− BM cells had no changes in cortical bone parameters (Supplementary Figs 6 and 8).
Trabecular bone phenotype in female and male WT recipients of Cntf−/− and Cntf+/+ BM.
Female (a–d) or male WT mice (e–j) were transplanted with Cntf−/− (KO) and Cntf+/+ (WT) BM cells (female cells into female mice and male cells into male mice) and femurs were analysed using micro-computed tomography at 12 weeks post-transplantation. Shown are the trabecular bone parameters: bone volume/total volume (BV/TV) (a,e), trabecular thickness (b,f), trabecular number (c,g) and trabecular separation (d,h). Representative micro-CT images of the femurs of WT female mice transplanted with (i) female Cntf+/+ BM or (j) female Cntf−/− BM and femurs of WT male mice transplanted with (k) male Cntf+/+ BM or (l) male Cntf−/− BM are shown at 12 weeks post-transplant. Data are shown as mean ± SEM, n = 5–10. The unpaired Student’s T-test was used for statistical comparisons. *P < 0.05.
The bone phenotypes observed in Cntf−/− male mice were also recapitulated in male WT recipients of Cntf−/− BM cells. These recipients had no changes in trabecular bone parameters (Fig. 5e–h,k,l), but did have significant reductions in cortical bone parameters (Supplementary Figs 6 and 8). Similar to the phenotypes observed in 12-week-old male Cntf−/− mice5, WT male recipients of male Cntf−/− BM cells had significant reductions in endocortical and periosteal perimeters (Supplementary Figs 6 and 8). There were slight but not significant reductions in cortical thickness (Supplementary Figs 6 and 8), significant reductions in mean polar movement of inertia, cortical area and marrow area (Supplementary Figs 6 and 8).
In contrast, when Cntf+/+ BM cells were transplanted into a Cntf−/− microenvironment (hence measuring extrinsic regulation of haematopoiesis by CNTF), we could not observe any changes to haematopoietic parameters except for decreased spleen weights and spleen leukocyte cellularity in male Cntf−/− recipient mice (Supplementary Fig. 6 and Fig. 6a–p). Interestingly, the increase in trabecular bone in the full Cntf−/− females was normalised after transplantation of WT BM into female Cntf−/− recipients (Fig. 7a–d,i,j). However, analysis of cortical bone (Supplementary Figs 6 and 9) showed that endocortical perimeter and marrow area were significantly reduced when WT BM was transplanted into female Cntf−/− recipients compared to female Cntf+/+ recipients (Supplementary Figs 6 and 9). In contrast, there were no differences in cortical bone (Supplementary Figs 6 and 9) or trabecular bone (Fig. 7e–j,k,l) in the male Cntf−/− transplant recipients.
Haematopoietic lineage analysis of BM from Cntf−/− and Cntf+/+ mice following transplantation of WT BM.
Female (a–h) or male Cntf−/− (KO) and Cntf+/+ (WT) mice (i–p) were transplanted with WT BM cells (female cells into female mice and male cells into male mice) and the BM content was analysed using flow cytometry at 12 weeks post-transplantation. Lineage analysis shows B220+IgM+ immature B cells (a,i), B220+IgM- B cells (b,j), pre-pro B cells (c,k), pro-B cells (d,l), pre-B cells (e,m), CD11b+Gr-1low immature granulocytes (f,n), CD11b+Gr-1br mature granulocytes (g,o) and F4/80+CD11b− pre-osteoclasts (h,p). Data are shown as mean ± SEM, n = 5–6. The unpaired Student’s T-test was used for statistical comparisons.
Trabecular bone phenotype in female and male Cntf−/− and Cntf+/+ recipients of WT BM.
Female (a–d,i,j) or male Cntf−/− (KO) and Cntf+/+ (WT) mice (e–h,k,l) were transplanted with WT BM cells (female cells into female mice and male cells into male mice) and femurs were analysed using micro-computed tomography at 12 weeks post-transplantation. Shown are the trabecular bone parameters: bone volume/total volume (BV/TV) (a,e), trabecular thickness (b,f), trabecular number (c,g) and trabecular separation (d,h). Representative micro-CT images of the femurs of (i) female Cntf+/+ mice or (j) female Cntf−/− mice transplanted with female WT BM and femurs of (k) male Cntf+/+ mice or (l) male Cntf−/− mice transplanted with male WT BM are shown at 12 weeks post-transplant. Data are shown as mean ± SEM, n = 5–6. The unpaired Student’s T-test was used for statistical comparisons.
Discussion
In this study, we present data that reveal that haematopoietic-cell derived CNTF regulates haematopoiesis and bone mass. We show that, similarly to the bone phenotypes previously reported5 and also shown here (Fig. 2), the haematopoietic phenotype is sex-specific in the full Cntf−/− mice. Furthermore, transplantation studies revealed that the majority of the haematopoietic and bone cell phenotypes observed in Cntf−/− mice were due to transplantable Cntf−/− BM cells. Interestingly, however, the B cell phenotypes observed in female WT mice transplanted with female Cntf−/− BM cells were more striking than those observed in full Cntf−/− female mice. Furthermore, the male WT mice transplanted with male Cntf−/− BM cells showed a similar B lymphocyte phenotype to the female transplant recipients of female Cntf−/− BM cells, whereas full Cntf−/− male mice had no significant haematopoietic cell phenotypes. In addition, the trabecular bone phenotype observed in 12- and 24-week-old Cntf−/− female mice was largely recapitulated in female WT recipients of Cntf−/− female BM cells. Likewise, the cortical bone phenotype reported in 12-week-old full Cntf−/− male mice was phenocopied in male WT recipients transplanted with Cntf−/− male BM cells.
The main haematopoietic cell type affected by the loss of Cntf were the immature BM B220+IgM+ cells, which were significantly reduced in 12-week-old Cntf−/− female mice and increased in 12-week-old Cntf−/− male mice and B220+IgM− cells, which were significantly reduced in 24-week-old Cntf−/− female mice. The reduction of B cells in the female mice was not due to increased death of the immature B cells since no differences were observed in apoptosis in any of the developing B cell populations in the BM, including immature B cells, in Cntf−/− compared to Cntf+/+ female mice. Hence we focused on determining if key regulators of B cell development13 were perturbed in Cntf−/− female mice. While we observed no changes in Flt3L or Rankl transcripts in whole bone marrow, there were trends to increased levels of Cxcl12 and Il7, both of which have previously been shown to be expressed by osteoblast lineage cells12. Given that osteoblast numbers are increased in 12-week-old Cntf−/− female mice5 we therefore FACS-sorted osteoblast progenitors and osteoblastic cells from these mice and their WT littermates to assess their expression of Cxcl12 and Il7. We could not detect any significant differences in the expression of Cxcl12 in osteoblast progenitors or osteoblasts from either genotype. However, Il7 was significantly deregulated in both osteoblasts progenitors and osteoblasts, with reduced expression of Il7 observed in Cntf−/− osteoblast progenitors and increased expression of Il7 in the Cntf−/− mature osteoblasts compared to those FACS-sorted from the wildtype littermate controls.
Surprisingly, Il7 expression was also detected in pro-B cells sorted from female Cntf−/− mice. We cannot explain why Il7 was increased in these cells, or if it had any functional consequences. However, it is possible that Il7 was expressed by the pro-B cells in a compensatory manner in response to deregulated Il7 expression by the different osteoblast lineage cells. Alternatively, it may be that Il7 was increased in response to loss of CNTF in pro-B cells, either directly or indirectly due to increased signalling via other gp130 cytokine family members, such as IL-6. In support of this, elevated production of IL-7 has been reported in mice that have a mutation in the gp130 IL-6 receptor subunit, which results in enhanced gp130-mediated activation of signal transducer and activator of transcription 3 (STAT3)16.
Interestingly, IL-7 is essential for the development of pro-B and pre-B lymphocytes in the BM and has also been shown to be important in regulating the differentiation of pre-pro-B cells into pro-B cells17,18,19. While we did not observe any alterations in pro-B or pre-B cells in full Cntf−/− mice, it is interesting that pre-pro-B, pro-B, pre-B and immature B220+IgM+ cells were increased in the BM of female WT recipients transplanted with BM from female Cntf−/− mice. Furthermore, increases in pre-pro-B and pro-B cells were observed in male WT recipients transplanted with BM from male Cntf−/− mice, whereas in full male Cntf−/− mice there were no B lymphocyte phenotypes, with the exception of increased B220+IgM+ cells in 12-week-old male Cntf−/− mice. We cannot explain why the B cell phenotype is different in full Cntf−/− mice compared to the WT recipients transplanted with Cntf−/− BM cells. However, it is possible that loss of CNTF in other environments, including the brain, or compensatory mechanisms in the BM microenvironment, such as the altered Il7 expression observed in the osteoblast lineage cells in Cntf−/− female mice, may contribute to haematopoietic cell regulation in the full Cntf−/− mice.
The differences in the haematopoietic cell phenotypes observed in the full Cntf−/− mice compared to chimeras where the BM microenvironment was WT and the haematopoietic cells were Cntf−/− do, however, support a role for CNTF as being a negative regulator of B lymphopoiesis. It cannot be excluded that the altered B lymphopoiesis observed in WT recipients of Cntf−/− BM cells is regulated partly by the microenvironment since the Cntf−/− haematopoietic cells altered the bone microenvironment in the WT recipients and this, in turn, could de-regulate B lymphopoiesis. Indeed, the B lymphocyte phenotypes were accompanied by striking bone phenotypes, further adding to the evidence that there is a reciprocal relationship between B lymphopoiesis and the skeletal system (reviewed by Manilay and Zouali, 2014)20. Our data reveal that the increased trabecular bone and the reduced cortical bone parameters previously reported in 12-week-old female mice and 12-week-old male mice5, respectively, are also largely induced by Cntf−/− haematopoietic cells.
In female recipients of Cntf−/− BM cells, we observed increased trabecular number and reduced trabecular separation, but not increased bone volume. We have recently shown that bone marrow transplantation causes irreversible bone loss in mice, due to enhanced osteoclastogenesis early after the transplant21. This potent response to the transplant procedure likely prevented the increase in bone volume in these transplant recipients compared to non-ablated Cntf−/− female mice. In male recipients of Cntf−/− BM cells, the loss of cortical bone was accompanied by increased numbers of F4/80+CD11b− pre-osteoclast cells22. Hence, the reduction of cortical bone observed in both the full Cntf−/− male mice and WT male recipients transplanted with Cntf−/− BM cells could be a result of increased osteoclast numbers and activity in the cortical region of bone.
As previously mentioned, CNTF belongs to the large IL-6 family of cytokines that all signal through the gp130 receptor. In mice, deletion of the gp130 receptor is embryonic lethal and the embryos develop defects of the haematopoietic system23. Haematopoietic stem and progenitor cells, T cells and megakaryocytes are severely reduced in the gp130 deficient embryos and approximately 20% of the embryos are anaemic23. However, when individual members of the IL-6 cytokine family such as IL-6, oncostatin M receptor (OSMR), leukaemia inhibitory factor (LIF) or CNTF are deleted, milder haematopoietic phenotypes appear. This is not surprising considering that there are likely overlapping functions of the various cytokines and in addition, the expression pattern of the different gp130 cytokines is not as broad as gp13024,25,26.
Il-6−/−, Osmr−/− and Lif−/− mice all had altered regulation of haematopoietic stem and progenitor cells, although they all exhibited different defects. Il-6−/− mice had a mild defect where only the progenitors that give rise to colony-forming unit-spleen (CFU-S) were reduced24. The reduction of progenitors was more severe in Lif−/− mice where CFU-S were severely reduced in both BM and spleen. Furthermore, other BM progenitor types such as the BFU-E and GM-CFC were reduced in Lif−/− mice26. Osmr−/− mice had reduced peripheral erythrocytes and platelets and this was reflected by reduced numbers of erythrocyte- and megakaryocyte-forming progenitors in the BM25. The reduction of progenitors in the BM was compensated for in the spleen where the same progenitor types were increased. In contrast to this, we did not observe any changes to the haematopoietic stem and progenitor compartment in Cntf−/− mice, nor did we observe anaemia or thrombocytopenia in their peripheral blood.
For Cntf−/− mice, the primary haematopoietic cell defect appears to involve B cell differentiation. This is different to the other IL-6 family members mentioned above. B cell numbers were normal in Il-6−/−, Osmr−/− and Lif−/− mice, although the function of mature B cells was somewhat compromised in Il-6−/− mice. Like the Cntf−/− mice described here, Il-6−/−, Osmr−/− and Lif−/− mice were all complete KOs, meaning that the defects observed could potentially arise due to changes in the microenvironment rather than due to direct effects on the haematopoietic cells. For the Lif−/− mice it appears that lack of LIF in the microenvironment caused the haematopoietic defects26. The phenotypes of the Osmr−/− mice are more complex where both direct and indirect effects on the haematopoietic cells caused the defects in erythrocyte and platelet differentiation25. Results from our studies of the Cntf−/− mice suggests that CNTF has mainly intrinsic effects on haematopoiesis. In all, members of the IL-6 cytokine family, including CNTF, are important for haematopoietic cell regulation but their effects appear to be distinct to each other rather than redundant.
In conclusion, we show here that, in addition to its roles in regulating neurons and bone, CNTF has intrinsic regulatory effects on haematopoiesis, in particular B lymphopoiesis. Furthermore, we reveal, for the first time, that the bone phenotypes observed in Cntf−/− mice occur largely due to loss of CNTF in haematopoietic cells.
Methods
Mice
All animal experiments were approved and conducted in accordance with the guidelines of the St. Vincent’s Health Animal Ethics Committee. Cntf−/− mice have been previously described4 and are on a C57BL/6 background, their Cntf+/+ controls were generated from heterozygous matings. For bone marrow transplant experiments, WT B6.SJL-Ptprca mice (CD45.1+) were obtained from Animal Resources Centre, Perth, WA, Australia for use as either WT donor BM cells transplanted into Cntf−/− or Cntf+/+ mice or as transplant recipients of Cntf−/− or Cntf+/+ BM cells. All transplant experiments were performed using 12-week-old recipients and the mice were euthanased for analysis at 12 weeks post-transplant. For the transplants, all recipients were lethally irradiated (10 Gy γ-irradiation, split dose given three hours apart) using a Gammacell 40 Exactor (Best Theratronics, Ontario, Canada) on the day of transplant. Recipient mice were each intravenously injected with 5 × 106 unfractionated BM cells obtained from the donor mice and received enrofloxacin via drinking water for 4 weeks post irradiation. All studies were performed as a minimum of two independent experiments. Mice were housed in cages and were fed with food and water ad libitum, with a 12 h light and 12 h dark cycle.
Haematopoietic cell analysis
Haematopoietic cell counts from peripheral blood (PB), spleen and flushed BM were determined using a haematological analyser (Sysmex KX-21N, Roche Diagnostics). For FACS, cells obtained by pooling flushed BM and BM from crushed femurs, tibiae and ileac crests were stained with fluorescence-conjugated antibodies against murine B220, IgM, CD43, CD19, Gr-1, CD11b, F4/80, CD4 and CD8 for mature cell lineage assessment (eBioscience). Immature haematopoietic stem cell and progenitors and common lymphoid progenitors were assessed in lineage negative cells (ie. cells that did not express CD2, CD3, CD4, CD5, CD8, CD11b, Gr-1, B220 or Ter119) and positive staining with antibodies against Sca-1, c-kit and CD150 or CD127, respectively as previously described27. Gating strategies for some of the mature and immature haematopoietic cells are provided in Supplementary Figure 10. Apoptosis was measured in B cell populations using AnnexinV and 7AAD staining27. BM B cell populations were sorted using a FACSAria (BD Biosciences) or the BM, spleen, thymus and hemolysed PB cells were stained and collected for analysis using a LSRII Fortessa (BD Biosciences) with data analysed using FlowJo software version 8.8.6 (TreeStar).
In vitro bone analysis
Bones were fixed in 2% paraformaldehyde (PFA, Sigma) in phosphate buffer solution (PBS) pH8.0 for 16–24 h and stored in 70% ethanol until analysed. For micro-computed tomography (micro-CT) analysis, the secondary spongiosa of the proximal femur were assessed, in accordance to standard guidelines28. Bones were scanned at an x-ray potential of 49 kV, a current of 100 μA and at an isotropic voxel size of 9 μm using the Skyscan1076 (Bruker-MicroCT, Kontich, Belgium). Serial tomograms were reconstructed using NRecon (Version 1.6.3.1, SkyScan) with a smoothing of 1, a ring artifact reduction of 6 and a beam hardening correction of 35%. A trabecular region 2.4 mm distal from the top of the femur extending 2 mm was analysed in CTAn (Version 1.10.1.0, SkyScan). All trabecular measurements for transplant recipients were made by manually delineating trabecular bone from the endocortical boundary, with an adaptive pre-threshold of 35–255. All trabecular measurements for 24-week-old Cntf−/− and Cntf+/+ mice were performed using automated settings. For 24-week-old males the threshold was 46, for 24-week-old females the threshold was 31.
Isolation of osteoblast progenitor and osteoblastic cells from bone
Osteoblast progenitor cells (lineage negative, CD45−, CD31−, CD51+, Sca-1+) and osteoblastic cells (lineage negative, CD45−, CD31−, CD51+, Sca-1−) were sorted from collagenase-digested long bones obtained from 12-week-old female Cntf−/− and Cntf+/+ mice as previously described11,15. All antibodies were obtained from eBioscience.
Quantitative real-time PCR analysis (qPCR)
Quantitative real-time PCR (qPCR) was performed on cDNA using Brilliant II Sybr Green QPCR master mix (Agilent Technologies) on the MX3000P Multiplex Quantitative PCR system (Stratagene) with oligonucleotide primers (IDT). Primers for Rankl and housekeeping genes have been previously published21. Primers for Il7 are also published29. Primer sequences are as follows: Cxcl12: Forward: GAG CCA ACG TCA AGC ATC TG; Reverse: GAG CCA ACG TCA AGC ATC TG. Flt3-L: Forward: CCC AGC CAG TCA GCG TTG GT; Reverse: CAC GTG CAT CGG ATT CGT GGG T.
Statistical analysis
One-way analysis of variance followed by post-hoc testing was used for multiple comparisons. The unpaired Student’s T-test was used for statistical comparisons between two different populations. All statistical analysis was performed using Prism 6 software (GraphPad).
Additional Information
How to cite this article: Askmyr, M. et al. Ciliary neurotrophic factor has intrinsic and extrinsic roles in regulating B cell differentiation and bone structure. Sci. Rep. 5, 15529; doi: 10.1038/srep15529 (2015).
References
Sims, N. A. & Walsh, N. C. GP130 cytokines and bone remodelling in health and disease. BMB Reports. 43, 513–523 (2010).
Wagener, E. M. et al. The amino acid exchange R28E in ciliary neurotrophic factor (CNTF) abrogates interleukin-6 receptor-dependent but retains CNTF receptor-dependent signaling via glycoprotein 130 (gp130)/leukemia inhibitory factor receptor (LIFR). J. Biol. Chem. 289, 18442–18450, doi: 10.1074/jbc.M114.568857 (2014).
DeChiara, T. M. et al. Mice lacking the CNTF receptor, unlike mice lacking CNTF, exhibit profound motor neuron deficits at birth. Cell. 83, 313–322 (1995).
Masu, Y. et al. Disruption of the CNTF gene results in motor neuron degeneration. Nature. 365, 27–32, doi: 10.1038/365027a0 (1993).
McGregor, N. E. et al. Ciliary neurotrophic factor inhibits bone formation and plays a sex-specific role in bone growth and remodeling. Calcif. Tissue Int. 86, 261–270, doi: 10.1007/s00223-010-9337-4 (2010).
Askmyr, M., Sims, N. A., Martin, T. J. & Purton, L. E. What is the true nature of the osteoblastic hematopoietic stem cell niche? Trends Endocrinol. Metab. 20, 303–309, doi: 10.1016/j.tem.2009.03.004 (2009).
Calvi, L. M. et al. Osteoblastic cells regulate the haematopoietic stem cell niche. Nature. 425, 841–846, doi: 10.1038/nature02040 (2003).
Zhang, J. et al. Identification of the haematopoietic stem cell niche and control of the niche size. Nature. 425, 836–841 (2003).
Tokoyoda, K., Egawa, T., Sugiyama, T., Choi, B. I. & Nagasawa, T. Cellular niches controlling B lymphocyte behavior within bone marrow during development. Immunity. 20, 707–718, doi: 10.1016/j.immuni.2004.05.001 (2004).
Zhu, J. et al. Osteoblasts support B-lymphocyte commitment and differentiation from hematopoietic stem cells. Blood. 109, 3706–3712, doi: 10.1182/blood-2006-08-041384 (2007).
Visnjic, D. et al. Hematopoiesis is severely altered in mice with an induced osteoblast deficiency. Blood. 103, 3258–3264, doi: 10.1182/blood-2003-11-4011 (2004).
Wu, J. Y. et al. Osteoblastic regulation of B lymphopoiesis is mediated by Gs{alpha}-dependent signaling pathways. Proc. Natl. Acad. Sci. USA 105, 16976–16981, doi: 10.1073/pnas.0802898105 (2008).
Nagasawa, T. Microenvironmental niches in the bone marrow required for B-cell development. Nat. Rev. Immunol. 6, 107–116, doi: 10.1038/nri1780 (2006).
Semerad, C. L. et al. G-CSF potently inhibits osteoblast activity and CXCL12 mRNA expression in the bone marrow. Blood. 106, 3020–3027, doi: 10.1182/blood-2004-01-0272 (2005).
Noll, J. E. et al. Myeloma plasma cells alter the bone marrow microenvironment by stimulating the proliferation of mesenchymal stromal cells. Haematologica. 99, 163–171, doi: 10.3324/haematol.2013.090977 (2014).
Sawa, S. et al. Autoimmune arthritis associated with mutated interleukin (IL)-6 receptor gp130 is driven by STAT3/IL-7-dependent homeostatic proliferation of CD4+ T cells. J. Exp. Med. 203, 1459–1470, doi: 10.1084/jem.20052187 (2006).
Peschon, J. J. et al. Early lymphocyte expansion is severely impaired in interleukin 7 receptor-deficient mice. J. Exp. Med. 180, 1955–1960 (1994).
von Freeden-Jeffry, U. et al. Lymphopenia in interleukin (IL)-7 gene-deleted mice identifies IL-7 as a nonredundant cytokine. J. Exp. Med. 181, 1519–1526 (1995).
Dias, S., Silva, H., Jr., Cumano, A. & Vieira, P. Interleukin-7 is necessary to maintain the B cell potential in common lymphoid progenitors. J. Exp. Med. 201, 971–979, doi: 10.1084/jem.20042393 (2005).
Manilay, J. O. & Zouali, M. Tight relationships between B lymphocytes and the skeletal system. Trends Mol. Med. 20, 405–412, doi: 10.1016/j.molmed.2014.03.003 (2014).
Quach, J. M. et al. Myelosuppressive therapies significantly increase pro-inflammatory cytokines and directly cause bone loss. J. Bone Miner. Res. doi: 10.1002/jbmr.2415 (2014).
Takeshita, S., Kaji, K. & Kudo, A. Identification and characterization of the new osteoclast progenitor with macrophage phenotypes being able to differentiate into mature osteoclasts. J. Bone Miner. Res. 15, 1477–1488, doi: 10.1359/jbmr.2000.15.8.1477 (2000).
Yoshida, K. et al. Targeted disruption of gp130, a common signal transducer for the interleukin 6 family of cytokines, leads to myocardial and hematological disorders. Proc. Natl. Acad. Sci. USA 93, 407–411 (1996).
Kopf, M. et al. Pleiotropic defects of IL-6-deficient mice including early hematopoiesis, T and B cell function and acute phase responses. Ann. NY Acad. Sci. 762, 308–318 (1995).
Tanaka, M. et al. Targeted disruption of oncostatin M receptor results in altered hematopoiesis. Blood. 102, 3154–3162, doi: 10.1182/blood-2003-02-0367 (2003).
Escary, J. L., Perreau, J., Dumenil, D., Ezine, S. & Brulet, P. Leukaemia inhibitory factor is necessary for maintenance of haematopoietic stem cells and thymocyte stimulation. Nature. 363, 361–364, doi: 10.1038/363361a0 (1993).
Purton, L. E. et al. RARgamma is critical for maintaining a balance between hematopoietic stem cell self-renewal and differentiation. J. Exp. Med. 203, 1283–1293, doi: 10.1084/jem.20052105 (2006).
Bouxsein, M. L. et al. Guidelines for assessment of bone microstructure in rodents using micro-computed tomography. J. Bone Miner. Res. 25, 1468–1486, doi: 10.1002/jbmr.141 (2010).
Green, A. C. et al. RARgamma is a negative regulator of osteoclastogenesis. J. Steroid Biochem. Mol. Biol. 150, 46–53, doi: 10.1016/j.jsbmb.2015.03.005 (2015).
Acknowledgements
The authors would like to thank SVH BioResources Centre for care of experimental animals. This work was supported in part by grants from the National Health and Medical Research Council of Australia (NHMRC; to L.E.P.); NHMRC Career Development Award (L.E.P.); NHMRC Senior Research Fellowship (L.E.P.); Post-doctoral Fellowship from the Swedish Research Council (M.A.); and in part by the Victorian State Government Operational Infrastructure Support Program (to St. Vincent’s Institute). Generous support from the Ian Potter Foundation assisted with the purchase of the μCT and irradiator used in these studies.
Author information
Authors and Affiliations
Contributions
Study design: L.E.P. Study conduct: M.A., K.E.W., T.J., H.A.K., J.M.Q., E.K.B. and L.E.P. Data collection: M.A., K.E.W., T.J., H.A.K., J.M.Q., E.K.B. and L.E.P. Data analysis: M.A., K.E.W., T.J., H.A.K., J.M.Q., A.C.M., E.K.B., M.F.S. and L.E.P. Data interpretation: M.A., M.F.S., C.R.W. and L.E.P. Drafting manuscript: M.A. and L.E.P. Revising manuscript content: all authors. Approving final version of manuscript: all authors.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Askmyr, M., White, K., Jovic, T. et al. Ciliary neurotrophic factor has intrinsic and extrinsic roles in regulating B cell differentiation and bone structure. Sci Rep 5, 15529 (2015). https://doi.org/10.1038/srep15529
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep15529
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.