Abstract
Backround:
The target substrates of DNA mismatch recognising factors MutSα (MSH2+MSH6) and MutSβ (MSH2+MSH3) have already been widely researched. However, the extent of their functional redundancy and clinical substance remains unclear. Mismatch repair (MMR)-deficient tumours are strongly associated with microsatellite instability (MSI) and the degree and type of MSI seem to be dependent on the MMR gene affected, and is linked to its substrate specificities. Deficiency in MSH2 and MSH6 is associated with both mononucleotide and dinucleotide repeat instability. Although no pathogenic MSH3 mutations have been reported, its deficiency is also suggested to cause low dinucleotide repeat instability.
Methods:
To assess the substrate specificities and functionality of MutSα and MutSβ we performed an in vitro MMR assay using three substrate constructs, GT mismatch, 1 and 2 nucleotide insertion/deletion loops (IDLs) in three different cell lines.
Results:
Our results show that though MutSα alone seems to be responsible for GT and IDL1 repair, MutSα and MutSβ indeed have functional redundancy in IDL2 repair and in contrast with earlier studies, MutSβ seems to exceed MutSα.
Conclusion:
The finding is clinically relevant because the strong role of MutSβ in IDL2 repair indicates MSH3 deficiency in tumours with low dinucleotide and no mononucleotide repeat instability.
Similar content being viewed by others
Main
The five proteins involved in the human mismatch repair (MMR) mechanism to maintain genomic integrity function as heterodimers are MutLα (MLH1+PMS2), MutSα (MSH2+MSH6) and MutSβ (MSH2+MSH3). MMR proteins correct base/base mismatches and small insertion/deletion loops (IDLs) that arise on the newly synthesised strand during DNA replication and recombination. Larger loop structures (⩾5 nt) are believed to require a different combination of repair proteins and hence are not targets of the MMR mechanism (Umar et al, 1998). Approximately 25% of sporadic colon tumours, as well as a number of tumours of endometrium, ovary and some other organs and tissues, are deficient in MMR (Peltomäki, 2003). Moreover, germline mutations in MMR genes predispose to hereditary nonpolyposis colorectal cancer (HNPCC) syndrome/Lynch syndrome. To date, 659 MLH1 (44% of all identified MMR gene variations), 595 MSH2 (39%), 216 MSH6 (14%) and 45 PMS2 (3%) germline variations have been reported in the database (Woods et al, 2007; http://www.med.mun.ca/MMRvariants/). However, no HNPCC predisposing MSH3 mutations have yet been identified.
MMR-deficient tumours are strongly associated with microsatellite instability (MSI) (Aaltonen et al, 1993). However, the degree and type of MSI differ from high to low and between mono-, di-, tri- and tetranucleotide instability or elevated microsatellite alterations at selected tetranucleotide repeats (EMAST) (Peltomäki and Vasen, 2004; Plaschke et al, 2004; Haugen et al, 2008) depending on the MMR gene affected. MLH1- and MSH2-deficient tumours are characterised by both mono- and dinucleotide repeat instability, whereas the level of MSI is lower in MSH6-deficient tumours (Bhattacharyya et al, 1995; Papadopoulos et al, 1995). MSH6-deficient cells are unable to repair single base mismatches, whereas they retain proficiency to repair two, three and four base loops (Drummond et al, 1995; Risinger et al, 1996; Umar et al, 1997), thus, causing only mononucleotide repeat instability in tumours (Wagner et al, 2001; Plaschke et al, 2004). Recently, EMAST and also low dinucleotide repeat instability have been associated with MSH3 deficiency both in tumour cell lines and in sporadic colorectal tumours (Haugen et al, 2008).
The type of MSI seems to be dependent on the substrate specificities of the MMR protein affected. In human cells, the MMR process is initiated by the binding of the mismatch recognition factor MutSα or MutSβ to the mispair, followed by the initiation of the assembly of the repairosome by MutLα (Constantin et al, 2005; Zhang et al, 2005). MutSβ has a high binding affinity to IDLs but, in contrast, a very low affinity to simple base/base mispairs (Acharya et al, 1996; Palombo et al, 1996), whereas MutSα has been shown to bind and repair both base/base mispairs and IDLs (Drummond et al, 1995; Palombo et al, 1996). Lesion specificity is believed to lie within the MSH3/MSH6-specific sequences, which differ notably (Owen et al, 2009). The process through which ADP–ATP exchange occurs on MSH2 seems to be dependent on the protein it forms a complex with; MSH6 requires ATP stabilisation, whereas MSH3 requires ATP hydrolysis, both of which are dependent on specific lesion binding (Owen et al, 2009). However, findings based on assays analysing the binding properties of these MMR proteins do not yet prove their functional ability to repair the bound mismatches (Ou et al, 2007).
In this study, we applied the in vitro MMR assay to analyse the substrate specificities and functionality of MutSα and MutSβ using substrates, GT, IDL1 and IDL2 in three different cell lines. The in vitro MMR assay allows the functional analysis of all different MMR protein complexes and all kinds of missense variations in individual genes in a homologous human MMR system. In this study, the assay was for the first time applied to test the interference of an MSH3 variation with repair efficiency.
Materials and methods
Cell lines and nuclear extracts
Cancer cell lines HeLa, LoVo, HCT116 (American Type Culture Collection, Manassas, VA, USA) and GP5d (European Collection of Cell Cultures, Salisbury, UK) were cultured according to instructions of manufacturers. HeLa cells are MMR proficient, whereas HCT116, LoVo and GP5d cells are MMR deficient. HCT116 cells lack MLH1 and MSH3 (MSH3 is mutated as a consequence of the primary MMR defect) (Cannavo et al, 2005), whereas in LoVo cells, the MSH2 gene is inactivated causing a deficiency of MSH2, MSH3 and MSH6 proteins (Drummond et al, 1997). The lack of MSH2 has been associated with the proteolytic degradation of its counterparts MSH3 and MSH6 (Cannavo et al, 2005). GP5d cells are MMR deficient because of primary alterations in MSH2 and MLH3, resulting in lack of MSH6 and MSH3 proteins as well (Cannavo et al, 2005; di Pietro et al, 2005).
Nuclear proteins were extracted as described earlier (Lahue et al, 1989; Holmes et al, 1990). Approximately 2–10 × 108 cells were collected and treated with 30–40 ml of cold isotonic buffer (20 mM Hepes pH 7.5, 5 mM KCl, 1.5 mM MgCl, 250 mM sucrose, 0.2 mM PMSF, 1 × complete EDTA-free protease inhibitor mixture (Roche Diagnostics GmbH, Mannheim, Germany), 0.25 μg ml−1 aprotinin, 0.7 μg ml−1 pepstatin, 0.5 μg ml−1 leupeptin, 1 mM DTT). The cells were resuspended in cold hypotonic buffer (isotonic buffer without sucrose) followed by immediate pelleting. Approximately 1 ml per 1–2 × 108 cells of hypotonic buffer was used to disrupt the cell membranes with a syringe and a narrow-gauge needle. Nuclei were collected by centrifugation and suspended in cold extraction buffer (25 mM Hepes pH 7.5, 10% sucrose, 1 mM PMSF, 0.5 mM DTT, 1 μg ml−1 leupeptin) and NaCl up to 155 mM by rotation in +4°C for 1 h. The supernatant was dialysed for 2 h against cold dialysis buffer (25 mM Hepes pH 7.5, 50 mM KCl, 0.1 mM EDTA pH 8, 10% sucrose, 1 mM PMSF, 2 mM DTT, 1 μg ml−1 leupeptine) and collected after further centrifugation.
Preparation of heteroduplex molecules
The heteroduplex DNA molecule is a circular 3193 bp long molecule with a single-strand nick 445 bp upstream from the site of the mismatch. Three different heteroduplex constructs were prepared; a G–T mismatch (5′GT), and a single and two nucleotide IDLs (5′IDL1, 5′IDL2). Site-directed mutagenesis was carried out according to manufacturer's instructions (QuickChance Site-directed mutagenesis, Stratagene, La Jolla, CA, USA) to create the 1 nt (delA) and 2 nt (delAT) deletions to the positive pGEM IDL40 plasmid strand at the BglII restriction site. The GT mismatch was created by replacing adenine with guanine maintaining a thymine on the complementary strand. Single-stranded DNA was prepared by infecting pGEM IDL40 transformed XL1-blue bacteria cells with the M13K07 bacteriophage (Amersham Biosciences, Piscataway, NJ, USA), which replicates the antisense strand. Single-stranded DNA was extracted from the bacteriophages and used in excess to re-anneal with the linearised plasmid DNA creating heteroduplex molecules. Plasmid-safe DNAse and BND cellulose treatments were carried out to purify the final product.
Production of wild-type heterodimer protein complexes
Spodoptera frugiperda (Sf9) (Invitrogen, Carlsbad, CA, USA) insect cells were transfected with bacmid DNA carrying wild-type (WT) MSH2, MSH3, MSH6, PMS2 or MLH1 cDNA fragments. The cells were then re-infected to obtain a higher yield of recombinant baculoviruses (Nyström-Lahti et al, 2002). WT-recombinant baculoviruses were used to co-infect Sf9 cells for protein production forming the heterodimer complexes assayed: MutLα (MLH1+PMS2), MutSα (MSH2+MSH6) and MutSβ (MSH2+MSH3). The heterodimeric complexes were extracted as total protein extracts (TE) at 50 h (MutLα) or 72 h (MutSα and MutSβ) as described earlier (Kariola et al, 2002; Nyström-Lahti et al, 2002; Raevaara et al, 2004; Ollila et al, 2006).
MSH3 mutagenesis
The MSH3 missense mutation (c.2386 C>T, RefSeq NM 002439.2) was constructed with a PCR-based site-directed mutagenesis kit according to manufacturer's instructions (QuickChance Site-directed mutagenesis, Stratagene) substituting arginine with tryptophan in codon 796 (p.R796W). The mutated MSH3 cDNA was introduced into a pFastBac1 vector (Invitrogen) and sequenced (ABIPrism 3100 Genetic Analyzer; Applied Biosystems, Foster City, CA, USA). The primer sequences and PCR parameters are available on request. Proteins were produced and extracted from Sf9 cells as described in the previous paragraph.
Western blot analysis
Protein expression levels in the nuclear extracts (NEs) were studied by western blot analysis using 50 μg of NE and 0.1–5 μl of WT-TE by means of sodium dodecyl sulphate polyacrylamide gel electrophoresis. The proteins were blotted into nitrocellulose membranes (Hypond, PVDF, Amersham Pharmacia Biotech, Uppsala, Sweden), which were subsequently incubated with monoclonal antibodies anti-MSH2 (Calbiochem, San Diego, CA, USA, MSH2-Ab1, NA-26, 0.2 μg ml−1), anti-MSH3 (BD Transduction Laboratories, Lexington, KY, USA, M94120, 250 μg ml−1), anti-MSH6 (BD Transduction Laboratories, clone 44, 0.02 μg ml−1), anti-PMS2 (Calbiochem/Oncogene Research, San Diego, CA, USA, Ab-1, 0.2 μg ml−1) and anti-MLH1 (BD Biosciences/Pharmingen, San Diego, CA, USA, clone 168-15, 0.5 μg ml−1). Ubiquitously expressed α-tubulin was used as a loading control to estimate the MMR protein levels in the extracts (anti-α-tubulin; Sigma, Louis, MO, USA, DM1A, 0.2 μg ml−1).
The in vitro MMR assay
The roles of MutSα-WT and MutSβ-WT in 5′GT/5′IDL1/5′IDL2 repair were analysed by an in vitro MMR assay as described earlier (Nyström-Lahti et al, 2002). Repair reactions were standardised to include 75–100 μg of MMR-deficient NE (HCT116, LoVo or GP5d), or an equal amount of MMR-proficient HeLa extract. The excess amount of the heteroduplex DNA substrate (5′GT, 5′IDL1 or 5′IDL2) was set to 100 ng. The functionality of WT-proteins was assayed by complementing HCT116, LoVo and GP5d NEs with an appropriate amount of Sf9 total extract including the overexpressed MutLα-WT (50 ng), MutSα-WT (200 ng) or MutSβ-WT (600 ng). The amount of WT-protein in the reaction was titrated to obtain maximum repair efficiency in each cell line. Owing to the low PMS2 expression, GP5d NE was complemented with MutLα-WT in each reaction (Figure 1). MMR-proficient HeLa NE was used as a positive control, whereas uncomplemented NEs as well as extracts complemented with untransfected Sf9 proteins were used as negative controls. The substrates were linearised with Eco31I restriction enzyme. As the repair reaction converts a GT heteroduplex to an AT homoduplex or fills the 1 or 2 nt loop structures recreating the BglII restriction site, the repair efficiency can be measured by the efficiency of the double restriction. The functionality of mutated MSH3 TE was studied using 5′IDL2 substrate and GP5d NE. Repair percentages were analysed using Image-Pro 4.0 (Media Cybernetics, Silver Spring, MD, USA) and calculated as an average of three independent experiments. Statistical t-test analysis was carried out to evaluate the significance of the percentage differences observed between MutSα and MutSβ in IDL2 repair.
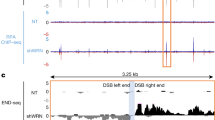
Western blot analysis of the MMR protein contents in the NEs used in the functional assay. HeLa, a positive control, includes all five MMR proteins, MLH1, PMS2, MSH2, MSH3 and MSH6. HCT116 lacks MLH1, PMS2 and MSH3. Both GP5d and LoVo lack MSH2, MSH3 and MSH6. As an assay control, Sf9 TE are included with and without the overexpressed WT MMR proteins. The loading control, α-tubulin is not shown.
Results
MMR protein contents of the cell lines used in the in vitro MMR assay
Western blot analysis was used to characterise the MMR protein contents in the cell lines used in the functional assay. The analysis confirmed the absence of MSH2, MSH6 and MSH3 in both LoVo and GP5d NEs, thus making them suitable for substrate specificity and functionality studies of MutSα and MutSβ (Figure 1). Owing to the significantly reduced level of PMS2 in GP5d NE, together with the MutS complex, it was complemented with MutLα-WT. HCT116 NE was shown to express only MSH6 and MSH2 presenting an opportunity to study the substrate specificity and repair efficiency of MutSβ (MSH3) and MutLα. The presence of all five MMR proteins in HeLa NE establishes its aptitude for functioning as a positive control.
The in vitro MMR assay elucidates the substrate specificities and repair efficiencies of MutSα and MutSβ
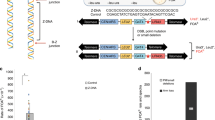
With the right selection of cell lines, the in vitro MMR assay allows the functional analysis of all different MMR protein complexes in a homologous human MMR system. Here, three different substrates, 5′GT, 5′IDL1 and 5′IDL2 were used to study the substrate specificities and repair efficiencies of MutSα and MutSβ. In contrast with MutLα, the presence of which is known to be vital for all these substrates, the type of MutS complex required for optimal repair efficiency is determined by the substrate construct. The MMR assay with LoVo, GP5d and HCT116, with various combinations of natural or complemented MutLα demonstrated that the role of MutSα is evident in the repair of 5′GT and 5′IDL1, whereas the repair of dinucleotide loops requires MutSβ for efficient repair (Figure 2). Remarkably, all three cell lines demonstrate more efficient dinucleotide repair with MutSβ than with MutSα. In HCT116, the mean repair efficiency was 26% higher with MutSβ than with MutSα (P=0.0014), in LoVo it was 14% higher (P=0.284) and in GP5d 5% higher (P=0.230).
MMR efficiency of HCT116, LoVo and GP5d NEs complemented with MutSα, MutSβ and MutLα complexes for 5′GT, 5′IDL1 and 5′IDL2 substrates. (A) Mock represents heteroduplex only, with no added NE or recombinant protein. MMR-proficient HeLa NE including all five MMR proteins is used as a positive control. MMR-deficient HCT116, LoVo and GP5d NEs and NEs complemented with Sf9 insect cell TE are used as negative controls. The top fragment (3193 bp) represents the unrepaired linearised heteroduplexes and the two lower fragments (1833 and 1360 bp) show the migration of the repaired and double-digested DNA molecules. The repair percentages (R%) represent fractions of repaired DNA calculated as a ratio of double-digested DNA relative to total DNA added to the reaction. Values are a mean of three independent experiments. (B) The comparison of substrate-specific repair efficiencies of the MMR protein complexes (repair efficiency R% and s.d.±%). MutSα is able to repair all three substrates (5′GT/5′IDL1/5′IDL2), whereas MutSβ does not repair 5′GT or 5′IDL1 in any extracts. However, complementation of HCT116 NE (lacking MLH1, PMS2 and MSH3) with MutLα alone yields a considerably lower IDL2 repair percentage (12%, s.d.±5%) than after co-complementation with MutLα and MutSβ (38%, s.d.±5%). Moreover, complementation of LoVo and GP5d NEs (lacking MSH2, MSH3 and MSH6) with MutSα yields lower IDL2 repair percentages, 17% (s.d.±17%) and 13% (s.d.±4%), than when complemented with MutSβ, 31% (s.d.±21%) and 18% (s.d.±9%), respectively.
The functional analysis of an MSH3 variation
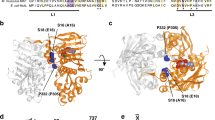
The in vitro MMR assay allows the functional analysis of all kinds of missense variations of the five different MMR genes. The strong role of MutSβ (MSH2+MSH3) in dinucleotide loop repair and the use of LoVo and GP5d NEs, which lack both MutSα and MutSβ, allow the functional analysis of MSH3 variations in a manner excluding false positives resulting from the presence of MutSα. In this study, for the first time, the assay was applied to test the effect of an MSH3 variation (MSH3-R796W) on its repair efficiency. The variation was found in a putative HNPCC family (unpublished). Our result suggests that the mutated MSH3-R796W protein is proficient with repair percentages of MSH3-WT 20% (s.d.±5%) and MSH3-R796W 18% (s.d.±8%) (P=0.358) (Figure 3).
Discussion
Using different substrate structures, the in vitro MMR assay is able to demonstrate differences in substrate specificities as well as in repair efficiencies of MutSα and MutSβ. The overlapping roles of these heterodimeric complexes have been reported earlier (Acharya et al, 1996; Genschel et al, 1998) generally emphasising the role of MutSα predominantly for the recognition of base/base mispairs and small IDLs and MutSβ for the recognition of larger (>2 bp) IDLs (Acharya et al, 1996; Palombo et al, 1996). Our experiments support the functional redundancy but contradictory to the previous impression, in this study, the repair efficiency of MutSβ was shown to exceed that of MutSα in the repair of dinucleotide loop structures.
The lack of a functional MMR mechanism causes MSI. HCT116 cells, which are deficient in MLH1 and MSH3, complemented with MLH1 through the addition of chromosome 3 have been shown to demonstrate mononucleotide repeat stability but still a low level of dinucleotide and a high level of tetranucleotide repeat instability suggesting a problem in MSH3. Although, the tetranucleotide repeat markers represented a level of instability five times higher than dinucleotide repeats supporting the functional overlap of MutSβ and MutSα in IDL2 repair, low dinucleotide repeat instability was caused by defected MutSβ (MSH3) (Haugen et al, 2008). The microsatellite stability was indeed reversible by complementing HCT116 cells with both chromosomes 3 and 5, hence expressing both lost proteins MLH1 and MSH3 (Haugen et al, 2008). In this study, MutSβ not only participated in IDL2 repair but exceeded the repair efficiency of MutSα proven in three different cell lines, HCT116, LoVo and GP5d. Although, HCT116 expressed a sufficient amount of MutSα to repair GT and IDL1 mismatches, the repair efficiency of IDL2 increased three-fold when the cells were complemented with MutSβ. An increase in repair efficiencies was also seen in LoVo and GP5d cells when complemented with MutSβ but the differences of repair efficiencies between MutSα and MutSβ were not statistically significant as in HCT116.
By selecting a cell line that lacks the analysed MMR protein, the in vitro MMR assay allows the functional analysis of all different MMR proteins and any missense mutation in an individual MMR gene. The assay has been applied earlier to a large number of MSH2/6 and MLH1 mutations using GT and IDL1 as target substrates (Nyström-Lahti et al, 2002; Kariola et al, 2004; Raevaara et al, 2005; Ollila et al, 2006). In this study, the finding of the strong role of MutSβ (MSH2+MSH3) in IDL2 repair enables efficient testing of MSH3 variations. By selecting LoVo and GP5d NEs, which lack both MutSα and MutSβ, the assay was adapted to study the functional significance of an MSH3 variation for the first time. Although the analysed variant was shown to be proficient in IDL2 repair, the assay itself functioned well suggesting its utility for further MSH3 testing.
In cancer diagnostics, the MSI phenotype has been a hallmark of HNPCC tumours. However, the levels have varied from high to low or to no MSI and between mono-, di-, tri- and tetranucleotide repeat instability dependent on the MMR gene affected and its substrate specificities. Generally, the MSI marker panel used in the diagnostics includes mono- and dinucleotide markers, and in MSI-positive cases, MLH1, MSH2 and MSH6 genes associated with mono- and dinucleotide repeat instability are analysed for mutations. Our results are clinically relevant emphasising the importance of MSH3 in dinucleotide loop repair and we encourage performing MSH3 mutation analysis when a tumour shows dinucleotide but no mononucleotide repeat instability.
Change history
16 November 2011
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Aaltonen LA, Peltomäki P, Leach FS, Sistonen P, Pylkkänen L, Mecklin JP, Järvinen H, Powell SM, Jen J, Hamilton SR, Petersen GM, Kinzler KW, Vogelstein B, de la Chapelle A (1993) Clues to the pathogenesis of familial colorectal cancer. Science 260: 812–816
Acharya S, Wilson T, Gradia S, Kane M, Guerrette S, Marsischky G, Kolodner R, Fishel R (1996) hMSH2 forms specific mispair-binding complexes with hMSH3 and hMSH6. Proc Natl Acad Sci USA 93: 13629–13634
Bhattacharyya NP, Ganesh A, Phear G, Richards B, Skandalis A, Meuth M (1995) Molecular analysis of mutations in mutator colorectal carcinoma cell lines. Hum Mol Genet 4: 2057–2064
Cannavo E, Marra G, Sabates-Bellver J, Menigatti M, Lipkin SM, Fischer F, Cejka P, Jiricny J (2005) Expression of the MutL homologue hMLH3 in human cells and its role in DNA mismatch repair. Cancer Res 65: 10759–10766
Constantin N, Dzantiev L, Kadyrov FA, Modrich P (2005) Human mismatch repair reconstitution of a nick-directed bidirectional reaction. J Biol Chem 280: 39752–39761
di Pietro M, Sabates Bellver J, Menigatti M, Bannwart F, Schnider A, Russell A, Truninger K, Jiricny J, Marra G (2005) Defective DNA mismatch repair determines a characteristic transcriptional profile in proximal colon cancers. Gastroenterology 129: 1047–1059
Drummond JT, Li GM, Longley MJ, Modrich P (1995) Isolation of an hMSH2-p160 heterodimer that restores DNA mismatch repair to tumor cells. Science 268: 1909–1912
Drummond JT, Genschel J, Wolf E, Modrich P (1997) DHFR/MSH3 amplification in methotrexate-resistant cells alters the hMutSalpha/hMutSbeta ratio and reduces the efficiency of base-base mismatch repair. Proc Natl Acad Sci USA 94: 10144–10149
Genschel J, Littman SJ, Drummond JT, Modrich P (1998) Isolation of MutSbeta from human cells and comparison of the mismatch repair specificities of MutSbeta and MutSalpha. J Biol Chem 31: 19895–19901
Haugen AC, Goel A, Yamada K, Marra G, Nguyen TP, Nagasaka T, Kanazawa S, Koike J, Kikuchi Y, Zhong X, Arita M, Shibuya K, Oshimura M, Hemmi H, Boland CR, Koi M (2008) Genetic instability caused by loss of MutS homologue 3 in human colorectal cancer. Cancer Res 68: 8465–8472
Holmes Jr J, Clark S, Modrich P (1990) Strand-specific mismatch correction in nuclear extracts of human and Drosophila melanogaster cell lines. Proc Natl Acad Sci USA 87: 5837–5841
Kariola R, Raevaara TE, Lönnqvist KE, Nyström-Lahti M (2002) Functional analysis of MSH6 mutations linked to kindreds with putative hereditary non-polyposis colorectal cancer syndrome. Hum Mol Genet 11: 1303–1310
Kariola R, Hampel H, Frankel WL, Raevaara TE, de la Chapelle A, Nyström-Lahti M (2004) MSH6 missense mutations are often associated with no or low cancer susceptibility. Br J Cancer 91: 1287–1292
Lahue RS, Au KG, Modrich P (1989) DNA mismatch correction in a defined system. Science 245: 160–164
Nyström-Lahti M, Perrera C, Räschle M, Panyushkina-Seiler E, Marra G, Curci A, Ouaresima B, Constanzo F, D'Urso M, Venuta S, Jiricny J (2002) Functional analysis of MLH1 mutations linked to hereditary nonpolyposis colon cancer. Genes Chromosomes Cancer 33: 160–167
Ollila S, Sarantaus L, Kariola R, Chan P, Hampel H, Holinski-Feder E, Macrae F, Kohonen-Corish M, Gerdes AM, Peltomäki P, Mangold E, de la Chapelle A, Greenblatt M, Nyström M (2006) Pathogenicity of MSH2 missense mutations is typically associated with impaired repair capability of the mutated protein. Gastroenterology 131: 1408–1417
Ou J, Niessen RC, Lützen A, Sijmons RH, Kleibeuker JH, de Wind N, Rasmussen LJ, Hofstra RM (2007) Functional analysis helps to clarify the clinical importance of unclassified variants in DNA mismatch repair genes. Hum Mutat 28: 1047–1054
Owen BA, H Lang W, McMurray CT (2009) The nucleotide binding dynamics of human MSH2-MSH3 are lesion dependent. Nat Struct Mol Biol 16: 550–557
Papadopoulos N, Leach FS, Kinzler KW, Vogelstein B (1995) Monoallelic mutation analysis (MAMA) for identifying germline mutations. Nat Genet 11: 99–102
Palombo F, Iaccarino I, Nakajima E, Ikejima M, Shimada T, Jiricny J (1996) hMutSb, a heterodimer of hMSH2 and hMSH3, binds to insertion/deletion loops in DNA. Curr Biol 6: 1181–1184
Peltomäki P (2003) Role of DNA mismatch repair defects in the pathogenesis of human cancer. J Clin Oncol 21: 174–179
Peltomäki P, Vasen H (2004) Mutations associated with HNPCC predisposition – Update of ICG-HNPCC/INSiGHT mutation database. Dis Markers 20: 269–276
Plaschke J, Engel C, Kruger S, Holinski-Feder E, Pagenstecher C, Mangold E, Moeslein G, Schulmann K, Gebert J, von Knebel Doeberitz M, Ruschoff J, Loeffler M, Schackert HK (2004) Lower Incidence of Colorectal Cancer and Later Age of Disease Onset in 27 Families With MLH1 or MSH2 Mutations: The German Hereditary Nonpolyposis Colorectal Cancer Consortium. J Clin Oncol 22: 4486–4494
Raevaara TE, Gerdes AM, Lönnqvist KE, Tybjaerg-Hansen A, Abdel-Rahman WM, Kariola R, Peltomäki P, Nyström-Lahti M (2004) HNPCC mutation MLH1 P648S makes the functional protein unstable and homozygosity predisposes to mild neurofibromatosis type 1. Genes Chromosomes Cancer 40: 261–265
Raevaara TE, Korhonen MK, Lohi H, Hampel H, Lynch E, Lönnqvist KE, Holinski-Feder E, Sutter C, McKinnon W, Duraisamy S, Gerdes AM, Peltomäki P, Kohonen-Ccorish M, Mangold E, Macrae F, Greenblatt M, de la Chapelle A, Nyström M (2005) Functional significance and clinical phenotype of nontruncating mismatch repair variants of MLH1. Gastroenterology 129: 537–549
Risinger JI, Umar A, Boyd J, Berchuck A, Kunkel TA, Barrett JC (1996) Mutation of MSH3 in endometrial cancer and evidence for its functional role in heteroduplex repair. Nat Genet 14: 102–105
Umar A, Koi M, Risinger JI, Glaab WE, Tindall KR, Kolodner RD, Boland CR, Barrett JC, Kunkel TA (1997) Correction of hypermutability, N-methyl-N′-nitro-N-nitrosoguanidine resistance, and defective DNA mismatch repair by introducing chromosome 2 into human tumor cells with mutations in MSH2 and MSH6. Cancer Res 57: 3949–3955
Umar A, Risinger JI, Glaab WE, Tidall KR, Barrett JC, Kunkel TA (1998) Functional overlap in mismatch repair by human MSH3 and MSH6. Genetics 148: 1637–1646
Wagner A, Hendriks Y, Meijers-Heijboer EJ, de Leeuw WJ, Morreau H, Hofstra R, Tops C, Bik E, Bröcker-Vriends AH, van Der Meer C, Lindhout D, Vasen HF, Breuning MH, Cornelisse CJ, van Krimpen C, Niermeijer MF, Zwinderman AH, Wijnen J, Fodde R (2001) Atypical HNPCC owing to MSH6 germline mutations: analysis of a large Dutch pedigree. J Med Genet 38: 318–322
Woods MO, Williams P, Careen A, Edwards L, Bartlett S, McLaughlin J, Younghusband HB (2007) A new variant database for mismatch repair genes associated with Lynch syndrome. Hum Mut 28: 669–673
Zhang Y, Yuan F, Presnell SR, Tian K, Gao Y, Tomkinson AE, Gu L, Li G-M (2005) Reconstitution of 5′-directed human mismatch repair in a purified system. Cell 122: 693–705
Acknowledgements
We thank Professor Josef Jiricny for providing the pGEM IDL40 plasmid. This study was supported by grants from the Academy of Finland, grant number 110300; the Sigrid Juselius Foundation; the European Community 7th Framework Program; The Research Foundation of the University of Helsinki; Finnish Cancer Organisations; and Krebsliga beider Basel.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Kantelinen, J., Kansikas, M., Korhonen, M. et al. MutSβ exceeds MutSα in dinucleotide loop repair. Br J Cancer 102, 1068–1073 (2010). https://doi.org/10.1038/sj.bjc.6605531
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6605531
Keywords
This article is cited by
-
Loss of MSH2 and MSH6 due to heterozygous germline defects in MSH3 and MSH6
Familial Cancer (2017)
-
Agenesis of the corpus callosum and gray matter heterotopia in three patients with constitutional mismatch repair deficiency syndrome
European Journal of Human Genetics (2013)
-
A putative Lynch syndrome family carrying MSH2 and MSH6 variants of uncertain significance—functional analysis reveals the pathogenic one
Familial Cancer (2011)