Abstract
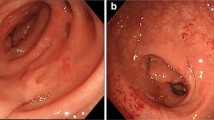
Diversion colitis and ulcerative colitis (UC) can be caused by different mechanisms; however, several case reports have described the development of typical UC following diversion colitis. A 63-year-old man underwent Hartmann’s operation following a diagnosis of perforation of a sigmoid colon diverticulum and peritonitis. Stoma closure was performed 4 months later, and the portion of the sigmoid colon with the diverticulum was unintentionally left as a blind end. Following stoma closure, hematochezia worsened, and he was diagnosed as having developed diversion colitis only in the blind sigmoid colon. Intermittent use of topical mesalazine enemas controlled the bowel symptoms; however, 4 years after the stoma closure, bloody stools were observed again. Colonoscopy revealed coarse and friable granular mucosa with adherent mucopurulent exudate in the rectum, and mucosal erythematous edema with adherent mucopurulent exudate in the blind sigmoid colon. The histological findings indicated basal plasmacytosis, and goblet cell depletion and cryptitis in the lamina propria, which is characteristic of UC. To the best of our knowledge, this is the fourth description of a patient who developed UC following diversion colitis. Local inflammation may have triggered the development of UC through hematogenous or lymphogenous circulation of lymphocytes or autoantibodies.




Similar content being viewed by others
Abbreviations
- UC:
-
Ulcerative colitis
- SCFA:
-
Short chain fatty acid
References
Ungaro R, Mehandru S, Allen PB, et al. Ulcerative colitis. Lancet. 2017;389:1756–70.
Glotzer DJ, Glick ME, Goldman H. Proctitis and colitis following diversion of the fecal stream. Gastroenterology. 1981;80:438–41.
Morson BC, Dawson IM. Gastrointestinal pathology. 1st ed. London: Blackwell Scientific Publications; 1972.
Lim AG, Langmead FL, Feakins RM, et al. Diversion colitis: a trigger for ulcerative colitis in the in-stream colon? Gut. 1999;44:279–82.
Jowett SL, Cobden I. Diversion colitis as a trigger for ulcerative colitis. Gut. 2000;46:294.
Tominaga K, Kamimura K, Takahashi K, et al. Diversion colitis and pouchitis: a mini-review. World J Gastroenterol. 2018;24:1734–47.
Hokama A, Kinjo F, Tomiyama R, et al. Progression of diverticular colitis to ulcerative colitis. Inflamm Bowel Dis. 2005;11:681.
Ikeda A, Mizushima T, Egashira Y, et al. Diverticular colitis with progression to ulcerative colitis after sigmoidectomy. Clin J Gastroenterol. 2018;11:42–7.
Gore S, Shepherd NA, Wilkinson SP. Endoscopic crescentic fold disease of the sigmoid colon: the clinical and histopathological spectrum of a distinctive endoscopic appearance. Int J Colorectal Dis. 1992;7:76–81.
Makapugay LM, Dean PJ. Diverticular disease-associated chronic colitis. Am J Surg Pathol. 1996;20:94–102.
Vulsteke F, De Hertogh G, Vermeire S. Therapeutic outcome of diverticular associated colitis–a retrospective single centre experience. Acta Gastroenterol Belg. 2021;84:275–81.
Matsune Y, Yaguchi K, Saito S, et al. Simultaneous development of ulcerative colitis in the sigmoidocolon autotransplant neovagina and the residual colorectum. Inflamm Bowel Dis. 2022;28:e18–20.
Swidsinski A, Ladhoff A, Pernthaler A, et al. Mucosal flora in inflammatory bowel disease. Gastroenterology. 2002;122:44–54.
Johansson ME, Gustafsson JK, Holmén-Larsson J, et al. Bacteria penetrate the normally impenetrable inner colon mucus layer in both murine colitis models and patients with ulcerative colitis. Gut. 2014;63:281–91.
Kuwada T, Shiokawa M, Kodama Y, et al. Identification of an anti-integrin αvβ6 autoantibody in patients with ulcerative colitis. Gastroenterology. 2021;160:2383–94.
Geng X, Biancone L, Dai HH, et al. Tropomyosin isoforms in intestinal mucosa: production of autoantibodies to tropomyosin isoforms in ulcerative colitis. Gastroenterology. 1998;114:912–22.
Acknowledgements
We thank Jane Charbonneau, DVM, from Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Contributions
KY, MY, and RK: literature search, data collection and interpretation, and manuscript writing. KA, HK, YI, and SM: interpretation and critical revision of the manuscript. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human/animal rights
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendment.
Informed consent
Written Informed consent was obtained from the patient.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yaguchi, K., Matsune, Y., Kunisaki, R. et al. Progression of ulcerative colitis following diversion colitis. Clin J Gastroenterol 15, 1088–1093 (2022). https://doi.org/10.1007/s12328-022-01696-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-022-01696-4