Abstract
Introduction
IL-13 is the primary upregulated cytokine in atopic dermatitis (AD) skin and is the pathogenic mediator driving AD pathophysiology. Lebrikizumab, tralokinumab and cendakimab are therapeutic monoclonal antibodies (mAb) that target IL-13.
Methods
We undertook studies to compare in vitro binding affinities and cell-based functional activities of lebrikizumab, tralokinumab and cendakimab.
Results
Lebrikizumab bound IL-13 with higher affinity (as determined using surface plasma resonance) and slower off-rate. It was more potent in neutralizing IL-13-induced effects in STAT6 reporter and primary dermal fibroblast periostin secretion assays than either tralokinumab or cendakimab. Live imaging confocal microscopy was employed to determine the mAb effects on IL-13 internalization into cells via the decoy receptor IL-13Rα2, using A375 and HaCaT cells. The results showed that only the IL-13/lebrikizumab complex was internalized and co-localized with lysosomes, whereas IL-13/tralokinumab or IL-13/cendakimab complexes did not internalize.
Conclusion
Lebrikizumab is a potent, neutralizing high-affinity antibody with a slow disassociation rate from IL-13. Additionally, lebrikizumab does not interfere with IL-13 clearance. Lebrikizumab has a different mode of action to both tralokinumab and cendakimab, possibly contributing to the clinical efficacy observed by lebrikizumab in Ph2b/3 AD studies.
Similar content being viewed by others
Skin biopsies of patients with AD show an overexpression of IL-13 as compared to healthy individuals |
The objective of the study is to compare clinical IL-13 monoclonal antibodies’ binding affinities and cell-based functional activities |
The differences in molecular characteristics between these IL-13 therapies may help in the understanding of the differences seen in the clinical trial results, though head-to-head studies have not been conducted |
Lebrikizumab has a higher binding affinity and in vitro potency than other IL-13 therapies compared in the study |
Introduction
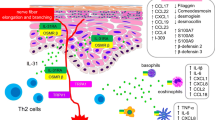
Atopic dermatitis (AD) is a complex disease that is determined by genetic, environmental and immunologic factors [1, 2]. Interleukin-13 (IL-13) is a central pathogenic inflammatory mediator of AD which drives effects such as a defective skin barrier, dermal inflammation, allergic response and lichenification [3,4,5]. IL-13 gene polymorphisms [4, 4,6,7,8] are associated with an increased risk for developing AD. IL-13 can reduce epithelial integrity through the downregulation of filaggrin, loricrin and involucrin [6, 9], increasing the risk of sensitization to environmental allergens. Additionally, IL-13 can act on keratinocytes to downregulate their differentiation [10, 11], decrease the production of antimicrobial peptides [12] and induce the production of T-cell chemoattractants that mediate T-cell infiltration into AD lesions [13]. IL-13-mediated tissue inflammation promotes fibrotic skin remodeling and skin thickening [14]. Finally, IL-13 may also sensitize peripheral sensory neurons that induce pruritus [15]. In skin biopsies of patients with AD, there is an overexpression of IL-13 in lesional and nonlesional skin compared to healthy individuals with the severity of AD being directly related to the IL-13 levels [16, 17]. At the lesional level, there is evidence of IL-13 overexpression with nearly undetectable expression of interleukin-4 (IL-4) suggesting that AD is an IL-13 dominant disease [7, 17, 18].
IL-13 is a cytokine secreted by T helper type 2 (Th2) cells and natural killer cells, as well as mast cells, basophils, eosinophils and innate lymphoid cell (ILC) type 2 cells [19]. The secondary structural features of IL-13 are like those of IL-4; however, IL-13 only has 25% sequence homology to IL-4 [20, 21]. The IL-13 receptor is a heterodimeric receptor complex consisting of IL-4 receptor α (IL-4Rα) and IL-13 receptor α1 (IL-13Rα1). Heterodimerization of the receptor complex activates STAT6 signaling, which is important in initiation of the type 1 allergic response [22]. IL-13 also binds to another receptor known as IL-13 receptor α 2 (IL-13Rα2). This receptor has no significant cytoplasmic domain, does not seem to function as a signal mediator and often is referred to as the decoy receptor [23, 24]. The expression of IL-13Rα2 can be induced by several pro-inflammatory cytokines, including IL-13 and IL-4, as well as tumor necrosis factor α (TNFα), suggesting this is a negative feedback mechanism [25, 26].
Lebrikizumab is a monoclonal immunoglobulin G4 antibody that specifically binds and neutralizes IL-13. Lebrikizumab has an affinity to human IL-13 that is < 10 pM with an epitope that allows IL-13 to bind to IL-13Rα1, but inhibits human IL-13 signaling through the IL-4Rα/IL-13Rα1 receptor complex [27]. Lebrikizumab is in phase 3 development for moderate-to-severe AD (NCT04146363 and NCT04178967). Tralokinumab and cendakimab are mAbs to IL-13 that prevent its binding to IL-13Rα1 [28, 29]. Tralokinumab has recently been approved for the treatment of moderate-to-severe AD in adults [30]. Cendakimab is in phase 2 development for moderate-to-severe AD (NCT04800315). Here, we describe results from studies aiming to compare the in vitro binding affinities and cell-based functional activities of lebrikizumab, tralokinumab and cendakimab. Additionally, we investigated whether IL-13 mAb binding interfered with IL-13 binding to IL-13Rα2 and its subsequent internalization.
The purpose of this study was to compare the in vitro binding affinities and cell-based functional activities of clinical IL-13 monoclonal antibodies, with the goal of aiding understanding of the differences seen in clinical trial results reported to date.
Methods
Expression and Purification of Recombinant IL-13 and IL-4
Mammalian expression plasmids encoding either His-tagged human IL-13 (P35225) or His-tagged human IL-4 (P24394) were generated. The vectors were transiently transfected into Human Embryonic Kidney 293 (HEK293) cells (ATCC, Manassas, VA, USA). IL-13 (N-1) His-tag was purified from the harvest media using Q Sepharose FF column in tandem with IMAC capture followed by HiLoad 26/600 Superdex 75 (Cytiva). IL-13 was expressed as glycosylated and aglycosylated species, which were separated on Superdex column. Purified glycosylated IL-13, aglycosylated IL-13 and IL-4 were evaluated for purity and identity using SDS-PAGE and analytical size-exclusion chromatography (aSEC) using TSKgel UP-SW3000 column (TOSOH and LC/MS analysis. Endotoxin was measured at < 1 EU/mg using Endosafe ® PTS (Charles River Laboratories).
Generation of Fluorophore-labeled Recombinant IL-13 and IL-4
To visualize cytokine binding, recombinant glycosylated IL-13 and IL-4 were labeled with Alexa Fluor (AF) 568 by site-selective click chemistry using 10 mol equivalents of AZDye 568 DBCO (Click Chemistry Tool, 1294–5). Free dye was separated from conjugated protein using HiLoad 26/600 Superdex 200 size-exclusion chromatography column (Cytiva, 28–9893-36). The activity of the fluorophore-conjugated protein (IL-13-AF568, IL-4-AF568) was confirmed in a HEK293 STAT6 reporter assay. AF568 labeling of IL-13 did not change the IL-13 activity, whereas AF568-labeled IL-4 had reduced bioactivity (Supplement Fig. 1). In subsequent experiments both IL-13 and IL-4 were used at 500 ng/ml, which is above saturating conditions.
Expression and Purification of mAbs
Mammalian expression vectors encoding the respective heavy chain (HC) and light chain (LC) genes of tralokinumab (CAS: 1044515–88-9) and cendakimab (CAS: 2151032–62-9) were generated and transiently transfected into Chinese Hamster Ovary cells (Lonza). The mAbs were purified from the harvest media using Protein-A affinity chromatography (Cytiva) followed by cation exchange chromatography (Thermo Fisher). Purified mAbs were buffer exchanged into phosphate-buffered saline (PBS), pH7.2, and evaluated for purity and identity using SDS-PAGE, aSEC and LC/MS analysis. Endotoxin was measured at < 1 EU/mg using Endosafe ® PTS (Charles River Laboratories). At the time of this study marketed tralokinumab and cendakimab were not available for purchase. Therefore, these mAbs were expressed and purified at Eli Lilly and Company. Lebrikizumab and IgG control antibody were expressed using Chinese Hamster Ovary cells and were also purified at Eli Lilly and Company.
Binding Kinetics and Affinity
The binding kinetics and affinity of lebrikizumab, tralokinumab and cendakimab to human IL-13 were determined using a Biacore T200 instrument primed with HBS-EP + , 0.05 mg/ml BSA (10 mM Hepes pH 7.4, 150 mM NaCl, 3 mM EDTA and 0.05% surfactant P20 (GE Healthcare Life Sciences, Marlborough, MA, USA) running buffer with analysis temperature at 37 °C. Protein A was immobilized on flow cells of a CM4 chip using amine coupling (Cytiva, BR100050) to enable antibody capture. Antibody samples were prepared at 5 µg/ml. IL-13 samples were prepared at final concentrations of 100, 50, 25, 12.5, 6.25, 3.125, 1.56, 0.78, 0.39 and 0 (blank) nM in running buffer. Data were processed using standard double referencing and fit to a 1:1 binding model using Biacore Evaluation software (version 2.0.1) to determine the association rate (on-rate, kon, M−1 s−1 units) and the dissociation rate (off-rate, koff, s−1 units). The equilibrium dissociation constant (KD) was calculated from the relationship KD = koff/kon and is in molar units.
Competitive Binding of Anti-IL-13 mAbs to Recombinant Glycosylated Human IL-13 at 25 °C
Cendakimab and tralokinumab were directly immobilized on separate flow cells of a CM4 chip (Cytiva, BR100050). Sequential injections of human IL-13 (100 nM) and cendakimab, lebrikizumab, tralokinumab or control IgG (5 µg/ml) were made to assess binding. Experiments were conducted in triplicate using a Biacore T200 (Cytiva, Marlborough, MA, USA).
Cell-Based Neutralization Assays
STAT6 Reporter Assay
HEK293 cells transfected with STAT-6 SEAP-Blue reporter (HEK-Blue IL-4/IL-13 cells, InvivoGen, San Diego, CA, USA) were cultured in assay medium (DMEM, 10% FBS, Normocin, Zeocin and Blasticidin). HEK-Blue IL-4/IL-13 cells (300,000/well) were plated into a 96-well plate, which was placed in tissue culture incubator (37 °C, 95% relative humidity, 5% CO2) overnight. Cells were treated with a dose range from 0 to 13.3 nM IL-13 mAbs, IL-4 mAb (R&D Systems, Minneapolis, MN) or isotype control in the presence of 3 ng/ml glycosylated IL-13, 0.3 ng/ml aglycosylated IL-13 or 1 ng/ml IL-4 and placed overnight in tissue culture incubator. Cell supernatant (25 µl) was removed from each well, and AP activity was measured using QUANTI-Blue solution (InvivoGen, San Diego, CA, USA) following the manufacturer’s instructions. Testing was done in triplicate. The testing of the fluorophore conjugated IL-13 and IL-4 was done in a similar manner with the cytokines being tested in triplicate from 0 to 60 ng/ml.
Human Dermal Fibroblast Periostin Secretion Assay
Primary human dermal fibroblast cells (Lonza, Basel, Switzerland) were cultured in supplemented fibroblast growth medium (Lonza). Cells were plated at 7500 cells/well in 96-well tissue culture plate and placed in an overnight tissue culture incubator. The next day, cells were treated with a dose range from 0 to 200 nM IL-13 mAbs or isotype control mAb in the presence of 200 ng/ml glycosylated IL-13 and placed in a tissue culture incubator for 48 h; 100 µl/well of supernatant was collected to measure periostin levels by ELISA (R&D Systems, Minneapolis, MN, USA) according to the manufacturer’s instructions. Testing was done in triplicate.
IL-13Rα2 Internalization Experiments
Human A375 skin melanoma cells and HaCaT (spontaneously transformed keratinocyte cell line from adult human skin) were purchased from ATCC and AddexBio, respectively. The cells were cultured on CellCarrier-96 Ultra microplates (Perkin Elmer, Waltham, MA, USA) or chambered coverglass (ThermoFisher Scientific, Waltham, MA, USA). HaCaT cells were induced to express IL-13Ra2 with 3 days co-treatment of 10 ng/ml IL-4 and 50 ng/ml TNF-alpha. For imaging experiments, confluent cell layers were incubated with 0.1 µg/ml Hoechst 33342 (ThermoFisher Scientific) for nuclear stain and different combinations of 5 µg/ml anti-IL-13Rα2-Alexa Fluor (AF) 488 (R&D Systems, Minneapolis, MN, USA) or 5 µg/ml anti-IL-13Rα1-AF488 (made internally by Eli Lilly) for receptor stain or 500 ng/ml IL-13-AF568 or 500 ng/ml IL-4-AF568 or 7.5 µg/ml lebrikizumab-AF647 or 7.5 µg/ml cendakimab-AF647 or 24.8 µg/ml tralokinumab-AF647 or 7.5 µg/ml isotype control-AF647 for 1 h. Media were replaced and cells were imaged using an Opera Phenix (Perkin Elmer, Waltham, MA, USA) with a 40× water objective or with an LSM880 (Zeiss, Oberkochen, Germany) with a 40× water objective and 1.5× zoom, both at 37 °C, 5% CO2 and humidity. For IL-13/lebrikizumab complex and IL-13/isotype co-localization with Lysoview-488 (Biotium, Fremont, CA), media were replaced with media containing 1:30,000 dilution of Lysoview-AF488, and cells were imaged using an Opera Phenix with 7–11 fields of view every 30 min for 10 h. Co-localizations with Lysoview-AF488 at 7 h post-complex addition to cells from three independent experiments were quantified using Manders’ co-localization coefficients.
Ethics Statement
This study was not a clinical trial and was focused on in vitro experiments, using commercial cell lines. No individual human samples were used in this study. Accordance to the Declaration of Helsinki was not applicable. IRB approval is not done for this type of research.
Results
Binding Affinity and Epitope
Surface plasmon resonance (SPR) experiments were conducted at 37 °C to determine the binding kinetics (kon, koff) and affinity (KD) of IL-13 mAbs to human IL-13. Because the endogenous glycosylation state of IL-13 in humans is not known, we tested the binding of lebrikizumab, cendakimab and tralokinumab to both glycosylated and aglycosylated forms of the molecule. All three mAbs exhibited binding to both glycosylated and aglycosylated IL-13 (Fig. 1). While the on-rates for the three mAbs were comparable, lebrikizumab had the slowest off-rate for both glycosylated and aglycosylated human IL-13 compared to tralokinumab and cendakimab, driving differences in overall binding affinity. Lebrikizumab bound glycosylated and aglycosylated human IL-13 with a KD of 187 ± 7.9 pM and 6.3 ± 0.9 pM, respectively. Tralokinumab exhibited the weakest binding affinity of the three mAbs with a KD of 1804 ± 154 pM to glycosylated IL-13 and 904 ± 119 pM to aglycosylated IL-13. In comparison, cendakimab exhibited weaker binding to both glycosylated and aglycosylated IL-13 with a KD of 1132 ± 67 pM and 130 ± 8.7 pM, respectively. SPR was also used to evaluate whether the antibodies bind to IL-13 at the same or different epitopes (Supplement Fig. 2). Cendakimab or tralokinumab was immobilized on separate flow cells of a Biacore CM4 chip, and IL-13 was injected and its binding detected. A subsequent injection of lebrikizumab, tralokinumab, cendakimab or IgG control to cendakimab-or tralokinumab-bound IL-13 was made to assess whether binding could occur. Lebrikizumab exhibited binding to both cendakimab-bound IL-13 and tralokinumab-bound IL-13. In contrast, cendakimab did not bind cendakimab-bound IL-13 or tralokinumab-bound IL-13. Similarly, tralokinumab did not bind IL-13 that was pre-bound to either cendakimab or tralokinumab. These data demonstrate that tralokinumab and cendakimab bind to overlapping epitopes on IL-13 whereas lebrikizumab binds to a different epitope on IL-13 than either tralokinumab or cendakimab.
Surface plasmon resonance sensorgrams for the binding of anti-IL-13 mAbs to recombinant glycosylated or aglycosylated human IL-13 at 37 °C. The mAbs were captured on the surface of a CM4 chip with immobilized Protein A followed by the injection of different concentrations of IL-13 to assess the binding kinetics on a T200 Biacore. IL-13 reagents were expressed in HEK293 and purified by standard methods. Double reference subtracted binding sensorgrams and a 1:1 binding model fit are shown. Three independent experimental replicates (n) were conducted for the binding of lebrikizumab, tralokinumab and cendakimab human glycosylated and aglycoslyated IL-13
Cell-based IL-13 Neutralization Assays
A human HEK293-STAT6 reporter cell line naturally expressing IL-4Rα and IL-13Rα1 was used to measure IL-13 mAbs inhibition of the STAT6 pathway by glycosylated and aglycosylated human IL-13. As shown in Fig. 2A and 2B, lebrikizumab, tralokinumab and cendakimab inhibited both glycosylated and aglycosylated IL-13-induced STAT6 activity in a dose-dependent manner. The average half maximal inhibitory concentration IC50 (± SD) from three independent experiments showed that lebrikizumab inhibited human glycosylated IL-13 at 13 ± 1 pM; the IC50 of tralokinumab was 97 ± 16 pM and 37 ± 16 pM for cendakimab. The mAbs neutralized aglycosylated IL-13 in the same relative order with lebrikizumab having the highest potency. The STAT6 reporter assay was also used to confirm that lebrikizumab, tralokinumab and cendakimab did not neutralize IL-4-induced STAT6 signaling (Supplement Fig. 3). A primary human dermal fibroblast assay was used to measure IL-13 mAbs inhibition of the IL-13 induced periostin secretion in cell culture supernatant by immunoassay [31]. Lebrikizumab, tralokinumab and cendakimab all inhibited human IL-13-induced periostin secretion in a dose-dependent manner (Fig. 2C) with lebrikizumab being the most potent. The average IC50 (\(\pm\) SD) from three independent experiments showed that lebrikizumab inhibited periostin secretion at 7 ± 1 nM whereas tralokinumab and cendakimab had an IC50 of 21 ± 1 and 13 ± 2 nM, respectively.
Cell-based neutralization assays. Human STAT6-HEK293 cells were incubated overnight with compounds and 3 ng/ml glycosylated hIL-13 (A) or 0.3 ng/ml aglycosylated IL-13 (B) at 37 °C at 5% CO2. STAT6-reporter activation was measured by absorbance of QuantiBlue reagent. Results are representative of three independent experiments. C Human dermal fibroblast cells were incubated for 48 h with compounds and 200 ng/ml glycosylated hIL-13 at 37 °C at 5% CO [2] in serum-free media. Periostin levels were measured by ELISA. All IL-13 mAbs completely inhibited IL-13-induced periostin activity in a dose-dependent manner. Results are representative of three independent experiments
IL-13 bound to membrane and internalized through IL-13Rα2 on A375 cells. A A375 cells were incubated with Hoechst 33342 (blue) and anti-IL-13Rα2-AF488 (green), IL-13-AF568 (red), anti-IL-13Rα1-AF488 (green) or IL-4-AF568 (red). IL-13-AF568 (red) bound to IL-13Rα2 is expressed by A375, but IL-4-AF568 (red) is not. IL-13Rα1 is not expressed by the cells. Merge image shows the overlay of IL-13Rα2 with IL-13. B IL-13-AF568 (red) bound to IL-13Rα2 on the membrane of A375 cells after 1 h incubation, and IL-13 internalization was observed at 3 and 7 h
IL-13 Internalization Through IL-13Rα2
IL-13 binding and internalization into cells through IL-13Rα2 were studied in A375 (human melanoma cell line) cells. A375 cells do not express IL-13Rα1 (as shown by the absence of anti-IL13Rα1 or IL-4 staining) but do express IL-13Rα2 (Fig. 3A). In addition, membrane binding of anti-IL-13Rα2 and IL-13 was observed on A375 cells, and IL-13 co-localized with the IL-13Rα2 (Fig. 3A). After binding, IL-13 was internalized within 7 h (Fig. 3B). Then, we determined whether IL-13 internalization through IL-13Rα2 occurred in the presence of anti-IL-13 mAbs. IL-13 was pre-incubated with each mAb and added to A375 cells. The IL-13/lebrikizumab complex bound to the A375 cells but neither the IL-13/tralokinumab nor the IL-13/cendakimab complexes bound (Fig. 4A). Due to the lower affinity and faster off-rate of tralokinumab, more of this antibody was added to the cell culture system than cendakimab to completely inhibit IL-13 binding to the A375 cells. The isotype control mAb did not impede IL-13 binding to A375 cells (Fig. 4A). Next, we tracked internalization into the A375 cells. After 7 h, the IL-13/lebrikizumab complex was internalized similarly to the IL-13/isotype control and was found to co-localize with lysosomes (Fig. 4B) with > 95% of the internalized IL-13/lebrikizumab complex co-localizing with the lysosome marker inside A375 cells (Fig. 4C).
Lebrikizumab/IL-13 complex binding, internalization and co-localization with lysosome marker in A375 cells. A Only IL-13/lebrikizumab complex bound to IL-13Rα2 on cell membrane. Cells were stained with Hoechst 33342 (blue) and with IL-13-AF568 (red) complexed with lebrikizumab-AF647 or cendakimab-AF647 or tralokinumab-AF647 or isotype control-AF647 (green). B IL-13-AF568 (yellow) in the presence of isotype control-AF647 or lebrikizumab-AF647 (red) bound on the membrane at 1 h and completely internalized through IL-13Rα2 at 7 h. Matching punctate staining pattern of internalized IL-13/lebrikizumab complex with Lysoview-AF488 was observed in multiple wells from three independent experiments. C More than 95% of internalized IL-13/lebrikizumab co-localized with Lysoview-AF488 (green), which suggested that the complex went into lysosomes. Co-localization with Lysoview-AF488 at 7 h from triplicate wells was quantified using Manders’ co-localization coefficient
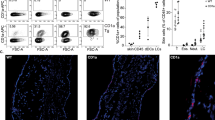
To examine IL-13 internalization through IL-13Rα2 on keratinocytes, HaCaT cells, a spontaneously immortalized human keratinocyte cell line, were used. HaCaT cells express IL-13Rα2 in response to IL-4 or IL-13 stimulation [32] suggesting functional IL-4R and IL-13Rα1 on the surface of the cells. IL-13Rα2 was undetectable in untreated HaCaT cells; however, following 3 days of treatment with IL-4/TNF-α, positive anti-IL-13Rα2 staining was observed (Fig. 5A). Additionally, IL-13-AF568 can be seen binding to the membrane of the IL-4/TNF-α-treated cells (Fig. 5A). IL-13Rα1 could not be detected through staining on either the untreated or IL-4/TNFα-treated HaCaT cells. To ensure IL-13 only bound to IL-13Rα2 and not to IL-13Rα1, HaCaT cells were preincubated with IL-13Rα1 inhibitory antibody in all subsequent imaging experiments. Following induction of IL-13Rα2 on HaCaT cells, IL-13 was internalized into the cells within 7 h (Fig. 5B). Next, we evaluated whether the IL-13 mAbs interfered with internalization of IL-13. Like the results with A375 cells, the IL-13/lebrikizumab complex bound to the surface of the HaCaT cells, while IL-13/tralokinumab or IL-13/cendakimab complexes did not (Fig. 6A). Due to the lower affinity and faster off-rate of tralokinumab, more of this antibody was also added to the HaCaT cell system than cendakimab to completely inhibit IL-13 binding to the cells. The isotype mAb did not impede IL-13 binding to the HaCaT cells. The IL-13/lebrikizumab complex was internalized into the HaCaT cells within 7 h and co-localized with lysosomes (Fig. 6B). More than 95% of the internalized IL-13/lebrikizumab complex co-localized with lysosome marker inside HaCaT cells (Fig. 6C). Together, these results indicate a complex of lebrikizumab/IL-13 can internalize through the IL13Rα2 decoy receptor and co-localize with lysosomes, where it is likely to be degraded resulting in the clearance of IL-13.
IL-13 bound to membrane and internalized through IL-13Rα2 on activated HaCaT cells. A IL-13Rα2 expression was induced on human HaCaT cells with IL-4/TNF-alpha co-treatment. Hoechst 33342 (blue) and anti-IL-13Rα1-AF488 (green) or anti-IL-13Rα2-AF488 (green) or IL-13-AF568 (red) was added for 1 h. IL-13Rα2 was expressed on the membrane following induction, and IL-13 bound to the receptor on the membrane after 1 h incubation. IL13Rα1 could not be visualized with staining. B IL-13-AF568 internalization through induced IL-13Rα2 in human HaCaT cells. IL-13-AF568 (red) bound to IL-13Rα2 on the membrane of HaCaT cells after 1 h incubation, and IL-13 internalization was observed at 3 and 7 h
Lebrikizumab/IL-13 complex binding, internalization and co-localization with lysosome marker in HaCaT cells. A Only IL-13/lebrikizumab complex bound to IL-13Rα2 on cell membrane. Cells were stained with Hoechst 33342 (blue) and with IL-13-AF568 (red) complexed with lebrikizumab-AF647 or cendakimab-AF647 or tralokinumab-AF647 or isotype control-AF647 (green). B IL-13-AF568 (yellow) in the presence of isotype control-AF647 or lebrikizumab-AF647 (red) bound on the membrane at 1 h and completely internalized through IL-13Rα2 at 7 h. Matching punctate staining pattern of internalized IL-13/lebrikizumab complex with Lysoview-AF488 was observed in multiple wells from three independent experiments. C More than 95% of internalized IL-13/lebrikizumab co-localized with Lysoview-AF488 (green), which suggested that the complex went into lysosomes. Co-localization with Lysoview-AF488 at 7 h from triplicate wells was quantified using Manders’ co-localization coefficient
Discussion
IL-13 is a central pathogenic mediator driving multiple features of AD pathophysiology [3,4,5], and inhibition of the IL-13 pathway is a target for multiple therapeutic mAbs in AD, including lebrikizumab, tralokinumab and cendakimab [33, 34]. The molecular characteristics of each of these mAbs likely determine aspects of clinical efficacy in patients with AD. Lebrikizumab binds to both the glycosylated and aglycosylated forms of IL-13 with stronger binding affinity driven by a slower dissociation rate than either tralokinumab or cendakimab. Because the endogenous glycosylation state of IL-13 in humans is not known, we tested the binding of the IL-13 mAbs to both glycosylated and aglycosylated forms of the molecule. Additionally, lebrikizumab demonstrated higher potency in cell-based inhibition assays compared to tralokinumab or cendakimab. This higher potency of lebrikizumab is probably a direct function of the higher binding affinity with slower off-rate, which allows lebrikizumab to sequester IL-13 from the IL-4Rα/IL-13Rα1 receptor complex for a longer period. For the primary cell-based inhibition assay, we utilized IL-13 induced secretion of periostin from dermal fibroblasts. Periostin secretion was selected because of its upregulation with IL-13 stimulation and association with type 2 immunity and AD. Periostin influences tissue remodeling and fibrosis and contributes to itch induction, thus further driving inflammatory processes [35, 36] and has been shown to be elevated in patients with AD [37].
The results demonstrate that lebrikizumab binds to IL-13 via a different, non-overlapping epitope than tralokinumab or cendakimab. This difference has important consequences as it allows binding and internalization of the IL-13/lebrikizumab complex to IL-13Rα2, whereas tralokinumab and cendakimab prevent IL-13 binding to IL-13Rα2 providing a mechanistic differentiation from lebrikizumab. IL-13Rα2 can be induced by IL-4 or IL-13 through activation of the IL-4Rα/IL-13Rα1 receptor and is believed to represent a negative regulatory loop of IL-13 in AD [38]. Results from a clinical trial testing IL-13 mAbs with two different, nonoverlapping epitopes in patients with asthma suggested that epitope specificity may impact the clearance of IL-13 [39]. Kasaian et al. proposed that IL-13Ra2-mediated IL-13 clearance modulated the IL-13 levels that were observed in that study. Based upon our in vitro observations, we are proposing a similar mechanism is at work when comparing lebrikizumab to tralokinumab and cendakimab. We demonstrate that the internalization of the IL-13/lebrikizumab complex co-localized to lysosomes, suggesting that the internalized IL-13 and lebrikizumab proteins are degraded. Lysosomes dispose of, and recycle, macromolecules, such as proteins, as part of their canonical role in cellular waste clearance [40]. This mechanism for regulation of IL-13 levels is inhibited by tralokinumab and cendakimab and might lead to continued presence of IL-13 in the system, dictated by the binding equilibrium of the mAbs to IL-13.
The differences in molecular characteristics between these IL-13 therapeutic mAbs may help in the understanding of the differences seen in the clinical trial results reported to date. Head-to-head clinical data comparing the efficacy of lebrikizumab to the other IL-13 therapeutic mAbs are not available. However, published data suggest that more patients achieve clinically meaningful outcomes (percent of patients achieving IGA score of 0/1 or EASI75) after 16 weeks of treatment with monotherapy lebrikizumab [41] versus those treated with tralokinumab [42]. The differences in AD clinical efficacy between lebrikizumab and tralokinumab are likely due to multiple factors, including different mechanisms of action for IL-13 inhibition, dosing regimens, pharmacokinetics and/or trial patient population. Clinical AD trial results have yet to be published for cendakimab. In our studies, we did not include the activity of dupilumab, a mAb that binds to IL-4Rα and inhibits downstream signaling of the receptor induced by both IL-4 and IL-13 [43] because of the difficulty of making direct comparisons between mAbs binding to receptors or cytokines in in vitro systems. These in vitro systems do not allow for other mechanistic differences that occur during in vivo use such as pharmacokinetic variations and target-mediated drug disposition, which have been reported for dupilumab [44].
The results document several differences between IL-13 mAbs currently in clinical development. Nonetheless, it is not known if or how these different characteristics translate to the response observed in the clinic; factors such as pharmacokinetic variations, biological complexity or trial patient populations are not recapitulated in the current study. The IL-13/lebrikizumab internalization studies through the IL-13Ra2 receptor were performed using skin-derived cell lines and not primary cells or tissue models and may not reflect the complexity of this mechanism in patients. Furthermore, we did not use clinical grade material antibodies for our studies, as those were not available at the time of our studies; it is unclear whether that impacted our results.
Conclusion
In conclusion, lebrikizumab is an IL-13 mAb with higher binding affinity, slower binding disassociation rate and higher in vitro potency than other IL-13 mAbs, tralokinumab or cendakimab. Additionally, lebrikizumab binds to a different epitope on IL-13 that does not interfere with the natural IL-13 clearance through the IL-13Rα2 compared to tralokinumab and cendakimab. These in vitro results provide evidence for molecular and mechanistic differences among lebrikizumab, tralokinumab and cendakimab, which might translate into differences in clinical efficacy for patients with AD.
References
Werfel T, Allam JP, Biedermann T, et al. Cellular and molecular immunologic mechanisms in patients with atopic dermatitis. J Allergy Clin Immunol. 2016;138(2):336–49.
Simon D, Wollenberg A, Renz H, Simon HU. Atopic Dermatitis: Collegium Internationale Allergologicum (CIA) Update 2019. Int Arch Allergy Immunol. 2019;178(3):207–18.
Brandt EB, Sivaprasad U. Th2 Cytokines and Atopic Dermatitis. J Clin Cell Immunol. 2011;2(3).
Brunner PM, Guttman-Yassky E, Leung DY. The immunology of atopic dermatitis and its reversibility with broad-spectrum and targeted therapies. J Allergy Clin Immunol. 2017;139(4S):S65–76.
Buzney CD, Gottlieb AB, Rosmarin D. Asthma and Atopic Dermatitis: A Review of Targeted Inhibition of Interleukin-4 and Interleukin-13 As Therapy for Atopic Disease. J Drugs Dermatol. 2016;15(2):165–71.
Bin L, Leung DY. Genetic and epigenetic studies of atopic dermatitis. Allergy Asthma Clin Immunol. 2016;12:52.
Bieber T. Interleukin-13: Targeting an underestimated cytokine in atopic dermatitis. Allergy. 2020;75(1):54–62.
Hummelshoj T, Bodtger U, Datta P, et al. Association between an interleukin-13 promoter polymorphism and atopy. Eur J Immunogenet. 2003;30(5):355–9.
Kim BE, Leung DY, Boguniewicz M, Howell MD. Loricrin and involucrin expression is down-regulated by Th2 cytokines through STAT-6. Clin Immunol. 2008;126(3):332–7.
Cabanillas B, Novak N. Atopic dermatitis and filaggrin. Curr Opin Immunol. 2016;42:1–8.
Howell MD, Fairchild HR, Kim BE, et al. Th2 cytokines act on S100/A11 to downregulate keratinocyte differentiation. J Invest Dermatol. 2008;128(9):2248–58.
Howell MD, Boguniewicz M, Pastore S, et al. Mechanism of HBD-3 deficiency in atopic dermatitis. Clin Immunol. 2006;121(3):332–8.
Purwar R, Werfel T, Wittmann M. IL-13-stimulated human keratinocytes preferentially attract CD4+CCR4+ T cells: possible role in atopic dermatitis. J Invest Dermatol. 2006;126(5):1043–51.
Nguyen JK, Austin E, Huang A, Mamalis A, Jagdeo J. The IL-4/IL-13 axis in skin fibrosis and scarring: mechanistic concepts and therapeutic targets. Arch Dermatol Res. 2020;312(2):81–92.
May RD, Fung M. Strategies targeting the IL-4/IL-13 axes in disease. Cytokine. 2015;75(1):89–116.
Choy DF, Hsu DK, Seshasayee D, et al. Comparative transcriptomic analyses of atopic dermatitis and psoriasis reveal shared neutrophilic inflammation. J Allergy Clin Immunol. 2012;130(6):1335–43.
Tazawa T, Sugiura H, Sugiura Y, Uehara M. Relative importance of IL-4 and IL-13 in lesional skin of atopic dermatitis. Arch Dermatol Res. 2004;295(11):459–64.
Tsoi LC, Rodriguez E, Degenhardt F, et al. Atopic Dermatitis Is an IL-13-Dominant Disease with Greater Molecular Heterogeneity Compared to Psoriasis. J Invest Dermatol. 2019;139(7):1480–9.
Junttila IS. Tuning the Cytokine Responses: An Update on Interleukin (IL)-4 and IL-13 Receptor Complexes. Front Immunol. 2018;9:888.
Minty A, Chalon P, Derocq JM, et al. Interleukin-13 is a new human lymphokine regulating inflammatory and immune responses. Nature. 1993;362(6417):248–50.
Zurawski G, de Vries JE. Interleukin 13, an interleukin 4-like cytokine that acts on monocytes and B cells, but not on T cells. Immunol Today. 1994;15(1):19–26.
Rael EL, Lockey RF. Interleukin-13 signaling and its role in asthma. World Allergy Organ J. 2011;4(3):54–64.
Chiaramonte MG, Mentink-Kane M, Jacobson BA, et al. Regulation and function of the interleukin 13 receptor alpha 2 during a T helper cell type 2-dominant immune response. J Exp Med. 2003;197(6):687–701.
Moyle M, Cevikbas F, Harden JL, Guttman-Yassky E. Understanding the immune landscape in atopic dermatitis: The era of biologics and emerging therapeutic approaches. Exp Dermatol. 2019;28(7):756–68.
Sivaprasad U, Warrier MR, Gibson AM, et al. IL-13Ralpha2 has a protective role in a mouse model of cutaneous inflammation. J Immunol. 2010;185(11):6802–8.
Bernard FX, Morel F, Camus M, et al. Keratinocytes under Fire of Proinflammatory Cytokines: Bona Fide Innate Immune Cells Involved in the Physiopathology of Chronic Atopic Dermatitis and Psoriasis. J Allergy (Cairo). 2012;2012: 718725.
Ultsch M, Bevers J, Nakamura G, et al. Structural basis of signaling blockade by anti-IL-13 antibody Lebrikizumab. J Mol Biol. 2013;425(8):1330–9.
Popovic B, Breed J, Rees DG, et al. Structural Characterisation Reveals Mechanism of IL-13-Neutralising Monoclonal Antibody Tralokinumab as Inhibition of Binding to IL-13Ralpha1 and IL-13Ralpha2. J Mol Biol. 2017;429(2):208–19.
Tripp CS, Cuff C, Campbell AL, et al. RPC4046, A Novel Anti-interleukin-13 Antibody, Blocks IL-13 Binding to IL-13 alpha1 and alpha2 Receptors: A Randomized, Double-Blind, Placebo-Controlled. Dose-Escalation First-in-Human Study Adv Ther. 2017;34(6):1364–81.
BLA Approval. 2021; https://www.accessdata.fda.gov/drugsatfda_docs/appletter/2021/761180Orig1s000ltr.pdf. Accessed 2022.
Maeda D, Kubo T, Kiya K, et al. Periostin is induced by IL-4/IL-13 in dermal fibroblasts and promotes RhoA/ROCK pathway-mediated TGF-beta1 secretion in abnormal scar formation. J Plast Surg Hand Surg. 2019;53(5):288–94.
David M, Ford D, Bertoglio J, Maizel AL, Pierre J. Induction of the IL-13 receptor alpha2-chain by IL-4 and IL-13 in human keratinocytes: involvement of STAT6, ERK and p38 MAPK pathways. Oncogene. 2001;20(46):6660–8.
Newsom M, Bashyam AM, Balogh EA, Feldman SR, Strowd LC. New and Emerging Systemic Treatments for Atopic Dermatitis. Drugs. 2020;80(11):1041–52.
Ratchataswan T, Banzon TM, Thyssen JP, Weidinger S, Guttman-Yassky E, Phipatanakul W. Biologics for Treatment of Atopic Dermatitis: Current Status and Future Prospect. J Allergy Clin Immunol Pract. 2021;9(3):1053–65.
Sonnenberg-Riethmacher E, Miehe M, Riethmacher D. Periostin in Allergy and Inflammation. Front Immunol. 2021;12: 722170.
Hashimoto T, Mishra SK, Olivry T, Yosipovitch G. Periostin, an Emerging Player in Itch Sensation. J Investig Dermatol. 2021;141(10):2338–43.
Kou K, Okawa T, Yamaguchi Y, et al. Periostin levels correlate with disease severity and chronicity in patients with atopic dermatitis. Br J Dermatol. 2014;171(2):283–91.
Furue M. regulation of skin barrier function via competition between AHR axis versus IL-13/IL-4JAKSTAT6/STAT3 axis: Pathogenic and therapeutic implications in atopic dermatitis. J Clin Med. 2020;9(11).
Kasaian MT, Raible D, Marquette K, et al. IL-13 antibodies influence IL-13 clearance in humans by modulating scavenger activity of IL-13Ralpha2. J Immunol. 2011;187(1):561–9.
Trivedi PC, Bartlett JJ, Pulinilkunnil T. Lysosomal biology and function: Modern view of cellular debris bin. Cells. 2020;9(5).
Silverberg J, Thaci, D; Seneschal, J; Gold, LS; Blauvelt, A; Simpson, E; Chu, C; Liu, ZT; Lima, RJ; Pillai, S; Guttman-Yassky, E Efficacy and Safety of Lebrikizumab in Moderate-to-Severe Atopic Dermatitis: Results From Two Phase 3, Randomized, Double-Blinded, Placebo-Controlled Trials. Paper presented at: American Academy of Dermatology; March 26, 2022, 2022; Boston.
Wollenberg A, Blauvelt A, Guttman-Yassky E, et al. Tralokinumab for moderate-to-severe atopic dermatitis: results from two 52-week, randomized, double-blind, multicentre, placebo-controlled phase III trials (ECZTRA 1 and ECZTRA 2). Br J Dermatol. 2021;184(3):437–49.
Harb H, Chatila TA. Mechanisms of Dupilumab. Clin Exp Allergy. 2020;50(1):5–14.
Li Z, Radin A, Li M, et al. Pharmacokinetics, Pharmacodynamics, Safety, and Tolerability of Dupilumab in Healthy Adult Subjects. Clin Pharmacol Drug Dev. 2020;9(6):742–55.
Acknowledgements
Funding
Eli Lilly and Company funded this study and the journal’s Rapid Service Fee (no grant numbers apply).
Medical Writing and Editorial Assistance
Matthew Jeffries and Henning Stockmann provided consultation on site-selective protein conjugation. Anthony Ransdell provided protein generation. Zhe Sun provided statistical support. Parth Patel, PharmD, and Rebecca Anderson, PhD, provided medical writing and editorial support.
Author Contributions
Angela J. Okragly, Aya Ryuzoji, Isabella Wulur, Montanea Daniels, Robert D. Van Horn, Chetan N. Patel and Robert J. Benschop contributed to the study conception and design. Material preparation, data collection and analysis were performed by all authors. The first draft of the manuscript was written by Angela Okragly and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Disclosures
Angela J. Okragly, Aya Ryuzoji, Isabella Wulur, Montanea Daniels, Robert D. Van Horn, Chetan N. Patel and Robert J. Benschop are employees of Eli Lilly and Company. The authors report no other conflicts of interest in this work.
Compliance with Ethics Guidelines
This study was not a clinical trial and focused on in vitro experiments using commercial cell lines. No individual human samples were used in this study. Accordance to the Declaration of Helsinki was not applicable. IRB approval is not done for this type of research.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Okragly, A.J., Ryuzoji, A., Wulur, I. et al. Binding, Neutralization and Internalization of the Interleukin-13 Antibody, Lebrikizumab. Dermatol Ther (Heidelb) 13, 1535–1547 (2023). https://doi.org/10.1007/s13555-023-00947-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13555-023-00947-7