Abstract
Background
Studies on frequency and risk factors of gastroesophageal reflux disease (GERD) in the rural Indian population are scanty.
Methods
This household survey was undertaken by the trained interviewers in the adult population (≥ 18 years) in four villages in northern India using translated-validated Enhanced Asian Rome III and hospital anxiety and depression questionnaires.
Results
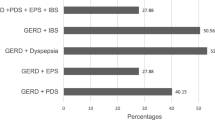
Of 2774 subjects, 2019 (72.8%) had no heartburn. Heartburn frequency was as follows: 314 (11.3%) once/week, 143 (5.2%) twice/week, 85 (3.1%) thrice/week, 69 (2.5%) four times/week, 48 (1.7%) five times/week, 18 (0.6%) six times/week, 41 (1.5%) daily, 37 (1.4%) > once daily. A total of 298 (10.7%) had GERD (definition: heartburn > twice/week). Older age (36.5 vs. 35 years), non-Hindu religion (7, 2.4% vs. 30, 1.2%), lower education (127, 42.6% vs. 789, 31.9%), lower socioeconomic class (94, 31.5% vs. 517, 20.9%) and income (below Indian National Rupees [INR] 458; 105, 35.2% vs. 599, 24.2%), non-vegetarian diet (15, 5% vs. 105, 4.2%), intake of tea/coffee (260, 87.2% vs. 1687, 68.1%), carbonated soft drinks (216, 72.5% vs. 1234, 49.8%), and alcohol (48, 16.1% vs. 313, 12.6%), tobacco chewing (116, 38.9% vs. 681, 27.5%), and smoking (105, 35.2% vs. 672, 27.1%) were associated with GERD on univariate analysis. On multivariate analysis, body mass index > 25 kg/m2 (odds ratio [OR] 1.23; 95% CI 0.88–1.71), predominant rice eating (1.13; 0.74–1.74), tobacco chewing and smoking (1.68; 1.24–2.30 and 1.36; 0.99–1.88), and alcohol (1.2; 0.78–1.83) and carbonated soft drinks (2.48; 1.79–3.44) intake were associated with GERD. A total of 122 (41%) had associated functional dyspepsia. Psychological comorbidities were commoner among those with than without GERD.
Conclusion
In this rural Indian population, 10.7% had GERD and predominant rice eating, tobacco chewing, and carbonated soft drink intake were the risk factors. Psychological comorbidities were common.




Similar content being viewed by others
References
Clarrett DM, Hachem C. Gastroesophageal reflux disease (GERD). Mo Med. 2018;115:214–8.
Sharma PK, Ahuja V, Madan K, Gupta S, Raizada A, Sharma MP. Prevalence, severity, and risk factors of symptomatic gastroesophageal reflux disease among employees of a large hospital in northern India. Indian J Gastroenterol. 2011;30:128–34.
Chowdhury SD, George G, Ramakrishna K, et al. Prevalence and factors associated with gastroesophageal reflux disease in southern India: a community-based study. Indian J Gastroenterol. 2019;38:77–82.
Bhatia SJ, Reddy DN, Ghoshal UC, et al. Epidemiology and symptom profile of gastroesophageal reflux in the Indian population: report of the Indian Society of Gastroenterology Task Force. Indian J Gastroenterol. 2011;30:118–27.
Jung HK. Epidemiology of gastroesophageal reflux disease in Asia: a systematic review. J Neurogastroenterol Motil. 2011;17:14–27.
Kumar S, Sharma S, Norboo T, et al. Population based study to assess prevalence and risk factors of gastroesophageal reflux disease in a high altitude area. Indian J Gastroenterol. 2011;30:135–43.
Nirwan JS, Hasan SS, Babar ZU, Conway BR, Ghori MU. Global prevalence and risk factors of gastro-oesophageal reflux disease (GORD): systematic review with meta-analysis. Sci Rep. 2020;10:5814.
Mohammed I, Nightingale P, Trudgill NJ. Risk factors for gastro-oesophageal reflux disease symptoms: a community study. Aliment Pharmacol Ther. 2005;21:821–7.
Eusebi LH, Ratnakumaran R, Yuan Y, Solaymani-Dodaran M, Bazzoli F, Ford AC. Global prevalence of, and risk factors for, gastro-oesophageal reflux symptoms: a meta-analysis. Gut. 2018;67:430–40.
Yamasaki T, Hemond C, Eisa M, Ganocy S, Fass R. The changing epidemiology of gastroesophageal reflux disease: are patients getting younger? J Neurogastroenterol Motil. 2018;24:559–69.
Bor S, Kitapcioglu G, Kasap E. Prevalence of gastroesophageal reflux disease in a country with a high occurrence of Helicobacter pylori. World J Gastroenterol. 2017;23:525–32.
Chandran S, Raman R, Kishor M, Nandeesh HP. The effectiveness of mindfulness meditation in relief of symptoms of depression and quality of life in patients with gastroesophageal reflux disease. Indian J Gastroenterol. 2019;38:29–38.
Bruley des Varannes S, Löfman HG, Karlsson M, et al. Cost and burden of gastroesophageal reflux disease among patients with persistent symptoms despite proton pump inhibitor therapy: an observational study in France. BMC Gastroenterol. 2013;13:39.
Zhang L, Tu L, Chen J, et al. Health-related quality of life in gastroesophageal reflux patients with noncardiac chest pain: emphasis on the role of psychological distress. World J Gastroenterol. 2017;23:127–34.
Maleki I, Masoudzadeh A, Khalilian A, Daheshpour E. Quality of life in patients with gastroesophageal reflux disease in an Iranian population. Gastroenterol Hepatol Bed Bench. 2013;6:96–100.
Lee SW, Lee TY, Lien HC, Peng YC, Yeh HJ, Chang CS. Correlation between symptom severity and health-related life quality of a population with gastroesophageal reflux disease. Gastroenterology Res. 2017;10:78–83.
Wiklund I. Review of the quality of life and burden of illness in gastroesophageal reflux disease. Dig Dis. 2004;22:108–14.
Irvine EJ. Quality of life assessment in gastro-oesophageal reflux disease. Gut. 2004;53 Suppl 4:iv35–9.
Chang P, Friedenberg F. Obesity and GERD. Gastroenterol Clin N Am. 2014;43:161–73.
Pan J, Cen L, Chen W, Yu C, Li Y, Shen Z. Alcohol consumption and the risk of gastroesophageal reflux disease: a systematic review and meta-analysis. Alcohol Alcohol. 2019;54:62–9.
Bhatia SJ, Makharia GK, Abraham P, et al. Indian consensus on gastroesophageal reflux disease in adults: a position statement of the Indian Society of Gastroenterology. Indian J Gastroenterol. 2019;38:411–40.
El-Serag HB, Satia JA, Rabeneck L. Dietary intake and the risk of gastro-oesophageal reflux disease: a cross sectional study in volunteers. Gut. 2005;54:11–7.
Kubo A, Levin TR, Block G, et al. Alcohol types and sociodemographic characteristics as risk factors for Barrett’s esophagus. Gastroenterology. 2009;136:806–15.
Sethi S, Richter JE. Diet and gastroesophageal reflux disease: role in pathogenesis and management. Curr Opin Gastroenterol. 2017;33:107–11.
Newberry C, Lynch K. The role of diet in the development and management of gastroesophageal reflux disease: why we feel the burn. J Thorac Dis. 2019;11:S1594–601.
Ghoshal UC, Gwee KA, Chen M, et al. Development, translation and validation of enhanced Asian Rome III Questionnaires for diagnosis of functional bowel diseases in major Asian languages: a Rome Foundation-Asian Neurogastroenterology and Motility Association working team report. J Neurogastroenterol Motil. 2015;21:83–92.
Ghoshal UC, Singh R. Frequency and risk factors of functional gastro-intestinal disorders in a rural Indian population. J Gastroenterol Hepatol. 2017;32:378–87.
Richter JE, Rubenstein JH. Presentation and epidemiology of gastroesophageal reflux disease. Gastroenterology. 2018;154:267–76.
Arivan R, Deepanjali S. Prevalence and risk factors of gastro-esophageal reflux disease among undergraduate medical students from a southern Indian medical school: a cross-sectional study. BMC Res Notes. 2018;11:448.
Wang HY, Leena KB, Plymoth A, et al. Prevalence of gastro-esophageal reflux disease and its risk factors in a community-based population in southern India. BMC Gastroenterol. 2016;16:36.
Delshad SD, Almario CV, Chey WD, Spiegel BMR. Prevalence of gastroesophageal reflux disease and proton pump inhibitor-refractory symptoms. Gastroenterology. 2020;158:1250–1261.e2.
Rahman MM, Ghoshal UC, Kibria MG, et al. Prevalence, risk factors, and healthcare-seeking among subjects with esophageal symptoms: a community-based study in a rural Bangladeshi population. JGH Open. 2020;4:1167–75.
Geeraerts A, Van Houtte B, Clevers E, et al. Gastroesophageal reflux disease-functional dyspepsia overlap: do birds of a feather flock together? Am J Gastroenterol. 2020;115:1167–82.
Acknowledgments
The authors thank the Shanti Public Educational and Development Society (www.spreadhealth.in) for its support and Mr. Kailash Chaurasia (Village: Chhataura) and Ritesh Kumar Singh (Village: Bastibandgan) from Jaunpur for helping in the fieldwork. The authors also thank Prashant Singh for his assistance. The authors also thank all the community subjects for participating in the study. Rajan Singh thanks the Indian Council of Medical Research (ICMR) for junior and senior research fellowships.
Author information
Authors and Affiliations
Contributions
Uday C. Ghoshal: study concept, design, contribution to planning, execution of the work, supervision of work, contribution to data analysis, and critical revision of the manuscript for important intellectual content; Rajan Singh: execution of the work, data collection, data analysis, and drafting of the manuscript. Sushmita Rai: help in data analysis and manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
UCG, RS, and SR declare that they have no conflict of interest.
Ethics statement
The study was performed conforming to the Helsinki declaration of 1975, as revised in 2000 and 2008 concerning human and animal rights, and the authors followed the policy concerning informed consent as shown on Springer.com.
Disclaimer
The authors are solely responsible for the data and the contents of the paper. In no way, the Honorary Editor-in-Chief, Editorial Board Members, the Indian Society of Gastroenterology or the printer/publishers are responsible for the results/findings and content of this article.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ghoshal, U.C., Singh, R. & Rai, S. Prevalence and risk factors of gastroesophageal reflux disease in a rural Indian population. Indian J Gastroenterol 40, 56–64 (2021). https://doi.org/10.1007/s12664-020-01135-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-020-01135-7