Abstract
Background
We assessed the effect of supervised, combined aerobic and resistance exercise on diabetic parameters in Japanese patients with type 2 diabetes mellitus (T2DM).
Methods
This 12-week, multicenter (17 medical institutions), open-label, parallel-group study (clinicaltrials.jp; JapicCTI-184002), randomized (1:1) Japanese patients aged 20–75 years with T2DM and hemoglobin A1c (HbA1c) of 7.0–10.0% to supervised exercise (n = 113) or standard therapy (n = 115). The supervised exercise group undertook supervised aerobic (30 min) and resistance exercise 3 times/week (20 designated gyms). Primary endpoint was change in HbA1c from baseline at week 13. Secondary endpoints were change in fasting blood glucose (FBG), glycoalbumin, fasting insulin, homeostatic model assessment of insulin resistance (HOMA-IR), and HOMA-β at week 13.
Results
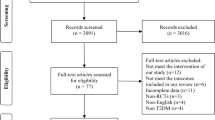
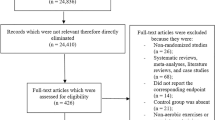
Of 228 randomized patients, 97 (85.8%) in the supervised exercise group and 108 (93.9%) in the standard therapy group completed the study. Supervised exercise significantly lowered HbA1c at week 13 versus standard therapy (estimated difference in change from baseline [95% confidence interval]: − 0.44% [− 0.61, − 0.28], p < 0.001). Supervised exercise also significantly decreased FBG (estimated difference: − 13.0 [− 19.2, − 6.7] mg/dL) and glycoalbumin (estimated difference: − 1.52% [− 2.10, − 0.93]) compared with standard therapy. Fasting insulin (− 0.5 µIU/mL) and HOMA-IR (− 0.3) decreased with supervised exercise, but group differences were not significant. Treatment-emergent adverse events were more frequent in the supervised exercise group (42.5%) than in the standard therapy group (29.6%); however, no major safety concerns were identified.
Conclusions
A structured, supervised, aerobic and resistance exercise program improved HbA1c and was well accepted among patients with T2DM.


Similar content being viewed by others
Data accessibility and materials
Researchers may request access to anonymized participant level data, trial level data, and protocols from Astellas-sponsored clinical trials at www.clinicalstudydatarequest.com. For the Astellas criteria on data sharing, see: https://clinicalstudydatarequest.com/Study-Sponsors/Study-Sponsors-Astellas.aspx.
References
Boulé NG, Haddad E, Kenny GP, Wells GA, Sigal RJ. Effects of exercise on glycemic control and body mass in type 2 diabetes mellitus: a meta-analysis of controlled clinical trials. JAMA. 2001;286(10):1218–27. https://doi.org/10.1001/jama.286.10.1218.
Gordon BA, Benson AC, Bird SR, Fraser SF. Resistance training improves metabolic health in type 2 diabetes: a systematic review. Diabetes Res Clin Pract. 2009;83(2):157–75. https://doi.org/10.1016/j.diabres.2008.11.024.
Sampath Kumar A, Maiya AG, Shastry BA, Vaishali K, Ravishankar N, Hazari A, et al. Exercise and insulin resistance in type 2 diabetes mellitus: a systematic review and meta-analysis. Ann Phys Rehabil Med. 2019;62(2):98–103. https://doi.org/10.1016/j.rehab.2018.11.001.
Snowling NJ, Hopkins WG. Effects of different modes of exercise training on glucose control and risk factors for complications in type 2 diabetic patients: a meta-analysis. Diabetes Care. 2006;29(11):2518–27. https://doi.org/10.2337/dc06-1317.
Nery C, Moraes SRA, Novaes KA, Bezerra MA, Silveira PVC, Lemos A. Effectiveness of resistance exercise compared to aerobic exercise without insulin therapy in patients with type 2 diabetes mellitus: a meta-analysis. Braz J Phys Ther. 2017;21(6):400–15. https://doi.org/10.1016/j.bjpt.2017.06.004.
Pan B, Ge L, Xun YQ, Chen YJ, Gao CY, Han X, et al. Exercise training modalities in patients with type 2 diabetes mellitus: a systematic review and network meta-analysis. Int J Behav Nutr Phys Act. 2018;15(1):72. https://doi.org/10.1186/s12966-018-0703-3.
Umpierre D, Ribeiro PA, Kramer CK, Leitão CB, Zucatti AT, Azevedo MJ, et al. Physical activity advice only or structured exercise training and association with HbA1c levels in type 2 diabetes: a systematic review and meta-analysis. JAMA. 2011;305(17):1790–9. https://doi.org/10.1001/jama.2011.576.
Araki E, Goto A, Kondo T, Noda M, Noto H, Origasa H, et al. Japanese clinical practice guideline for diabetes 2019. Diabetol Int. 2020;11(3):165–223. https://doi.org/10.1007/s13340-020-00439-5.
Japan Diabetes Society: Treatment guide for diabetes 2016–2017. http://www.fa.kyorin.co.jp/jds/uploads/Treatment_Guide_for_Diabetes_2016-2017.pdf. Accessed September 8, 2020.
Colberg SR, Sigal RJ, Yardley JE, Riddell MC, Dunstan DW, Dempsey PC, et al. Physical activity/exercise and diabetes: a position statement of the American Diabetes Association. Diabetes Care. 2016;39(11):2065–79. https://doi.org/10.2337/dc16-1728.
Kamiya A, Ohsawa I, Fujii T, Nagai M, Yamanouchi K, Oshida Y, et al. A clinical survey on the compliance of exercise therapy for diabetic outpatients. Diabetes Res Clin Pract. 1995;27(2):141–5. https://doi.org/10.1016/0168-8227(95)01032-9.
Arakawa S, Watanabe T, Sone H, Tamura Y, Kobayashi M, Kawamori R, et al. The factors that affect exercise therapy for patients with type 2 diabetes in Japan: a nationwide survey. Diabetol Int. 2015;6:19–25. https://doi.org/10.1007/s13340-014-0166-y.
Okada S, Hiuge A, Makino H, Nagumo A, Takaki H, Konishi H, et al. Effect of exercise intervention on endothelial function and incidence of cardiovascular disease in patients with type 2 diabetes. J Atheroscler Thromb. 2010;17(8):828–33. https://doi.org/10.5551/jat.3798.
Takenami E, Iwamoto S, Shiraishi N, Kato A, Watanabe Y, Yamada Y, et al. Effects of low-intensity resistance training on muscular function and glycemic control in older adults with type 2 diabetes. J Diabetes Investig. 2019;10(2):331–8. https://doi.org/10.1111/jdi.12926.
American Diabetes Association Standards of Medical Care in Diabetes—2016. 3. Foundations of care and comprehensive medical evaluation. Diabetes Care. 2016;39(Suppl 1):S23–35. https://doi.org/10.2337/dc16-S006.
Haneda M, Noda M, Origasa H, Noto H, Yabe D, Fujita Y, et al. Japanese clinical practice guideline for diabetes 2016. J Diabetes Investig. 2018;9(3):657–97. https://doi.org/10.1111/jdi.12810.
American College of Sports Medicine. ACSM’s guidelines for exercise testing and prescription (10th edition). Philadelphia: Wolters Kluwer; 2018.
Colberg SR, Sigal RJ, Fernhall B, Regensteiner JG, Blissmer BJ, Rubin RR, et al. Exercise and type 2 diabetes: the American College of Sports Medicine and the American Diabetes Association: joint position statement. Diabetes Care. 2010;33(12):e147–67. https://doi.org/10.2337/dc10-9990.
Church TS, Blair SN, Cocreham S, Johannsen N, Johnson W, Kramer K, et al. Effects of aerobic and resistance training on hemoglobin A1c levels in patients with type 2 diabetes: a randomized controlled trial. JAMA. 2010;304(20):2253–62. https://doi.org/10.1001/jama.2010.1710.
Sigal RJ, Kenny GP, Boulé NG, Wells GA, Prud’homme D, Fortier M, et al. Effects of aerobic training, resistance training, or both on glycemic control in type 2 diabetes: a randomized trial. Ann Intern Med. 2007;147(6):357–69. https://doi.org/10.7326/0003-4819-147-6-200709180-00005.
Vinetti G, Mozzini C, Desenzani P, Boni E, Bulla L, Lorenzetti I, et al. Supervised exercise training reduces oxidative stress and cardiometabolic risk in adults with type 2 diabetes: a randomized controlled trial. Sci Rep. 2015;5:9238. https://doi.org/10.1038/srep09238.
Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346(6):393–403. https://doi.org/10.1056/NEJMoa012512.
Umpierrez G, Tofé Povedano S, Pérez Manghi F, Shurzinske L, Pechtner V. Efficacy and safety of dulaglutide monotherapy versus metformin in type 2 diabetes in a randomized controlled trial (AWARD-3). Diabetes Care. 2014;37(8):2168–76. https://doi.org/10.2337/dc13-2759.
Seino Y, Hiroi S, Hirayama M, Kaku K. Efficacy and safety of alogliptin added to sulfonylurea in Japanese patients with type 2 diabetes: a randomized, double-blind, placebo-controlled trial with an open-label, long-term extension study. J Diabetes Investig. 2012;3(6):517–25. https://doi.org/10.1111/j.2040-1124.2012.00226.x.
DeFronzo RA, Fleck PR, Wilson CA, Mekki Q, Alogliptin Study 010 Group. Efficacy and safety of the dipeptidyl peptidase-4 inhibitor alogliptin in patients with type 2 diabetes and inadequate glycemic control: a randomized, double-blind, placebo-controlled study. Diabetes Care. 2008;31(12):2315–7. https://doi.org/10.2337/dc08-1035.
Balducci S, Leonetti F, Di Mario U, Fallucca F. Is a long-term aerobic plus resistance training program feasible for and effective on metabolic profiles in type 2 diabetic patients? Diabetes Care. 2004;27(3):841–2. https://doi.org/10.2337/diacare.27.3.841.
Sato Y, Sone H, Kobayashi M, Kawamori R, Atsumi Y, Oshida Y, et al. Current situation of exercise therapy in patients with diabetes mellitus in Japan (Report No. 2): a nationwide survey to patients using the questionnaires. J Japan Diab Soc. 2015;58(11):850–9. https://doi.org/10.11213/tonyobyo.58.850
Ministry of Health Labour and Welfare: 2018 National Health and Nutrition Survey Report. https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/kenkou_iryou/kenkou/eiyou/h30-houkoku_00001.html. Accessed September 8, 2020.
Japan Diabetes Clinical Data Management Study Group. 2018. http://jddm.jp/data/index-2018. Accessed 10 July 2020.
Acknowledgements
The authors would like to thank all study participants, medical staff, and exercise trainers. We also acknowledge the contribution of Motohiro Kanayama (Astellas Pharma Inc.) in the design of the exercise program and assistance with conducting the trial.
This study was funded by Astellas Pharma Inc. Medical writing assistance was provided by Rebecca Lew, PhD, CMPP, and Joanna Best, PhD, of ProScribe-Envision Pharma Group, funded by Astellas Pharma Inc. ProScribe’s services complied with international guidelines for Good Publication Practice (GPP3).
Funding
Astellas Pharma Inc. was involved in the study design, data collection, data analysis, and preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
All authors participated in the study design, analysis, and interpretation of study results, and in the drafting, critical revision, and approval of the final version of the manuscript. Tetsushi Takada collected the data. All authors agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflicts of interest
Yasuo Terauchi has received lecture fees from Astellas Pharma Inc., AstraZeneca K.K., Daiichi Sankyo Co., Ltd., Dainippon Sumitomo Pharma Co., Ltd., Eli Lilly Japan K.K., Merck Sharp & Dohme K.K., Mitsubishi Tanabe Pharma Corporation, Nippon Boehringer Ingelheim Co., Ltd., Novo Nordisk Pharma Ltd., Ono Pharmaceutical Co., Ltd., Sanofi K.K., Sanwa Kagaku Kenkyusho Co., Ltd., Taisho Toyama Pharmaceutical Co., Ltd., and Takeda Pharmaceutical Co., Ltd., and has received research donations from AstraZeneca K.K., Daiichi Sankyo Co., Ltd., Dainippon Sumitomo Pharma Co., Ltd., Eli Lilly Japan K.K., Merck Sharp & Dohme K.K., Nippon Boehringer Ingelheim Co., Ltd., Novo Nordisk Pharma Ltd., Ono Pharmaceutical Co., Ltd., Sanofi K.K., and Takeda Pharmaceutical Co., Ltd. Tetsushi Takada is an employee of Astellas Pharma Inc. Satoshi Yoshida is an employee of Astellas Pharma Inc.
Ethical standards
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and/or with the Helsinki Declaration of 1964 and later versions. Informed consent was obtained from all patients for being included in the study.
Human rights statement
This research involves human participants. The study protocol was approved by the local ethics committee at each medical institution, the Medical Corporation Toukeikai Kitamachi Clinic Ethical Review Board (approval number AST05921, approved June 28, 2018), or the Joint Ethical Review Board (approval number 14000050.20180817-4654, approved August 17, 2018).
Informed consent
All patients provided written informed consent before participating.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Terauchi, Y., Takada, T. & Yoshida, S. A randomized controlled trial of a structured program combining aerobic and resistance exercise for adults with type 2 diabetes in Japan. Diabetol Int 13, 75–84 (2022). https://doi.org/10.1007/s13340-021-00506-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-021-00506-5