Abstract
Background/Objectives:
Semisolid formulae are increasingly used in Japan to reduce the risks of gastroesophageal reflux (GER) and aspiration pneumonia in patients undergoing percutaneous endoscopic gastrostomy (PEG). We compared the incidences of GER after the use of liquid or semisolid contrast agents during PEG.
Subjects/Methods:
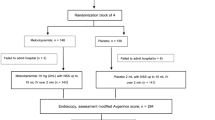
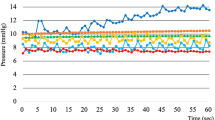
Patients who planned to undergo PEG were randomly assigned to the liquid-first (LF) group (liquid contrast agent on day 1 after PEG and a semisolid contrast agent on day 2) or the semisolid-first (SF) group (reversed order). A 200-ml agent bolus was administered via a PEG tube to the patient in the supine position. The upper gastrointestinal tract was radiologically examined from onset to 1 min after the end of administration. The incidences of GER were compared. We also evaluated the daily changes in GER incidence, effect of hiatal hernia severity and adverse events.
Results:
We analyzed the results of 66 patients (32, LF group; 34, SF group). The incidence of GER observed using only liquid contrast was 27% (18/66) and that using only semisolid was 11% (7/66) (P=0.028). There was no difference in the GER incidences between day 1 and day 2. In patients with severe, mild and no hiatal hernia, GER incidences in the liquid contrast agent were 80% (4/5), 61% (11/18) and 33% (13/43), respectively (P=0.031). GER incidence after using the semisolid contrast agent was lower in patients with no and mild hiatal hernia. The predominant adverse event was diarrhea; aspiration was not observed.
Conclusions:
Semisolid contrast agents reduced the incidence of GER after PEG.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Johnson DA, Hacker JF III, Benjamin SB, Ciarleglio CA, Chobanian SJ, Van Ness MM et al. Percutaneous endoscopic gastrostomy effects on gastroesophageal reflux and the lower esophageal sphincter. Am J Gastroenterol 1987; 82: 622–624.
McClave SA, Lukan JK, Stefater JA, Lowen CC, Looney SW, Matheson PJ et al. Poor validity of residual volumes as a marker for risk of aspiration in critically ill patients. Crit Care Med 2005; 33: 324–330.
Pick N, McDonald A, Benet N, Litsche M, Dietsche L, Legerwood R et al. Pulmonary aspiration in a long-term care setting: clinical and laboratory observations and an analysis of risk factors. J Am Geriatr Soc 1996; 44: 763–768.
Bourdel-Marchasson I, Dumas F, Pinganaud G, Emeriau JP, Decamps A . Audit of percutaneous endoscopic gastrostomy in long-term enteral feeding in a nursing home. Int J Qual Health Care 1997; 9: 297–302.
Langmore SE, Terpening MS, Schork A, Chen Y, Muray JT, Lopatin D et al. Predictors of aspiration pneumonia: how important is dysphagia? Dyspagia 1998; 13: 69–81.
Kanie J, Suzuki Y, Iguchi A, Akatsu H, Yamamoto T, Shimokata H . Prevention of gastroesophageal reflux using an application of half-solid nutrients in patients with percutaneous endoscopic gastrostomy feeding. J Am Geriatr Soc 2004; 52: 466–467.
Nishiwaki S, Araki H, Shirakami Y, Kawaguchi J, Kawade N, Iwashita M et al. Inhibition of gastroesophageal reflux by semisolid nutrients in patients with percutaneous endoscopic gastrostomy. J Parenter Enteral Nutr 2009; 33: 513–519.
Shimizu A, Moritani I, Hashimoto A . Prediction of pneumonia after percutaneous endoscopic gastrostomy-comparison endoscopic findings with radiographic findings [in Japanese]. Home Health Care Endoscopic Therapy and Quality of Life 2006; 10: 2–7.
Muramatsu H, Inomata H, Nagashima H, Nozawa E, Nishino M, Numata T et al. The gastroesophageal reflux influences the incidence of acute pneumonia after percutaneous endoscopic gastrostomy (PEG) and survival [in Japanese]. Home Health Care, Endoscopic Therapy and Quality of Life 2006; 10: 17–22.
Kusano M, Kouzu T, Kawano T, Ohara S . The prevalence of hiatus hernia in the Japanese [in Japanese]. Gastroenterol Endosc 2005; 47: 962–973.
O'Donell LJ, Virjee J, Heaton KW . Detection of pseudodiarrhoea by simple clinical assessment of intestinal transit rate. BMJ 1990; 300: 439–440.
Adachi K, Furuta K, Morita T, Nakata S, Ohara S, Tanimura T et al. Half-solidification of nutrient does not decrease gastro-esophageal reflux events in patients fed via percutaneous endoscopic gastrostomy. Clin Nutr 2009; 28: 648–651.
Pati MG, Goldberg HI, Arcerito M, Bortolasi L, Tong J, Way LW . Hiatal hernia size affects lower esophageal sphincter function, esophageal acid exposure, and the degree of mucosal injury. Am J Surg 1996; 171: 182–186.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Shimizu, A., Muramatsu, H., Kura, T. et al. Incidence of gastroesophageal reflux associated with percutaneous endoscopic gastrostomy contrast agent viscosity: a randomized controlled crossover trial. Eur J Clin Nutr 70, 1057–1061 (2016). https://doi.org/10.1038/ejcn.2016.76
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2016.76
This article is cited by
-
Differences in the incidence of postoperative pneumonia after percutaneous endoscopic gastrostomy between liquid and semi-solid nutrient administration
European Journal of Clinical Nutrition (2019)