Abstract
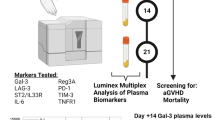
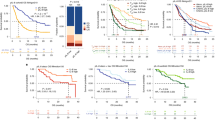
Early molecular response (EMR, BCR-ABL1 (IS)⩽10% at 3 months) is a strong predictor of outcome in imatinib-treated chronic phase chronic myeloid leukemia (CP-CML) patients, but for patients who transform early, 3 months may be too late for effective therapeutic intervention. Here, we employed multiplex cytokine profiling of plasma samples to test newly diagnosed CP-CML patients who subsequently received imatinib treatment. A wide range of pro-inflammatory and angiogenesis-promoting cytokines, chemokines and growth factors were elevated in the plasma of CML patients compared with that of healthy donors. Most of these normalized after tyrosine kinase inhibitor treatment while others remained high in remission samples. Importantly, we identified TGF-α and IL-6 as novel biomarkers with high diagnostic plasma levels strongly predictive of subsequent failure to achieve EMR and deep molecular response, as well as transformation to blast crisis and event-free survival. Interestingly, high TGF-α alone can also delineate a poor response group raising the possibility of a pathogenic role. This suggests that the incorporation of these simple measurements to the diagnostic work-up of CP-CML patients may enable therapy intensity to be individualized early according to the cytokine-risk profile of the patient.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Hochhaus A, O'Brien SG, Guilhot F, Druker BJ, Branford S, Foroni L et al. Six-year follow-up of patients receiving imatinib for the first-line treatment of chronic myeloid leukemia. Leukemia 2009; 23: 1054–1061.
Saglio G, Kim DW, Issaragrisil S, le Coutre P, Etienne G, Lobo C et al. Nilotinib versus imatinib for newly diagnosed chronic myeloid leukemia. N Engl J Med 2010; 362: 2251–2259.
Kantarjian H, Shah NP, Hochhaus A, Cortes J, Shah S, Ayala M et al. Dasatinib versus imatinib in newly diagnosed chronic-phase chronic myeloid leukemia. N Engl J Med 2010; 362: 2260–2270.
Marin D, Ibrahim AR, Lucas C, Gerrard G, Wang L, Szydlo RM et al. Assessment of BCR-ABL1 transcript levels at 3 months is the only requirement for predicting outcome for patients with chronic myeloid leukemia treated with tyrosine kinase inhibitors. J Clin Oncol 2012; 30: 232–238.
Hanfstein B, Muller MC, Hehlmann R, Erben P, Lauseker M, Fabarius A et al. Early molecular and cytogenetic response is predictive for long-term progression-free and overall survival in chronic myeloid leukemia (CML). Leukemia 2012; 26: 2096–2102.
Branford S, Yeung DT, Ross DM, Prime JA, Field CR, Altamura HK et al. Early molecular response and female sex strongly predict stable undetectable BCR-ABL1, the criteria for imatinib discontinuation in patients with CML. Blood 2013; 121: 3818–3824.
Yeung DT, Osborn MP, White DL, Branford S, Braley J, Herschtal A et al. TIDEL-II: frontline use of imatinib in CML with early switch to nilotinib for failure to achieve time-dependent molecular targets. Blood 2015; 125: 915–923.
Hughes TP, Saglio G, Kantarjian HM, Guilhot F, Niederwieser D, Rosti G et al. Early molecular response predicts outcomes in patients with chronic myeloid leukemia in chronic phase treated with frontline nilotinib or imatinib. Blood 2014; 123: 1353–1360.
Marin D, Hedgley C, Clark RE, Apperley J, Foroni L, Milojkovic D et al. Predictive value of early molecular response in patients with chronic myeloid leukemia treated with first-line dasatinib. Blood 2012; 120: 291–294.
Tefferi A, Vaidya R, Caramazza D, Finke C, Lasho T, Pardanani A . Circulating interleukin (IL)-8, IL-2R, IL-12, and IL-15 levels are independently prognostic in primary myelofibrosis: a comprehensive cytokine profiling study. J Clin Oncol 2011; 29: 1356–1363.
Pardanani A, Finke C, Lasho TL, Al-Kali A, Begna KH, Hanson CA et al. IPSS-independent prognostic value of plasma CXCL10, IL-7 and IL-6 levels in myelodysplastic syndromes. Leukemia 2012; 26: 693–699.
Kornblau SM, McCue D, Singh N, Chen W, Estrov Z, Coombes KR . Recurrent expression signatures of cytokines and chemokines are present and are independently prognostic in acute myelogenous leukemia and myelodysplasia. Blood 2010; 116: 4251–4261.
Reynaud D, Pietras E, Barry-Holson K, Mir A, Binnewies M, Jeanne M et al. IL-6 controls leukemic multipotent progenitor cell fate and contributes to chronic myelogenous leukemia development. Cancer Cell 2011; 20: 661–673.
Zhang B, Ho Yin W, Huang Q, Maeda T, Lin A, Lee S-u et al. Altered microenvironmental regulation of leukemic and normal stem cells in chronic myelogenous leukemia. Cancer Cell 2012; 21: 577–592.
Hantschel O, Gstoettenbauer A, Colinge J, Kaupe I, Bilban M, Burkard TR et al. The chemokine interleukin-8 and the surface activation protein CD69 are markers for Bcr-Abl activity in chronic myeloid leukemia. Mol Oncol 2008; 2: 272–281.
Johnson WE, Li C, Rabinovic A . Adjusting batch effects in microarray expression data using empirical Bayes methods. Biostatistics 2007; 8: 118–127.
Breiman L . Random forests. Mach Learn 2001; 45: 5–32.
Liaw A, Wiener M . Classification and regression by randomForest. R News 2002; 2: 18–22.
Breiman L, Friedman J, Olshen R, Stone C . Classification and Regression Trees. Wadsworth, 1984.
Therneau T, Atkinson B, Ripley B rpart: Recursive Partitioning and Regression Trees. R package version 4.1-5; 2014, Available on: http://CRAN.R-project.org/package=rpart.
Williams G . Data Mining with Rattle and R: The Art of Excavating Data for Knowledge Discovery, Use R!. Springer, 2011.
Branford S, Yeung DT, Parker WT, Roberts ND, Purins L, Braley JA et al. Prognosis for patients with CML and >10% BCR-ABL1 after 3 months of imatinib depends on the rate of BCR-ABL1 decline. Blood 2014; 124: 511–518.
Schmidt T, Masouleh Behzad K, Loges S, Cauwenberghs S, Fraisl P, Maes C et al. Loss or inhibition of stromal-derived PlGF prolongs survival of mice with imatinib-resistant Bcr-Abl1+ leukemia. Cancer Cell 2011; 19: 740–753.
Diakos CI, Charles KA, McMillan DC, Clarke SJ . Cancer-related inflammation and treatment effectiveness. Lancet Oncol 2014; 15: e493–e503.
Hanahan D, Weinberg RA . Hallmarks of cancer: the next generation. Cell 2011; 144: 646–674.
Coussens LM, Werb Z . Inflammation and cancer. Nature 2002; 420: 860–867.
Mantovani A, Allavena P, Sica A, Balkwill F . Cancer-related inflammation. Nature 2008; 454: 436–444.
Braig M, Pallmann N, Preukschas M, Steinemann D, Hofmann W, Gompf A et al. A 'telomere-associated secretory phenotype' cooperates with BCR-ABL to drive malignant proliferation of leukemic cells. Leukemia 2014; 28: 2028–2039.
Gallipoli P, Pellicano F, Morrison H, Laidlaw K, Allan EK, Bhatia R et al. Autocrine TNF-α production supports CML stem and progenitor cell survival and enhances their proliferation. Blood 2013; 122: 3335–3339.
Verstovsek S, Kantarjian H, Manshouri T, Cortes J, Giles FJ, Rogers A et al. Prognostic significance of cellular vascular endothelial growth factor expression in chronic phase chronic myeloid leukemia. Blood 2002; 99: 2265–2267.
Korkolopoulou P, Viniou N, Kavantzas N, Patsouris E, Thymara I, Pavlopoulos PM et al. Clinicopathologic correlations of bone marrow angiogenesis in chronic myeloid leukemia: a morphometric study. Leukemia 2003; 17: 89–97.
Aguayo A, Kantarjian H, Manshouri T, Gidel C, Estey E, Thomas D et al. Angiogenesis in acute and chronic leukemias and myelodysplastic syndromes. Blood 2000; 96: 2240–2245.
Negaard HF, Iversen N, Bowitz-Lothe IM, Sandset PM, Steinsvik B, Ostenstad B et al. Increased bone marrow microvascular density in haematological malignancies is associated with differential regulation of angiogenic factors. Leukemia 2009; 23: 162–169.
Janowska-Wieczorek A, Majka M, Marquez-Curtis L, Wertheim JA, Turner AR, Ratajczak MZ . Bcr-abl-positive cells secrete angiogenic factors including matrix metalloproteinases and stimulate angiogenesis in vivo in Matrigel implants. Leukemia 2002; 16: 1160–1166.
Chiodoni C, Iezzi M, Guiducci C, Sangaletti S, Alessandrini I, Ratti C et al. Triggering CD40 on endothelial cells contributes to tumor growth. J Exp Med 2006; 203: 2441–2450.
Konopleva MY, Jordan CT . Leukemia stem cells and microenvironment: biology and therapeutic targeting. J Clin Oncol 2011; 29: 591–599.
Zhang B, Li M, McDonald T, Holyoake TL, Moon RT, Campana D et al. Microenvironmental protection of CML stem and progenitor cells from tyrosine kinase inhibitors through N-Cadherin and Wnt-β-catenin signaling. Blood 2013; 121: 1824–1838.
Naka K, Hoshii T, Muraguchi T, Tadokoro Y, Ooshio T, Kondo Y et al. TGF-beta-FOXO signalling maintains leukaemia-initiating cells in chronic myeloid leukaemia. Nature 2010; 463: 676–680.
Kreutzman A, Rohon P, Faber E, Indrak K, Juvonen V, Kairisto V et al. Chronic myeloid leukemia patients in prolonged remission following Interferon-alpha monotherapy have distinct cytokine and oligoclonal lymphocyte profile. PLoS One 2011; 6: e23022.
Mauer J, Denson JL, Bruning JC . Versatile functions for IL-6 in metabolism and cancer. Trends Immunol 2015; 36: 92–101.
Panteli KE, Hatzimichael EC, Bouranta PK, Katsaraki A, Seferiadis K, Stebbing J et al. Serum interleukin (IL)-1, IL-2, sIL-2Ra, IL-6 and thrombopoietin levels in patients with chronic myeloproliferative diseases. Br J Haematol 2005; 130: 709–715.
Bhatia R, McGlave PB, Dewald GW, Blazar BR, Verfaillie CM . Abnormal function of the bone marrow microenvironment in chronic myelogenous leukemia: role of malignant stromal macrophages. Blood 1995; 85: 3636–3645.
Rosean TR, Tompkins VS, Olivier AK, Sompallae R, Norian LA, Morse HC 3rd et al. The tumor microenvironment is the main source of IL-6 for plasma cell tumor development in mice. Leukemia 2014; 29: 233–237.
Huang WH, Chang MC, Tsai KS, Hung MC, Chen HL, Hung SC . Mesenchymal stem cells promote growth and angiogenesis of tumors in mice. Oncogene 2013; 32: 4343–4354.
Ishikawa N, Daigo Y, Takano A, Taniwaki M, Kato T, Hayama S et al. Increases of amphiregulin and transforming growth factor-alpha in serum as predictors of poor response to gefitinib among patients with advanced non-small cell lung cancers. Cancer Res 2005; 65: 9176–9184.
Masago K, Fujita S, Hatachi Y, Fukuhara A, Sakuma K, Ichikawa M et al. Clinical significance of pretreatment serum amphiregulin and transforming growth factor-alpha, and an epidermal growth factor receptor somatic mutation in patients with advanced non-squamous, non-small cell lung cancer. Cancer Sci 2008; 99: 2295–2301.
Addison CL, Ding K, Zhao H, Le Maitre A, Goss GD, Seymour L et al. Plasma transforming growth factor alpha and amphiregulin protein levels in NCIC Clinical Trials Group BR.21. J Clin Oncol 2010; 28: 5247–5256.
Zhang H, Li H, Xi HS, Li S . HIF1α is required for survival maintenance of chronic myeloid leukemia stem cells. Blood 2012; 119: 2595–2607.
Dreux AC, Lamb DJ, Modjtahedi H, Ferns GA . The epidermal growth factor receptors and their family of ligands: their putative role in atherogenesis. Atherosclerosis 2006; 186: 38–53.
Lanaya H, Natarajan A, Komposch K, Li L, Amberg N, Chen L et al. EGFR has a tumour-promoting role in liver macrophages during hepatocellular carcinoma formation. Nat Cell Biol 2014; 16: 972–981.
Pesonen K, Viinikka L, Myllyla G, Kiuru J, Perheentupa J . Characterization of material with epidermal growth factor immunoreactivity in human serum and platelets. J Clin Endocrinol Metab 1989; 68: 486–491.
MacNeil S, Dawson RA, Crocker G, Barton CH, Hanford L, Metcalfe R et al. Extracellular calmodulin and its association with epidermal growth factor in normal human body fluids. J Endocrinol 1988; 118: 501–509.
Schreiber AB, Winkler ME, Derynck R . Transforming growth factor-alpha: a more potent angiogenic mediator than epidermal growth factor. Science 1986; 232: 1250–1253.
Ebner R, Derynck R . Epidermal growth factor and transforming growth factor-alpha: differential intracellular routing and processing of ligand-receptor complexes. Cell regulation 1991; 2: 599–612.
Roepstorff K, Grandal MV, Henriksen L, Knudsen SL, Lerdrup M, Grovdal L et al. Differential effects of EGFR ligands on endocytic sorting of the receptor. Traffic 2009; 10: 1115–1127.
Acknowledgements
We thank Verity Saunders, Jarrad Goyne, Amity Frede and Jenny McLean for excellent technical assistance with patient sample processing and Bob Mirzai for excellent technical help with TGF-α immunocytochemistry. This study was supported by an NH&MRC Project Grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
JR is a Novartis Shareholder. DTY and TPH receive honoraria and research funding from Novartis Oncology, Bristol-Myers Squibb and Ariad. DLW receives research funding from Novartis Oncology, Bristol-Myers Squibb and Ariad. MB and GV are employed by CSL Limited, and SJB was employed by CSL Limited. EN, CHK, DBW, KF, WNE, TS, RG, AFL and DKH declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Rights and permissions
About this article
Cite this article
Nievergall, E., Reynolds, J., Kok, C. et al. TGF-α and IL-6 plasma levels selectively identify CML patients who fail to achieve an early molecular response or progress in the first year of therapy. Leukemia 30, 1263–1272 (2016). https://doi.org/10.1038/leu.2016.34
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2016.34
This article is cited by
-
Interleukin-9 production by type 2 innate lymphoid cells induces Paneth cell metaplasia and small intestinal remodeling
Nature Communications (2023)
-
Clonal haematopoiesis and dysregulation of the immune system
Nature Reviews Immunology (2023)
-
Mast cell deficiency prevents BCR::ABL1 induced splenomegaly and cytokine elevation in a CML mouse model
Leukemia (2023)
-
Comparative expression analysis of dasatinib and ponatinib-regulated lncRNAs in chronic myeloid leukemia and their network analysis
Medical Oncology (2022)
-
Therapy Resistance and Disease Progression in CML: Mechanistic Links and Therapeutic Strategies
Current Hematologic Malignancy Reports (2022)