Abstract
Background
The objective of this study was to characterize hypernatremia patients at hospital admission into clusters using an unsupervised machine learning approach and to evaluate the mortality risk among these distinct clusters.
Methods
We performed consensus cluster analysis based on demographic information, principal diagnoses, comorbidities, and laboratory data among 922 hospitalized adult patients with admission serum sodium of > 145 mEq/L. We calculated the standardized difference of each variable to identify each cluster’s key features. We assessed the association of each hypernatremia cluster with hospital and 1-year mortality.
Results
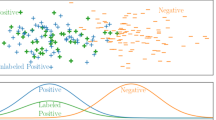
There were three distinct clusters of patients with hypernatremia on admission: 318 (34%) patients in cluster 1, 339 (37%) patients in cluster 2, and 265 (29%) patients in cluster 3. Cluster 1 consisted of more critically ill patients with more severe hypernatremia and hypokalemic hyperchloremic metabolic acidosis. Cluster 2 consisted of older patients with more comorbidity burden, body mass index, and metabolic alkalosis. Cluster 3 consisted of younger patients with less comorbidity burden, higher baseline eGFR, hemoglobin, and serum albumin. Compared to cluster 3, odds ratios for hospital mortality were 15.74 (95% CI 3.75–66.18) for cluster 1, and 6.51 (95% CI 1.48–28.59) for cluster 2, whereas hazard ratios for 1-year mortality were 6.25 (95% CI 3.69–11.46) for cluster 1 and 4.66 (95% CI 2.73–8.59) for cluster 2.
Conclusion
Our cluster analysis identified three clinically distinct phenotypes with differing mortality risk in patients hospitalized with hypernatremia.
Graphic abstract





Similar content being viewed by others
References
Adrogué HJ, Madias NE (2000) Hypernatremia. N Engl J Med 342:1493–1499
Muhsin SA, Mount DB (2016) Diagnosis and treatment of hypernatremia. Best Pract Res Clin Endocrinol Metab 30:189–203
Palevsky PM, Bhagrath R, Greenberg A (1996) Hypernatremia in hospitalized patients. Ann Intern Med 124:197–203
Chauhan K, Pattharanitima P, Patel N et al (2019) Rate of correction of hypernatremia and health outcomes in critically ill patients. Clin J Am Soc Nephrol 14:656–663
Funk GC, Lindner G, Druml W et al (2010) Incidence and prognosis of dysnatremias present on ICU admission. Intensive Care Med 36:304–311
Tanemoto M (2021) Lessons for the clinical nephrologist: a midsummer night's cluster of hypernatremia cases. J Nephrol PMID: 33856684. https://doi.org/10.1007/s40620-021-01047-5
Sterns RH (2015) Disorders of plasma sodium–causes, consequences, and correction. N Engl J Med 372:55–65
Kim SW (2006) Hypernatemia: successful treatment. Electrolyte Blood Press 4:66–71
Lien YH, Shapiro JI, Chan L (1990) Effects of hypernatremia on organic brain osmoles. J Clin Investig 85:1427–1435
Chewcharat A, Thongprayoon C, Cheungpasitporn W et al (2020) Trajectories of serum sodium on in-hospital and 1-year survival among hospitalized patients. Clin J Am Soc Nephrol 15:600–607
Thongprayoon C, Cheungpasitporn W, Yap JQ et al (2020) Increased mortality risk associated with serum sodium variations and borderline hypo- and hypernatremia in hospitalized adults. Nephrol Dial Transplant 35:1746–1752
MacEachern SJ, Forkert ND (2021) Machine learning for precision medicine. Genome 64(4):416–425. PMID: 33091314. https://doi.org/10.1139/gen-2020-0131
Yang C, Kong G, Wang L et al (2019) Big data in nephrology: Are we ready for the change? Nephrology 24:1097–1102
Thongprayoon C, Kaewput W, Kovvuru K, Hansrivijit P, Kanduri SR, Bathini T, Chewcharat A, Leeaphorn N, Gonzalez-Suarez ML, Cheungpasitporn W (2020) Promises of big data and artificial intelligence in nephrology and transplantation. J Clin Med 9(4):1107. PMID: 32294906; PMCID: PMC7230205 https://doi.org/10.3390/jcm9041107
Monti S, Tamayo P, Mesirov J et al (2003) Consensus clustering: a resampling-based method for class discovery and visualization of gene expression microarray data. Mach Learn 52:91–118
Wilkerson MD, Hayes DN (2010) ConsensusClusterPlus: a class discovery tool with confidence assessments and item tracking. Bioinformatics 26:1572–1573
Thongprayoon C, Vaitla P, Nissaisorakarn V et al (2021) Clinically distinct subtypes of acute kidney injury on hospital admission identified by machine learning consensus clustering. Med Sci 9:60
Zheng Z, Waikar SS, Schmidt IM et al (2021) Subtyping CKD patients by consensus clustering: the chronic renal insufficiency cohort (CRIC) study. J Am Soc Nephrol 32:639–653
Thongprayoon C, Hansrivijit P, Mao MA et al (2021) Machine learning consensus clustering of hospitalized patients with admission hyponatremia. Diseases 9:54
Thongprayoon C, Kattah AG, Mao MA, Keddis MT, Pattharanitima P, Vallabhajosyula S, Nissaisorakarn V, Erickson SB, Dillon JJ, Garovic VD, Cheungpasitporn W (2021) Distinct Phenotypes of Hospitalized Patients with Hyperkalemia by Machine Learning Consensus Clustering and Associated Mortality Risks. QJM. 16:hcab194. PMID: 34270780. https://doi.org/10.1093/qjmed/hcab194
Thongprayoon C, Cheungpasitporn W, Petnak T et al (2020) The prognostic importance of serum sodium levels at hospital discharge and one-year mortality among hospitalized patients. Int J Clin Pract 74:e13581
Șenbabaoğlu Y, Michailidis G, Li JZ (2014) Critical limitations of consensus clustering in class discovery. Sci Rep 4:6207
Palmer BF, Clegg DJ (2019) The use of selected urine chemistries in the diagnosis of kidney disorders. Clin J Am Soc Nephrol 14:306–316
Lee JW (2010) Fluid and electrolyte disturbances in critically ill patients. Electrolyte Blood Press 8:72–81
Bataille S, Baralla C, Torro D et al (2014) Undercorrection of hypernatremia is frequent and associated with mortality. BMC Nephrol 15:37
Rein JL, Coca SG (2019) “I don’t get no respect”: the role of chloride in acute kidney injury. Am J Physiol Renal Physiol 316:F587-f605
Korgaonkar S, Tilea A, Gillespie BW et al (2010) Serum potassium and outcomes in CKD: insights from the RRI-CKD cohort study. Clin J Am Soc Nephrol 5:762–769
Vlagopoulos PT, Tighiouart H, Weiner DE et al (2005) Anemia as a risk factor for cardiovascular disease and all-cause mortality in diabetes: the impact of chronic kidney disease. J Am Soc Nephrol 16:3403–3410
Lee PC, Kini AS, Ahsan C et al (2004) Anemia is an independent predictor of mortality after percutaneous coronary intervention. J Am Coll Cardiol 44:541–546
Ezekowitz JA, McAlister FA, Armstrong PW (2003) Anemia is common in heart failure and is associated with poor outcomes: insights from a cohort of 12 065 patients with new-onset heart failure. Circulation 107:223–225
Chertow GM, Burdick E, Honour M et al (2005) Acute kidney injury, mortality, length of stay, and costs in hospitalized patients. J Am Soc Nephrol 16:3365–3370
Dam Fialla A, Schaffalitzky de Muckadell OB, TouborgLassen A (2012) Incidence, etiology and mortality of cirrhosis: a population-based cohort study. Scand J Gastroenterol 47:702–709
Todd S, Barr S, Roberts M et al (2013) Survival in dementia and predictors of mortality: a review. Int J Geriatr Psychiatry 28:1109–1124
Tsipotis E, Price LL, Jaber BL et al (2018) Hospital-associated hypernatremia spectrum and clinical outcomes in an unselected cohort. Am J Med 131:72-82.e71
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they do not have any financial or non-financial potential conflict of interest.
Ethical approval
The study was approved by the Institutional Review Board of Mayo Clinic (IRB number 21-003088; date of approval: 3/30/2021).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Thongprayoon, C., Mao, M.A., Keddis, M.T. et al. Hypernatremia subgroups among hospitalized patients by machine learning consensus clustering with different patient survival. J Nephrol 35, 921–929 (2022). https://doi.org/10.1007/s40620-021-01163-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-021-01163-2