Abstract
Purpose of Review
To discuss the current evidence regarding the association and mechanistic interaction between asthma and obstructive sleep apnea (OSA).
Recent Findings
The co-existence of OSA is highly prevalent in asthmatics and significantly associated with increased severity, decreased control, more frequent exacerbations, and hospitalizations despite medical management. Pre-existing asthma may also be a risk factor for new onset OSA. Rhinitis, obesity, and gastro-esophageal reflux are risk factors in both conditions. The obese asthmatic with OSA may present a unique phenotype. Positive airway pressure in severe asthma improves outcomes.
Summary
Pathophysiologic mechanisms and co-morbidities overlap between OSA and asthma, but the exact link has yet to be confirmed. Screening for OSA is recommended in those with severe asthma. Further investigations are needed to delineate the cellular processes with therapeutic targets. Similarly, prospective investigations are needed to evaluate the longitudinal relationship in pre-existing asthma and the development of OSA.
Similar content being viewed by others
Introduction
Over the last decade, there has been increasing interest in the relationship between asthma and obstructive sleep apnea (OSA). Both asthma and OSA are highly prevalent airway disorders with significant impact on the healthcare system [1, 2]. Evidence supports a bidirectional association where each disorder adversely affects the other and both disorders independently impair sleep quality resulting in poor daytime functioning and decreased quality of life [3•, 4,5,6]. Importantly, the co-existence of OSA in asthmatics has been associated with worse asthma control and more severe exacerbations. OSA not only relates to asthma symptoms but also affects persistent daytime asthma control [5, 7,8,9]. In 2013, the co-existence of asthma with OSA was coined as the “alternative overlap syndrome” [10].
Asthma is a heterogenous disease that affects approximately 6.3% of men and 9% of females in the USA and is characterized by chronic airway inflammation resulting in wheezing, shortness of breath, chest tightness, and/or cough with variable expiratory airflow limitation [1, 11]. A significant number of patients have nocturnal asthma with symptoms occurring only during sleep. Both uncontrolled asthma and nocturnal asthma have a deleterious effect on sleep quality [6].
Obstructive sleep apnea is underdiagnosed with approximately 13% of men and 6% of women in the USA estimated to have moderate to severe disease [2, 13••]. OSA causes fragmented sleep, fatigue, and excessive daytime sleepiness due to recurrent episodes of complete or partial upper airway obstruction during sleep resulting in impaired gas exchange, sympathetic overactivity, intrathoracic pressure changes, and gasping and choking [13••].
Studies have consistently demonstrated that asthmatics have an increased risk of OSA with prevalence rates as high as 70%, particularly in those with severe asthma [3•, 4]. Although most investigations have focused on the prevalence of OSA in the asthma population, the reverse relationship has also been demonstrated [14].
Additionally, asthma and OSA share similar underlying pathophysiology with increased airway resistance involving local and systemic inflammation and co-morbidities, such as gastro-esophageal reflex (GER), obesity, and rhinitis [15, 16, 17]. Important to asthma and OSA therapy is identification of risk factors, co-morbidities, and modifiable factors [15]. Furthermore, long-term use of continuous positive airway pressure (CPAP) has been reported to significantly alleviate asthma symptoms in patients with co-existing asthma and OSA [16, 17].
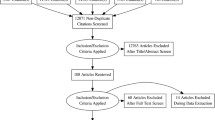
We will review the current data regarding the impact of asthma and OSA on clinical outcomes, potential pathophysiologic links between asthma and OSA, along with therapeutic information and address the role of screening (Fig. 1).
Pathophysiologic links between asthma and OSA. Modified from Davies SE 2019 Reference 14. Used with permission from Taylor and Francis
The Co-existence of Asthma and OSA: Epidemiology
OSA is typically thought to occur in obese individuals. However, like asthma, OSA also has different phenotypes largely based on craniofacial morphology. Common risk factors for OSA include male gender, age, obesity, family history, increase in neck size (> 17 inches in males and 16 inches in females), craniofacial abnormalities (i.e., micrognathia or retrognathia), and hypertension. Recently, it has been suggested that the co-existence of asthma with OSA may be a separate phenotype of asthma [12, 18]
Cross-sectional studies describe an increased prevalence of OSA in asthmatics ranging from 19 to 60% [18,19,20,21,22]. In severe and difficult-to-treat asthma populations, co-existence of OSA has been reported at high rates from 50 to 95% [18]. This wide variation in prevalence rates may be due to the difference in methodology used for diagnosing OSA and asthma. Several studies used symptom-based questions where others employed well-validated questionnaires, such as the Berlin questionnaire [20, 21]. Others used limited polysomnography or home-based studies with few studies employing the gold standard overnight-attended polysomnography [14, 22]. Additionally, a variation of methods was also used for diagnosing asthma. Most studies used questionnaires related to asthma symptoms and medications or a reported physician-based diagnosis [3, 14, 22]. Only a few studies used spirometry to determine diagnosis [21,22,23].
Despite the difference in methodology, it is difficult to ignore such results. In a large population-based study with over 38,000 newly diagnosed asthma patients evaluated over a 10-year period, the overall incidence of OSA was 2.51-fold higher in asthmatics than in non-asthmatics (12.1 vs. 4.84, respectively) [22]. Additionally, the adjusted hazard ratio (HR) for OSA was 1.78 in the asthma patients who had one or less annual emergency room (ER) visits compared to non-asthmatics. However, the risk for OSA substantially increased (HR of 23.8) for those asthmatics who had > 1 ER visit/year. This study supports that asthmatic patients have a greater risk for OSA and the risk seems to be inversely related to asthma control [22]. The risk of OSA has also shown to be positively correlated with the dose of inhaled and oral steroids [22, 23].
This is further supported by the landmark prospective longitudinal Wisconsin Sleep Cohort Study where individuals with asthma were shown to have an increased incidence of new onset OSA [3•]. Over 1000 subjects have been followed since 1988 with PSG performed every 4 years. Eligible participants were identified as free of OSA (AHI < 5 events/hr and never treated) by 2 baseline PSG studies. At the very first 4-year follow-up, 27% of those with asthma developed sleep apnea compared to 16% of the non-asthmatic subjects. Over the full study period after correcting for confounders and covariates, asthma patients faced an almost 40% greater risk for sleep apnea than asthma-free participants. Furthermore, the longer an individual had asthma, the greater their increased risk for developing OSA [3•].
Most investigations have focused on prevalence of OSA in the asthma population; the reverse relationship has also been demonstrated. Alharbi et al. investigated 616 patients with pre-existing OSA demonstrated by polysomnography and found that asthma was present in 35.1% [14••]. This illustrates the need for further prospective investigations to evaluate the subsequent development of asthma in individuals with OSA.
Co-morbidities Associated with the Alternative Overlap Syndrome
Rhinitis, obesity, and gastro-esophageal reflux (GER) are shared co-morbidities in developing asthma and OSA. These conditions have both direct and indirect effects on the pathophysiology between asthma and OSA.
Rhinitis
Asthmatics have higher rates of allergic and non-allergic rhinitis, as well as nasal polyposis [24]. Rhinitis causes chronic inflammation and nasal obstruction which results in higher negative oropharyngeal pressure during inspiration and predisposes to airway collapse and symptoms of OSA with snoring and apneic episodes [25]. Additionally, cortisol’s normal circadian regulation results in a nocturnal dip that leads to increased nasal resistance and inflammatory mediators perpetuating nocturnal asthma symptoms, nasal congestion/rhinitis, and OSA symptoms [26, 27]
Gastro-esophageal Reflux
GER is a common disorder and is self-reported in approximately 58–65% of individuals with OSA and up to 80% of asthmatics, independent of other confounders [15, 28]. Increased snoring and excessive daytime sleepiness have been reported in subjects with nocturnal GER as compared to those without nocturnal GER suggesting that GER may be an independent risk factor for development of OSA [28]. Persistent GER can cause direct injury to the upper airway resulting in inflammation and edema, which can precipitate nocturnal arousals and sleep fragmentation, snoring, and choking episodes [29].
OSA reciprocally promotes GER via increased negative intrathoracic pressure during inspiration causing reflux of gastric contents. Micro-aspiration directly injures the airway mucosa causing inflammation and reflex-mediated vagal-induced bronchoconstriction. Hence, OSA-induced acid reflux may play a role in triggering asthma symptoms [30].
However, it is not completely clear why asthmatics without co-existing OSA still have a higher prevalence of GER. One postulation is the change in intrathoracic pressure much like that in OSA creates retrograde movement of gastric contents. Additionally, medications used in treating asthma, such as beta-agonist, reduce lower esophageal sphincter tone and promote GER [15, 31]
Obesity
Obesity is a well-known risk factor for developing OSA but is also an independent risk factor for asthma [31, 32]. In a 4-year longitudinal study, a 10% increase in body weight predicated a 32% increase in AHI and a 6-fold increase in the odds of developing moderate to severe OSA (AHI > 15). Importantly, a weight loss of 10% predicted a 26% reduction in AHI, indicating that weight management is important in treatment of OSA [33]. Obesity is a complex entity that impairs breathing by altering mechanical and physiologic processes. Fat deposition causes narrowing of the upper airway, increased airway resistance, and collapsibility. In addition, excessive adipose tissue surrounding the chest and abdomen creates a restrictive process where functional residual capacity (FRC) is reduced, ventilatory drive is impaired, and oxygen demand and work of breathing are increased. Because FRC is decreased, exhalation must occur at a lower lung volume further compromising expiratory air flow rates and increasing airway obstruction [34, 35].
Obesity is also independent predictor of asthma even after adjusting for demographics, smoking status, oral corticosteroid use, and GER and is associated with poorer outcomes [36]. Whereas OSA is more common in obese men than obese women, the opposite occurs in obesity-related asthma: asthma is twice as likely to develop in obese women than in obese men suggesting a potential hormonal influence [37]. Obese asthmatics present a specific phenotype with more frequent or more severe asthma exacerbations, difficult-to-control symptoms with less eosinophilic inflammation, and relative resistance to glucocorticoids [36]. An improvement in asthma symptoms and reduction in medication requirements have been observed after weight loss in the obese asthmatics [7].
Pathophysiologic Links
In addition to the shared risk factors and co-morbidities associated with OSA and asthma, there are various intrinsic mechanisms that each disorder may contribute to the development of the other. These mechanisms include neuro-mechanical, hypoxia, cardiovascular, sleep fragmentation, and chronic inflammation.
Neuro-mechanical
OSA and asthma alter mechanical properties of the airway. Intermittent collapse of the upper airway associated with OSA leads to increased airway resistance caused from direct mechanical trauma due to vibratory damage from snoring. Additionally, inhalation against a closed glottis (Muller maneuver) causes increased intrathoracic pressure triggering a vagal reflex that stimulates the muscarinic receptors in the central airways potentiating bronchoconstriction [38].
Reciprocally, mechanical consequences of asthma can contribute to the development of OSA. Asthmatic patients have hyperinflation resulting in an increased functional residual capacity (FRC) compared to healthy controls. During sleep, FRC normally decreases, but asthmatics have a much greater FRC reduction, which may contribute to airway resistance and precipitate nocturnal symptoms of snoring, gasping, and choking [38]. The abrupt decline in lung volume also causes a decrease in tracheal tug resulting in altered pharyngeal airway stiffness further impacting resistance [39].
Corticosteroids used to treat asthma may further impair upper airway diameter due to excessive intrapharyngeal fat deposition. Prolonged oral corticosteroids used in treating severe asthmatics may also induce a muscle myopathy and decrease contractile properties of the pharyngeal dilator muscles making the airway more “floppy”, prone to collapse, and increase the risk for obstruction during sleep [23, 40].
Hypoxia
Hypoxia associated with airway obstruction results in increased sympathetic discharge causing vasoconstriction, deoxygenation-reoxygenation (redox) injury, platelet activation, inflammation, and ultimately endothelial dysfunction. Intermittent hypoxia also stimulates the carotid body receptors and may create a reflex bronchoconstriction and precipitate nocturnal asthma symptoms [41].
The increased sympathetic tone from hypoxia and negative intrathoracic pressure associated with intermittent airway obstruction leads to increased afterload of left ventricular causing or worsening heart failure. Congestive heart failure itself has been known to worsen the asthma symptoms by inducing airway hyper-responsiveness [41].
Additionally, vascular endothelial growth factors (VEGF) may play a role in the pathogenesis of both asthma and OSA [41, 42]. VEGF is a hypoxia-sensitive glycoprotein, and both OSA and asthma can promote its expression. VEGF contributes to bronchial inflammation, hyper-responsiveness, and vascular remodeling. Studies indicate that the concentration of VEGF correlates with the severity of obstructive events in OSA and the degree of hypoxia but also with the severity of airway obstruction in asthmatics [42].
Sleep Fragmentation
The hallmark of OSA is intermittent upper airway obstruction leading to hypoxia and central nervous system (CNS) activation causing sleep fragmentation with cortical arousals and awakenings with daytime sleepiness. Disturbance in the sleep architecture itself may contribute to the bidirectional interactions of OSA and asthma. Frequent persistent obstruction can result in blunting of the arousal response to hypoxia, as well as to bronchoconstriction. Asthmatics are reported to have more frequent sleep disruption with more irregular breathing, hypopneas, and snoring, particularly during REM sleep, than those without asthma [43]. This may be related to the increased cholinergic activity that occurs during REM sleep, which in turn modulates airway caliber and reactivity via the muscarinic receptors.
Inflammation
OSA is becoming more commonly thought of as a chronic inflammatory disease by inducing both airway and systemic inflammation via repeated upper airway mechanical stress. The repetitive partial or complete upper airway collapse leads to hypoxia and oxidative stress not just locally but systemically, with increased serum cytokines, including C-reactive protein (CRP), tumor necrosis factor (TNF-α), and interleukin-6 (IL-6) [44]. Repeated snoring has been shown to cause edema and damage to the soft tissue resulting in direct mechanical trauma and airway inflammation [44, 45]. Biopsies from nasal and tonsillar tissue have shown increased polymorphonuclear cells (PMN’s), bradykinin, vasoactive intestinal peptide (VIP), and increased leukotriene receptors (LTR-1 and 2). These are known mediators of inflammation, bronchoconstriction, microvascular permeability, and eosinophilic recruitment and may cause similar changes in central airways precipitating bronchoconstriction that may impact or promote asthma [46].
Studies have demonstrated significantly higher neutrophil percentage, independent of other cofounders, in patients with high OSA risk as compared to those without OSA, whereas sputum eosinophil percentages were similar [47]. Similar results were observed in another study where patients with OSA and severe asthma showed airway inflammation and remodeling with a higher proportion of neutrophils and lower proportion of macrophages, elevated interleukin-8 (IL-8), and matrix metalloproteinase 9 (MMP-9) in sputum and thinner bronchial basement membrane, compared to non-OSA patients with severe asthma. The thickness of the bronchial basement membrane was negatively associated with the severity of sleep apnea [7, 47]. This supports that OSA may be an important contributor to neutrophilic asthma and may contribute to airway remodeling eventually leading to difficult-to-treat asthma. However, further studies are necessary to confirm those findings and better understand the mechanisms.
Inflammatory changes associated with asthma may reciprocally promote upper airway obstruction. Chronic coughing leads to persistent inflammation causing thickening of the upper airways. Radiographic studies have demonstrated decreased pharyngeal cross-sectional area in asthmatics during bronchoprovocation [48]. This creates upper airway resistance and high negative pressure on inspiration thus increasing the risk of upper airway collapse [38].
Furthermore, leptin may be a linking component between asthma and OSA. Leptin is a protein hormone produced by adipose tissue that circulates systemically and acts on the hypothalamus to induce satiety and increase metabolism. However, leptin is also proinflammatory and stimulates the release of IL-6 and TNF-a by adipocytes, as well monocytes and macrophages to express cytokines, and increases T cell proliferation [41, 49]. Obesity is known to induce a chronic low-grade state of inflammation by directly releasing pro-inflammatory mediators, such as leptin, resistin, and other adipokines. This triggers systemic inflammation, as well as airway inflammation independently of the inflammation associated with asthma. However, patients with OSA have also been shown to have increased levels of serum leptin compared with non-apneic patients irrelevant to obesity [41]. Furthermore, leptin has been shown to be increased in asthmatic patients compared with non-asthmatics even after controlling for obesity and may also contribute to airway hyper-responsiveness [41, 49].
This supports that increased levels of serum leptin observed in both OSA and asthma independently of obesity suggest leptin may play a pivotal role in the pathogenesis of these respiratory disorders. Obesity further compounds the severity of inflammation and adversely impacts both OSA and asthma [50].
Clinical Outcome of Asthma-OSA Overlap
Not only does OSA seem to be associated with development of nocturnal asthma, it is also associated with persistent daytime asthma symptoms, particularly in those with severe and difficult-to-treat asthma. Thus, unrecognized OSA may be the cause of persistent daytime and nocturnal asthma [8].
There is still little evidence on the impact of OSA on asthmatic patients’ pulmonary function. Based on a 15-year follow-up study of ventilatory function in asthmatic patients, the unadjusted decline in forced expiratory volume in one second (FEV1) was 38 ml/year [51]. There are several factors identified for the decline of FEV1 in asthma, including age, sex, asthma exacerbation, smoking status, obesity, and hypoxia [52]. In a recent retrospective study, asthmatic patients with OSA were followed for more than 5 years with spirometry and showed a greater decline in FEV1 compared to those without OSA [53•]. In this study, the decline of FEV1 among asthmatic patients with severe OSA was 72.4 ml/year compared to 41.9 ml/year in those with mild to moderate OSA and 24.3 ml/year in those without OSA. After adjusting for confounder, OSA severity was the only independent factor affecting pulmonary function decline [53•]. However, in another recent meta-analysis, no significant difference of FEV1 was seen between asthmatic patients with and without OSA [54]. Larger prospective studies are needed to verify long-term effects on pulmonary function.
Sleep quality is known to be poor in individuals with OSA and in asthmatics. A recent evaluated sleep architecture in adult women showed that both asthma and OSA subjects have more light sleep and less time in REM sleep compared to either condition alone. In those with both asthma and OSA, mean oxygen saturation was lower than those with only OSA. The results were consistent even after adjustment of age, BMI, and smoking status. The authors concluded that the combination of OSA and asthma is associated with poorer sleep quality with more profound hypoxemia than with either condition alone [21]. Similar results have been described difficult-to-treat asthmatics with longer periods of oxygen saturations remaining <90% [55].
Mortality associated with OSA in asthmatics has been poorly investigated. To our awareness, the literature is limited to an isolated study that investigated the risk of mortality in asthmatics with various sleep disorders. Asthmatic patients with sleep disorders had increased risk of death compared to those asthma patients alone even with adjusting for possible confounders (HR 1.451, 95% confidence interval: 1.253–1.681) [56]. Although this study is limited by inclusion of many types of sleep disorders, it suggests that sleep fragmentation may negatively impact outcomes in asthma.
Therapeutic Implications
Early studies which evaluated the effect of CPAP on asthma were limited by small sample size and short follow-up period. A large survey study was conducted in a group of patients with OSA and asthma to investigate the effect of long-term use of CPAP on control of asthma symptoms [57]. Thirteen percent of CPAP users had co-existing asthma and used CPAP for over 5 years with a daily duration of 6.3 h. Self-reported asthma severity decreased significantly, and the asthma control test score improved despite no significant change in body mass index. The percentage of patients using daily rescue medication also decreased from 36 to 8% with CPAP usage (p < 0.001) [57]. In another prospective, multicenter study, asthma outcomes were examined after 6 months of CPAP use in 99 adult asthma patients with OSA [16]. The study assessed asthma control and quality of life using the Asthma Control Questionnaire (ACQ) and mini asthma quality of life questionnaire (MiniAQLQ), respectively. Both disease control and quality of life significantly improved. But when diseases were stratified according to severity, only patients with moderate-severe asthma and severe OSA who used CPAP > 4 h/day showed significance in improvement. Asthma exacerbations also decreased from 35.4 to 17.2%. Bronchial reversibility, gastro-esophageal reflux, rhinitis, and exhaled nitric oxide levels all significantly improved. All changes occurred without significant asthma drug therapy modification, change in body weight, and other asthma comorbidities [16].
Data is conflicting regarding the effect of CPAP treatment on FEV1 decline in asthmatic patients. A retrospective study in asthmatics with severe OSA demonstrated a positive effect, however this was not confirmed in other studies [16, 17, 53•]. Additionally, a single study reported a decrease in airway reactivity with even a short 7-day nocturnal CPAP [58]. Randomized trials are needed to scientifically investigate the effect of PAP therapy on pulmonary function and airway responsiveness to medication management.
Equally important is treatment of the underlying risk factors, namely, allergic rhinitis, obesity, and GER [28]. A meta-analysis showed significant improvement in OSA among those that received intranasal corticosteroid therapy [59, 60]. Obesity is a well-recognized risk factor for asthma and OSA, and their interplay has been recognized in an outpatient setting [50]. Bariatric surgery is known to improve OSA, as well as asthma control and pulmonary function [61, 62].
Role of Screening
Given the high prevalence and the adverse effect of OSA and asthma on each other, it is important to consider screening for OSA in asthma patients. A recent study in China evaluated the predictive performance of the two most common OSA screening questionnaires, the Berlin questionnaire (BQ) and STOP-BANG questionnaire (SBQ) in asthmatic patients. In comparison with BQ, SBQ was easier and demonstrated higher diagnostic sensitivity (84.4% vs 60%), lower specificity (79.5% vs 91%), lower positive predictive value (70.4% vs 79.4%), and higher negative predictive value (90% vs 80%), in detecting moderate-to-severe OSA with an AHI > 15. The SBQ seems to be the preferable sleep questionnaire over BQ in the detection of moderate and severe OSA but needs to be further validated with a larger asthma population [18, 63].
Conclusion
The co-existence of OSA in asthma patients is significantly associated with duration, severity, and control of asthma with increased daytime and nocturnal symptoms, worsening nocturnal hypoxemia, and sleep quality, leading to increased asthma exacerbations and hospitalizations. Although most studies have demonstrated that OSA impacts asthma, data has also shown that asthma may be a risk factor for new onset OSA. Pathophysiologic mechanisms and co-morbidities overlap between OSA and asthma, but a causal relationship has yet to be confirmed. Further investigations are needed to delineate cellular processes with therapeutic targets, as well as to validate the effect of current therapies, such as CPAP on pulmonary function. Additionally, given the high prevalence of OSA in asthmatics and significant adverse impact, screening for OSA should be considered.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Center for Disease Control and Prevention. Asthma. Most recent Data. CDC 2019 [updated 2019 March; cited 2020 January 2]. Available from: https://www.cdc.gov/asthma/most_recent_data.htm
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM. Increased prevalence of sleep-disordered breathing in adults. American Journal of Epidemiology. 2013;177(9):1006–14. https://doi.org/10.1093/aje/kws342.
• Teodorescu M, Barnet J, Hagen E, Palta M, Young T, Peppard P. Association between asthma and risk of developing obstructive sleep apnea. JAMA. 2015;313(2):156–64. https://doi.org/10.1001/jama.2014.17822Longitudinal study that supports the development of new onset OSA in asthmatics.
Julien JY, Martin JG, Ernst P, Olivenstein R, Hamid Q, Lemiere C, et al. Prevalence of obstructive sleep apnea-hypopnea in severe versus moderate asthma. The Journal of Allergy and Clinical Immunology. 2009;124:371–6. https://doi.org/10.1016/j.jaci.2009.05.016.
Teodorescu M, Polomis D, Gangnon RE, Peterson AG, Consens FB, et al. Association of obstructive sleep apnea risk or diagnosis with daytime asthma in adults. J Asthma. 2012;49(6):620–8. https://doi.org/10.3109/02770903.2012.689408.
Luyster FS, Teodorescu M, Bleecker E, Busse W, Calhoun W, Castro M, et al. Sleep quality and asthma control and quality of life in non-severe and severe asthma. Sleep Breath. 2012;16:1129–37. https://doi.org/10.1007/s11325-011-0616-8.
Teodorescu M, Polomis DA, Hall SV, Teodorescu MC, Gangnon RE, Peterson AG, et al. Association of obstructive sleep apnea risk with asthma control in adults. Chest. 2010;138:543–50. https://doi.org/10.1378/chest.09-3066.
Wang Y, Liu K, Hu K, Yang J, Li Z, Nie M, et al. Impact of obstructive sleep apnea on severe asthma exacerbations. Sleep Medicine. 2016;26:1–5. https://doi.org/10.1016/j.sleep.2016.06.013.
Zidan M, Daabis R, Gharraf H. Overlap of obstructive sleep apnea and bronchial asthma: Effect on asthma control. Egypt J Chest Dis Tuberc. 2015;64(2):425–30. https://doi.org/10.1016/j.ejcdt.2015.01.007.
Ioachimescu OC, Teodorescu M. Integrating the overlap of obstructive lung disease and obstructive sleep apnoea. OLDOSA syndrome. Respirology. 2013;18:421–31. https://doi.org/10.1111/resp.12062.
Global Initiative for Asthma. Asthma management and prevention for adults and children older than 5 years. GINA; 2019. [updated 2019 March; cited 2020 January 5]. Available from: https://ginasthma.org/wp-content/uploads/2019/04/GINA-2019-main-Pocket-Guide-wms.pdf
American Academy of Sleep Medicine. International classification of sleep disorders, 3rd ed. Darien, IL: American Academy of Sleep Medicine, 2014.
•• Alharbi M, Almutairi A, Alotaibi D, et al. The prevalence of asthma in patients with obstructive sleep apnoea. Prim Care Respir J. 2009;18:328–30. https://doi.org/10.4104/pcrj.2009.00020Novel study which demonstrates new onset asthma in individuals with pre-existing OSA.
Davis S, Bishopp A, Wharton S, Turner A, Mansur A. The association between asthma and obstructive sleep apnea (OSA): systemic review. Journal of Asthma. 2019;56(2):118–29. https://doi.org/10.1080/02770903.2018.1444049.
Serrano-Pariente J, Plaza V, Soriano JB, Mayos M, López-Viña A, Picado C, et al. CPASMA Trial Group. Asthma outcomes improve with continuous positive airway pressure for obstructive sleep apnea. Allergy. 2017;72:802–12. https://doi.org/10.1111/all.13070.
Lafond C, Sériès F, Lemière C. Impact of CPAP on asthmatic patients with obstructive sleep apnoea. Eur. Respir. J. 2007;29:307–11. https://doi.org/10.1183/09031936.00059706.
Franklin KA, Lindberg E. Obstructive sleep apnea is a common disorder in the population-a review on the epidemiology of sleep apnea. Journal of Thoracic Disease. 2015;7(8):1311–22. https://doi.org/10.3978/j.issn.2072-1439.2015.06.11.
Damianaki A, Vagiakis E, Sigala I, et al. The co-existence of obstructive sleep apnea and bronchial asthma: revelation of a new asthma phenotype? J Clin Med. 2019;8(9):1476. https://doi.org/10.3390/jcm8091476.
Teodorescu M, Consens FB, Bria WF, Coffey MJ, McMorris MS, Weatherwax KJ, et al. Correlates of daytime sleepiness in patients with asthma. Sleep Med. 2006;7:607–13. https://doi.org/10.1016/j.sleep.2006.02.001.
Kim MY, Jo EJ, Kang SY, et al. Obstructive sleep apnea is associated with reduced quality of life in adult patients with asthma. Ann Allergy Asthma Immunol. 2013;110:253–7. https://doi.org/10.1016/j.anai.2013.01.005.
Sundbom F, Janson C, Malinovschi A, Lindberg E. Effects of co-existing asthma and obstructive sleep apnea on sleep architecture, oxygen saturation, and systemic inflammation in women. J. Clin. Sleep Med. 2018;14:253–9. https://doi.org/10.5664/jcsm.6946.
Shen TC, Lin CL, Wei CC, Chen CH, Tu CY, Hsia TC, et al. Risk of obstructive sleep apnea in adult patients with asthma: a population-based cohort study in Taiwan. PLoS ONE. 2015;10:e0128461. https://doi.org/10.1371/journal.pone.0128461.
Teodorescu M, Xie A, Sorkness CA, Robbins JA, Reeder S, Gong Y, et al. Effects of inhaled fluticasone on upper airway during sleep and wakefulness in asthma: a pilot study. J Clin Sleep Med. 2014;10(2):183–93. https://doi.org/10.5664/jcsm.3450.
Togias A. Rhinitis and asthma: evidence for respiratory system integration. The Journal of Allergy and Clinical Immunology. 2003;111(6):1171–83. https://doi.org/10.1067/mai.2003.1592.
Kalpaklıoglu AF, Kavut AB, Mehmet E. Allergic and nonallergic rhinitis: the threat for obstructive sleep apnea. Ann Allergy, Asthma Immunol. 2009;103:20–5. https://doi.org/10.1016/S1081-1206(10)60138-X.
Martin R, S. B-S. Chronobiology of asthma. Am J Respir Crit Care Med. 1998;158:1002–7. https://doi.org/10.1164/ajrccm.158.3.9712132.
Koinis-Mitchell D, Craig T, Esteban CA, Klein RB. Sleep and allergic disease: a summary of the literature and future directions for research. The Journal of Allergy and Clinical Immunology. 2012;130:1275–128. https://doi.org/10.1016/j.jaci.2012.06.026.
Harding SM. Gastroesophageal reflux: a potential asthma trigger. Immunol Allergy Clin North Am. 2005;25(1):131–48. https://doi.org/10.1016/j.iac.2004.09.006.
Emilsson OI, Bengtsson A, Franklin KA, Torén K, Benediktsdóttir B, Farkhooy A, et al. Nocturnal gastro-oesophageal reflux, asthma and symptoms of OSA: a longitudinal, general population study. The European Respiratory Journal. 2013;41:1347–54. https://doi.org/10.1183/09031936.00052512.
Kasasbeh A, Kasasbeh E, Krishnaswamy G. Potential mechanisms connecting asthma, esophageal reflux, and obesity/sleep apnea complex--a hypothetical review. Sleep Medicine Reviews. 2007;11:47–58. https://doi.org/10.1016/j.smrv.2006.05.001.
Young T, Skatrud J, Peppard PE. Risk factors for obstructive sleep apnea in adults. JAMA. 2004;291:2013–6. https://doi.org/10.1001/jama.291.16.2013.
Beuther DA, Sutherland ER. Overweight, obesity, and incident asthma: a meta-analysis of prospective epidemiologic studies. AJRCCM. 2007;175:661–6. https://doi.org/10.1164/rccm.200611-1717OC.
Peppard PE, Young T, Palta M, Dempsey J, Skatrud J. Longitudinal study of moderate weight change and sleep-disordered breathing. JAMA. 2000;284(23):3015–21. https://doi.org/10.1001/jama.284.23.3015.
Isono S. Obesity and obstructive sleep apnea: mechanisms for increased collapsibility of the passive pharyngeal airway. Respirology. 2012;17:32–42. https://doi.org/10.1111/j.1440-1843.2011.02093.x.
Salome CM, King GG, Berend N. Physiology of obesity and effects on lung function. J Appl Physiol. 2010;108(1):206–11. https://doi.org/10.1152/japplphysiol.00694.2009.
Ali Z, Ulrik CS. Obesity and asthma: a coincidence or a causal relationship? A systematic review. Respiratory Medicine. 2013;107(9):128–300. https://doi.org/10.1016/j.rmed.2013.03.019.
Chen Y, Dales R, Tang M, Krewski D. Obesity may increase the incidence of asthma in women but not in men: longitudinal observations from the Canadian National Population Health Surveys. Am J Epidemiol. 2002;155:191–7. https://doi.org/10.1093/aje/155.3.191.
Ballard RD, Irvin CG, Martin RJ, Pak J, Pandey R, White DP. Influence of sleep on lung volume in asthmatic patients and normal subjects. J Appl Physiol. 1990;68:2034–41. https://doi.org/10.1152/jappl.1990.68.5.2034.
Van de Graaff WB. Thoracic influence on upper airway patency. J Appl Physiol. 1988;65:2124–31. https://doi.org/10.1152/jappl.1988.65.5.2124.
Yigla M, Tov N, Solomonov A, Rubin AHE, Harlev D. Difficult-to-control asthma and obstructive sleep apnea. J Asthma. 2003;40:865–71. https://doi.org/10.1081/jas-120023577.
Alkhalil M, Schulman E, Getsy J. Obstructive sleep apnea syndrome and asthma: what are the links? Journal of Clinical Sleep Medicine. 2009;5(1):71–8. https://doi.org/10.5664/jcsm.27397.
Schulz R, Hummel C, Heinemann S, et al. Serum levels of vascular endothelial growth factor are elevated in patients with obstructive sleep apnea and severe nighttime hypoxia. AJRCCM. 2002;165:67–70. https://doi.org/10.1164/ajrccm.165.1.2101062.
Khatri SB, Ioachimescu OC. The intersection of obstructive lung disease and sleep apnea. Cleveland Clinic Journal of Medicine. 2016;83(2):127–40. https://doi.org/10.3949/ccjm.83a.14104.
Salerno FG, Carpagnano E, Guido P, Bonsignore MR, Roberti A, Aliani M, et al. Airway inflammation in patients affected by obstructive sleep apnea syndrome. Respir Med. 2004;98:25–8. https://doi.org/10.1016/j.rmed.2003.08.003.
Hatipoglu U, Rubinstein I. Inflammation and obstructive sleep apnea syndrome: how many ways do I look at thee? Chest. 2004;126(1):1–2. https://doi.org/10.1378/chest.126.1.1.
Goldbart AD, Goldman JL, Li RC, Brittian KR, Tauman R, Gozal D. Differential expression of cysteinyl leukotriene receptors 1 and 2 in tonsils of children with obstructive sleep apnea syndrome or recurrent infection. Chest. 2004;126:13–8. https://doi.org/10.1378/chest.126.1.13.
Taillé C, Rouve-Tallec A, Stoica TM, et al. Obstructive sleep apnoea modulates airway inflammation and remodelling in severe asthma. PLoS ONE. 2016;11(3):e0150042. https://doi.org/10.1371/journal.pone.0150042.
Collett PW, Brancatisano AP, Engel LA. Upper airway dimensions and movements in bronchial asthma. Am Rev Respir Dis. 1986;133:1143–9. https://doi.org/10.1164/arrd.1986.133.6.1143.
Sideleva O, Suratt BT, Black KE, Tharp WG, Pratley RE, Forgione P, et al. Obesity and asthma: an inflammatory disease of adipose tissue not the airway. AJRCCM. 2012;186(7):598–605. https://doi.org/10.1164/rccm.201203-0573OC.
Jubber AS. Respiratory complications of obesity. Int J Clin Pract. 2004;58(6):573–80. https://doi.org/10.1111/j.1368-5031.2004.00166.x.
Lange P, Parner J, Vestbo J, Schnohr P, Jensen G. A 15-year follow-up study of ventilatory function in adults with asthma. NEJM. 1998;339(17):1194–200. https://doi.org/10.1056/NEJM199810223391703.
Dijkstra A, Vonk JM, Jongepier H, Koppelman GH, Schouten JP, ten Hacken N, et al. Lung function decline in asthma: Association with inhaled corticosteroids, smoking and sex. Thorax. 2006;61:105–10. https://doi.org/10.1136/thx.2004.039271.
• Wang TY, Lo YL, Lin SM, et al. Obstructive sleep apnoea accelerates FEV1 decline in asthmatic patients. BMC Pulm Med. 2017;17:1–6. https://doi.org/10.1186/s12890-017-0398-2Study shows the accelerated decrease in lung function of those with overlapping disease.
Kong D, Qin Z, Shen H, et al. Association of obstructive sleep apnea with asthma: A meta-analysis. Sci Rep. 2017;7:4088–9. https://doi.org/10.1038/s41598-017-04446-6.
Shaker A. Study of obstructive sleep apnea (OSA) in asthmatics. Egypt J Chest Dis Tuberc. 2017;66:293–8. https://doi.org/10.1016/j.ejcdt.2017.04.002.
Han KT, Bae HC, Lee SG, Kim SJ, Kim W, Lee HJ, et al. Are sleep disorders associated with increased mortality in asthma patients? BMC Pulm. Med. 2016;16:154–9. https://doi.org/10.1186/s12890-016-0313-2.
Kauppi P, Bachour P, Maasilta P, Bachour A. Long-term CPAP treatment improves asthma control in patients with asthma and obstructive sleep apnoea. Sleep Breath. 2016;20:1217–24. https://doi.org/10.1007/s11325-016-1340-1.
Busk M, Busk N, Puntenney P, Hutchins J, Yu Z, Gunst SJ, et al. Use of continuous positive airway pressure reduces airway reactivity in adults with asthma. Eur Respir J. 2013;41:317–22. https://doi.org/10.1183/09031936.00059712.
Kim SH, Won HK, Moon SD, Kim BK, Chang YS, Kim KW, et al. Impact of self-reported symptoms of allergic rhinitis and asthma on sleep disordered breathing and sleep disturbances in the elderly with polysomnography study. PLoS ONE. 2017;12(2):e0173075. https://doi.org/10.1371/journal.pone.0173075.
Liu HT, Lin YC, Kuan Y, et al. Intranasal corticosteroid therapy in the treatment of obstructive sleep apnea: a meta-analysis of randomized controlled trials. Am. J. Rhinol Allergy. 2016;30:215–21. https://doi.org/10.2500/ajra.2016.30.4305.
Aguiar IC, Freitas WR, Santos IR, Apostolico N, Nacif SR, Urbano J, et al. Obstructive sleep apnea and pulmonary function in patients with severe obesity before and after bariatric surgery: a randomized clinical trial. Multidiscip Respir Med. 2014;9:43. https://doi.org/10.1186/2049-6958-9-43.
Dixon AE, Pratley RE, Forgione PM, Kaminsky DA, Whittaker-Leclair LA, Griffes LA, et al. Effects of obesity and bariatric surgery on airway hyperresponsiveness, asthma control and inflammation. J Allergy Clin Immunol. 2011;128:508–15. https://doi.org/10.1016/j.jaci.2011.06.009.
Lu H, Fu C, Li W, et al. Screening for obstructive sleep apnea syndrome in asthma patients: A prospective study based on berlin and STOP-Bang questionnaires. J Thorac Dis. 2017;9:1945–58. https://doi.org/10.21037/jtd.2017.06.03.
Author information
Authors and Affiliations
Contributions
DP and KH conducted literature review, synthesized the literature, and wrote the manuscript. JM edited and reviewed references.
Corresponding author
Ethics declarations
Conflict of Interest
Donna L. Pepito, Jamal M. Mohammed, and Kimberly A. Hardin declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on COPD and Asthma
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pepito, D.L., Mohammed, J.M. & Hardin, K.A. Obstructive Sleep Apnea and Asthma: More Than Chance?. Curr Pulmonol Rep 10, 84–91 (2021). https://doi.org/10.1007/s13665-021-00271-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13665-021-00271-5