Abstract
The aim of the present study was to evaluate advantages of partial posterior fundoplication (PPF) compared with traditional total fundoplication (TF). The study included 90 patients with GERD at El-Minia University Hospital between January 2019 and January 2023, divided randomly into group A: PPF (no. 45 patients) and group B: TF (no. 45 patients). All included patients had endoscopic hiatal hernia and various degrees of esophagitis. Postoperative follow-up included satisfaction questionnaire, degree of heartburn questionnaire, frequent belching, inability to belch, bloating, diarrhea, vomiting, abdominal pain, and endoscopic evaluations. Heartburn improved in all patients (p = 0.000). Shorter operative time was observed in group B (p = 0.007). There is no significant difference in overall satisfaction level between the two groups (p = 0.5). Surgical treatment is the favorite option for the treatment of GERD. PPF has the advantage of shorter operative time and can be safely used with outcomes similar to that of TF.
Similar content being viewed by others
Introduction
Proton pump inhibitors (PPIs) are one of the therapeutic options for patients with GERD. However, anti-reflux surgery is now a well-established therapeutic option. Laparoscopic anti-reflux surgery has been proved to be more effective than PPIs for treatment of GERD [1, 2] with elimination of some dangerous long-term side effects of PPIs [3, 4]. Laparoscopic anti-reflux surgery restores the functional and anatomical insufficiencies in the EGJ. However, it is considered much invasive and has some unavoidable mechanical complications such as bloating and dysphagia [5]. Total Nissen fundoplication (TF) is the most commonly performed anti-reflux surgery [6]. Alternative surgical procedures have been invented aiming at minimizing the mechanical complications of TF [7]. Toupet invented his 180° posterior wrap in the 1960s, and thereafter an anterior 180° wrap was designed [8]. A series of randomized clinical studies reported that partial fundoplication (PF) is associated with fewer mechanical complications (e.g., flatulence and bloating) than TF [9, 10]. However, it is reported that TF is better than PF in terms of reflux control, durable function of the wrap and recurrence rate [11, 12]. This implemented modification of PF to encircle 3/4 the circumference of the lower esophagus what is called laparoscopic posterior partial fundoplication (PPF). The aim was to maintain the advantages of fewer mechanical complications of the partial wrap and the advantages of reflux control of TF. The aim of the present study was to evaluate the advantages of PPF compared with a traditional TF.
Patients and Methods
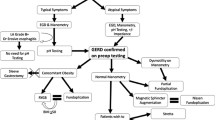
The study included 90 patients with GERD at El-Minia University Hospital between January 2019 and January 2023. The study was approved by Minia College of Medicine Institutional Ethics Committee. Written informed consent was obtained from all included patients. Patients were divided randomly into two groups; group A: PPF (no. 45 patients) and group B: TF (no. 45 patients). Patient selection was made using simple randomization (1:1 ratio); PPF was applied to one patient and TF to the other patient, in sequential order. The study included patients aged 18–75 years with GERD symptoms, mainly heartburn and acid regurgitation. GERD diagnosis was confirmed by ambulatory pH monitoring showing increased acid exposure over 24 h. Esophagitis was graded according to Los Angeles classification (LA) [13]. Patients with previous anti-reflux surgery or major upper abdominal surgical procedures, type II to IV hiatal hernia and those with esophageal motility disorders were excluded. All included patients had endoscopic hiatal hernia and various degrees of esophagitis. Patients’ data including age, sex, grade of esophagitis, duration of preoperative symptoms and medical treatment, date of surgery, duration of operation, postoperative follow-up, postoperative complications, and reoperation were all recorded. Preoperative investigations included 24-h pH monitoring, upper GI endoscopy, and esophageal manometry. Postoperative follow-up included satisfaction questionnaire assessing presence or absence of dysphagia to solids or liquids on 0–4 scale (0: no swallowing problems, 1: difficult swallowing of solid food, 2: difficult swallowing of soft food, 3: difficult swallowing of liquids, and 4: difficult swallowing of both solids and liquids). Another questionnaire determining the degree of heartburn, frequent belching, inability to belch, bloating, diarrhea, vomiting, abdominal pain on 0–4 scale (0: no symptoms, 1: mild (notable but not annoying every day), 2: moderate (notable and annoying every day), 3: often (influencing daily life), and 4: very often (limiting daily life)) was administered to all patients [14]. Gastroesophageal reflux disease health-related quality of life (GERD-HRQoL) questionnaire was administered to patients preoperatively, 2 and 12 months postoperatively together with endoscopic evaluations. Postoperative satisfaction was assessed using 0–4 scale (1: very satisfied, 2: satisfied, 3: neutral, and 4: not satisfied) [16]. All patients were followed up for 1 year.
Surgical Technique [15]
With patient in reversed Trendelenburg, 5-trocar technique was used with surgeon standing between patient’s legs. Ultracision harmonic scalpel was used. Incision of the lesser omentum and peritoneum covering the hiatal region with exposure of left and right crus was done. Division of short gastric vessels was done to mobilize the upper part of gastric fundus. The distal esophagus was mobilized for at least 5 cm to ensure intra-abdominal position of EGJ and wrap. For PPF patients, gastric fundus was pulled posteriorly around the distal part of esophagus and EGJ for approximately 3/4 the circumference and anchored posteriorly to left and right crus with 3 ethibond 2/0 sutures for each. Then, 3–4 sutures were applied between edges of the wrap and esophageal wall (Fig. 1). For TF patients, right and left edges of the wrap were sutured together 3 ethibond 2/0 sutures from EGJ and cranially for at least 2 cm (Fig. 2). Bougies were used in all patients. All procedures were performed by only one surgeon.
Statistical Analysis
Values were given as medians ± SD (standard deviation) or percentage. Independent sample T-test was used to compare parametric data, whereas chi-square tests used to compare non-parametric data. P value of less than 0.05 was considered statistically significant.
Results
The involved 90 patients were divided randomly into two groups; group A: PPF (no. 45 patients) and group B: TF (no. 45 patients). There were no significant differences in age, sex, BMI, incidence of esophagitis or Barrett’s esophagus between the two groups. There was also no significant difference in the preoperative clinical data as regard duration of symptoms or duration of medical treatment between the two groups (p = 0.4, 0.6; respectively). Preoperative Grade A esophagitis was the most common in both groups (64% vs. 60%), with no significant difference between the two groups (p = 0.5) (Table 1). Operative time was significantly shorter in group B (PPF) (p = 0.007). Hospital stay was almost the same for both groups (mean = 1.86, 1.73 days; respectively) (p = 0.3). Complications in group A developed in 2 patients; port site bleeding in one patient which was controlled laparoscopically and infected hematoma in another patient treated conservatively. However, in group B, only one patient developed DVT which was treated conservatively. There was no significant difference in incidence of complications between the two groups (p = 0.5). Reoperation was needed in one patient in group A due to unimproved difficult swallowing during the year of follow-up, but without significant difference between the two groups (p = 0.3). There was also no significant difference between the two groups as regard postoperative symptoms which were treated conservatively. Endoscopy at second postoperative month showed no esophagitis in 11 patients (12%), while endoscopy at twelfth postoperative month revealed complete improvement of esophagitis in 78 patients (86.7%). There was no significant difference between the two groups as regards the two follow-up endoscopies (p = 0.8, 0.5; respectively). As regards overall satisfaction level, 48 patients were very satisfied (53.3%); 35 patients were satisfied (38.9%); 5 patients were neutral (5.5%); and 2 patients were not satisfied (2.2%) with their resulting condition (p = 0.5) (Table 2). Heartburn was improved in all patients with significant difference between preoperative and postoperative periods in each group (p = 0.000) (Table 3). PPIs were recommended for all patients with grade A and B esophagitis diagnosed in the twelfth postoperative month.
Discussion
PPF had been shown to be as successful as TF in randomized controlled trials [16,17,18]. A study by Negre [19] showed bothersome gastrointestinal symptoms in 26% of patients and unbearable gastrointestinal complaints in 10%, while Swanstrom and Wayne [20] reported postoperative gastrointestinal symptoms in 96% of patients. This wide difference in results in literature may be due to that not all patients were operated on by the same surgeon and postoperative evaluation was made by different observers. This was overcome in the present study as all patients were operated on by the same surgeon, and postoperative assessment was done by a single observer. Dysphagia and bloating were discussed in the literature as the most common postoperative symptoms [21, 22]. In the present study, 23 patients (25.5%) reported various degrees of bloating, with equal number in both groups reporting mild bloating not affecting daily life. Only one patient in TF group reported medium bloating that affects daily life which may not be related to reflux surgery [23, 24]. Postoperative dysphagia may be divided into early and late forms. It may be due to several reasons (e.g., undiagnosed motility disorder, denervation of the lower esophagus, and tight wrap) [25, 26]. Different rates of dysphagia were reported in the literature; 25% by Beldi and Glattti [27], 34% by Frantzides et al. [28] and 10% by Parsak et al., it was mainly to solid food [14]. In the present study, dysphagia was reported in 6 patients (6.7%) which was consistent with the literature and was mainly linked to swallowing of solid food [14]. While frequent belching postoperatively may indicate loose fundoplication, late frequent belching may suggest shift of the wrap representing an important symptom during follow-up. Inability to belch is also a common postoperative complaint in reflux patients which may be due to injury of afferent nerves of belch reflex during dissection of short gastric vessels. A recent study by Parsak et al. found that the rate of frequent belching and inability to belch to be 11.3% and 20%; respectively [14], while our study reported lower rate of 4.4% and 7.8%; respectively, which may be due to higher learning curve and meticulous dissection by our surgeon. Postoperative heartburn is not necessarily a symptom of GERD, as it may be attributed to previous irritation of the esophagus, and it may take 3 months to resolve [28, 29]. Our study demonstrated heartburn to various degrees in all patients preoperatively, while this rate declines significantly to 8.9% postoperatively (p = 0.000) and occurred mostly once a week which did not bother the patient. Only 5.5% of patients had recurrent symptoms and underwent medical treatment. This was consistent with results of a study by Parsak et al. who reported postoperative decline of heartburn to 11.23% and recurrent symptoms in 7.5% of patients [14]. About 92.2% of patients were satisfied with their current condition, which was comparable to a previous study reporting satisfaction rate of 92.5% [14], proving that operation is well-tolerated and effective. Laparoscopic anti-reflux surgeries had been proven to be successful with low morbidity. Development of different postoperative symptoms may be attributed to nerve injury, tight wrap, shift of wrap into the chest, dietary habits, postoperative adhesions, and swallowing of air [30]. Our study limitations were small sample size and subjective nature of some data. Our study concluded that surgical treatment is a favorite option for treatment of GERD. PPF has the advantage of shorter operative time and can be safely used with outcomes similar to that of TF.
Data Availability
The authors confirm that the data supporting the findings of this study are available within the article.
References
Lundell L, Miettinen P, Myrvold HE, Nordic GERD Study Group et al (2009) Comparison of outcomes twelve years after antireflux surgery or omeprazole maintenance therapy for reflux esophagitis. Clin Gastroenterol Hepatol. 7(12):1292–1298
Galmiche JP, Hatlebakk J, Attwood S, LOTUS Trial Collaborators et al (2011) Laparoscopic antireflux surgery vs esomeprazole treatment for chronic GERD: the LOTUS randomized clinical trial. JAMA. 305(19):1969–1977
Brusselaers N, Wahlin K, Engstrand L et al (2017) Maintenance therapy with proton pump inhibitors and risk of gastric cancer: a nationwide population-based cohort study in Sweden. BMJ Open 7(10):e017739
Cheung KS, Chan EW, Wong AYS et al (2018) Long-term proton pump inhibitors and risk of gastric cancer development after treatment for Helicobacter pylori: a population-based study. Gut 67(1):28–35
Scarpellini E, Ang D, Pauwels A et al (2016) Management of refractory typical GERD symptoms. Nat Rev Gastroenterol Hepatol 13(5):281–294
Nissen R (1956) A simple operation for control of reflux esophagitis [in German]. Schweiz Med Wochenschr 86(suppl 20):590–592
Rossetti M, Hell K (1977) Fundoplication for the treatment of gastroesophageal reflux in hiatal hernia. World J Surg 1(4):439–443
Toupet A (1963) Technic of esophago-gastroplasty with phrenogastropexy used in radical treatment of hiatal hernias as a supplement to Heller’s operation in cardiospasms [in French]. Mem Acad Chir (Paris) 89:384–389
Roks DJ, Broeders JA, Baigrie RJ (2017) Long-term symptom control of gastro-oesophageal reflux disease 12 years after laparoscopic Nissen or 180° anterior partial fundoplication in a randomized clinical trial. Br J Surg 104(7):852–856
Broeders JA, Mauritz FA, Ahmed Ali U et al (2010) Systematic review and meta-analysis of laparoscopic Nissen (posterior total) versus Toupet (posterior partial) fundoplication for gastro-oesophageal reflux disease. Br J Surg 97(9):1318–1330
Hagedorn C, Jönson C, Lönroth H et al (2003) Efficacy of an anterior as compared with a posterior laparoscopic partial fundoplication: results of a randomized, controlled clinical trial. Ann Surg 238(2):189–196
Catarci M, Gentileschi P, Papi C et al (2004) Evidence-based appraisal of antireflux fundoplication. Ann Surg 239(3):325–337
Lundell LR, Dent J, Bennett JR et al (1999) Endoscopic assessment of oesophagitis: clinical and functional correlates and further validation of the Los Angeles classification. Gut 45(2):172–180
Parsak CK, Halvacı I, Topal U (2023) Comparison of Nissen Rossetti and Floppy Nissen techniques in laparoscopic reflux surgery. Ann Med 55(1):1000–1008
Håkanson BS, Lundell L, Bylund A et al (2019) Comparison of laparoscopic 270° posterior partial fundoplication vs total fundoplication for the treatment of gastroesophageal reflux disease. JAMA Surg 154(6):479–486
Chrysos E, Tzortzinis A, Tsiaoussis J et al (2001) Prospective randomized trial comparing Nissen to Nissen-Rossetti technique for laparoscopic fundoplication. Am J Surg 182(3):215–221
Leggett PL, Bissell CD, Churchman-Winn R et al (2000) A comparison of laparoscopic Nissen fundoplication and Rossetti’s modification in 239 patients. Surg Endosc 14(5):473–477
Watson DI, Jamieson GG, Pike GK et al (1999) Prospective randomized double-blind trial between laparoscopic Nissen fundoplication and anterior partial fundoplication. Br J Surg 86(1):123–130
Negre JB (1983) Post-fundoplication symptoms. Do they restrict the success of Nissen fundoplication? Ann Surg. 198(6):698–700
Swanstrom L, Wayne R (1994) Spectrum of gastrointestinal symptoms after laparoscopic fundoplication. Am J Surg 167(5):538–541
Leggett PL, Churchman-Winn R, Ahn C (1998) Resolving gastroesophageal reflux with laparoscopic fundoplication. Findings in 138 cases. Surg Endosc. 12(2):142–147
Klingler PJ, Hinder RA, DeVault KR (1997) Laparoscopic antireflux surgery experience and outcomes. Chir Gastroenterol 13(2):138–142
Lundell L (2007) Therapy of gastroesophageal reflux: evidence-based approach to antireflux surgery. Dig Dis 25(3):188–196
Serafini FM, Bloomston M, Zervos E et al (2001) Laparoscopic revision of failed antireflux operations. J Surg Res 95(1):13–18
Fumagalli U, Bona S, Battafarano F et al (2008) Persistent dysphagia after laparoscopic fundoplication for gastro-esophageal reflux disease. Dis Esophagus 21(3):257–261
Biertho L, Sebajang H, Anvari M (2006) Effects of laparoscopic Nissen fundoplication on esophageal motility: long-term results. Surg Endosc 20(4):619–623
Beldi G, Glattli A (2002) Long-term gastrointestinal symptoms after laparoscopic Nissen fundoplication. Surg Laparosc Endosc Percutan Tech 12:316–319
Frantzides CT, Carlson MA, Zografakis JG et al (2006) Postoperative gastrointestinal complaints after laparoscopic Nissen fundoplication. JSLS 10:39–42
DeMeester TR, Bonavina L, Albertucci M (1986) Nissen fundoplication for gastroesophageal reflux disease. Evaluation of primary repair in 100 consecutive patients. Ann Surg. 204(1):9–20
Granderath FA, Kamolz T, Schweiger UM et al (2002) Longterm results of laparoscopic antireflux surgery. Surg Endosc 16(5):753–757
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Consent to Participate
Informed consent was obtained from all the individual participants included in the study. The study was approved by Minia College of Medicine Institutional Ethics Committee.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mohamed, A.A., Elian, M.A., Abdelzaher, M.A. et al. Laparoscopic Posterior Partial Fundoplication Versus Total Fundoplication in Anti-reflux Surgery: A Comparative Study. Indian J Surg (2024). https://doi.org/10.1007/s12262-023-04016-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12262-023-04016-3