Abstract
Purpose of Review
Review latest data regarding the intersection of pediatric obesity epidemic with telemedicine expansion to meet the need of equitable obesity care in children.
Recent Findings
Prevalence of pediatric obesity in the USA continues to worsen particularly in rural, underserved areas. Although there is an increasing number of obesity medicine specialists over the last decade, availability varies by geographic location. Pre-pandemic centers were limited, rarely located in rural areas, and required in-person visits for reimbursement. Telemedicine changes, responding to pandemic needs, provided increase in telemedicine utilization and acceptance with similar or improved obesity care outcomes.
Summary
Given pediatric obesity prevalence and need for chronic, effective obesity care, leveraging telemedicine to expand reach and decrease access barriers provides a critical and creative remedy. Data cites similar outcomes between telemedicine and in-person care. The time to reimagine a full spectrum of care delivery for pediatric obesity is now.

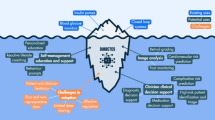
Source: Upper Midwest Telehealth Resource Center (https://www.umtrc.org/clientuploads/UMTRC%20Resource%20PDF/Updated_Telehealth_and_Telemedicine_Timeline.pdf) with permission [29]
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Important reference •• Very important reference
World Health Organization. World obesity day 2022. WHO. Accessed Jun 11, 2023. https://www.who.int/news/item/04-03-2022-world-obesity-day-2022-accelerating-action-to-stop-obesity.
Woodruff RC, Campbell AP, Taylor CA, Chai SJ, Kawasaki B, Meek J, Anderson EJ, Weigel A, Monroe ML, Reeg L, Bye E, Sosin DM, Muse A, Bennett NM, Billing LM, Sutton M, Talbot HK, McCaffrey K, Pham H, Patel K, Whitaker M, L McMorrow M, P Havers F. Risk factors for severe COVID-19 in children. Pediatrics. 2022;149(1):e2021053418. https://doi.org/10.1542/peds.2021-053418. Epub 2021 Dec 22. PMID: 34935038; PMCID: PMC9213563.
Ward ZJ, Long MW, Resch SC, Giles CM, Cradock AL, Gortmaker SL. Simulation of growth trajectories of childhood obesity into adulthood. N Engl J Med. 2017;377(22):2145–53. https://doi.org/10.1056/NEJMoa1703860. PMID: 29171811; PMCID: PMC9036858.
Gudzune KA, Johnson VR, Bramante CT, Stanford FC. Geographic availability of physicians certified by the American Board of Obesity Medicine relative to obesity prevalence. Obesity (Silver Spring). 2019;27(12):1958–1966. https://doi.org/10.1002/oby.22628. Epub 2019 Sep 13. PMID: 31515965; PMCID: PMC6868336.
Kaye AD, Okeagu CN, Pham AD, Silva RA, Hurley JJ, Arron BL, Sarfraz N, Lee HN, Ghali GE, Gamble JW, Liu H, Urman RD, Cornett EM. Economic impact of COVID-19 pandemic on healthcare facilities and systems: international perspectives. Best Pract Res Clin Anaesthesiol. 2021;35(3):293–306. https://doi.org/10.1016/j.bpa.2020.11.009. Epub 2020 Nov 17. PMID: 34511220; PMCID: PMC7670225.
• Cuda S, Censani M, Kharofa R, O'Hara V, Conroy R, Williams D, Paisley J, Browne A, Karjoo S, Browne NT. Medication-induced weight gain and advanced therapies for the child with overweight and obesity: an Obesity Medicine Association (OMA) Clinical Practice Statement 2022, Obesity Pillars. 2022;4:100048, ISSN 2667–3681. https://doi.org/10.1016/j.obpill.2022.100048. Provides comprehensive review of advanced treatment for pediatric obesity.
O’Hara V, Cuda S, Kharofa R, Censani M, Conroy R, Browne NT. Clinical review: guide to pharmacological management in pediatric obesity medicine. Obesity Pillars. 2023;6:100066, ISSN 2667–3681. https://doi.org/10.1016/j.obpill.2023.100066.
Flattum C, Friend S, Horning M, Lindberg R, Beaudette J, Fulkerson JA. Family-focused obesity prevention program implementation in urban versus rural communities: a case study. BMC Public Health. 2021;21(1):1915. https://doi.org/10.1186/s12889-021-11967-3. PMID: 34674674; PMCID: PMC8532281.
SanGiovanni C, McElligott J, Morella K, Basco W Jr. Underdiagnosis and lower rates of office visits for overweight/obese pediatric patients in rural compared with urban areas. South Med J. 2017;110(7):480–5. https://doi.org/10.14423/SMJ.0000000000000672. PMID: 28679018.
Strochlic R, Au LE, Ritchie L. Is urban-rural location associated with weight status in school children? An examination of 42 small and rural Californian counties. Rural Remote Health. 2017;17(2):3966. https://doi.org/10.22605/RRH3966. Epub 2017 Apr 18. PMID: 28415846.
Ogden CL, Fryar CD, Hales CM, Carroll MD, Aoki Y, Freedman DS. Differences in obesity prevalence by demographics and urbanization in US children and adolescents, 2013–2016. JAMA. 2018;319(23):2410–8. https://doi.org/10.1001/jama.2018.5158. PMID: 29922826; PMCID: PMC6393914 .
Srivastava G, Browne N, Kyle TK, O’Hara V, Browne A, Nelson T, Puhl R. Caring for US children: barriers to effective treatment in children with the disease of obesity. Obesity (Silver Spring). 2021;29(1):46–55. https://doi.org/10.1002/oby.22987. PMID: 34494365.
Halford JCG, Bereket A, Bin-Abbas B, Chen W, Fernández-Aranda F, Garibay Nieto N, López Siguero JP, Maffeis C, Mooney V, Osorto CK, Reynoso R, Rhie YJ, Toro-Ramos M, Baur LA. Misalignment among adolescents living with obesity, caregivers, and healthcare professionals: ACTION Teens global survey study. Pediatr Obes. 2022;17(11):e12957. https://doi.org/10.1111/ijpo.12957. Epub 2022 Jul 15. PMID: 35838551.
• Hampl SE, Hassink SG, Skinner AC, Armstrong SC, Barlow SE, Bolling CF, Avila Edwards KC, Eneli I, Hamre R, Joseph MM, Lunsford D, Mendonca E, Michalsky MP, Mirza N, Ochoa ER, Sharifi M, Staiano AE, Weedn AE, Flinn SK, Lindros J, Okechukwu K. Clinical Practice Guideline for the evaluation and treatment of children and adolescents with obesity. Pediatrics. 2023;151(2):e2022060640. https://doi.org/10.1542/peds.2022-060640. Important first AAP CPG since 2007 highlighting the need to treat obesity as a chronic disease using all available therapies.
Di Cesare M, Sorić M, Bovet P, Miranda JJ, Bhutta Z, Stevens GA, Laxmaiah A, Kengne AP, Bentham J. The epidemiological burden of obesity in childhood: a worldwide epidemic requiring urgent action. BMC Med. 2019;17(1):212. https://doi.org/10.1186/s12916-019-1449-8. PMID: 31760948; PMCID: PMC6876113.
Kelly AS, Auerbach P, Barrientos-Perez M, Gies I, Hale PM, Marcus C, Mastrandrea LD, Prabhu N, Arslanian S; NN8022–4180 Trial Investigators. A randomized, controlled trial of Liraglutide for adolescents with obesity. N Engl J Med. 2020;382(22):2117–2128. https://doi.org/10.1056/NEJMoa1916038. Epub 2020 Mar 31. PMID: 32233338.
Kelly AS, Bensignor MO, Hsia DS, Shoemaker AH, Shih W, Peterson C, Varghese ST. Phentermine/topiramate for the treatment of adolescent obesity. NEJM Evid. 2022. https://doi.org/10.1056/evidoa2200014. Epub 2022 Apr 30. PMID: 36968652; PMCID: PMC10035585.
Weghuber D, Barrett T, Barrientos-Pérez M, Gies I, Hesse D, Jeppesen OK, Kelly AS, Mastrandrea LD, Sørrig R, Arslanian S; STEP TEENS Investigators. Once-weekly semaglutide in adolescents with obesity. N Engl J Med. 2022;387(24):2245–2257. https://doi.org/10.1056/NEJMoa2208601. Epub 2022 Nov 2. PMID: 36322838; PMCID: PMC9997064.
Clément K, van den Akker E, Argente J, Bahm A, Chung WK, Connors H, De Waele K, Farooqi IS, Gonneau-Lejeune J, Gordon G, Kohlsdorf K, Poitou C, Puder L, Swain J, Stewart M, Yuan G, Wabitsch M, Kühnen P; Setmelanotide POMC and LEPR Phase 3 Trial Investigators. Efficacy and safety of setmelanotide, an MC4R agonist, in individuals with severe obesity due to LEPR or POMC deficiency: single-arm, open-label, multicentre, phase 3 trials. Lancet Diab Endocrinol. 2020;8(12):960–970. https://doi.org/10.1016/S2213-8587(20)30364-8. Epub 2020 Oct 30. PMID: 33137293.
Cuda S, Censani M. Progress in pediatric obesity: new and advanced therapies. Curr Opin Pediatr. 2022;34(4):407–13. https://doi.org/10.1097/MOP.0000000000001150. Epub 2022 Jul 5 PMID: 35797460.
Lazareva J, Brady SM, Yanovski JA. An evaluation of setmelanotide injection for chronic weight management in adult and pediatric patients with obesity due to Bardet-Biedl syndrome. Expert Opin Pharmacother. 2023;24(6):667–674. https://doi.org/10.1080/14656566.2023.2199152. Epub 2023 Apr 6. PMID: 37013719; PMCID: PMC10121918.
Gross AC, Kaizer AM, Kelly AS, Rudser KD, Ryder JR, Borzutzky CR, Santos M, Tucker JM, Yee JK, Fox CK; POWER Work Group. Long and short of it: early response predicts longer-term outcomes in pediatric weight management. Obesity (Silver Spring). 2019;27(2):272–279. https://doi.org/10.1002/oby.22367. PMID: 30677263; PMCID: PMC6352906.
Herdes RE, Tsao DD, Pratt JSA. Why earlier may be better: a look at the use of metabolic and bariatric surgery in the treatment of severe childhood obesity. Surg Obes Relat Dis. 2021;17(12):2107–10. https://doi.org/10.1016/j.soard.2021.09.003. (Epub 2021 Sep 8 PMID: 34565685).
Borzutzky C, King E, Fox CK, Stratbucker W, Tucker J, Yee JK, Kumar S, Cuda S, Sweeney B, Kirk S, On Behalf Of The Power Work Group. Trends in prescribing anti-obesity pharmacotherapy for paediatric weight management: data from the POWER Work Group. Pediatr Obes. 2021;16(1):e12701. https://doi.org/10.1111/ijpo.12701. Epub 2020 Sep 2. PMID: 32877010.
• Woo Baidal JA, Chang J, Hulse E, Turetsky R, Parkinson K, Rausch JC. Zooming toward a telehealth solution for vulnerable children with obesity during coronavirus disease 2019. Obesity (Silver Spring). 2020;28(7):1184–1186. https://doi.org/10.1002/oby.22860. Epub 2020 Jun 10. PMID: 32352650; PMCID: PMC7267304. Provides a review of utility of telemedicine for children with obesity which was highlighted during COVID.
Project ECHO. University of New Mexico. Accessed June 11, 2023. Available at https://hsc.unm.edu/echo/.
Lewiecki EM, Rochelle R. Project ECHO: telehealth to expand capacity to deliver best practice medical care. Rheum Dis Clin North Am. 2019;45(2):303–14. https://doi.org/10.1016/j.rdc.2019.01.003.
Novick MB, Wilson CT, Walker-Harding LR. Potential solutions for pediatric weight loss programs in the treatment of obesity in rural communities. Transl Behav Med. 2019;9(3):460–7. https://doi.org/10.1093/tbm/ibz030.
Updated telehealth and telemedicine timeline. Accessed June 11, 2023. https://www.umtrc.org/clientuploads/UMTRC%20Resource%20PDF/Updated_Telehealth_and_Telemedicine_Timeline.pdf.
•• Centers for Medicare and Medicaid Services. COVID-19 emergency declaration blanket waivers for health care providers. Updated October 13, 2023. Accessed June 11, 2023. Available at COVID-19 Emergency Declaration Blanket Waivers for Health Care Providers (cms.gov). Important reference for all providers using telehealth now and going forward after PHE.
Assistant Secretary for Planning and Evaluation. Medicare beneficiaries’ use of telehealth in 2020: trends by beneficiary characteristics and location. ASPE Office of Health Policy Research. Published December 2021. Accessed June 11, 2023. https://aspe.hhs.gov/sites/default/files/documents/a1d5d810fe3433e18b192be42dbf2351/medicare-telehealth-report.pdf.
Center for Connected Health Policy. Medicare telehealth/connected health waivers post-PHE. Published March 2, 2023. Accessed June 11, 2023 at https://www.cchpca.org/2023/03/MEDICARE-TELEHEALTH-POLICIES-POST-PHE-AT-A-GLANCE-FINAL-MAR-2023.pdf.
Drug Enforcement Association & Health and Human Services Department. Temporary extension of COVID-19 telemedicine flexibilities for prescription of controlled medications. Published May 10, 2023. Accessed June 11, 2023 at https://www.federalregister.gov/documents/2023/05/10/2023-09936/temporary-extension-of-covid-19-telemedicine-flexibilities-for-prescription-of-controlled.
National Center for Interstate Compacts. Interstate licensure compacts. Accessed June 11, 2023. https://compacts.csg.org/covid-policy-responses/interstate-licensure-compacts/.
Fang ML, Walker M, Wong KLY, Sixsmith J, Remund L, Sixsmith A. Future of digital health and community care: exploring intended positive impacts and unintended negative consequences of COVID-19. Healthc Manage Forum. 2022;35(5):279–285. https://doi.org/10.1177/08404704221107362. Epub 2022 Jul 1. PMID: 35775162; PMCID: PMC9253718.
U.S. Department of Commerce National Telecommunications and Information Administration. Digital Equity Plan Guidance. https://broadbandusa.ntia.gov/sites/default/files/2022-09/Digital_Equity_Plan_Guidance.pdf. Accessed 11 June 2023.
Federal Communications Commission. Chairman Pai Archive: Bridging The Digital Divide For All Americans. Accessed June 11, 2023 at https://www.fcc.gov/ajit-pai-initiatives-archive.
Friedman AB, Gervasi S, Song H, Bond AM, Chen AT, Bergman A, David G, Bailey JM, Brooks R, Smith-McLallen A. Telemedicine catches on: changes in the utilization of telemedicine services during the COVID-19 pandemic. Am J Manag Care. 2022;28(1):e1–6. https://doi.org/10.37765/ajmc.2022.88771. PMID: 35049260.
North S. Expanding telehealth in adolescent care: moving beyond the COVID-19 pandemic. Pediatrics. 2023;151(Suppl 1):e2022057267J. https://doi.org/10.1542/peds.2022-057267J. PMID: 37010401.
Notario PM, Gentile E, Amidon M, Angst D, Lefaiver C, Webster K. Home-based telemedicine for children with medical complexity. Telemed J E Health. 2019 Nov;25(11):1123–1132. https://doi.org/10.1089/tmj.2018.0186. Epub 2019 Jan 30. PMID: 30628860; PMCID: PMC6842894
Moorman EL, Koskela-Staples NC, Mathai BB, Fedele DA, Janicke DM. Pediatric obesity treatment via telehealth: current evidence and future directions. Curr Obes Rep. 2021;10(3):371–84. https://doi.org/10.1007/s13679-021-00446-w. Epub 2021 Jul 24 PMID: 34302603.
Qiu LT, Sun GX, Li L, Zhang JD, Wang D, Fan BY. Effectiveness of multiple eHealth-delivered lifestyle strategies for preventing or intervening overweight/obesity among children and adolescents: a systematic review and meta-analysis. Front Endocrinol (Lausanne). 2022;5(13):999702. https://doi.org/10.3389/fendo.2022.999702. PMID: 36157474; PMCID: PMC9491112 .
Srivastava G, Fox CK, Kelly AS, Jastreboff AM, Browne AF, Browne NT, Pratt JSA, Bolling C, Michalsky MP, Cook S, Lenders CM, Apovian CM. Clinical considerations regarding the use of obesity pharmacotherapy in adolescents with obesity. Obesity (Silver Spring). 2019;27(2):190–204. https://doi.org/10.1002/oby.22385. PMID: 30677262; PMCID: PMC6449849 .
• O'Hara VM, Johnston SV, Browne NT. The paediatric weight management office visit via telemedicine: pre- to post-COVID-19 pandemic. Pediatr Obes. 2020;15(8):e12694. https://doi.org/10.1111/ijpo.12694. Epub 2020 Jul 6. PMID: 32627434; PMCID: PMC7361154. Provides pre-pandemic to post-pandemic pediatric clinical care in a multidisciplinary setting experience along with important telehealth policies.
•• DeSilva S, Vaidya SS. The application of telemedicine to pediatric obesity: lessons from the past decade. Telemed J e-Health. 2021;27(2):159–66. https://doi.org/10.1089/tmj.2019.0314. Provides important 10-year review specifically for pediatric obesity using telemedicine.
Pecoraro P, Gallè F, Muscariello E, Di Mauro V, Daniele O, Forte S, Ricchiuti R, Liguori G, Valerio G. A telehealth intervention for ensuring continuity of care of pediatric obesity during the CoVid-19 lockdown in Italy. Nutr Metab Cardiovasc Dis. 2021;31(12):3502–3507. https://doi.org/10.1016/j.numecd.2021.09.026. Epub 2021 Oct 7. PMID: 34728130; PMCID: PMC8496959.
Calcaterra V, Verduci E, Vandoni M, Rossi V, Di Profio E, CarnevalePellino V, Tranfaglia V, Pascuzzi MC, Borsani B, Bosetti A, Zuccotti G. Telehealth: a useful tool for the management of nutrition and exercise programs in pediatric obesity in the COVID-19 era. Nutrients. 2021;13(11):3689. https://doi.org/10.3390/nu13113689. PMID: 34835945; PMCID: PMC8618189.
• Kouvari M, Karipidou M, Tsiampalis T, et al. Digital health interventions for weight management in children and adolescents: systematic review and meta-analysis. J Med Internet Res. 2022;24(2):e30675. Published 2022 Feb 14. https://doi.org/10.2196/30675. Review of telehealth tools in hybrid model, need for more research for fully telehealth delivery.
Whitley A, Yahia N. Efficacy of clinic-based telehealth vs. face-to-face interventions for obesity treatment in children and adolescents in the United States and Canada: a systematic review. Child Obes. 2021;17(5):299–310. https://doi.org/10.1089/chi.2020.0347. Epub 2021 Apr 29. PMID: 33926238.
• Umano GR, Di Sessa A, Guarino S, Gaudino G, Marzuillo P, Miraglia Del Giudice E. Telemedicine in the COVID-19 era: taking care of children with obesity and diabetes mellitus. World J Diabetes. 2021;12(5):651–7. https://doi.org/10.4239/wjd.v12.i5.651. PMID: 33995852; PMCID: PMC8107973. Discusses impact of telemedicine on obesity and related complication of diabetes during covid.
Rajkumar E, Gopi A, Joshi A, et al. Applications, benefits, and challenges of telehealth in India during COVID-19 pandemic and beyond: a systematic review. BMC Health Serv Res. 2023;23(1):7. Published 2023 Jan 4. https://doi.org/10.1186/s12913-022-08970-8
Aras M, Tchang BG, Crawford A, Bledsoe M, Fujioka K, Aronne LJ. Impact of telemedicine during the COVID-19 pandemic on patient attendance. Obesity (Silver Spring). 2021;29(7):1093–1094. https://doi.org/10.1002/oby.23180. Epub 2021 May 7. PMID: 33963678; PMCID: PMC8242458.
• Tchang BG, Morrison C, Kim JT, Ahmed F, Chan KM, Alonso LC, Aronne LJ, Shukla AP. Weight loss outcomes with telemedicine during COVID-19. Front Endocrinol (Lausanne). 2022;10(13):793290. https://doi.org/10.3389/fendo.2022.793290. PMID: 35360066; PMCID: PMC8960113. Provides data comparing various delivery models for obesity medicine care with clinical outcomes across telemedicine, hybrid, and face-to-face comparison. Highlights the need for pediatric data regarding similar study.
•• Crawford A, Serhal E. Digital health equity and COVID-19: the innovation curve cannot reinforce the social gradient of health. J Med Internet Res. 2020;22(6):e19361. https://doi.org/10.2196/19361. PMID: 32452816; PMCID: PMC7268667. Provides important perspectives on equity as well as insights for potential solutions.
Cueto V, Sanders LM. Telehealth opportunities and challenges for managing pediatric obesity. Pediatr Clin North Am. 2020;67(4):647–54. https://doi.org/10.1016/j.pcl.2020.04.007. PMID: 32650862.
• Christison AL, Ariza AJ, Fernandez C, Kumar S, Novick MB, Santos M, Stratbucker WB, Sweeney BR, Vidmar A, Kirk S. Challenges and solutions to sustaining paediatric weight management programs in the United States. Clin Obes. 2023;11:e12577. https://doi.org/10.1111/cob.12577. Epub ahead of print. PMID: 36631245. Addresses multiple considerations regarding sustaining pediatric obesity care assess, telemedicine a key factor learned because of the pandemic experience.
Kaplan LM, Golden A, Jinnett K, Kolotkin RL, Kyle TK, Look M, Nadglowski J, O’Neil PM, Parry T, Tomaszewski KJ, Stevenin B, Lilleøre SK, Dhurandhar NV. Perceptions of barriers to effective obesity care: results from the national ACTION Study. Obesity (Silver Spring). 2018;26(1):61–9. https://doi.org/10.1002/oby.22054. Epub 2017 Oct 31 PMID: 29086529.
Puhl RM, Lessard LM. Weight stigma in youth: prevalence, consequences, and considerations for clinical practice. Curr Obes Rep. 2020;9(4):402–11. https://doi.org/10.1007/s13679-020-00408-8. Epub 2020 Oct 20 PMID: 33079337.
Pearl R, Wayling B. The telehealth era is just beginning. Harv Bus Rev. 2022. https://hbr.org/2022/05/the-telehealth-era-is-just-beginning.
Author information
Authors and Affiliations
Contributions
All authors were involved in writing the article and had final approval of the submitted and published versions.
Corresponding author
Ethics declarations
Conflict of Interest
Valerie M. O’Hara: Novo Nordisk that includes consulting speaking and lecture fee Danielle Louder: U.S. HHS Health Resources and Services Administration: Regional Resource Center (TRC) Program Cooperative Agreement 2021–2024;Telehealth Technology Enabled Learning Program Cooperative Agreement (TTELP) 2021–2025. Maine DHHS—Office of MaineCare Services: Contract for telehealth integration into Private non-Medical Institutions (PNMIs) 2022–2024. Maine DHHS – Center for Disease Control and Prevention: Contract for piloting a state-wide eConsult Network 2022–2024. Children’s Oral Health Network: Contract for Virtual Dental Home pilot 2022–2023. Vermont Program for Quality in Health Care: Contract for state-wide Telepsychiatry Network development 2022–2023. DHHS Health Resources and Services Administration – Office for the Advancement of Telehealth: Travel expenses for conferences, presentations and meetings under Regional Telehealth Resource Center Cooperative Agreement. All other authors have no conflict of interest to declare.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
O’Hara, V.M., Louder, D., Johnston, S.V. et al. Pediatric Obesity Care via Telemedicine: Expanding the Path Forward—A Review. Curr Obes Rep 12, 546–556 (2023). https://doi.org/10.1007/s13679-023-00537-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13679-023-00537-w