Abstract
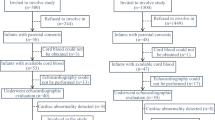
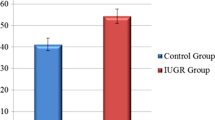
To evaluate umbilical cord blood creatine kinase MB (CK-MB), troponin T (TnT-hs), pro-brain natriuretic peptide (proBNP), ischaemia modified albumin (IMA) levels and fetal cardiac function in intrauterine growth retardation (IUGR). The study included 39 pregnant women with IUGR and 42 healthy pregnant women in control group. IUGR was diagnosed when estimated fetal weight was < 10 percentile. Fetal cardiac function was evaluated by ultrasound in the third trimester of pregnancy and compared with the control group. Umbilical cord blood biochemical test (CK-MB, TnT-hs, proBNP, IMA) results compared between the groups. In cardiac morphological evaluation, cardiothoracic index was higher, and the left sphericity index was lower in the IUGR group compared to the control group (p < 0.001, p = 0,018). Left myocardial performance index (MPI) was higher, and tricuspid and mitral annular plane systolic excursion (TAPSE and MAPSE) values were lower in the IUGR group than the control group (p = 0.035, p = 0.038 and p = 0.011 respectively). In IUGR group, only proBNP levels were increased compare to the control group in umbilical cord blood biochemical tests (p = 0.018). There was negative correalation between umbilical cord blood proBNP levels and MAPSE value (r = − 0,332, p = 0,002). We observed that IUGR was associated with fetal cardiac morphological changes and systolic dysfunction. Also, in IUGR group cord, blood proBNP level was increased and negatively correlated with MAPSE value.
Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in the article.
Code availability
None.
References
Kesavan K, Devaskar SU. Intrauterine growth restriction: postnatal monitoring and outcomes. Pediatr Clin North Am. 2019;66:403–23.
Martins JG, Biggio JR, Abuhamad A. Society for Maternal-Fetal Medicine Consult Series #52: diagnosis and management of fetal growth restriction: (Replaces Clinical Guideline Number 3, April 2012). Am J Obstet Gynecol. 2020;223:B2-17.
Zur RL, Kingdom JC, Parks WT, Hobson SR. The placental basis of fetal growth restriction. Obstet Gynecol Clin North Am. 2020;47:81–98.
Patey O, Carvalho JS, Thilaganathan B. Perinatal changes in cardiac geometry and function in growth-restricted fetuses at term. Ultrasound in Obstetrics & Gynecology : The Official J Int Soc Ultrasound in Obstetrics Gynecol. 2019;53:655–62.
Bahtiyar MO, Copel JA. Cardiac changes in the intrauterine growth-restricted fetus. Semin Perinatol. 2008;32:190–3.
Yildirim A, Ozgen F, Ucar B, Alatas O, Tekin N, Kilic Z. The diagnostic value of troponin T level in the determination of cardiac damage in perinatal asphyxia newborns. Fetal Pediatr Pathol. 2016;35:29–36.
Ker JA, Soma-Pillay P. NT-proBNP: when is it useful in obstetric medicine? Obstetric Medicine. 2018;11:3–5.
Kocylowski RD, Dubiel M, Gudmundsson S, Sieg I, Fritzer E, Alkasi Ö, et al. Biochemical tissue-specific injury markers of the heart and brain in postpartum cord blood. Am J Obstet Gynecol. 2009;200:273.e1-273.e25.
Yarcı Gursoy A, Caglar GS, Demirtas S. Ischemia modified albumin in perinatology. Eur J Obstet Gynecol Reprod Biol. 2017;210:182–8.
Awadh AMA, Prefumo F, Bland JM, Carvalho JS. Assessment of the intraobserver variability in the measurement of fetal cardiothoracic ratio using ellipse and diameter methods. Ultrasound Obstet Gynecol. 2006;28:53–6.
DeVore GR, Klas B, Satou G, Sklansky M. 24-segment sphericity index: a new technique to evaluate fetal cardiac diastolic shape. Ultrasound in Obstetrics & Gynecology : The Official J Int Soc Ultrasound in Obstetrics Gynecol. 2018;51:650–8.
García-Otero L, Gómez O, Rodriguez-López M, Torres X, Soveral I, Sepúlveda-Martínez Á, et al. Nomograms of fetal cardiac dimensions at 18–41 weeks of gestation. Fetal Diagn Ther. 2020;47:387–98.
Patey O, Gatzoulis MA, Thilaganathan B, Carvalho JS. Perinatal changes in fetal ventricular geometry, myocardial performance, and cardiac function in normal term pregnancies. J Am Soc Echocard : Official Publication Am Soc of Echocardio. 2017;30:485-492.e5.
Cruz-Lemini M, Crispi F, Valenzuela-Alcaraz B, Figueras F, Sitges M, Gómez O, et al. Value of annular M-mode displacement vs tissue Doppler velocities to assess cardiac function in intrauterine growth restriction. Ultrasound in Obstetrics & Gynecology : The Official J Int Soc Ultrasound Obstetrics Gynecol. 2013;42:175–81.
Crispi F, Crovetto F, Gratacos E. Intrauterine growth restriction and later cardiovascular function. Early Human Dev. 2018;126:23–7.
Rizzo G, Mattioli C, Mappa I, Bitsadze V, Khizroeva J, Słodki M, et al. Hemodynamic factors associated with fetal cardiac remodeling in late fetal growth restriction: a prospective study. J Perinat Med. 2019;47:683–8.
Pérez-Cruz M, Cruz-Lemini M, Fernández MT, Parra JA, Bartrons J, Gõmez-Roig MD, et al. Fetal cardiac function in late-onset intrauterine growth restriction vs small-for-gestational age, as defined by estimated fetal weight, cerebroplacental ratio and uterine artery Doppler. Ultrasound in Obstetrics & Gynecology : The Official J Int Soc Ultrasound Obstetrics Gynecol. 2015;46:465–71.
Channing A, Szwast A, Natarajan S, Degenhardt K, Tian Z, Rychik J. Maternal hyperoxygenation improves left heart filling in fetuses with atrial septal aneurysm causing impediment to left ventricular inflow. Ultrasound Obstet Gynecol 2015;45:664–669.
Zhang L, Han J, Zhang N, Li Z, Wang J, Xuan Y, et al. Assessment of fetal modified myocardial performance index in early-onset and late-onset fetal growth restriction. Echocardiography (Mount Kisco, NY). 2019;36:1159–64.
Nguyen TTN, Kotani T, Imai K, Ushida T, Moriyama Y, Kobayashi T, et al. Assessment of myocardial performance index in late-onset fetal growth restriction. Nagoya J Med Sci. 2021;83:259–68.
Guo XF, Li YL, Zhao BW. Annular plane systolic excursion Z-scores in evaluation of heart systolic function of fetus with heart failure. J Matern Fetal Neonatal Med 2022;35(25):5301–5307.
Tello-Montoliu A, Marín F, Roldán V, Mainar L, López MT, Sogorb F, et al. A multimarker risk stratification approach to non-ST elevation acute coronary syndrome: implications of troponin T, CRP, NT pro-BNP and fibrin D-dimer levels. J Intern Med. 2007;262:651–8.
Katrukha IA. Human cardiac troponin complex. Structure and functions Biochemistry (Moscow). 2013;78:1447–65.
Gaggin HK, Januzzi JL. Biomarkers and diagnostics in heart failure. Biochem Biophys Acta. 2013;1832:2442–50.
Garofoli F, Mannarino S, Montanari L, Cerbo R, Tzialla C, Mazzucchelli I, et al. Variation of B-type natriuretic peptide concentrations and intrauterine growth restriction: mother, fetus and newborn. J Biol Regul Homeost Agents. 2012;26:733–9.
Mannarino S, Ciardelli L, Garofoli F, Perotti G, Mongini E, Damiano S, et al. Correlation between cord blood, perinatal BNP values and echocardiographic parameters in healthy Italian newborns. Early Human Dev. 2009;85:13–7.
Sari N, Ede H, Engin-Ustun Y, Göçmen AY, Çaǧlayan EK. Hyperemesis gravidarum is associated with increased maternal serum ischemia-modified albumin. J Perinat Med. 2017;45:421–5.
Dahiya K, Kulshrestha MR, Bansal P, Ghalaut VS, Kulshrestha R, Dahiya P, et al. Evaluation of cord blood ischemia modified albumin in normal pregnancies and pre-eclampsia. Hypertens Pregnancy. 2015;34:204–8.
Tayyar AT, Kozalı S, Yetkin Yildirim G, Karakus R, Yuksel IT, Erel O, et al. Role of ischemia-modified albumin in the evaluation of oxidative stress in intrahepatic cholestasis of pregnancy. J Matern Fetal Neonatal Med. 2019;32:3836–40.
Andıç E, Karaman E, Kolusarı A, Çokluk E. Association of cord blood ischemia-modified albumin level with abnormal foetal Doppler parameters in intrauterine growth-restricted foetuses. J Matern Fetal Neonatal Med. 2021;34:1–6.
Lacovidou N, Briana DD, Boutsikou M, Liosi S, Baka S, Boutsikou T, et al. Cord blood ischemia-modified albumin levels in normal and intrauterine growth restricted pregnancies. Mediators Inflamm 2008;2008:523081
Funding
This study was funded by Gazi University Research Committee (Project No: 6478/2021; no involvement in study design, collection, analysis, and writing the report).
Author information
Authors and Affiliations
Contributions
HÖ, BN, and ET searched, excluded, or included and rated the quality of the studies. DK, MB, CY, and ET interpreted the results and contributed to the writing process. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Gazi University Faculty of Medicine Clinical Research Ethics Committee with the decision number 25901600–604.01.01–17 ethics committee decision no: 439.
Consent to participate
Written consent was obtained from patients.
Consent for publication
All patients have signed consent for publication in the study protocol.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Medicine
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Turgut, E., Özdemir, H., Narlı, B. et al. Umbilical Cord Blood Biochemical Cardiac Markers and Fetal Cardiac Function in Cases of IUGR. SN Compr. Clin. Med. 5, 27 (2023). https://doi.org/10.1007/s42399-022-01370-3
Accepted:
Published:
DOI: https://doi.org/10.1007/s42399-022-01370-3