Abstract
Background
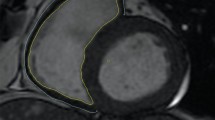
Left atrial (LA) volume is a well-established cardiovascular prognosticator in patients with end-stage renal disease. Although dialysis intensification is associated with left ventricular mass regression, there are limited data regarding LA remodeling. Using cardiac magnetic resonance imaging (CMR), we examined changes in LA size and function relative to ventricular remodeling and cardiac biomarkers after dialysis intensification.
Methods
In this prospective 2-centre cohort study, 37 patients receiving conventional hemodialysis (CHD, 4 h/session, 3×/week) were converted to in-centre nocturnal hemodialysis (INHD 7–8 h/session, 3×/week); 30 patients remained on CHD. CMR and biomarkers were performed at baseline and repeated at 52 weeks.
Results
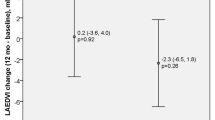
After 52 weeks, there were no significant changes in the LA volumes or LA ejection fraction (EF) within either the CHD or INHD group, and no significant differences between the two groups. Correlations existed between changes in LA and LV end-diastolic volume index (EDVi, Spearman’s r = 0.69, p < 0.001), LA and LV end-systolic volume index (ESVi, r = 0.44, p = 0.001), LAEF and LVEF (r = 0.28, p = 0.04), LA and RV EDVi (r = 0.51, p < 0.001), LA and RV ESVi (r = 0.29, p = 0.039), and LA ESVi and LV mass index (r = 0.31, p = 0.02). At baseline, indexed LA volumes positively correlated with NT-proBNP, whereas LAEF negatively correlated with NT-proBNP and Troponin I. After 52 weeks, changes in biomarker levels did not correlate with changes in LA volume or EF.
Conclusion
There was no significant change in LA size or systolic function after conversion to INHD. The significant correlations between LA and ventricular remodeling and cardiac biomarkers suggest common underlying pathophysiologic mechanisms.
Trial registration
ClinicalTrials.gov Identifier: NCT00718848.





Similar content being viewed by others
References
Canadian Institute for Health Information (2014) Canadian organ replacement register annual report: treatment of end-stage organ failure in Canada, 2003 to 2012. Ottawa, ON
Ross B, Wald R, Goldstein M et al (2017) Relationships between left ventricular structure and function according to cardiac MRI and cardiac biomarkers in end-stage renal disease. Can J Cardiol 33(4):501–507
Karur G, Wald R, Goldstein M et al (2017) Association between conversion to in-center nocturnal hemodialysis and right ventricular remodeling. Nephrol Dial Transplant 33:1–7
Bugeja A, Dacouris N, Thomas A et al (2009) In-center nocturnal hemodialysis: another option in the management of chronic kidney disease. Clin J Am Soc Nephrol 4(4):778–783
Tsang TS, Barnes ME, Gersh BJ, Bailey KR, Seward JB (2002) Left atrial volume as a morphophysiologic expression of left ventricular diastolic dysfunction and relation to cardiovascular risk burden. Am J Cardiol 90(12):1284–1289
Tripepi G, Benedetto FA, Mallamaci F, Tripepi R, Malatino L, Zoccali C (2007) Left atrial volume monitoring and cardiovascular risk in patients with end-stage renal disease: a prospective cohort study. J Am Soc Nephrol 18(4):1316–1322
Tripepi G, Benedetto FA, Mallamaci F, Tripepi R, Malatino L, Zoccali C (2006) Left atrial volume in end-stage renal disease: a prospective cohort study. J Hypertens 24:1173–1180
Culleton BF, Walsh M, Klarenbach SW et al (2007) Effect of frequent nocturnal hemodialysis vs conventional hemodialysis on left ventricular mass and quality of life: a randomized controlled trial. JAMA 298(11):1291–1299
FHN Trial Group, Chertow GM, Levin NW et al (2010) In-center hemodialysis six times per week versus three times per week. N Engl J Med 363(24):2287–2300
Rocco MV, Lockridge RS Jr, Beck GJ et al (2011) The effects of frequent nocturnal home hemodialysis: the frequent hemodialysis network nocturnal trial. Kidney Int 80(10):1080–1091
Casaclang-Verzosa G, Gersh BJ, Tsang TS (2008) Structural and functional remodeling of the left atrium: clinical and therapeutic implications for atrial fibrillation. J Am Coll Cardiol 51(1):1–11
Malik J, Lachmanova J, Kudlicka J et al (2016) Left atrial dysfunction in end-stage renal disease patients treated by hemodialysis. Nephron 133:169–174
Kim J, Song Y, Park G, Kim HJ, Kim SG (2017) Impact of rapid ultrafiltration rate on changes in the echocardiographic left atrial volume index in patients undergoing haemodialysis: a longitudinal observational study. BMJ Open 7:e013990
Tsang MY, Barnes ME, Tsang TS (2012) Left atrial volume: clinical value revisited. Curr Cardiol Rep 14(3):374–380
Tripepi G, Mattace-Raso F, Mallamaci F et al (2009) Biomarkers of left atrial volume: a longitudinal study in patients with end stage renal disease. Hypertension 54:818–824
Barberato SH, Bucharles SG, de Souza AM, Costantini CO, Costantini CR, Pecoits-Filho R (2013) Association between inflammatory markers and left atrial enlargement in patients on hemodialysis. Arq Bras Cardiol 100(2):141–146
Wald R, Goldstein MB, Perl J, Kiaii M et al (2016) The association between conversion to in-centre nocturnal hemodialysis and left ventricular mass regression in patients with end-stage renal disease. Can J Cardiol 32(3):369–377
Maceira AM, Cosin-Sales J, Roughton M, Prasad SK, Pennell DJ (2010) Reference left atrial dimensions and volumes by steady state free precession cardiovascular magnetic resonance. J Cardiovasc Magn Reson 12(65):1–10
Schulz-Menger J, Bluemke DA, Bremerich J et al (2013) Standardized image interpretation and post processing in cardiovascular magnetic resonance: society for cardiovascular magnetic resonance (SCMR) board of trustees task force on standardized post processing. J Cardiovasc Magn Reson 15:35
Posina K, Passick M, Reichek N, Cao JJ (2011) Left atrial volume measurement with magnetic resonance imaging: a comparison of biplane, short axis and long axis methods. J Cardiovasc Magn Reson 13(Suppl 1):P5
Lang RM, Badano LP, Mor-Avi V et al (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 28(1):1–39
Rodevan O, Bjornerheim R, Ljosland M, Maehle J, Smith HJ, Ihlen H (1999) Left atrial volumes assessed by three and two-dimensional echocardiography compared to MRI estimates. Int J Card Imaging 15:397–410
Mattioli AV, Bonatti S, Monopoli D, Zennaro M, Mattioli G (2005) Influence of regression of left ventricular hypertrophy on left atrial size and function in patients with moderate hypertension. Blood Press 14:273–278
Gerdts E, Wachtell K, Omvik P et al (2007) Left atrial size and risk of major cardiovascular events during antihypertensive treatment: losartan intervention for end-point reduction in hypertension trial. Hypertension 49(2):311–316
Barberato SH, Misocami M, Pecoits-Filho R (2009) Association between left atrium enlargement and intradialytic hypotension: role of diastolic dysfunction in the hemodynamic complications during hemodialysis. Echocardiography 26(7):767–771
Chao CT, Huang JW, Yen CJ (2015) Intradialytic hypotension and cardiac remodeling: a vicious cycle. Biomed Res Int 2015:724147
Satyan S, Light RP, Agarwal R (2007) Relationships of N-terminal pro-B-natriuretic peptide and cardiac troponin T to left ventricular mass and function and mortality in asymptomatic hemodialysis patients. Am J Kidney Dis 50(6):1009–1019
Bellenger NG, Davies LC, Francis JM, Coats AJ, Pennell DJ (2000) Reduction in sample size for studies of remodeling in heart failure by the use of cardiovascular magnetic resonance. J Cardiovasc Magn Reson 2:271–278
Grothues F, Smith GC, Moon JC et al (2002) Comparison of interstudy reproducibility of cardiovascular magnetic resonance with two-dimensional echocardiography in normal subjects and in patients with heart failure or left ventricular hypertrophy. Am J Cardiol 90:29–34
Acknowledgements
We are grateful to our patients and our research assistants who made this research possible.
Funding
This study was funded by an operating grant from the Canadian Institutes of Health Research (MOP-89982) and a grant-in-aid from the Heart and Stroke Foundation (Project Number G-14-0005856). The study sponsors had no role in the study design, data collection or analysis, interpretation of the findings, writing the manuscript or the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A.Y.M.W has received speaker honorarium from Sanofi, and grant from Baxter. The rest of the authors declare that they have no conflict of interest.
Ethical approval
The Research Ethics Board of each site approved the study and all study participants provided written informed consent.
Informed consent
Informed consent was obtained from all study participants.
Rights and permissions
About this article
Cite this article
Law, T.K., Wald, R., Goldstein, M. et al. Left Atrial Remodeling Assessed by Cardiac MRI after Conversion from Conventional Hemodialysis to In-Centre Nocturnal Hemodialysis. J Nephrol 32, 273–281 (2019). https://doi.org/10.1007/s40620-018-0522-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-018-0522-2