Abstract
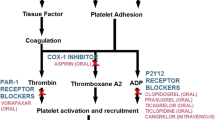
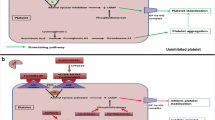
The benefits of aspirin use in the emergent care of MI and stroke have been well established. Recent studies have further demonstrated the importance of antiplatelet therapy in the acute setting, primarily with the use of intravenous glycoprotein IIb/IIIa receptor inhibitors. Aspirin and the thienopyridines (ticlopidine and clopidogrel) are oral antiplatelet agents that interfere with platelet activation in complementary, but separate pathways. Combination therapy of clopidogrel and aspirin has demonstrated benefit for the management of acute coronary syndromes, ischemic cerebrovascular disease and peripheral vascular disease in several large trials [1,2]. This article reviews the pathophysiology of platelet activation, landmark trials on oral antiplatelet agents, and the current recommendation for the use of oral antiplatelet agents in the emergency department
Similar content being viewed by others
References
Bertrand ME, Rupprecht HJ, Urban P, Gershlick AH, Investigators.Double-blind study of the safety of clopidogrel with and without a loading dose in combination with aspirin compared with ticlopidine in combination with aspirin after coronary stenting: The clopidogrel aspirin stent international cooperative study (CLASSICS). Circulation 2000;102:624–629.
Yusuf S, Zhao F, Mehta SR, et al. Effects of clopidogrel in addition to aspirin in patients with acute coronary syndromes without ST-segment elevation. N Engl J Med 2001;345:494–502.
Collaborative overview of randomised trials of antiplatelet therapy-I: Prevention of death, myocardial infarction, and stroke by prolonged antiplatelet therapy in various categories of patients. Antiplatelet Trialists' Collaboration. Bmj 1994;308:81–106.
Risk of myocardial infarction and death during treatment with low dose aspirin and intravenous heparin in men with unstable coronary artery disease. The RISC Group. Lancet 1990;336:827–830.
Lewis HD, Jr., Davis JW, Archibald DG, et al. Protective effects of aspirin against acute myocardial infarction and death in men with unstable angina. Results of a Veterans Administration Cooperative Study. N Engl J Med 1983;309:396–403.
CAPTURE Investigators. Randomized placebo controlled trial of abciximab before and during coronary intervention in refractory unstable angina: The CAPTURE study. Lancet 1997;349:1429–1435.
EPILOG Investigators. Platelet glycoprotein IIb/IIIa receptor blockade and low-dose heparin during percutaneous coronary revascularization. N Engl JMed 1997;336:1689–1696.
PRISM Investigators. A comparison of aspirin plus tirofiban with aspirin plus heparin for unstable angina.N Engl J Med 1998;338:1498–1505.
PRISM-PLUS Investigators. Inhibition of the platelet glycoprotein IIb/IIIa receptor with tirofiban in unstable angina and non-Q-wave myocardial infarction. N Engl J Med 1998;338:1488–1497.
PURSUIT Investigators. Inhibition of platelet glycoprotein IIb/IIIa with eptifibatide in patients with acute coronary syndromes. The PURSUIT Trial Investigators. Platelet Glycoprotein IIb/IIIa in Unstable Angina: Receptor Suppression Using Integrilin Therapy. N Engl J Med 1998;339:436–443.
RESTORE Investigators. Effects of platelet glycoprotein IIb/IIIa bolckade with tirofiban on adverse cardiac events in patients with unstable angina or acute myocardial infarction undergoing coronary angioplasty. Circulation 1997;96:1445–1453.
EPISTENT Investigators. Randomized placebo-controlled and balloon angioplasty controlled trial to assess safety of coronary stenting with use of platelet glycoprotein IIb/IIIa blockade. Lancet 1998;352:87–92.
Theroux P, Fuster V. Acute coronary syndromes: Unstable angina and non-Q-wavemyocardial infarction. Circulation 1998;97:1195–1206.
Randomized trial of intravenous streptokinase, oral aspirin, both, or neither among 17,187 cases of suspected acute myocardial infarction: ISIS-2.ISIS-2 (Second International Study of Infarct Survival) Collaborative Group. J Am Coll Cardiol 1988;12:3A–13A.
Patrono C, Coller B, Dalen JE, et al. Platelet-active drugs: The relationships among dose, effectiveness, and side effects. Chest 2001;119:39S–63S.
CAPRIE Investigators. A randomised, blinded, trial of clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE). CAPRIE Steering Committee. Lancet 1996;348:1329–1339.
Savi P, Nurden P, Nurden AT, et al. Clopidogrel: A review of its mechanism of action. Platelets 1998;9:251–255.
Cadroy Y, Bossavy JP, Thalamas C, Sagnard L, Sakariassen K, Boneu B. Early potent antithrombotic effect with combined aspirin and a loading dose of clopidogrel on experimental arterial thrombogenesis in humans. Circulation 2000;101:2823–2828.
Gent M. Benefit of Clopidogrel in patients with coronary disease. Circulation 1997;96:I–467 (abstract).
Schomig A, Neumann FJ, Kastrati A, et al. A randomized comparison of antiplatelet and anticoagulant therapy after the placement of coronary-artery stents. N Engl J Med 1996;334:1084–1089.
Bertrand ME, Legrand V, Boland J, et al. Randomized multicenter comparison of conventional anticoagulation versus antiplatelet therapy in unplanned and elective coronary stenting. The full anticoagulation versus aspirin and ticlopidine (fantastic) study. Circulation 1998;98:1597–1603.
Makkar RR, Eigler NL, Kaul S, et al. Effects of clopidogrel, aspirin and combined therapy in a porcine ex vivo model of high-shear induced stent thrombosis. Eur Heart J 1998;19:1538–1546.
Harker LA, Marzec UM, Kelly AB, et al. Clopidogrel inhibition of stent, graft, and vascular thrombogenesis with antithrombotic enhancement by aspirin in nonhuman primates. Circulation 1998;98:2461–2469.
Mehta SR, Yusuf S, Peters RJ, et al. Effects of pretreatment with clopidogrel and aspirin followed by long-term therapy in patients undergoing percutaneous coronary intervention: The PCI-CURE study. Lancet 2001;358:527–533.
Schafer AI. Antiplatelet therapy. Am JMed 1996;101:199–209.
Schafer AL. Pharmacodynamics of Oral Antiplatelet Agents. In: Smith TW, ed. Cardiovascular Therapeutics. Philadelphia, PA: W.B. Saunders, 1996:Chapter 27.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Volturo, G.A., Aghababian, R.V. Facilitating Optimal Care of Acute Coronary, Cerebrovascular and Peripheral Vascular Syndromes in the Emergency Department: The Role of Oral Antiplatelet Therapy. J Thromb Thrombolysis 17, 29–34 (2004). https://doi.org/10.1023/B:THRO.0000036026.86674.c8
Issue Date:
DOI: https://doi.org/10.1023/B:THRO.0000036026.86674.c8