Abstract
Objectives
To explore the value of an ultrasound contrast agent (Sonovue) as an interventional treatment for periappendiceal abscesses.
Methods
From January 2019 to December 2020, 30 patients were recruited who were admitted to Jinan Central Hospital due to periappendiceal abscesses. Before the operation, 2.5 ml of SonoVue® contrast agent was injected intravenously to determine the non-enhanced area of liquefaction and necrosis in the abscess cavity. The puncture sites were selected. Percutaneous catheterization and drainage (PCD) were performed under contrast-enhanced ultrasound guidance. After the operation, 1 ml of diluted SonoVue® suspension was injected through the drainage tube to observe the position of the drainage tube, the degree of drainage and the development of the abscess.
Results
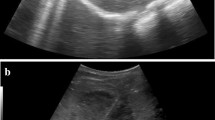
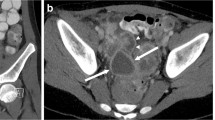
An ultrasound contrast agent was used preoperatively to assess the extent of the abscess. Liquefaction and necrosis were observed in the abscess cavity. CEUS showed hyperenhancement in the wall of the abscess in the arterial phase and the liquefied necrotic area in the abscess cavity was not enhanced before PCD. CEUS allowed operators to confidently identify the puncture site. Amongst the 30 cases of PCD, 27 cases showed the clear positioning of the drainage tube. The head of the drainage tube was placed in the ideal position and development could be seen in the abscess cavity. The diffusion effect of the contrast agent was good with no spillover and the drainage was unobstructed. Abscess development was observed in 3 patients after puncture injection of the contrast agent but the head of the drainage tube was not in the predetermined position. After adjusting the position of the drainage tube, CEUS was repeated and showed a strong diffusion effect of the contrast agent.
Conclusions
Intravenous injection of Sonovue before PCD of periappendiceal abscesses can evaluate the extent of the abscess, liquefaction and necrosis in the abscess cavity. The approach can also provide guidance for the placement of the drainage tube. After the operation, a diluted contrast agent was injected through the drainage tube. The position of the drainage tube and the flow direction of the contrast agent could be seen. This approach has good value for clinical applications to accurately judge the position of the drainage tube.




Similar content being viewed by others
References
Zhang Y, Stringel G, Bezahler I, Maddineni S (2020) Nonoperative management of periappendiceal abscess in children: a comparison of antibiotics alone versus antibiotics plus percutaneous drainage. J Pediatr Surg 55(3):414–417. https://doi.org/10.1016/j.jpedsurg.2019.09.005
Al-Kurd A, Mizrahi I, Siam B et al (2018) Outcomes of interval appendectomy in comparison with appendectomy for acute appendicitis. J Surg Res 225:90–94. https://doi.org/10.1016/j.jss.2018.01.012
Zani A, Hall NJ, Rahman A et al (2019) European Paediatric Surgeons’ Association survey on the management of pediatric appendicitis. Eur J Pediatr Surg 29(1):53–61. https://doi.org/10.1055/s-0038-1668139
Rosenbaum DG, Askin G, Beneck DM, Kovanlikaya A (2017) Differentiating perforated from non-perforated appendicitis on contrast-enhanced magnetic resonance imaging. Pediatr Radiol 47(11):1483–1490. https://doi.org/10.1007/s00247-017-3900-3
Luo CC, Cheng KF, Huang CS et al (2016) Therapeutic effectiveness of percutaneous drainage and factors for performing an interval appendectomy in pediatric appendiceal abscess. BMC Surg 16(1):72. https://doi.org/10.1186/s12893-016-0188-4
Guida E, Pederiva F, Grazia MD et al (2015) Perforated appendix with abscess: Immediate or interval appendectomy? Some examples to explain our choice. Int J Surg Case Rep 12:15–18. https://doi.org/10.1016/j.ijscr.2015.05.003
Gu G, Ren J, Liu S et al (2015) Comparative evaluation of sump drainage by trocar puncture, percutaneous catheter drainage versus operative drainage in the treatment of Intra-abdominal abscesses: a retrospective controlled study. BMC Surg 15:59. https://doi.org/10.1186/s12893-015-0049-6
Levin DC, Eschelman D, Parker L, Rao VM (2015) Trends in use of percutaneous versus open surgical drainage of abdominal abscesses. J Am Coll Radiol. 12(12 Pt A):1247–1250. https://doi.org/10.1016/j.jacr.2015.06.015
Yeom S, Kim MS, Park S et al (2014) Comparison of the outcomes of laparoscopic and open approaches in the treatment of periappendiceal abscess diagnosed by radiologic investigation. J Laparoendosc Adv Surg Tech A 24(11):762–769. https://doi.org/10.1089/lap.2014.0224
Yusuf GT, Fang C, Huang DY, Sellars ME, Deganello A, Sidhu PS (2018) Endocavitary contrast enhanced ultrasound (CEUS): a novel problem solving technique. Insights Imaging 9(3):303–311. https://doi.org/10.1007/s13244-018-0601-x
Badea R, Ciobanu L, Gomotirceanu A, Hagiu C, Socaciu M (2010) Contrast ultrasonography of the digestive tract lumen. Review of the literature and personal experience. Med Ultrason. 12(1):52–61
Horn CB, Coleoglou Centeno AA, Guerra JJ, Mazuski JE, Bochicchio GV, Turnbull IR (2018) Drain failure in intra-abdominal abscesses associated with appendicitis. Surg Infect (Larchmt) 19(3):321–325. https://doi.org/10.1089/sur.2017.224
Olsen J, Skovdal J, Qvist N, Bisgaard T (2014) Treatment of appendiceal mass–a qualitative systematic review. Dan Med J 61(8):A4881
Deelder JD, Richir MC, Schoorl T, Schreurs WH (2014) How to treat an appendiceal inflammatory mass: operatively or nonoperatively? J Gastrointest Surg 18(4):641–645. https://doi.org/10.1007/s11605-014-2460-1
Tannoury J, Abboud B (2013) Treatment options of inflammatory appendiceal masses in adults. World J Gastroenterol 19(25):3942–3950. https://doi.org/10.3748/wjg.v19.i25.3942
Bahram MA (2011) Evaluation of early surgical management of complicated appendicitis by appendicular mass. Int J Surg 9(1):101–103. https://doi.org/10.1016/j.ijsu.2010.10.006
Marin D, Ho LM, Barnhart H, Neville AM, White RR, Paulson EK (2010) Percutaneous abscess drainage in patients with perforated acute appendicitis: effectiveness, safety, and prediction of outcome. AJR Am J Roentgenol 194(2):422–429. https://doi.org/10.2214/AJR.09.3098
Farach SM, Danielson PD, Chandler NM (2015) Preprocedural coagulation studies in pediatric patients undergoing percutaneous intervention for appendiceal abscesses. Am Surg 81(9):859–864
Chang CR, Cheng CY (2014) Drainage of periappendiceal abscess and removal of free fecalith–extraperitoneal approach. Int Surg 99(4):379–383. https://doi.org/10.9738/INTSURG-D-13-00040.1
Kim M, Oh ST (2016) Effect of time delays for appendectomy as observed on computed tomography in patients with noncomplicated appendicitis. Am J Emerg Med 34(2):167–169. https://doi.org/10.1016/j.ajem.2015.10.009
McNeeley MF, Vo NJ, Prabhu SJ, Vergnani J, Shaw DW (2012) Percutaneous drainage of intra-abdominal abscess in children with perforated appendicitis. Pediatr Radiol 42(7):805–812. https://doi.org/10.1007/s00247-011-2337-3
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Jinan central hospital.
Informed consent
Informed consent was obtained from the individual participant included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, W., Zhao, X., Zhang, Q. et al. The Application of Dual-Pathway Contrast-Enhanced Ultrasound (CEUS) in the Treatment of Periappendiceal Abscesses. J Ultrasound 25, 973–977 (2022). https://doi.org/10.1007/s40477-022-00692-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-022-00692-1