Abstract
Introduction
Hepatic fibrosis is an inevitable process of hepatic sclerosis, malignancy, and insufficiency, and hydronidone is an innovative antifibrosis drug. This study focus on the pharmacokinetic interaction of hydronidone and entecavir in healthy Chinese male subjects.
Methods
An open-label, three-period, multiple-dosage, self-controlled clinical trial was executed in 12 healthy male subjects. In period 1, the subjects took hydronidone 60 mg, q8h, for 7 days. In period 2, they were given entecavir 0.5 mg once daily for 9 days. Then, hydronidone and entecavir were given in combination for 6 days (days 20–26). Blood samples were taken up to 24 h post-dosing, while pre-dose blood samples were drawn on days 7, 19, and 26.
Results
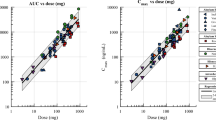
The area under the curve (AUC)0–t_ss of entecavir slightly increased from 15.56 ± 2.67 to 16.17 ± 2.77 ng h/ml with coadministration with hydronidone, while the other pharmacokinetic parameters of hydronidone and entecavir were comparable between monotherapy and combination therapy. The geometric mean ratios (GMRs) [90% confidence intervals (CIs)] of Cmax_ss, AUC0–t_ss, and AUC0–∞_ss of entecavir after coadministration compared with entecavir alone were 107.21% (97.04–118.45%), 103.85% (100.94–106.83%), and 110.81% (97.19–126.33%), respectively. And the GMRs and 90% CIs of Cmax,ss, AUC0–t_ss, and AUC0–∞_ss for combination therapy compared with the hydronidone monotherapy group were 102.72% (84.21–125.29%), 106.52% (97.06–116.90%), and 108.86% (96.42–122.89%), respectively.
Conclusions
There was no drug–drug interaction between hydronidone and entecavir in healthy male volunteers. However, multiple doses of hydronidone have a risk with increasing exposure to entecavir in vivo, which needs to be further clarified.
Registration number
ChiCTR2200059683 (retrospectively registered).




Similar content being viewed by others
References
Bansal R, Nagorniewicz B, Prakash J. Clinical advancements in the targeted therapies against liver fibrosis. Mediators Inflamm. 2016. https://doi.org/10.1155/2016/7629724.
Koyama Y, Brenner DA. Liver inflammation and fibrosis. J Clin Investig. 2017;127(1):55–64. https://doi.org/10.1172/JCI88881.
Moon AM, Singal AG, Tapper EB. Contemporary epidemiology of chronic liver disease and cirrhosis. Clin Gastroenterol Hepatol. 2020;18(12):2650–66. https://doi.org/10.1016/j.cgh.2019.07.060.
Liang TJ. Hepatitis B: the virus and disease. Hepatology (Baltimore, MD). 2009;49(5 Suppl):S13–21. https://doi.org/10.1002/hep.22881.
Cheemerla S, Balakrishnan M. Global epidemiology of chronic liver disease. Clin Liver Dis. 2021;17(5):365–70. https://doi.org/10.1002/cld.1061.
Naghavi M, Wang H, Lozano R, Davis A, Liang X, Zhou M, et al. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;385(9963):117–71. https://doi.org/10.1016/s0140-6736(14)61682-2.
Le S, Ansari U, Mumtaz A, Malik K, Patel P, Doyle A, et al. Lynch Syndrome and Muir-Torre Syndrome: An update and review on the genetics, epidemiology, and management of two related disorders. Dermatol Online J. 2017. https://doi.org/10.5070/D32311037239.
Guo Y-C, Lu L-G. Antihepatic fibrosis drugs in clinical trials. J Clin Transl Hepatol. 2020;8(3):304–12. https://doi.org/10.14218/jcth.2020.00023.
Tan Z, Sun H, Xue T, Gan C, Liu H, Xie Y, et al. Liver fibrosis: therapeutic targets and advances in drug therapy. Front Cell Dev Biol. 2021. https://doi.org/10.3389/fcell.2021.730176.
Chinese Society of Hepatology CMA, Chinese Society of Gastroenterology CMA, Chinese Society of Infectious Diseases CMA. Consensus on the diagnosis and therapy of hepatic fibrosis in 2019. Chin J Hepatol. 2019;27(9):657–67.
Hu H-H, Chen D-Q, Wang Y-N, Feng Y-L, Cao G, Vaziri ND, et al. New insights into TGF-beta/Smad signaling in tissue fibrosis. Chem Biol Interact. 2018;292:76–83. https://doi.org/10.1016/j.cbi.2018.07.008.
Armendariz-Borunda J, Islas-Carbajal MC, Meza-Garcia E, Rincon AR, Lucano S, Sandoval AS, et al. A pilot study in patients with established advanced liver fibrosis using pirfenidone. Gut. 2006;55(11):1663–5. https://doi.org/10.1136/gut.2006.107136.
Flores-Contreras L, Sandoval-Rodriguez AS, Mena-Enriquez MG, Lucano-Landeros S, Arellano-Olivera I, Alvarez-Alvarez A, et al. Treatment with pirfenidone for two years decreases fibrosis, cytokine levels and enhances CB2 gene expression in patients with chronic hepatitis C. Bmc Gastroenterol. 2014. https://doi.org/10.1186/1471-230x-14-131.
Liao H, Li Z, Deng L, Fan H, Luo Y. Hydronidone attenuates renal interstitial fibrosis in rat model of obstructive nephropathy. Chin J Pharm. 2014;45(10):950–5.
Dai T, Luo T, He Y, Gu X, Tang R, Dong J, et al. Effect of atrial fibrosis on atrial structural remodeling and inflammation in atrial fibrillation canines. J Third Military Med Univ. 2013;35(22):2409–14.
Hou J-L, Zhao W, Lee C, Hann H-W, Peng C-Y, Tanwandee T, et al. Outcomes of long-term treatment of chronic HBV infection with entecavir or other agents from a randomized trial in 24 countries. Clin Gastroenterol Hepatol. 2020;18(2):457. https://doi.org/10.1016/j.cgh.2019.07.010.
Chang T-T, Liaw Y-F, Wu S-S, Schiff E, Han K-H, Lai C-L, et al. Long-term entecavir therapy results in the reversal of fibrosis/cirrhosis and continued histological improvement in patients with chronic hepatitis B. Hepatology. 2010;52(3):886–93. https://doi.org/10.1002/hep.23785.
Xu Y, Zhang Y-G, Wang X, Qi W-Q, Qin S-Y, Liu Z-H, et al. Long-term antiviral efficacy of entecavir and liver histology improvement in Chinese patients with hepatitis B virus-related cirrhosis. World J Gastroenterol. 2015;21(25):7869–76. https://doi.org/10.3748/wjg.v21.i25.7869.
Wang B-Q, Wang Y-L, Shi K-Q. Four-year entecavir therapy reduces hepatocellular carcinoma, cirrhotic events and mortality in chronic hepatitis B patients. Liver Int. 2017;37(2):309–10. https://doi.org/10.1111/liv.13289.
China Food and Drug Administration Good clinical practice guideline. 2010. http://www.sda.gov.cn/WS01/CL0053/24473.html. Accessed 30 Oct 2010.
ICH Topic E 6 (R1): Guideline for Good Clinical Practice. Note for guidance on good clinical practice. 2010. http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2009/09/WC500002874.pdf. Accessed 30 Oct 2010.
World Medical Association Declaration of Helsinki—ethical principles for medical research involving human subjects. 2013. http://www.wma.net/en/30publications/10policies/b3/index.html. Accessed Oct 2013.
Blach S, Zeuzem S, Manns M, Altraif I, Duberg A-S, Muljono DH, et al. Global prevalence and genotype distribution of hepatitis C virus infection in 2015: a modelling study. Lancet Gastroenterol Hepatol. 2017;2(3):161–76. https://doi.org/10.1016/s2468-1253(16)30181-9.
Yang X, Ma Z, Zhou S, Weng Y, Lei H, Zeng S, et al. Multiple drug transporters are involved in renal secretion of entecavir. Antimicrob Agents Chemother. 2016;60(10):6260–70. https://doi.org/10.1128/aac.00986-16.
Xu Q, Wang C, Meng Q, Liu Q, Sun H, Peng J, et al. OAT1 and OAT3: targets of drug-drug interaction between entecavir and JBP485. Eur J Pharm Sci. 2013;48(4–5):650–7. https://doi.org/10.1016/j.ejps.2012.12.024.
Liu Y, Wu J, Li Z, Luo Y, Zeng F, Shi S. Tolerability and pharmacokinetics of hydronidone, an antifibrotic agent for hepatic fibrosis, after single and multiple doses in healthy subjects: an open-label, randomized, dose-escalating, first-in-human study. Eur J Drug Metab Pharmacokinet. 2017;42(1):37–48. https://doi.org/10.1007/s13318-015-0316-z.
Matthews SJ. Entecavir for the treatment of chronic hepatitis B virus infection. Clin Ther. 2006;28(2):184–203. https://doi.org/10.1016/j.clinthera.2006.02.012.
Acknowledgements
We thank the participants of the study.
Funding
This work was supported by National Natural Science Foundation of China (82104274, 82173902, 81874326), General Project of Wuhan Health Research Fund (WX21D55), Project of Beijing Medical Award Foundation (YXJL-2018-0095-0068). The Rapid Service Fee was funded by these foundations.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Author Contributions
Study concept and design (Shaojun-Shi, Yani-Liu), data acquisition and interpretation (all authors), literature research, statistical analysis and drafting of the manuscript (Rui-Zhang), approval of the final version (all author), administrative, technical, or material support (Shaojun-Shi), and study supervision (Yani-Liu). All authors have made a significant contribution to this study.
Disclosures
Shaojun-Shi, Yani-Liu, Rui-zhang, Peixia-Li, Pengpeng-Guo; Jinping-Zhou; Jing-Wan; Chunxiao-Yang and Jiali-Zhou declare that they have no competing interests.
Compliance with Ethics Guidelines
The trials were performed conform to Good Clinical Practice (GCP) standards of China National Medical Products Administration (NMPA)[20], the International Conference on Harmonisation GCP guidelines and the Declaration of Helsinki (as revised in Brazil, 2013). The approval number of this study was 2011S00434 which granted by NMPA, and the independent ethics committee of Tongji Medical College of Huazhong University of Science and Technology (Wuhan, China) agreed to implement this protocol [approval no. (2014)185]. All volunteers voluntarily signed informed consent.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, R., Li, P., Guo, P. et al. A Pharmacokinetic Drug–Drug Interactions Study between Entecavir and Hydronidone, a Potential Novel Antifibrotic Small Molecule, in Healthy Male Volunteers. Adv Ther 40, 658–670 (2023). https://doi.org/10.1007/s12325-022-02377-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-022-02377-x