Abstract
Background
A growing number of studies suggest that job loss has detrimental effects on cancer survivors. However, the underlying mechanisms are not well understood. Furthermore, minorities including Asian American cancer survivors remain understudied, yet they suffer from job loss more often. The present study examined the prevalence of job loss in Chinese American breast cancer survivors (CABCS) and investigated the relationship between job loss and well-being in this group and the underlying mechanisms.
Method
CABCS completed a questionnaire that included demographic, employment, and clinical information, as well as measures of psychosocial well-being. Descriptive analyses were conducted to gauge the prevalence of job loss, linear regressions were used to test associations between job loss and well-being, and path analyses were conducted to test mediations.
Results
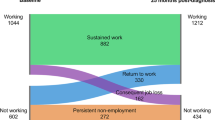
About 45.4% of survivors lost their job after being diagnosed with cancer, and only 35.2% of those who lost their job regained employment up to the assessment time. Job loss was associated with reduced income, which was associated with higher perceived stress, which, in turn, was associated with lower overall quality of life (QoL) and greater depressive symptoms.
Conclusions
Findings highlight the high prevalence of job loss and its negative effects on QoL and depression among CABCS. It is important for health care professionals to be sensitive to adverse financial events affecting minority BCS. In addition to offering BCS necessary practical assistance, psychosocial interventions focusing on reducing perceived stress associated with the cancer experience may be effective in mitigating some long-term consequences of job loss.


Similar content being viewed by others
References
Mujahid MS, Janz NK, Hawley ST, Griggs JJ, Hamilton AS, Graff J, et al. Racial/ethnic differences in job loss for women with breast cancer. J Cancer Surviv. 2011;5(1):102–11.
Mehnert A. Employment and work-related issues in cancer survivors. Crit Rev Oncol Hematol. 2011;77(2):109–30.
van Egmond MP, Duijts SFA, Loyen A, Vermeulen SJ, van der Beek AJ, Anema JR. Barriers and facilitators for return to work in cancer survivors with job loss experience: a focus group study. Eur J Cancer Care (Engl). 2017;26(5): e12420.
Bouknight RR, Bradley CJ, Luo Z. Correlates of return to work for breast cancer survivors. J Clin Oncol. 2006;24(3):345–53.
Tamminga SJ, De Boer AG, Verbeek JH, Frings-Dresen MH. Breast cancer survivors’ views of factors that influence the return-to-work process-a qualitative study. Scand J Work Environ Health. 2012:144–54.
Ketterl TG, Syrjala KL, Casillas J, Jacobs LA, Palmer SC, McCabe MS, et al. Lasting effects of cancer and its treatment on employment and finances in adolescent and young adult cancer survivors. Cancer. 2019;125(11):1908–17.
Smith GL, Lopez-Olivo MA, Advani PG, Ning MS, Geng Y, Giordano SH, et al. Financial burdens of cancer treatment: a systematic review of risk factors and outcomes. J Natl Compr Canc Netw. 2019;17(10):1184–92.
Bray F, Ren JS, Masuyer E, Ferlay J. Global estimates of cancer prevalence for 27 sites in the adult population in 2008. Int J Cancer. 2013;132(5):1133–45.
Lee SY, Kim SJ, Shin J, Han KT, Park EC. The impact of job status on quality of life: general population versus long-term cancer survivors. Psycho-Oncol. 2015;24(11):1552–9.
Lindbohm ML, Kuosma E, Taskila T, Hietanen P, Carlsen K, Gudbergsson S, et al. Early retirement and non-employment after breast cancer. Psycho-Oncol. 2014;23(6):634–41.
Cohen S, Gianaros PJ, Manuck SB. A stage model of stress and disease. Perspect Psychol Sci. 2016;11(4):456–63.
Dooley D. Unemployment, underemployment, and mental health: conceptualizing employment status as a continuum. Am J Community Psychol. 2003;32(1–2):9–20.
Montel S, Clark K, Loscalzo M. Elevated distress, race/ethnicity age, education, income, and type of cancer: it is complicated. Psycho-Oncol. 2018;27(4):1334–7.
Jørgensen L, Garne JP, Søgaard M, Laursen BS. The experience of distress in relation to surgical treatment and care for breast cancer: an interview study. Eur J Oncol Nurs. 2015;19(6):612–8.
Hobfoll SE, Halbesleben J, Neveu J-P, Westman M. Conservation of resources in the organizational context: the reality of resources and their consequences. Annu Rev Organ Psych. 2018;5(1):103–28.
Powell-Wiley TM, Baumer Y, Baah FO, Baez AS, Farmer N, Mahlobo CT, et al. Social determinants of cardiovascular disease. Circ Res. 2022;130(5):782–99.
Ell K, Xie B, Wells A, Nedjat-Haiem F, Lee PJ, Vourlekis B. Economic stress among low-income women with cancer: effects on quality of life. Cancer. 2008;112(3):616–25.
Low CA, Stanton AL, Thompson N, Kwan L, Ganz PA. Contextual life stress and coping strategies as predictors of adjustment to breast cancer survivorship. Ann Behav Med. 2006;32(3):235–44.
Beatty L, Lee C, Wade TD. A prospective examination of perceived stress as a mediator of the relationship between life-events and QOL following breast cancer. Br J Health Psychol. 2009;14(4):789–804.
Yearby R. Structural racism and health disparities: reconfiguring the social determinants of health framework to include the root cause. J Law Med Ethics. 2020;48(3):518–26.
Blinder VS, Eberle C, Patil S, Gany FM, Bradley CJ. Women with breast cancer who work for accommodating employers more likely to retain jobs after treatment. Health Affair. 2017;36(2):274–81.
Blinder VS, Patil S, Eberle CE, Jung G, Kampel LJ, Hwang C, et al. Work status after treatment for breast cancer: a controlled, prospective, longitudinal study of an ethnically diverse cohort. J Clin Oncol. 2018;36(15_suppl):6583.
Pisu M, Kenzik KM, Oster RA, Drentea P, Ashing KT, Fouad M, et al. Economic hardship of minority and non-minority cancer survivors 1 year after diagnosis: Another long-term effect of cancer? Cancer. 2015;121(8):1257–64.
Spencer JC, Rotter JS, Eberth JM, Zahnd WE, Vanderpool RC, Ko LK, et al. Employment changes following breast cancer diagnosis: the effects of race and place. J Natl Cancer Inst. 2020;112(6):647–50.
Samuel CA, Spencer JC, Rosenstein DL, Reeder-Hayes KE, Manning ML, Sellers JB, et al. Racial differences in employment and cost-management behaviors in patients with metastatic breast cancer. Breast Cancer Res Treat. 2020;179(1):207–15.
Han SJ. Asian values, intergenerational conflict, needs, and attachment in Asian/Asian American women’s disordered eating. Couns Psychol. 2020;48(4):526–50.
Lu Q, Gallagher MW, Loh A, Young L. Expressive writing intervention improves quality of life among Chinese-American breast cancer survivors: a randomized controlled trial. Ann Behav Med. 2018;52(11):952–62.
Tedeschi RG, Calhoun LG. The posttraumatic growth inventory: measuring the positive legacy of trauma. J Trauma Stress. 1996;9(3):455–71.
Cohen S, Kamarck T, Mermelstein R. A global measure of perceived stress. J Health Soc Behav. 1983;24:385–96.
Leung DY, Lam TH, Chan SS. Three versions of perceived stress scale: validation in a sample of Chinese cardiac patients who smoke. BMC Public Health. 2010;10(1):513.
Brady MJ, Cella DF, Mo F, Bonomi AE, Tulsky DS, Lloyd SR, et al. Reliability and validity of the functional assessment of cancer therapy-breast quality-of-life instrument. J Clin Oncol. 1997;15(3):974–86.
Wan C, Zhang D, Yang Z, Tu X, Tang W, Feng C, et al. Validation of the simplified Chinese version of the FACT-B for measuring quality of life for patients with breast cancer. Breast Cancer Res Treat. 2007;106(3):413–8.
Derogatis LR. The Brief Symptom Inventory-18 (BSI-18): Administration. Scoring, and Procedures Manual (3rd ed), Minneapolis: National Computer Systems. 2000.
Wang J, Kelly BC, Liu T, Zhang G, Hao W. Factorial structure of the Brief Symptom Inventory (BSI)-18 among Chinese drug users. Drug Alcohol Depend. 2013;133(2):368–75.
Andresen EM, Malmgren JA, Carter WB, Patrick DL. Screening for depression in well older adults: evaluation of a short form of the CES-D. Am J Prev Med. 1994;10(2):77–84.
Cheng ST, Chan AC. The center for epidemiologic studies depression scale in older Chinese: thresholds for long and short forms. Int J Geriatr Psychiatry. 2005;20(5):465–70.
Muthén LK, Muthén, BO (1998–2015). Mplus user’s guide. Seventh edition. Los Angeles, CA: Muthén & Muthén; 1998–2015.
Mackinnon DP, Lockwood CM, Williams J. Confidence limits for the indirect effect: distribution of the product and resampling methods. Multivariate Behav Res. 2004;39(1):99-.
Bradley CJ, Neumark D, Luo Z, Schenk M. Employment and cancer: findings from a longitudinal study of breast and prostate cancer survivors. Cancer Invest. 2007;25(1):47–54.
Maunsell E, Drolet M, Brisson J, Brisson C, Mâsse B, Deschênes L. Work situation after breast cancer: results from a population-based study. J Natl Cancer Inst. 2004;96(24):1813–22.
Cohen S, Janicki-Deverts D, Miller GE. Psychological stress and disease. JAMA. 2007;298(14):1685–7.
Ekwueme DU, Zhao J, Rim SH, de Moor JS, Zheng Z, Khushalani JS, et al. Annual out-of-pocket expenditures and financial hardship among cancer survivors aged 18–64 years—United States, 2011–2016. Morb Mortal Wkly Rep. 2019;68(22):494–9.
Edward J, Petermann VM, Eberth JM, Zahnd WE, Vanderpool RC, Askelson N, et al. Interventions to address cancer-related financial toxicity: recommendations from the field. J Rural Health. 2022;38(4):817–26.
Warmoth K, Cheung B, You J, Yeung NCY, Lu Q. Exploring the social needs and challenges of Chinese American immigrant breast cancer survivors: a qualitative study using an expressive writing approach. Int J Behav Med. 2017;24(6):827–35.
You J, Wang C, Yeung NCY, Lu Q. Socioeconomic status and quality of life among Chinese American breast cancer survivors: the mediating roles of social support and social constraints. Psycho-Oncol. 2018;27(7):1742–9.
Kong YC, Bhoo-Pathy N, Wong LP, Aziz A, Taib N, Yehgambaram P, et al. Employment challenges faced by breast cancer survivors in an upper middle–income Asian setting. J Glob Oncol. 2018;4 (Supple_2), 119s.
Bradley CJ, Wilk A. Racial differences in quality of life and employment outcomes in insured women with breast cancer. J Cancer Surviv. 2014;8(1):49–59.
Acknowledgements
The authors thank the Herald Cancer Association for their support in recruiting participants and data collection. The authors thank Kate J. Krause, in the Research Medical Library at MD Anderson Cancer Center, for her assistance with the literature review, and Gary Deyter for his editing service provided on this manuscript.
Funding
This study was funded by the American Cancer Society (grant number: MRSGT-10–011-01-CPPB, PI: Qian Lu). Lingjun Chen's research at Shanghai Jiao Tong University is partly supported by Shanghai Pujiang Program (grant number 21PJC077). Grace L. Smith’s research is supported by NIH/NCI K07CA211804 and the Andrew Sabin Family Fellowship.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The first author completed the data analysis and the first draft at The University of Texas MD Anderson Cancer Center and revised the manuscript to make it ready for submission at Shanghai Jiao Tong University.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, L., Wang, C., Smith, G.L. et al. Job Loss and Well-Being Among Chinese American Breast Cancer Survivors: The Mediating Role of Income and Perceived Stress. Int.J. Behav. Med. (2024). https://doi.org/10.1007/s12529-023-10245-3
Accepted:
Published:
DOI: https://doi.org/10.1007/s12529-023-10245-3