Abstract
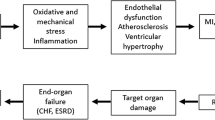
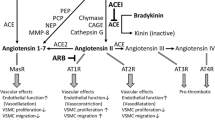
Angiotensin-converting enzyme inhibitors (ACE-I) were initially developed as therapeutic agents targeted for the treatment of hypertension. Since the initial application of these agents, several additional clinical indications have been identified such as coronary artery disease, stroke, congestive heart failure and prevention of diabetes-related complications. In addition to the blood pressure lowering effects, this class of agents has the ability to restore endothelial function, decrease oxidative stress and enhance endogenous fibrinolysis. Moreover, ACE-I possesses antiplatelet effects as well as antiproliferatory and antimigratory effects on smooth muscle cells. This article links the effects of ACE-I on thrombotic mediators to the potential clinical implications in the setting of coronary artery disease.
Similar content being viewed by others
References
Ryan TJ, Antman EM, Brooks NH, et al. 1999 update: ACC/AHA guidelines for the management of patients with acute myocardial infarction. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Acute Myocardial Infarction). J Am Coll Cardiol 1999;34:890.
Napoleone E, Di Santo A, Camera M, et al. Angiotensin-Converting Enzyme Inhibitors Downregulate Tissue Factor Synthesis in Monocytes. Circ Res 2000;86(2):139-143.
Hornig B, Kohler C, Drexler H. Role of bradykinin in mediating vascular effects of angiotensin-converting enzyme inhibitors in humans. Circulation 1997;95(5):1115-1118.
Rajagopalan S, Kurz S, Munzel T, et al. Angiotensin II mediated hypertension in rate increases vascular superoxide production via membrane NADH/NADPH oxidase activation: Contribution to alterations of vasomotor tone. J Clin Invest 1996;97:1916-1923.
Van Geel PP, Pinto YM, Buikema H, et al. Is the A1166C polymorphism of the angiotensin II receptor involved in cardiovascular disease? Eur Heart J 1998;19(Suppl G):G13-G17.
Ruzicka M, Skarda V, Leenen FH. Effects ofACEinhibitors on circulating versus cardiac angiotensin II in volume overload-induced cardiac hypertrophy in rats. Circulation 1995;92:3568-3573.
Pieruzzi F, Abassi ZA, Keiser HR. Expression of reninangiotensin system components in the heart, kidneys, and lungs of rats with experimental heart failure. Circulation 1995;92:3105-3112.
Hokimoto S, Yasue H, Fujimoto K, et al. Expression of angiotensin-converting enzyme in remaining viable myocytes of human ventricles after myocardial infarction. Circulation 1996;94:1513-1518.
Hirsch AT, Talsness CE, Schunkert H, et al. Tissue-specific activation of cardiac angiotensin converting enzyme in experimental heart failure. Circ Res 1991;69:475-482.
Fabris B, Jackson B, Kohzuki M, et al. Increased cardiac angiotensin-converting enzyme in rats with chronic heart failure. Clin Exp Pharmacol Physiol 1990;17:309-314.
Lee YA, Liang CS, Lee MA, et al. Local stress not systemic factors regulate gene expression of the cardiac renin-angiotensin system in vivo: A comprehensive study of all its components in the dogs. Proc Natl Acad Sci 1996;A93:11035-11040.
Falkenhahn M, Franke F, Bohle RM, et al. Cellular distribution of angiotensin-converting enzyme after myocardial infarction. Hypertension 1995;25:219-226.
Vaughn DE. Fibrinolytic balance, the renin-angiotensin system and atherosclerotic disease. Euro heart J 1998;19(Suppl G):G9-G12.
Hernandez-Presa M, Bustos C, Ortego M, et al. Angiotensin-converting enzyme inhibition prevents arterial nuclear factor-kappa B activation, monocyte chemoattractant protein-1 expression, and macrophage infiltration in a rabbit model of early-accelerated atherosclerosis. Circulation 1997;95:1532-1541.
Valentin, Reutlingsperger CP, Nordfang O, et al. Inhibition of factor X activation at extracellular matrix of fibroblasts during flow conditions: A comparison between tissue factor pathway inhibitor and inactive factor VIIa. Thromb Haemost 1995;74:1478-1485.
Varin R, Mulder P, Tamion F, et al. Improvement of endothelial function by chronic angiotensin-converting enzyme inhibition in heart failure: Role of nitric oxide, prostanoids, oxidant stress, and bradykinin. Circulation 2000;102:351-356.
Vaughn DE. The Renin angiotensin system and fibrinolysis.Am J Cardiol 1997;79:12-16.
Lupu F, Heim DA, Bachmann F, et al. Plasminogen activator expression in human atherosclerotic lesions. Arterioscler Thromb Vasc Biol 1995;15(9):1444-1455.
Nishimura H, Tsuji H, Masuda H, et al. The Effects of Angiotensin Metabolites on the Regulation of Coagulation and Fibrinolysis in Cultured Rat Aortic Endothelial Cells; Thromb Haemost 1999;82:1516-1521.
Nishimura H, Tsuji H, Masuda H, et al. Angiotensin II increases Plasminogen activator inhibitor-1 and tissue factor mRNA expression without changing that of tissue type Plasminogen activator or tissue factor pathway inhibitor in cultured rat aortic endothelial cells. Thromb Haemost 1997;77:1189-1195.
Ruf W, Edgington T.S. Structural biology of tissue factor, the initiator of thrombogenesis in vivo. FASEB J (1994);8:385-390.
Moriyama Y, Ogawa H, Oshima S, et al. Captopril reduced plasminogen activator inhibitor activity in patients with acute myocardial infarction. Japan Circ J 1997;61:308-314.
Huber K, Rosc D, Resch I, et al. Circadian fluctuations of plasminogen activator inhibitor and tissue plasminogen activator levels in plasma of patients with unstable coronary artery disease and acute myocardial infarction.Thromb Haemost 1988;60:372-376.
Hamsten A, De Faire U, Wallidius G, et al. Plasminogen Activator inhibitor in Plasma: Risk factor for recurrent Myocardial infarction. Lancet 1987;2:3-9.
Collet JP, Montalescot G, Vicaut E, et al. Acute release of plasminogen activator inhibitor-1 in ST-segment elevation myocardial infarction predicts mortality. Circulation 2003;108(4):391-394.
Thögerson AM, Jansson JH, Boman K, et al. High Plasminogen Activator Inhibitor and Tissue Plasminogen Activator Levels in Plasma precede a first acute myocardial infarction in both men and women: Evidence for the fibrinolytic System as an Independent Primary Risk factor.Circulation 1998;98(21):2241-2247.
Boman KO, Jansson JH, Nyhlen, et al. Improved fibrinolysis after one year of treatment with Enalapril in men and women with uncomplicated myocardial infarction. Thromb Haemost 2002;87(2):311-316.
Linz W, Wiemer G, Gohlke P, et al. Contribution of kinins to the cardiovascular actions of angiotensin-converting enzyme inhibitors. Pharmacol Rev 1995;47:25-49.
Brown NJ, Nadeau JH, Vaughan DE. Selective stimulation of tissue type plasminogen activator (t-PA) in vivo by infusion of bradykinin. Thromb Haemost 1997;77(3):522-525.
Osterud B, Bajaj MS, Bajaj SP. Sites of tissue factor pathway inhibitor (TFPI) and tissue factor expression under physiologic and pathologic conditions. On behalf of the Subcommittee on Tissue factor Pathway Inhibitor (TFPI) of the Scientific and Standardization Committee of the ISTH. Thromb Haemost 1995;73:873-875.
Nemerson Y. The tissue factor pathway of blood coagulation.Semin Hematol 1992;29:170-176.
Colli S, Lalli M, Rise P, et al. Increased thrombogenic potential of human monocyte derived macrophages spontaneously transformed into foam cells. Thromb Haemost 1999;81:576-581.
Lesnik P, Rouis M, Skarlatos S, Kruth HS, Chapman MJ.Uptake of exogenous free cholesterol induces upregulation of tissue factor expression in human monocyte derived macrophages. Proc Natl Acad Sci USA 1992;89:10370-10374.
Freeburn JC, Wallace JM, Strain JJ, et al. Monocyte tissue factor-like activity in post myocardial infarction patients. Br J Haematol 1998;102:605-608.
Jude B, Agraou B, McFadden EP, et al. Evidence for timedependent activation of monocytes in the systemic circulation in unstable angina but not in acute myocardial infarction or in stable angina. Circulation 1994; 90:1662-1668.
Misumi K, Ogawa H, Yasue H, et al.Comparison of plasma tissue factor levels in unstable and stable angina pectoris.Am J Cardiol 1998;81:22-26.
Soejima H, Ogawa H, Yasue H, et al. Heightened tissue factor associated with tissue factor pathway inhibitor and prognosis in patients with unstable angina. Circulation 1999;99:2908-2913.
Soejima H, Ogawa H, Yasue H, et al. Effects of enalapril on tissue in patients with uncomplicated acute myocardial infarction. Am J Cardiol 1996;78:336-340.
Kranzhofer R, Schmidt J, Pfeiffer CA, et al. Angiotensin induces inflammatory activation of human vascular smooth muscle cells. Arterioscler Thromb Vasc Biol 1999;19:1623- 1629.
Soejima H, Ogawa H, Yasue H, Kaikita K, et al. Angiotensin converting enzyme inhibition reduces monocyte chemo attractant protein -1 and tissue factor levels in patients with myocardial infarction. J Am Coll Cardiol 1999;34(4):983-988.
Berkenboom G, Langer I, Carpentier Y, et al. Ramipril prevents endothelial dysfunction induced by oxidized lowdensity lipoproteins: A bradykinin-dependent mechanism.Hypertension 1997;30:371-376.
Mancini GBJ, Henry GC, Macaya C, et al. Angiotensinconverting enzyme inhibition with Quinapril improves endothelial vasomotor dysfunction in patients with coronary artery disease: The Trend (Trial on Reversing Endothelial Dysfunction) Study. Circulation 1996;94:258-265.
O'Driscoll G, Green D, Rankin J, et al. Improvement in endothelial function by angiotensin converting enzyme inhibition in insulin-dependent diabetes mellitus. J Clin Invest 1997;100:678-684.
Higashi Y, Sasaki S, Nakagawa K, et al. A comparison of angiotensin-converting enzyme inhibitors, calcium antagonists, beta-blockers and diuretic agents on reactive hyperemia in patients with essential hypertension: A multicenter study. J AmColl Cardiol 2000;35:284-291.
Berk BC, Corson MA. Angiotensin II signals transduction in vascular smooth muscle: Role of tyrosine kinases. Circ Res 1997;80:607-617.
Baker KM, Aceto JF. Angiotensin II stimulation of protein synthesis and cell growth in chick heart cells.AmJ Physiol 1990;259(2 Pt 2):H610-H618.
Geisterfer AA, Peach MJ, Owens GK. Angiotensin II induces hypertrophy, not hyperplasia, of cultured rat aortic smooth muscle cells. Circ Res 1988;62:749-756.
Kawano H, Do Y, Kawano Y, et al. Angiotensin II has multiple profibrotic effects in human cardiac fibroblasts. Circulation 2000;101:1130-1137.
The Fourth International Study of Infarct Survival (ISIS-4) Collaborative Group. ISIS-4: A randomized factorial trial assessing early oral captopril, oral mononitrate, and intravenous magnesium sulfate in 58,050 patients with suspected acute myocardial infarction. Lancet 1995;345:669-685.
Chinese Cardiac Study Collaborative Group. Oral Captopril versus placebo among 13,634 patients with suspected acute myocardial infarction: Interim report from the Chinese Cardiac Study (CCS-1). Lancet 1995;345:686-687.
Swedberg K, Held P, Kjekshus J, et al. Effects of the early administration of enalapril on mortality in patients with acute myocardial infarction. Results of the Cooperative New Scandinavian Enalapril Survival Study II (CONSENSUS II). N Engl J Med 1992;327:678-684.
Gruppo Italiano per lo Studio della Sopravvivenza nell'infacto Miocardico. GISSI-3: Effects of lisinopril and transdermal glyceryl trinitrate singly and together on 6-week mortality and ventricular function after acute myocardial infarction. Lancet 1994;343:1115-1122.
Ambrosioni E, Borghi C, Magnani B, for the Survival of Myocardial Infarction Long-term Evaluation (SMILE) Study Investigators. The effect of the angiotensin-convertingenzyme inhibitor zofenopril on mortality and morbidity after anterior myocardial infarction. N Engl J Med 1995;332:80-85.
Pfeffer MA, Braunwald E, Moyé LA, et al. Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infarction: Results of the Survival and Ventricular Enlargement Trial. N Engl J Med 1992;327:669-677.
The Acute Infarction Ramipril Efficacy (AIRE) Study Investigators: Effect of ramipril on mortality and morbidity of survivors of acute myocardial infarction with clinical evidence of heart failure. Lancet 1993;342:821-828.
Kober L, Torp-Pedersen C, Carlsen JE, et al. A clinical trial of the angiotensin converting enzyme inhibitor, trandolapril in patients with left ventricular dysfunction after myocardial infarction. N Engl JMed 1995;333:1670-1676.
Heart Outcomes Prevention Evaluation Study Investigators, Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients.N Engl J Med 2000;342:145-153.
Hansson L, Lindholm L, Ekborn T, Dahlof B, et al. Randomized trial of old and new antihypertensive drugs in elderly patients: Cardiovascular mortality and morbidity the Swedish trial in old Patients with Hypertension *2 study. Lancet 1999;354:1751-1756.
The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and treatment of High Blood Pressure: The JNC 7 report. JAMA 2003;289:2560- 2572.
Dzau VJ. Vascular wall Renin Angiotensin pathway in control of the circulation: A hypothesis.AmJMed 1984;77:31-36.
Dzau VJ, Re RN. Evidence for the existence of renin in the heart. Circulation 1987;75(Suppl I):1134-1136.
Foy SG, Crozier IG, Turner JG, et al. Comparison of enalapril versus captopril on left ventricular function and survival three months after acute myocardial infarction (the 'PRACTICAL' study). Am J Cardiol 1994;73:1180- 1186.
Lyons D, Webster J, Benjamin N. Effect of enalapril and quinapril on forearm vascular ACE in man. Eur J Clin Pharmacol 1997;51:373-378.
Konermann M, Sanner BM, Grotz J, et al. Effect of infarct size and site, patency of the infarct vessel and perfusion of vital myocardium on remodeling of the left ventricle- studies with cine-magnetic resonance tomography in the first 6 months following myocardial infarct. Zeitschrift fur Kardiologie 1996;85(12):906-916.
Ray S, Dargie H. Infarct-related heart failure: The choice of ACE inhibitor does not matter. Cardiovasc Drugs Ther 1994;8:433-436.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kothari, S.A., Le, M.K. & Gandhi, P.J. Effects of Angiotensin Converting Enzyme Inhibitors on Thrombotic Mediators: Potential Clinical Implications. J Thromb Thrombolysis 15, 217–225 (2003). https://doi.org/10.1023/B:THRO.0000011379.68077.64
Issue Date:
DOI: https://doi.org/10.1023/B:THRO.0000011379.68077.64