Abstract
Aim
To evaluate possible associations between successful mandibular block injection and location of penetrating the oral mucosa, location of injection on the ramus and the needle insertion length.
Study design
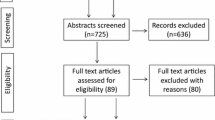
The study consisted of 101 dentists, of whom, 33 were oral surgeons, 33 certified paediatric dentists and 35 general dental practitioners. The dentists were asked to estimate their rate of success in mandibular block injections, defined as the proportion of their patients for whom only a single carpule was necessary, and to indicate the needle insertion length and the location of the injection on a photograph of a ramus and on a photograph of the oral mucosa.
Results
Injecting a single carpule for achieving full anaesthesia in 90 % or more of their patients was reported by 79.3 and 57.8 % of the dentists treating children and adults, respectively. Of practitioners treating children, experienced dentists (>5 years in occupation) reported higher success rates than did inexperienced ones (p = 0.05). A positive correlation was found between failure rate reported in children, shorter length of the inserted needle (R = 0.356, p = 0.001) and injecting at the central (superior inferior dimension) most anterior quarters of the ramus (p = 0.006; odd ratio = 3.9375). Routine waiting period of more than 5 min after the injection and before operative treatment was associated with higher rates of failure (p = 0.042, χ2 = 6.335).
No correlation was found between the success rates of mandibular block injection and the location of penetrating the oral mucosa in children (p = 0.94), adults (p = 0.57), or between success rates and the target location on the ramus in adults (p = 0.42).
Statistics
χ2 test was used to determine the significance of differences among proportions and t test for continuous variables. Pearson’s correlation analysis was used to analyse the correlation between the length of the needle inserted in children and adults by the same dentist.
Conclusions
Shorter needle insertion lengths and targeting the injecting to the most anterior quarters of the ramus were positively correlated with failure of anaesthesia in children, according to dentists’ reports. A routine waiting period of over 5 min did not increase the success rates of mandibular block injection.





Similar content being viewed by others
References
Ashkenazi M, Taubman L, Gavish A. Age-associated changes of the mandibular foramen position in anteroposterior dimension and of the mandibular angle in dry human mandibles. Anat Rec. 2011;294:1319–25.
Benham NR. The cephalometric position of the mandibular foramen with age. ASDC J Dent Child. 1976;43:233–7.
Childers M, Reader A, Nist R, Beck M, Meyers WJ. Anesthetic efficacy of the periodontal ligament injection after an inferior alveolar nerve block. J Endod. 1996;22:317–20.
da Fontoura RA, Vasconcellos HA, Campos AE. Morphologic basis for the intraoral vertical ramus osteotomy: anatomic and radiographic localization of the mandibular foramen. J Oral Maxillofac Surg 2002;60: 660–5 (discussion 665–6).
Fujimura K, Segami N, Kobayashi S. Anatomical study of the complications of intraoral vertico-sagittal ramus osteotomy. J Oral Maxillofac Surg. 2006;64:384–9.
Hayward J, Richardson ER, Malhotra SK. The mandibular foramen: its anteroposterior position. Oral Surg Oral Med Oral Pathol. 1977;44:837–43.
Harrison SM. Regional anesthesia for children. Dent Rec. 1948;68:146–55.
Hetson G, Share J, Frommer J, Kronman JH. Statistical evaluation of the position of the mandibular foramen. Oral Surg Oral Med Oral Pathol. 1988;65:32–4.
Jorgensen NB, Hayden JJ. Sedation, local and general anesthesia in dentistry, 3rd ed. Philadelphia: Lea & Febiger; 1980. p. 98.
Kaufman E, Weinstein P, Milgrom P. Difficulties in achieving local anesthesia. J Am Dent Assoc. 1984;108:205–8.
Malamed SF. Handbook of local anesthesia, 5th ed. California: Elsevier Mosby; 2004. p. 231, 274–5.
McDonald RE, Avery DR, Dean JA. Local anesthesia and pain control for the child and adolescent. In: McDonald RE, Avery DR, Dean JA, editors. Dentistry for the child and adolescent. 8th ed. St. Louis: Mosby; 2004. p. 273.
Monheim LM. Local anesthesia and pain control in dental practice. 4th ed. St. Louis: The C.V. Mosby Company; 1969. p. 47.
Nicholson ML. A study of the position of the mandibular foramen in the adult human mandible. Anat Rec. 1985;212:110–2.
Pinkham JR, Casamassimo PS, McTigue DJ, Fields HW, Nowak AJ, editors. Paediatric dentistry: infancy through adolescence. 4th ed. St. Louis, MO: Elsevier Saunders; 2005. p. 452–3.
Ricketts RM. Mechanisms of mandibular growth: a series of inquiries on the growth of the mandible, determinants of mandibular form and growth. Ann Arbor: Center for Human Growth and Development, The University of Michigan. 1975. p. 77–100.
Sweet APS. Canals and foramina of maxilla and mandible. Dent Radiogr Photogr. 1943;16:13–6.
Tsai HH. Panoramic radiographic findings of the mandibular growth from deciduous dentition to early permanent dentition. J Clin Pediatr Dent. 2002;26:279–84.
Tsai HH. Panoramic radiographic findings of the mandibular foramen from deciduous to early permanent dentition. J Clin Pediatr Dent. 2004;28:215–9.
Weiss KM. On the systematic bias in skeletal sexing. Am J Phys Anthropol. 1972;37:239–49.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Questionnaire
Demographic questions: gender; age; years in practice; specialty (yes/no); type of specialty (paediatric dentistry, oral surgery), number of years in specialty.
Which population do you usually treat? (Children, adults, children and adults).
Please mark on the attached figure of the oral mucosa the location you usually penetrate to inject routine inferior alveolar block (mandibular block) in children.
Please mark on the attached figure of the oral mucosa the location you usually penetrate to inject mandibular block in adults.
Please mark on the attached figure of the mandibular ramus the location you usually direct your injection to, when you deliver routine inferior alveolar block (mandibular block) in children.
Please mark on the attached figure of the mandibular ramus the location you usually direct your injection when you deliver routine inferior alveolar block (mandibular block) in adults.
What is the needle length that you usually leave out of the oral mucosa during delivery of routine inferior alveolar block (mandibular block) injection in children? Please mark the needle length on the attached figure according to the length of needle you usually used (short or long).
What is the needle length that you usually leave out of the oral mucosa during delivery of routine inferior alveolar block (mandibular block) injection in adults? Please mark the needle length on the attached figure according to the length of needle you usually used (short or long).
How long (minutes) do you usually wait after completion of routine inferior alveolar block (mandibular block) injection and before starting the operative treatment in children? (A. 0–1 min, B. 2–5 min, C. 5–10 min, D. Over 10 min).
How long (minutes) do you usually wait after completion of routine inferior alveolar block (mandibular block) injection and before starting the operative treatment in adults? (A. 0–1 min, B. 2–5 min, C. 5–10 min, D. Over 10 min).
In what percentage of your child patients do you need to inject another carpule of local analgesic in order to achieve full analgesia (no complaint of pain)? A. 0–5 %, B. 6–10 %, C. 11–15 %, D. 16–20 %, E. 21–25 %, F. 26–40 %, G. Over 40 %.
In what percentage of your adult-patients do you need to inject another carpule of local analgesic to achieve full analgesia (no complaint of pain)? A. 0–5 %, B. 6–10 %, C. 11–15 %, D. 16–20 %, E. 21–25 %, F. 26–40 %, G. Over 40 %.
When your patients complain of pain, in what frequency do you attribute it to pressure?
A. 0–10 % of the cases, B. 10–25 % of the cases, C. Over 25 %.
Rights and permissions
About this article
Cite this article
Ashkenazi, M., Sher, I., Rackoz, M. et al. Mandibular block success rate in relation to needle insertion and position: a self-report survey. Eur Arch Paediatr Dent 15, 121–126 (2014). https://doi.org/10.1007/s40368-013-0073-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-013-0073-0